How Are Autoimmune Diseases In Dermatology Diagnosed
A biopsy is usually needed for a definitive diagnosis of autoimmune skin disease, although a characteristic appearance may be suggestive of a particular condition .
Blood tests may include:
- Tests for circulating skin autoantibodies
- Tests for coeliac antibodies, such as IgA tissue transglutaminase antibodies
- Nonspecific tests for inflammatory markers
- An autoimmune screen .
Swabs may be taken of a ruptured blister to look for signs of a bacterial infection or herpes virus infection.
Autoimmune Blistering Disorder Diagnosis
You’ll see a dermatologist. They will look at your skin and see where the blisters have formed.
You might get one or more of these tests:
- Blister biopsy. Your doctor removes a piece of the blister and looks at it under a microscope. A biopsy can show where the skin layers have separated.
- Direct immunofluorescence. A chemical is placed on the skin biopsy sample. Then it is tested for antibodies. The type of antibodies in your skin can show which type of blistering disorder you have.
- Blood test. Your doctor tests a sample of your blood for antibodies. This test can show how severe your condition is. It can also help the doctor see whether treatment is working.
Sometimes itâs hard to tell the difference between autoimmune blistering disorders and other conditions, including:
- Genetic blistering disease, a group of disorders caused by changes in a gene needed for healthy skin
- Groverâs disease, a rare skin disorder that can cause small red lesions and blisters
- Other skin conditions that cause blisters, such as erythema multiforme or impetigo
Skin Barrier And Autoimmunitymechanisms And Novel Therapeutic Approaches For Autoimmune Blistering Diseases Of The Skin
- Regenerative Medicine Laboratory, Future Industries Institute, University of South Australia, Adelaide, SA, Australia
One of the most important functions of the skin besides regulating internal body temperature includes formation of the barrier between the organism and the external environment, hence protecting against pathogen invasion, chemical and physical assaults and unregulated loss of water and solutes. Disruption of the protective barrier is observed clinically in blisters and erosions of the skin that form in autoimmune blistering diseases where the body produces autoantibodies against structural proteins of the epidermis or the epidermal-dermal junction. Although there is no cure for autoimmune skin blistering diseases, immune suppressive therapies currently available offer opportunities for disease management. In cases where no treatment is sought, these disorders can lead to life threatening complications and current research efforts have focused on developing therapies that target autoantibodies which contribute to disease symptoms. This review will outline the involvement of the skin barrier in main skin-specific autoimmune blistering diseases by describing the mechanisms underpinning skin autoimmunity and review current progress in development of novel therapeutic approaches targeting the underlying causes of autoimmune skin blistering diseases.
Read Also: What If I Have Skin Cancer
What Medicines Treat Pemphigus
Medicines used to treat pemphigus include:
- Corticosteroids: Medication to reduce inflammation , delivered by mouth, by injection or topically .
- Immunosuppressive drugs: Drugs that manage your bodys autoimmune response, which is what happens when your body attacks healthy cells.
- Rituximab: A monoclonal antibody that targets problematic B cells.
- Intravenous immunoglobulin: Healthy antibodies , given through a needle into your vein, to help reduce the antibodies that cause your diagnosis.
- Antibiotics: In some cases, infections can develop in pemphigus blisters. If this happens, your doctor may prescribe antibiotic medicine to treat the infection.
Are there side effects of the treatment?
Side effects vary based on the type of treatment and could include:
- Upset stomach.
- Weight gain.
Your healthcare provider will monitor your condition regularly and order blood and/or urine tests to verify that your treatment is working. Tests also check for negative reactions to medications that treat pemphigus.
