Types Of Squamous Cell Carcinoma
There are several types of squamous cell carcinoma. Some are more likely to spread than others, but in general, most share similar characteristics. The primary difference between each subtype is histological .
To determine which type of squamous cell carcinoma a patient has, a pathologist will examine a tissue sample underneath a microscope. By identifying the type of cells that are present in a lesion, an oncologist can tailor a patients treatment plan to achieve the best possible outcome and quality of life.
The primary types of squamous cell carcinoma are:
- Adenoid/pseudoglandular squamous cell carcinoma
- Large cell keratinizing squamous cell carcinoma
- Large cell non-keratinizing squamous cell carcinoma
- Lymphoepithelial carcinoma
- Small cell keratinizing squamous cell carcinoma
- Spindle cell squamous cell carcinoma
- Verrucous squamous-cell carcinoma
At Moffitt Cancer Center, we diagnose and treat a complete range of skin cancers, including the unique variants of squamous cell carcinoma. Screening, staging and long-term follow-up services are also available as part of our commitment to providing comprehensive care.
Referrals are not required to seek a diagnosis or treatment at Moffitt. If youve been diagnosed with or are concerned that you are showing signs of one of the different types of squamous cell carcinoma, call or submit a new patient registration form online.
- BROWSE
What Are The Stages Of Squamous Cell Carcinoma
There are five stages of this form of skin cancer:
Most squamous cell carcinomas show up as Stage 0 or Stage 1.
- Stage 0 Also known as carcinoma in situ, this stage is not considered to be invasive. The abnormal cells are only in the upper layer of the epidermis, the outer skin.
- Stage 1 and Stage 2 Designation in these stages depends on how big the cancer is and if there are any high-risk features in the tumor.
- Stage 3 This stage has spread to areas below the skin, such as into the lymph nodes or other local structures like muscle, bone, or cartilage.
- Stage 4 The cancer has spread to distant sites in this stage.
Dont Miss: Cancer On Arm Pictures
Treatments For Skin Cancer That Spreads Beyond The Skin
When squamous cell carcinoma spreads to other parts of the body, drug treatments might be recommended, including:
- Chemotherapy. Chemotherapy uses powerful drugs to kill cancer cells. If squamous cell carcinoma spreads to the lymph nodes or other parts of the body, chemotherapy can be used alone or in combination with other treatments, such as targeted drug therapy and radiation therapy.
- Targeted drug therapy. Targeted drug treatments focus on specific weaknesses present within cancer cells. By blocking these weaknesses, targeted drug treatments can cause cancer cells to die. Targeted drug therapy is usually combined with chemotherapy.
- Immunotherapy. Immunotherapy is a drug treatment that helps your immune system to fight cancer. Your bodys disease-fighting immune system might not attack cancer because the cancer cells produce proteins that blind the immune system cells. Immunotherapy works by interfering with that process. For squamous cell carcinoma of the skin, immunotherapy might be considered when the cancer is advanced and other treatments arent an option.
Also Check: Merkel Cancer Prognosis
Postoperative And Rehabilitation Care
Preoperative exercises and rehabilitation program has shown significant postoperative outcomes and reduced postoperative pulmonary complications.. However, postoperative pulmonary rehabilitation alone without preoperative exercise showed only a small to moderate effect on postoperative exercise capacity on the short-term follow-up, but the long-term effect on functional capacity is unknown.
