The Stage Of Melanoma Depends On The Thickness Of The Tumor Whether Cancer Has Spread To Lymph Nodes Or Other Parts Of The Body And Other Factors
To find out the stage of melanoma, the tumor is completely removed and nearby lymph nodes are checked for signs of cancer. The stage of the cancer is used to determine which treatment is best. Check with your doctor to find out which stage of cancer you have.
The stage of melanoma depends on the following:
- The thickness of the tumor. The thickness of the tumor is measured from the surface of the skin to the deepest part of the tumor.
- Whether there are:
- Satellite tumors: Small groups of tumor cells that have spread within 2 centimeters of the primary tumor.
- Microsatellite tumors: Small groups of tumor cells that have spread to an area right beside or below the primary tumor.
- In-transit metastases: Tumors that have spread to lymph vessels in the skin more than 2 centimeters away from the primary tumor, but not to the lymph nodes.
What Is A 5
A relative survival rate compares people with the same type and stage of cancer to people in the overall population. For example, if the 5-year relative survival rate for a specific stage of melanoma of the skin is 90%, it means that people who have that cancer are, on average, about 90% as likely as people who dont have that cancer to live for at least 5 years after being diagnosed.
Patients May Want To Think About Taking Part In A Clinical Trial
For some patients, taking part in a clinical trial may be the best treatment choice. Clinical trials are part of the cancer research process. Clinical trials are done to find out if new cancer treatments are safe and effective or better than the standard treatment.
Many of today’s standard treatments for cancer are based on earlier clinical trials. Patients who take part in a clinical trial may receive the standard treatment or be among the first to receive a new treatment.
Patients who take part in clinical trials also help improve the way cancer will be treated in the future. Even when clinical trials do not lead to effective new treatments, they often answer important questions and help move research forward.
Also Check: How Many People Die From Skin Cancer Every Year
Fine Needle Aspiration Biopsy
FNA biopsy is not used on suspicious moles. But it may be used, for example, to biopsy large lymph nodes near a melanoma to find out if the melanoma has spread to them.
For this type of biopsy, the doctor uses a syringe with a thin, hollow needle to remove very small pieces of a lymph node or tumor. The needle is smaller than the needle used for a blood test. A local anesthetic is sometimes used to numb the area first. This test rarely causes much discomfort and does not leave a scar.
If the lymph node is just under the skin, the doctor can often feel it well enough to guide the needle into it. For a suspicious lymph node deeper in the body or a tumor in an organ such as the lung or liver, an imaging test such as ultrasound or a CT scan is often used to help guide the needle into place.
FNA biopsies are not as invasive as some other types of biopsies, but they may not always collect enough of a sample to tell if a suspicious area is melanoma. In these cases, a more invasive type of biopsy may be needed.
Diagnosis And Prognosis Of Melanoma

The early classification of melanoma was based on where the tumor arose from , but in the 1960s a prominent dermatologist, Wallace Clark, suggested that melanoma ought to be classified based on histological features instead, thus revolutionizing the way melanoma was diagnosed.- He initially described three histological variants of melanoma, superficial spreading melanoma , lentigo maligna melanoma and nodular melanoma ,, and while several new variants such as acral lentiginous melanoma, mucosal melanoma, desmoplastic melanoma and nevoid melanoma have since been described, SSM, LLM and NM are still variants recognized today. This was important work as melanoma was once thought of a homogenous disease Clark was the first to recognize that it is actually a heterogenous disease, to show that the variants behaved differently, had differences in prognosis and that not all melanomas should be treated in the same way.-
Furthermore, in 1966 Clark proposed a system for evaluating melanoma based the depth of invasion of melanoma cells into the dermis and subcutaneous fat.- Clark divided the skin into histologically-identifiable anatomic compartments as melanoma cells traversed each compartment , the risk of distant spread theoretically increased:
Stage I: less than or equal to 0.75 mm
Stage II: 0.76 1.5 mm
Stage III: 1.512.25 mm
Stage IV: 2.263.0 mm
Stage V: greater than 3.0 mm.22
Read Also: What Is Precancerous Skin Cancer
What Are The Symptoms Of Metastatic Melanoma
Many people find out they have melanoma when symptoms prompt them to visit the doctor.
They may be concerned about a mole that is painful, itchy, or bleeding that oozes or becomes scaly or lumpy or that shows other troubling signs.
Doctors looks for evidence of cancer in moles using whats called the ABCDE method:
- A It is asymmetrical.
- B It has an irregular border.
- C It contains more than one color or is an unusual color.
- D Its diameter is unusually big.
- E It evolves, changing size, color, shape, or another characteristic.
These are all traits that distinguish a cancerous mole from a benign one.