Thick Skin With Scales
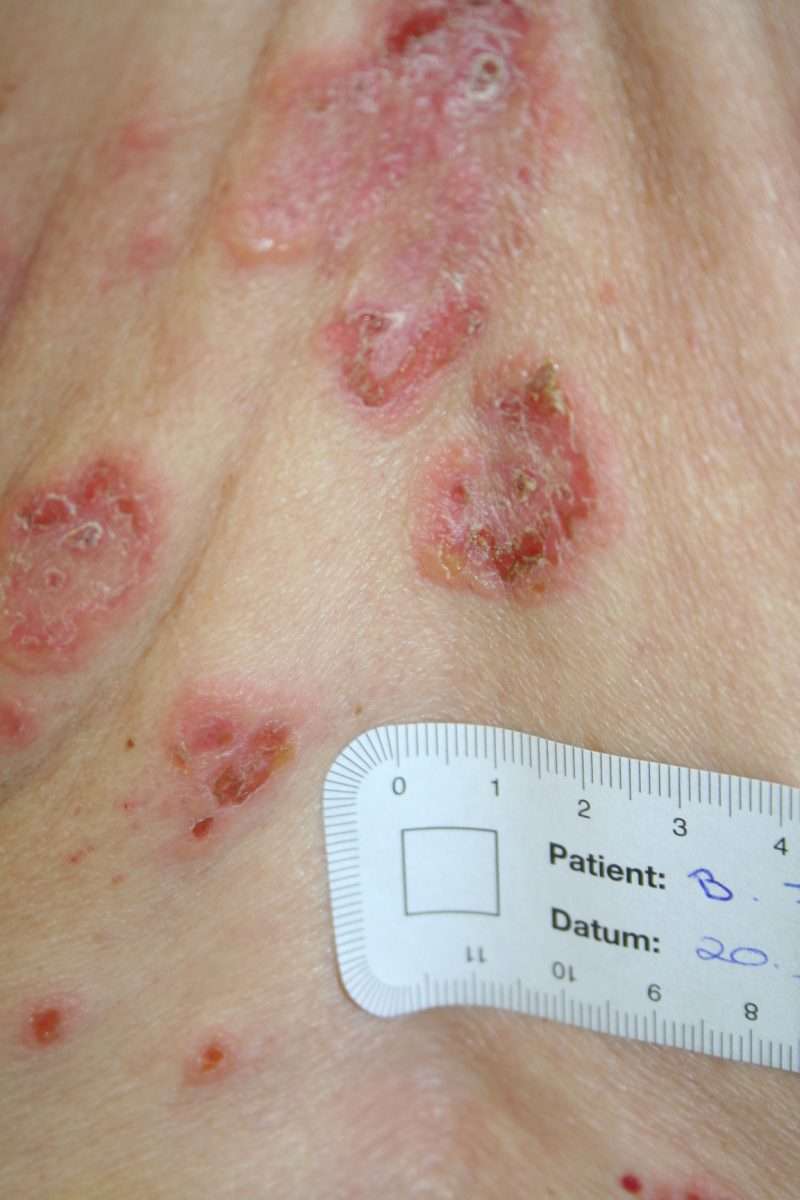
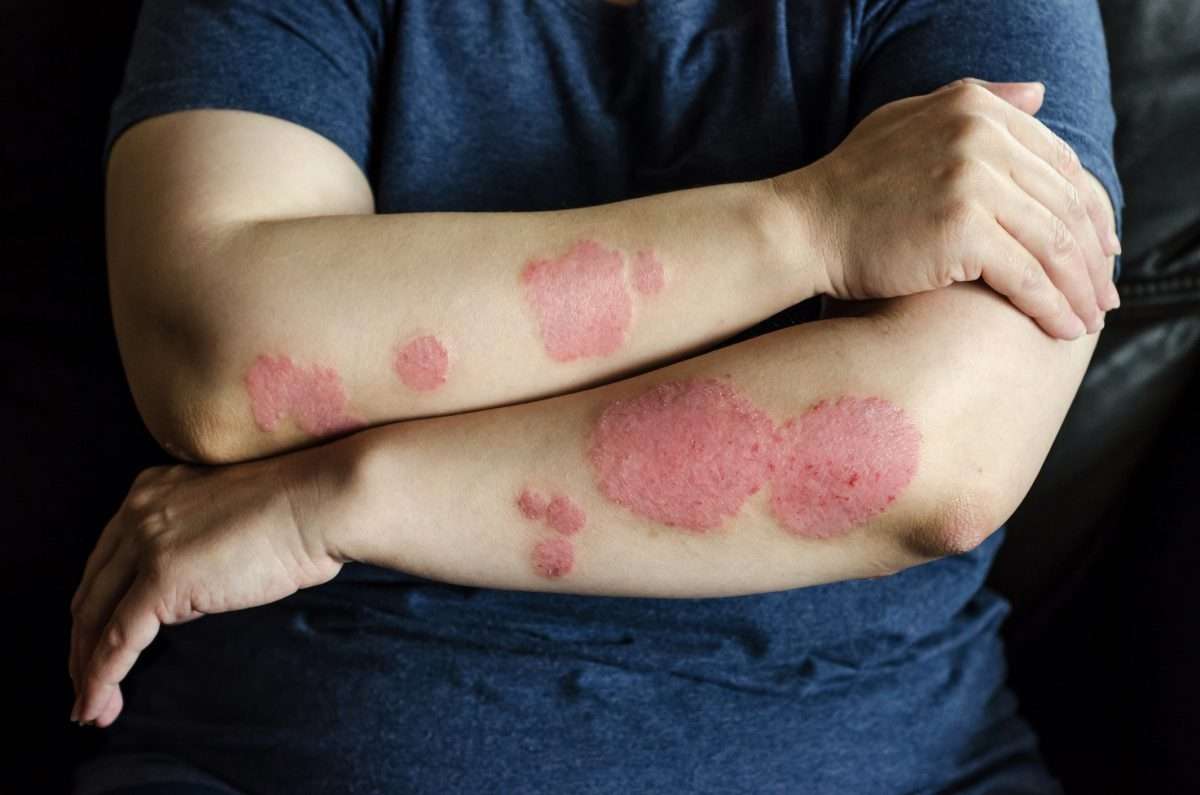
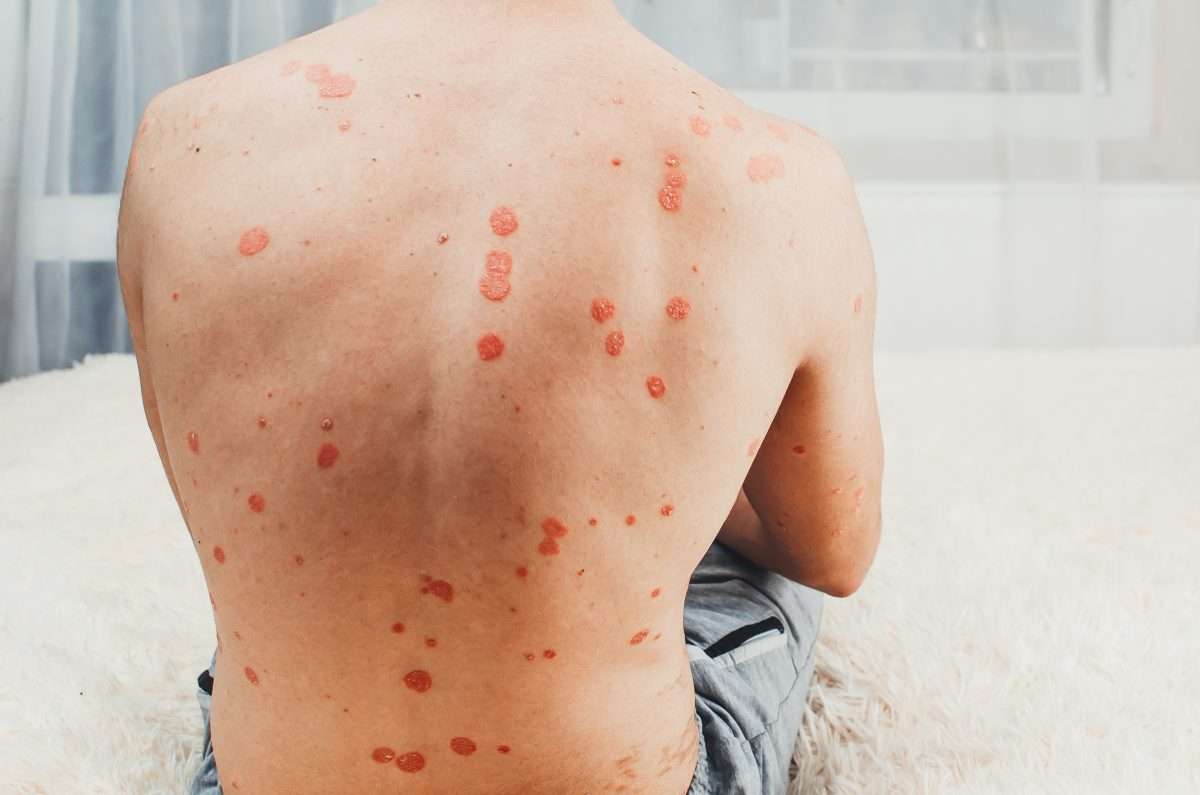
Psoriasis is a common autoimmune disease that affects about 3% of adults in the U.S. Its a chronic condition that causes patches of skin to grow too quickly. There are different types of psoriasis, and the most common one is called plaque psoriasis. This causes red patches with thick white scales to form, usually on the:
-
Elbows
Psoriasis is usually a life-long condition, and treatment depends on how severe the symptoms are. This usually includes medicated creams and pills or shots that can help lower the immune system.