What Does Scc Look Like
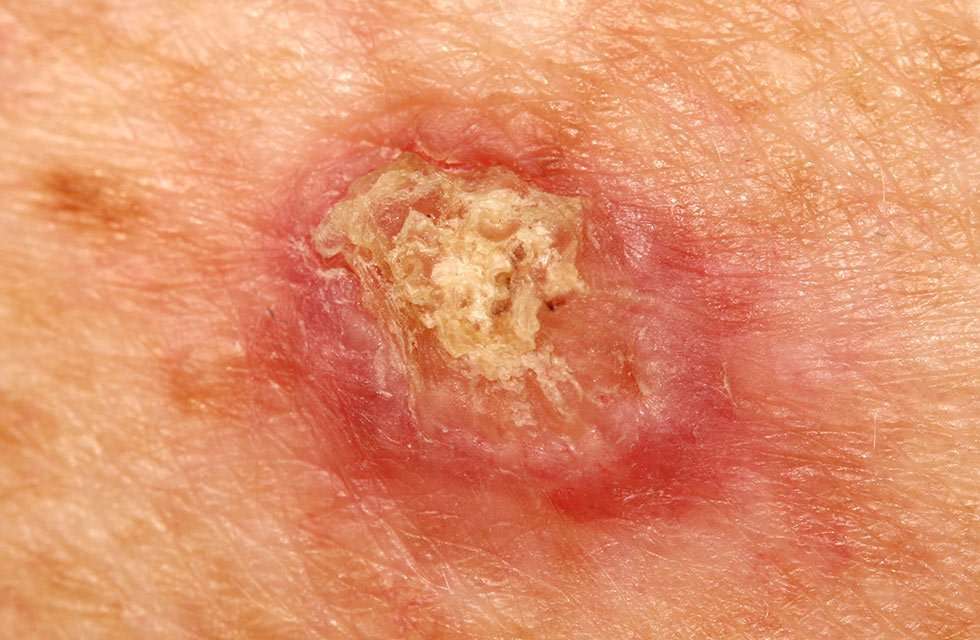
SCCs can appear as scaly red patches, open sores, rough, thickened or wart-like skin, or raised growths with a central depression. At times, SCCs may crust over, itch or bleed. The lesions most commonly arise in sun-exposed areas of the body.
SCCs can also occur in other areas of the body, including the genitals.
SCCs look different on everyone. You can find more images, as well as signs, symptoms and early detection strategies on our SCC Warning Signs page.
Please note: Since not all SCCs have the same appearance, these photos serve as general reference for what they can look like. If you see something new, changing or unusual on your skin, schedule an appointment with your dermatologist.
A persistent, scaly red patch with irregular borders that sometimes crusts or bleeds.
An open sore that bleeds or crusts and persists for weeks.
An elevated growth with a central depression that occasionally bleeds. It may rapidly increase in size.
A wart-like growth that crusts and occasionally bleeds.
Read Also: Well Differentiated
What Is Oral Cancer
Oral cancer starts in the cells of the mouth. A cancerous tumour is a group of cancer cells that can grow into and destroy nearby tissue. It can also spread to other parts of the body. The most common place oral cancer spreads to is the lymph nodes in the neck. Oral cancer may also be called oral cavity cancer or mouth cancer.
Cells in the mouth sometimes change and no longer grow or behave normally. These changes may lead to non-cancerous tumours such as warts and fibromas.
Changes to cells of the mouth can also cause precancerous conditions. This means that the abnormal cells are not yet cancer, but there is a chance that they may become cancer if they arent treated. The most common precancerous conditions of the mouth are leukoplakia and erythroplakia.
But in some cases, changes to the cells of the mouth can cause oral cancer. The mouth is covered by a lining called the oral mucosa . The oral mucosa is made up of squamous cells called the squamous epithelium. Most often, oral cancer starts in these flat, thin squamous cells. This type of cancer is called squamous cell carcinoma of the mouth.
Rare types of oral cancer can also develop. These include and .
What Is The Treatment For Advanced Or Metastatic Squamous Cell Carcinoma
Locally advanced primary, recurrent or metastatic SCC requires multidisciplinary consultation. Often a combination of treatments is used.
- Experimental targeted therapy using epidermal growth factor receptor inhibitors
Many thousands of New Zealanders are treated for cutaneous SCC each year, and more than 100 die from their disease.
Recommended Reading: Lobular Carcinoma Survival Rate
What Are The 5 Stages Of Skin Cancer
Staging is an important tool used to treat skin cancer. Your stage helps the medical team determine where the tumor is, how large it is, where it has spread, your prognosis, and the most effective treatment plan.
The five stages of squamous cell carcinoma include:
- Stage 0: Also known as carcinoma in situ, in this stage cancer is present in the epidermis. It has not spread to deeper layers.
- Stage 1: The tumor is smaller than 2 centimeters and has not spread to nearby lymph nodes or other organs. The individual has one or fewer risk factors for spread.
- Stage 2: The tumor is wider than 2 centimeters and has not spread to nearby lymph nodes or other organs. This stage also applies to any sized tumor when the individual has two or more risk factors.
- Stage 3: The tumor has spread into nearby facial bones or one lymph node. It has not spread to other organs.
- Stage 4: The tumor is of any size and has metastasized to one or more of the lymph nodes. It may have spread to the bones and other distant organs.