Its possible that by the time a physician diagnoses melanoma on the skin, cancer cells have already spread to other parts of the body. Melanoma can also appear in a different part of the body after initial diagnosis and treatment.
People with metastatic melanoma may feel tired or unwell in general. They also may have specific symptoms based on where in the body the cancer cells have spread. Some parts of the body that may be affected by metastatic melanoma include:
What Is Metastatic Melanoma Symptoms Stages And Treatment Of This Rare Disease
Shutterstock
Metastatic melanoma is an advanced form of melanoma, the most dangerous type of skin cancer.
Melanoma begins in skin cells called melanocytes. Melanocytes make a pigment called melanin, which protects skin from the sun. They also produce moles, which are usually harmless but occasionally can become cancerous.
A melanoma can look like a mole. It is usually brown or black but can also be skin-colored, purple, blue, red, pink, or white.
Knowing the difference between a normal mole and a cancerous one, doing regular skin self-exams, and visiting a dermatologist for skin checks on a regular schedule can all be lifesaving.
Also Check: Who Do You See For Skin Cancer Screening
Diagnosis And Management Of Malignant Melanoma
BETH G. GOLDSTEIN, M.D., and ADAM O. GOLDSTEIN, M.D.
University of North Carolina at Chapel Hill School of Medicine, Chapel Hill, North Carolina
Am Fam Physician. 2001 Apr 1 63:1359-1369.
See patient information handout on malignant melanoma, written by the authors of this article.
Malignant melanoma is the eighth most common cancer in the United States and causes 1 to 2 percent of all cancer deaths.1,2 Melanoma is a proliferation of transformed melanocytes or pigment-producing cells. These tumors occur primarily on the skin but may also arise in other tissues where pigment cells are found.
In men, melanomas occur most frequently on the trunk, whereas in women, melanomas occur most frequently on the lower extremities. Melanoma is almost exclusively a disease of adults. In children, melanoma predominantly occurs in the setting of giant congenital nevi or atypical/dysplastic nevus syndrome, or in the setting of xeroderma pigmentosum .
Subtypes Of Melanoma Defined By Gene Mutations
Melanoma cells are usually classified by histologic types , which are based on how the cells appear under a microscope. Recent information has shown that melanoma can also be classified into molecular subtypes. These molecular subtypes are based on the specific genetic changes in the melanoma cells, called mutations. These genetic changes include:
-
BRAF mutations. The most common genetic change in melanoma is found in the BRAF gene, which is mutated in about 50% of cutaneous melanomas.
-
NRAS mutations. NRAS is mutated in the tumors of around 20% of people with melanoma.
-
NF-1 mutations. NF-1 mutations are present in the tumors of around 10% to 15% of people with melanoma.
-
KIT mutations. These mutations occur more commonly in melanomas that develop from mucus membranes, melanomas on the hands or feet, or melanomas that occur in chronically sun-damaged skin, such as lentigo maligna melanoma.
Some melanomas do not have mutations in the BRAF, NRAS, NF-1, or KIT genes. These tumors have other genetic changes that cause them to grow. Researchers are trying to target other mutations found in these tumors in clinical trials.
The classification of melanoma into different subtypes based on genetic changes can have a major effect on the types of treatment used for advanced melanoma. Targeting specific mutated genes is an important way of treating invasive melanoma, called targeted therapy. Learn more about targeted therapy in the Types of Treatment and Latest Research sections.
Recommended Reading: How Does Skin Cancer Occur
Certain Factors Affect Prognosis And Treatment Options
The prognosis and treatment options depend on the following:
- The thickness of the tumor and where it is in the body.
- How quickly the cancer cells are dividing.
- Whether there was bleeding or ulceration of the tumor.
- How much cancer is in the lymph nodes.
- The number of places cancer has spread to in the body.
- The level of lactate dehydrogenase in the blood.
- Whether the cancer has certain mutations in a gene called BRAF.
- The patients age and general health.
Risk Factors Of Melanoma
While there is no one cause of melanoma, skin cancer can be caused by certain environmental and genetic factors. Understanding whether you are at a high risk of melanoma is the first step for preventing adverse outcomes.
These risk factors increase your probability of developing melanoma:
- Excessive UV ray exposure: Constant exposure to UV radiation, whether its from the sun or from tanning beds, can increase your risk of developing melanoma.
- Presence of many or irregular moles: Having many moles on your body puts you at a greater risk for melanoma, especially if these moles look irregular.
- Fair skin: Caucasians and light-skinned individuals are at higher risk for melanoma than darker-skinned individuals. The less melanin you have, the more youre at risk of developing melanoma. Darker-skinned people can still develop melanoma, although cases are relatively low.