Don’t Miss: How Long Can You Have Melanoma And Not Know It
Autoimmune Blistering Disorder Causes
When your immune system is working as it should, it attacks bacteria and other invaders before they can make you sick. In autoimmune blistering disorders, your system mistakes healthy cells in your skin and mucous membranes for unwanted intruders.
Your immune system makes proteins called antibodies. These attack the substances that hold the outer and inner layers of skin together. The damage causes the two layers of skin to separate. Fluid collects between the two and forms blisters.
Doctors don’t know what causes the immune system to misfire. Some people have genes that make them more likely to get one of these disorders. Then, something actually triggers it, such as:
- Ultraviolet light from the sun
- Chemicals used to kill pests
- Hormones
- Antibiotics such as amoxicillin , ciprofloxacin , and penicillin
Usually, the blisters go away once you stop taking the medicine causing them.
What Does An Autoimmune Rash Look Like
Different autoimmune diseases can cause different skin changes. Some symptoms are general while others are pretty specific for a specific condition. Some common skin changes are:
-
Pink or red rashes
-
Open sores
-
Blisters in the skin
Seeing a dermatologist or healthcare provider with skin expertise may be needed to get the right diagnosis. This may require a skin biopsy, a procedure done in your providers office that removes a small piece of tissue. Below, well discuss common skin changes seen in certain autoimmune diseases.
Read Also: How To Know You Have Skin Cancer
Alopecia Areata Can Cause Large Bald Spots
If you start losing large amounts of hair creating large bald spots, it may be due to alopecia areata, a condition where the immune system attacks the hair follicles in otherwise healthy people. This disease is marked by hair loss that occurs in round patches. You may lose all the hair on your scalp or body.
Alopecia areata is an unpredictable disease, and there is no cure. Hair growth sometimes restarts on its own, or there are treatments to spur regrowth. Your dermatologist can inject your scalp with corticosteroids and prescription creams may also help. Minoxidil, which is now available over the counter, is safe for children and adults to use. While you work with your doctor on treating alopecia, you may want to try changing your hairstyle to cover the alopecia patches or temporarily using a hair piece, suggests Dr. Simzar.
Are Skin Changes Permanent
The good news is that most autoimmune skin changes are not permanent. But there are some exceptions. When skin inflammation is deep enough, it can cause scarring or discoloration. Some examples include:
-
Discoid lupus erythematosus usually causes permanent scars, discoloration, or hair loss
-
Certain types of bullous pemphigoid can also leave permanent scars on the skin or mucous membranes .
Some conditions like morphea, psoriasis, and pemphigus can leave discolored skin even after the rash has improved. These changes are usually not permanent and fade over time.
Also Check: What Does Skin Cancer On The Outer Ear Look Like
Autoimmune Blistering Disorder Treatment
Your doctor will decide on a treatment based on your symptoms. Medicines for these disorders lower the immune system response and prevent it from attacking your skin and mucous membranes. Treatments might include prescriptions from these classes of drugs:
- Corticosteroids, such as prednisone , that also ease inflammation
- Immunosuppressive medicines, such as azathioprine , cyclophosphamide, or mycophenolate mofetil
- Biologic drugs, such as rituximab , also used in some cancer treatments
For more serious cases, your treatments might include:
- Intravenous immunoglobulin G . This is a blood product you get through a needle into a vein. IVIG is an antibody found in plasma — the liquid part of blood. It’s taken from thousands of donors and pooled together. IVIG treatment gives you healthy antibodies to take over for the unhealthy ones that caused your disorder.
- Plasmapheresis. This treatment removes the harmful antibodies from your blood. The part of blood that’s removed is replaced with blood from a donor that contains healthy antibodies.
Blisters that pop open can get infected. These drugs help prevent an infection:
- Antibiotics
- Antifungal drugs
Autoimmune Blistering Disorder Symptoms
The places on your body where blisters form depends on which disorder you have. Some types cause blisters to grow on the skin. Other types cause them to form in the mucous membranes that line the mouth, nose, throat, eyes, and genitals.