How Dangerous Is Scc
While the majority of SCCs can be easily and successfully treated, if allowed to grow, these lesions can become disfiguring, dangerous and even deadly. Untreated SCCs can become invasive, grow into deeper layers of skin and spread to other parts of the body.
Did you know?
Americans die each year from squamous cell carcinoma
You May Like: Well Differentiated Squamous Cell Carcinoma Stages
How Do Dermatologists Diagnose Squamous Cell Carcinoma Of The Skin
Because this cancer begins on the skin, its possible to find it early when its highly treatable.
When you see a board-certified dermatologist, your dermatologist will examine your skin carefully.
If your dermatologist finds a spot on your skin that could be any type of skin cancer, your dermatologist will first numb the area and then remove all of it. This can be done during an office visit and is called a skin biopsy. This is a simple procedure, which a dermatologist can quickly, safely, and easily perform.
Having a skin biopsy is the only way to know for sure whether you have skin cancer.
What your dermatologist removes will be examined under a high-powered microscope. Your dermatologist or a doctor who has in-depth experience diagnosing skin growths, such as a dermatopathologist, is best qualified to examine the removed tissue under a microscope.
After examining the removed tissue, the doctor writes a biopsy report. Also called a pathology report, this report explains what was seen under the microscope, including whether any skin cancer cells were seen.
If you have squamous cell carcinoma of the skin, the report will contain the following information when possible:
-
Type of SCC
-
Whether the cancer has any features that make it aggressive
How Serious Is Invasive Squamous Cell Carcinoma
Skin cancer in general is a slow-developing disease, often taking years to develop, but that does not mean treatment should be delayed. The longer squamous cell carcinoma is ignored, the more time it has to become invasive, potentially burrowing deeper into nearby organs, lymph nodes, and even bones.
Non-melanoma skin cancer is highly treatable when caught early, but the survival rate drops the further the cancer progresses. There are five stages of skin cancer:
- Stage 0: known as carcinoma in situ, this stage means the cancer cells are localized in the topmost layer of the skin
- Stage I: the cancerous area is under 2cm and has not spread
- Stage II: the cancerous area is over 2cm and may have spread to nearby tissue but not lymph nodes
- Stage III: the cancerous area can be any size and has started to spread to lymph nodes
- Stage IV: the cancerous area has become invasive, spreading to other major parts of the body
Delaying squamous cell carcinoma treatment increases risk significantly, so its important to seek medical attention as soon as you notice symptoms.
Don’t Miss: Well Differentiated Carcinoma
Treating Advanced Squamous Cell Cancers
Lymph node dissection:Removing regional lymph nodes might be recommended for some squamous cell cancers that are very large or have grown deeply into the skin, as well as if the lymph nodes feel enlarged and/or hard. The removed lymph nodes are looked at under a microscope to see if they contain cancer cells. Sometimes, radiation therapy might be recommended after surgery.
Immunotherapy: For advanced squamous cell cancers that cant be cured with surgery or radiation therapy, one option might be using an immunotherapy drug such as cemiplimab or pembrolizumab . However, these drugs havent been studied in people with weakened immune systems, such as people who take medicines for autoimmune diseases or who have had an organ transplant, so the balance between benefits and risks for these people isnt clear.
Systemic chemotherapy and/or targeted therapy:Chemotherapy and targeted therapy drugs might be other options for patients with squamous cell cancer that has spread to lymph nodes or distant organs. These types of treatment might be combined or used separately.