- History of sunburns: Increased number of sunburns means an increased risk of melanoma. Sunburns can dampen your skins protective mechanisms and increase the likelihood of mutations.
- Family history or personal history of melanoma: If you or someone in your family has already had melanoma, you are more likely to develop melanoma or get it again.
You May Like: What Does Early Squamous Skin Cancer Look Like
Cancer May Spread From Where It Began To Other Parts Of The Body
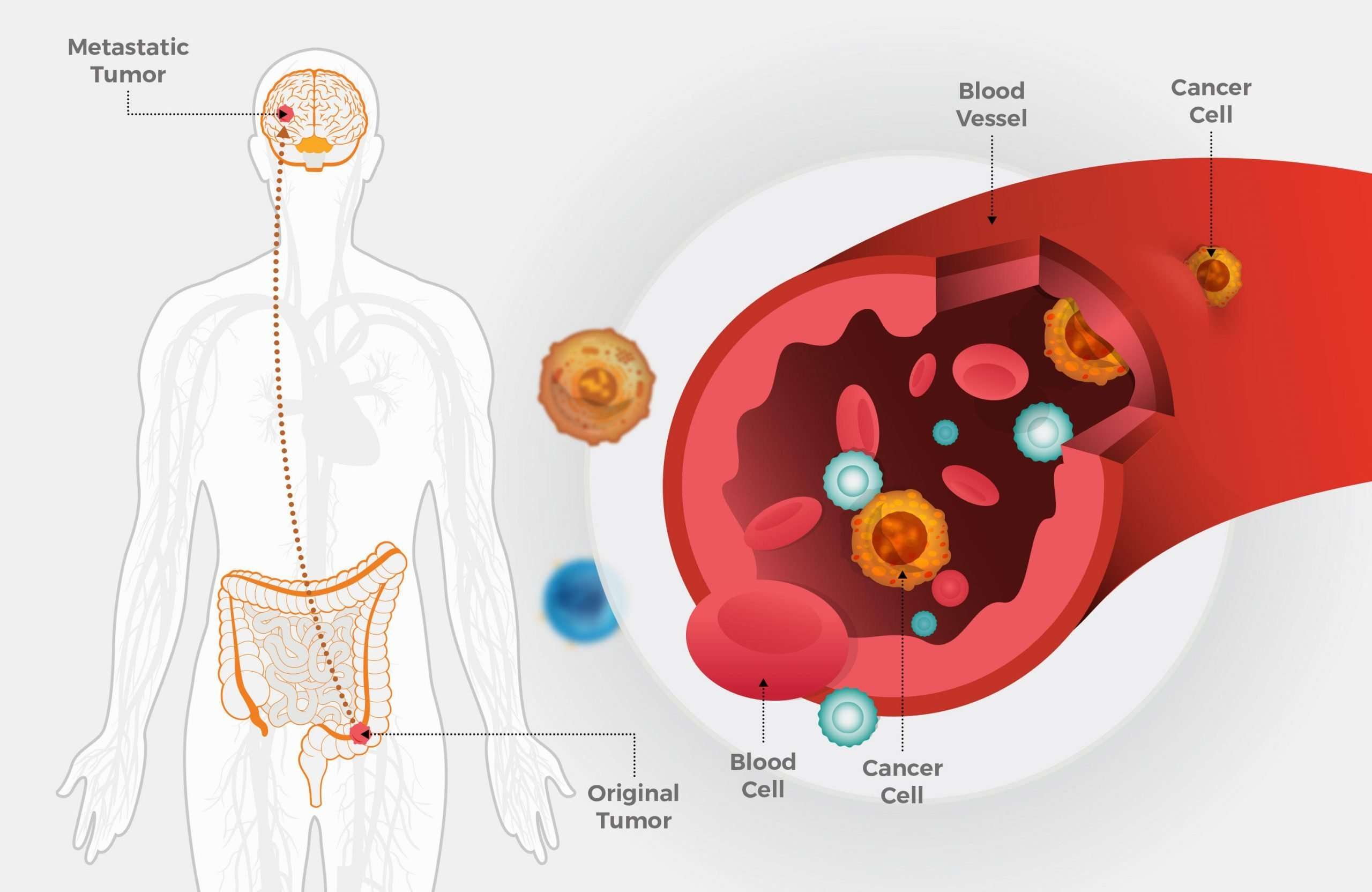
When cancer spreads to another part of the body, it is called metastasis. Cancer cells break away from where they began and travel through the lymph system or blood.
- Lymph system. The cancer gets into the lymph system, travels through the lymph vessels, and forms a tumor in another part of the body.
- Blood. The cancer gets into the blood, travels through the blood vessels, and forms a tumor in another part of the body.