They can be painful or itchy. They can break open and leave a sore.
Also Check: How Fast Does Malignant Melanoma Spread
How Do I Take Care Of Myself And Manage My Symptoms
You can take steps at home to manage your symptoms of pemphigus by:
- Avoiding crunchy, acidic or spicy foods that can irritate mouth and throat blisters.
- Caring for your blisters as directed by your healthcare provider.
- Staying out of the sunlight or covering your skin with sunscreen or wearing protective clothing to prevent UV ray damage to your skin.
- Using soaps and lotions designed for sensitive skin, without fragrances to prevent skin irritation.
Of Systemic Lupus Erythematosus 1
Systemic Lupus Erythematosus. Systemic lupus erythematosus is the most common form of the autoimmune disease lupus. This red scaly rash on a person’s cheek is typical. SLE affects the skin and other internal organs. It’s possible for the heart, lungs and brain to become involved, followed by the formation of scar tissue . SLE is usually treated with corticosteroids.
You May Like: What Is Squamous Cell Carcinoma In Mouth
Expert Diagnosis And Treatment For Autoimmune Blistering Skin Diseases
These blisters tend to be more widespread and heal more slowly than blisters caused by minor burns, friction, or injuries. They also may cause scarring.
Men and women are equally affected by autoimmune blistering diseases. Although most of these disorders occur in people in their 50s and 60s, they can develop in people of all ages, including children.
UT Southwestern is home to a Clinical Laboratory Improvement Amendments -certified Cutaneous Immunopathology Laboratory that is dedicated to the diagnosis and classification of autoimmune skin disorders. Our experienced physicians are recognized leaders in the treatment of both autoimmune diseases and complex skin conditions.
We also offer specialty clinics for patients with autoimmune blistering diseases.
Treating Autoimmune Blistering Skin Diseases
The primary treatment for these disorders is treatment withcorticosteroids such as prednisone. Additional medications that our doctorsmight prescribe include:
- Immunosuppressive biological therapies such as rituximab
- Immunosuppressive drugs, such as azathioprine, cyclophosphamide, or mycophenolate
- Antibiotic, antifungal, or antiviral medicationsto prevent infections
Also Check: Where Does Metastatic Melanoma Spread
What Are Autoimmune Disorders Of The Skin
Autoimmune diseases or disorders occur when the bodys immune system cannot distinguish between healthy body tissue and an antigen or foreign substance. Normally, the immune system reacts to viruses, bacteria or foreign harmful substances that invade the body. An autoimmune disease causes the bodys immune response to destroy healthy body tissue by mistake or to react to healthy tissue it would normally ignore.
There are more than 80 types of known autoimmune disorders that affect organs and tissues. Autoimmune diseases are often chronic diseases that affect:
- Blood vessels and red blood cells
- Connective tissues
- Glands such as the thyroid or pancreas
- Joints
- Skin
How Does Scleroderma Affect The Skin
Scleroderma is a term that just means ‘hard skin.’ Like lupus, patients having scleroderma skin changes have a variable risk for having associated damage to internal organs, especially the kidneys and lungs.
Some patients develop a form of scleroderma that never goes on to cause damage to internal organs. This form of the disease is called localized scleroderma or morphea. However, other patients with scleroderma do develop internal complications relatively soon after the onset of skin problems.
Also Check: What Can Skin Cancer Do To You
What Causes Autoimmune Disease
“Some theorize that genetics and/or environmental pollutants play a role.”
The cause or causes of autoimmune disease are not understood, although some theorize that genetics and/or environmental pollutants play a role. Certain drugs have also been reported as potential triggers for pemphigus foliaceus, a common form of autoimmune skin disease in cats. Early recognition is extremely important. Left untreated, the complications of autoimmune disease are serious and multiple system involvement is common. This can make diagnosis and treatment very challenging and complicated.
Your Skin And Autoimmune Disease
Your skin is your bodys largest organ. When something isnt right in your body, your skin is often the first indication that theres a problem. This is definitely true when it comes to autoimmune disease.
Virtually all autoimmune diseases can affect your skin, either directly or even through side effects from autoimmune disease treatments, says Dr. Erin Foster. A dermatologist, Dr. Foster is an expert in treating autoimmune blistering diseases.