Types Of Cutaneous Squamous Cell Carcinoma
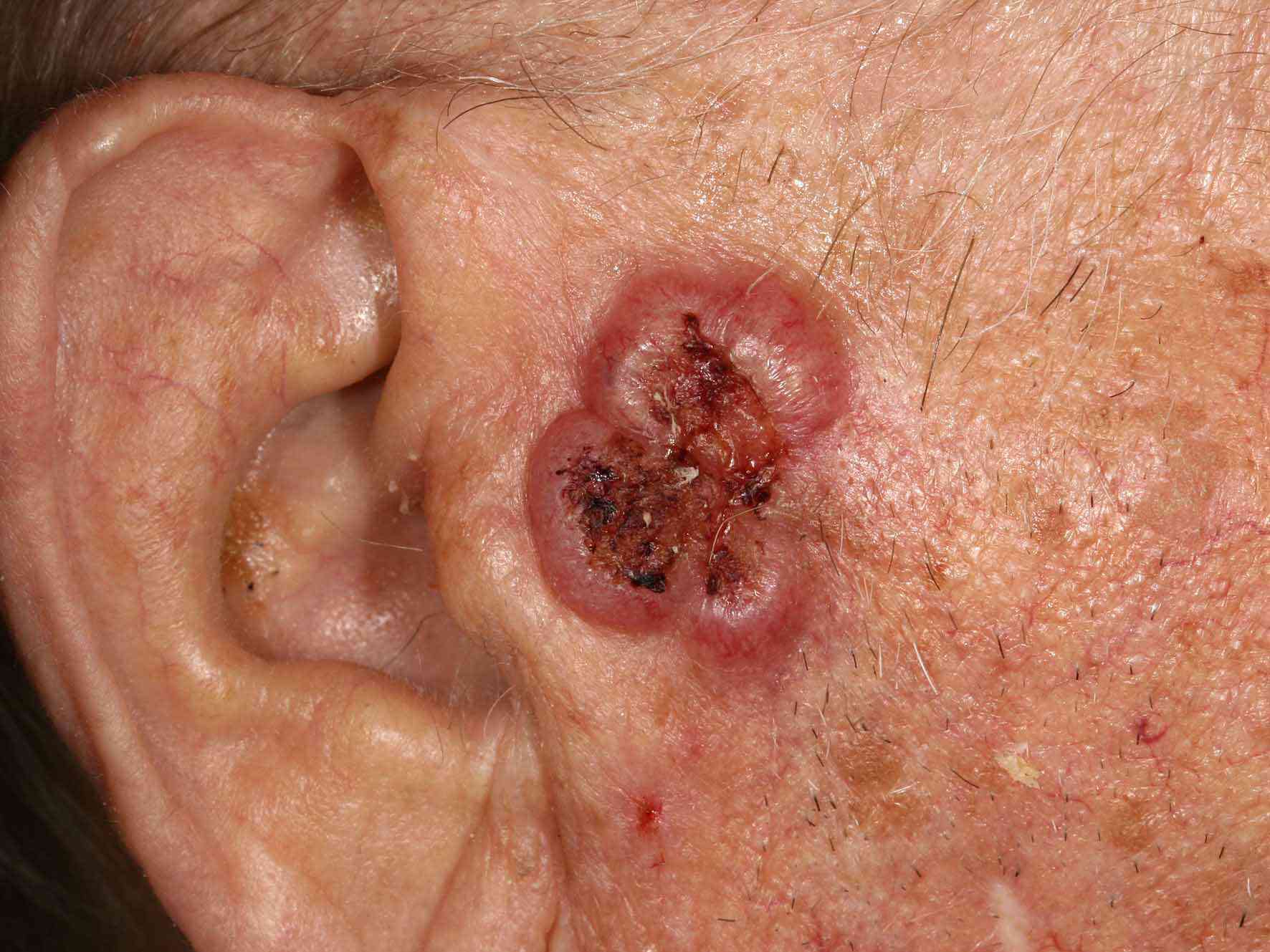
Distinct clinical types of invasive cutaneous SCC include:
- Cutaneous horn the horn is due to excessive production of keratin
- Keratoacanthoma a rapidly growing keratinising nodule that may resolve without treatment
- Carcinoma cuniculatum , a slow-growing, warty tumour on the sole of the foot
- – a cutaneous SCC that has developed in a scar or chronic ulcer
- Multiple eruptive SCC/KA-like lesions arising in syndromes, such as multiple self-healing squamous epitheliomas of Ferguson-Smith and Grzybowski syndrome
The pathologist may classify a tumour as well differentiated, moderately well differentiated, poorly differentiated or anaplastic cutaneous SCC. There are other variants.
Subtypes of cutaneous squamous cell carcinoma
Read Also: What Does Well Differentiated Mean
Squamous Cell Carcinoma Stages
Squamous cell carcinoma stages represent the size of a tumor and how far it has spread. However, squamous cell carcinoma is usually very slow to metastasize most cases are diagnosed while the cancer is still confined to the upper layer of the skin. As a result, these tumors may not be staged if it is clear that the cancer has not invaded nearby tissues at the time of diagnosis.