The metastatic tumor is the same type of cancer as the primary tumor. For example, if melanoma spreads to the lung, the cancer cells in the lung are actually melanoma cells. The disease is metastatic melanoma, not lung cancer.
Taking Care Of Yourself
Hearing that your cancer has spread is scary, but a lot of research is underway to find new treatments. And there are treatments available to try to stop the disease from spreading, so you can live longer.
It’s important to have support and to talk about your fears and feelings, too. Your doctor can help you find a cancer support group.
These tips may help you feel better during melanoma treatment:
- If you lose your appetite, eat small amounts of food every 2 to 3 hours instead of bigger meals. A dietitian can give you other tips on nutrition and eating during your cancer treatment. Ask your doctor for a referral.
- Exercise can help you feel better overall and fight fatigue. But listen to your body, and balance rest and activity.
- Get the kind of emotional support that’s right for you. It could be from family, friends, your cancer support group, or a religious group.
Read Also: What Doctor Treats Skin Cancer
The Following Stages Are Used For Melanoma:
Stage 0
Stage I
- Stage IA: The tumor is not more than 1millimeter thick, with or without ulceration.
- Stage IB: The tumor is more than 1 but not more than 2 millimeters thick, without ulceration. Enlarge Stage I melanoma. In stage IA, the tumor is not more than 1 millimeter thick, with or without ulceration . In stage IB, the tumor is more than 1 but not more than 2 millimeters thick, without ulceration. Skin thickness is different on different parts of the body.
Stage II
- Stage IIA: The tumor is either:
- more than 1 but not more than 2 millimeters thick, with ulceration or
- more than 2 but not more than 4 millimeters thick, without ulceration. Enlarge Stage IIA melanoma. The tumor is more than 1 but not more than 2 millimeters thick, with ulceration OR it is more than 2 but not more than 4 millimeters thick, without ulceration. Skin thickness is different on different parts of the body.
Stage III
Stage III is divided into stages IIIA, IIIB, IIIC, and IIID.
Skin Type And Sunburn History
People with a white racial background have at least a 10-fold increase in the incidence of melanoma compared with blacks and a sevenfold increased incidence compared with American Hispanics.8 Sun sensitivity refers to a person’s tendency to sunburn rather than tan. Persons who have a tendency to burn and freckle rather than tan also have an increased melanoma risk. A history of sunburns, even after the age of 20, is associated with an increased risk of melanoma.9 Blue eyes and red or blonde hair color, although useful as indicators of increased melanoma risk, are not as directly related to increased risk as skin type has been shown to be.10
Don’t Miss: Can Basal Cell Carcinoma Cure Itself
There Are Three Ways That Cancer Spreads In The Body
Cancer can spread through tissue, the lymph system, and the blood:
- Tissue. The cancer spreads from where it began by growing into nearby areas.
- Lymph system. The cancer spreads from where it began by getting into the lymph system. The cancer travels through the lymph vessels to other parts of the body.
- Blood. The cancer spreads from where it began by getting into the blood. The cancer travels through the blood vessels to other parts of the body.
Risk Factors For Metastatic Melanomas
You cannot get metastatic melanoma without first having melanoma, though the primary melanoma may be so small its undetectable. Major risk factors for melanomas include:
- Light skin, light-colored hair or light-colored eyes
- Skin prone to burning easily
- Multiple blistering sunburns as a child
- Family history of melanoma
- Frequent exposure to sun or ultraviolet radiation
- Certain genetic mutations
- Exposure to environmental factors, such as radiation or vinyl chloride
Other factors have been connected with increased metastasis. In a 2018 study in the Anais Brasileiros de Dermatologia and a 2019 study in the Journal of the National Cancer Institute, the following factors were associated with higher levels of metastasis:
- Male gender
- Primary tumor thickness of more than 4 mm
- Nodular melanoma, which is a specific subtype that a care team would identify
- Ulceration of the primary tumor
Also Check: How Quickly Can Melanoma Metastasis
Treatment Of Metastatic Melanoma
Metastatic melanomas can be difficult to treat. The five-year survival rate for people diagnosed with melanoma that has spread to nearby lymph nodes is 66 percent, according to the American Cancer Society. When cancer has spread to distant parts of the body, there may also be other metastases too small to detect by scans. For people diagnosed with stage 4 melanoma, or melanoma that has spread to distant parts of the body, the five-year survival rate is 27 percent.
For stage 3 and 4 melanomas, the following treatments may be used:
Multiple therapies can be used at any given time, and your care plan is a dynamic process. You and your care team should discuss all the options and decide on a treatment plan. Each treatment has different side effects, and its important to feel fully informed of all the associated risks. Other medications and options may help manage the symptoms of your cancer treatment, so you can live the highest quality of life possible throughout the course of your treatment and disease.
Expert