Along with fellow dermatologist, Dr. Noelle Teske, Dr. Foster is now seeing patients at the Center for Womens Health for everything from acne and skin cancer screening to more complex skin problems.
We asked Dr. Foster to help us understand the connection between autoimmune diseases and skin.
The skin is not just your largest, most visible organ, Dr. Foster says. Its full of the immune cells you need to prevent infection and when there are problems with your immune system, we often see problems in your skin too.
A few examples:
Many autoimmune diseases, including lupus, can also make your skin more sensitive to the sun. If you have skin issues along with autoimmune disease, a dermatologist can be an important part of your care. Even if you have rashes or sores caused by medication you take for your condition, a dermatologist can help you find an ointment or cream to lessen the side effects.
Dr. Noelle Teske has expertise in treating complex conditions caused by autoimmune diseases like lupus and scleroderma.
Don’t Miss: What Are The Symptoms Of Basal Cell Carcinoma
Autoimmune Diseases Of The Skin
Pathogenesis, Diagnosis, Management
You can also search for this editor inPubMed
-
Comprehensive presentation of pathophysiology, clinical diagnosis, and management of cutaneous autoimmune diseases
-
Thoroughly updated with new chapters on inflammatory diseases
-
Presented by world experts in the field
-
42k Accesses
This is a preview of subscription content, access via your institution.
Dermatomyositis Causes A Skin Rash
Dermatomyositis is an inflammatory disease that causes a skin rash on the face and eyelids, as well as on the shoulders, upper chest, and back, and around the knuckles. Other symptoms include muscle weakness, shortness of breath, and trouble swallowing. It is most common in children between ages five and 15 and in adults between ages 40 and 60.
The autoimmune disorder is treated with immunosuppressants and corticosteroids. In children, the symptoms often go away completely. Adults need to be more careful as this may be a sign of another underlying disease and could develop pneumonia or lung failure, which can be fatal in some cases.
Read Also: What Kind Of Cancer Is Melanoma
How Are These Autoimmune Diseases Treated
While there are currently no curative treatments for these autoimmune diseases, there are courses of action that can lead to periods of remission or a reduction in flare-ups. Depending on the symptoms, there is a range of options that may be used singularly or in conjunction with each other. The symptoms that affect the skin are often the first and sometimes the only ones that appear and are often comparatively easier to treat than those that affect internal organs.
- Lupus: Over-the-counter anti-inflammatory drugs such as Motrin may be used in some patients to treat swelling and pain. Another option to treat inflammation is corticosteroids, though side effects can include a higher risk of contracting infections. Anti-malarial drugs including Plaquenil are often used to treat the symptoms of lupus because theyve been shown to alleviate joint pain, improve skin rashes and help reduce flare-ups significantly. Doctors may also prescribe immunosuppressants such as Azasan , which suppress the immune system to prevent it from attacking the cells it shouldnt be attacking.
Additionally, because ultraviolet light can cause flare-ups, patients are advised to be very careful with sun exposure, wearing sun-protective clothing, hats and sunscreen with a high SPF. There are certain local treatments that can be helpful but number one is sun protection, says Dr. Ramachandran.
When Should I See My Healthcare Provider
Contact your healthcare provider if you:
- Develop blisters on your skin or in your mouth that heal very slowly or dont heal at all.
- Develop blisters on a large area of your body.
- Experience severe pain or discomfort.
- Have an infection, when your blisters break and leak a white to yellow fluid or your skin around your blisters get bigger .
Recommended Reading: What Different Types Of Skin Cancer Are There
Sores In The Mouth Or Genitals
Mouth ulcers, like canker sores, are common and usually go away on their own. If mouth ulcers keep coming back, or if you also have them on the genitals, it could be a sign of a rare autoimmune disorder called Behçet disease.
Behçet disease can happen at any age, but it usually affects people in their 20s and 30s. We dont know the exact cause, but many symptoms are caused by inflammation of blood vessels. The condition can be different in each person, and its common for symptoms to come and go. Some other symptoms include:
-
Skin rashes
-
Eye problems
-
Pain in the joints
-
Diarrhea
-
Headaches
There is no cure for Behçet disease, but symptoms can usually be controlled with different medications. In some people, the symptoms will go away for a period , and treatment may not be needed for a while.
Its important to note that other autoimmune diseases can also cause sores in the mouth or genitals, including lupus and pemphigus. Its a good idea to be checked out by your provider to determine what the underlying cause is.