If a squamous cell carcinoma does require staging, oncologists will evaluate a number of factors, including:
- The size of the tumor
- Whether the tumor has grown into the dermis or subcutis levels of the skin
- Whether the cancer has invaded the bones
- Where on the body the tumor developed
- How the cells appear when viewed under a microscope
- Whether the cancer has spread to lymph nodes or distant organs
After evaluating these factors, the oncologist will assign one of the following squamous cell carcinoma stages to the tumor:
- Stage 0 Cancer is only present on the epidermis .
- Stage 1 Cancer has grown deep into the skin, but has not spread to nearby lymph nodes or healthy tissues.
- Stage 2 Cancer has grown deep into the skin and displays one or more high-risk features , but has not spread to nearby lymph nodes or healthy tissues.
- Stage 3 Cancer has grown into lymph nodes, but has not spread to any organs other than the skin.
- Stage 4 Cancer has spread to one or more distant organs, such as the lungs, liver, brain or distant parts of the skin.
What Are The Signs And Symptoms Of Squamous Cell Carcinoma
SCC signs and symptoms include skin changes like:
- A rough-feeling bump or growth which might then crust over and bleed.
- A growth that is higher than the skin but has a depression in the middle.
- A sore that will not heal, or a sore that heals and then comes back.
- A piece of skin that is flat, is scaly and red.
- A precancerous growth called actinic keratosis, which is a bump or lump that can feel dry, itchy, scaly, or be discolored.
- A precancerous skin lesion called actinic cheilitis, which happens mainly on the lower lip. The tissue becomes pale, dry, and cracked.
- A precancerous condition called leukoplakia, in which white spots develop in the mouth, on the tongue, gums, or cheeks
Recommended Reading: Invasive Ductal Carcinoma Grade 2 Survival Rate
Pertinent Studies And Ongoing Trials
The immunotherapeutic atezolizumab is being evaluated in a phase III clinical trial as a potential first-line treatment for patients with non-squamous or squamous non-small cell lung cancer whose tumors express PDL1. A phase I trial evaluating atezolizumab in combination with erlotinib or alectinib in patients with non-small cell lung cancer is also ongoing. IPA-3 or OTSSP167 and auranofin was highly synergistic in EGFR or KRAS mutant squamous cell carcinoma cell lines and decreased tumor volume in mice models.
What Is Squamous Cell Carcinoma Of The Skin
Squamous cells are found throughout the human body. These cells line organs, such as the lungs, throat, and thyroid. We also have squamous cells in our skin.
The job of squamous cells is to protect what lies beneath. In our skin, these cells sit near the surface, protecting the tissue beneath.
Anywhere we have squamous cells, we can develop a type of cancer called squamous cell carcinoma .
In the skin, this cancer is usually not life-threatening. It tends to grow slowly, but it can grow deep. When the cancer grows deep, it can injure nerves, blood vessels, and anything else in its path. As the cancer cells pile up, a large tumor can form.
Most people who develop this skin cancer have fair skin that they seldom protected with sunscreen or sun-protective clothing. Before developing this skin cancer, they tend to notice signs of sun damage on their skin, such as age spots, patches of discolored skin, and deep wrinkles.
Anyone can develop squamous cell carcinoma
While anyone can develop this skin cancer, you have a greater risk if you live with a transplanted organ, use tanning beds, or have fair skin that you seldom protected from the sun.
Another sign of sun-damaged skin is having one or more pre-cancerous growths on your skin called actinic keratoses . Some AKs progress, turning into squamous cell carcinoma of the skin.
To find out what this skin cancer can look like and see pictures of it, go to: Squamous cell carcinoma of the skin: Signs and symptoms.
ImageGetty Images
Read Also: Metastatic Melanoma Cancer Life Expectancy
Deterrence And Patient Education
Education on avoiding or mitigating against risk factors such as tobacco products and causes of occupational disease can reduce SCC development. Education about early cancer screening with low dose CT scan of the chest is important for early recognization and treatment to prevent tumor burden. Counseling patients about stages of cancers and the chance of complete cure in case of early detection and counseling on palliative care in advanced stages is very important to reduce stress both for patients and loved ones.
What Causes Squamous Cell Cancer
Skin cancer is caused by mutations that occur in skin cell DNA. These changes cause abnormal cells to multiply out of control. When this occurs in the squamous cells, the condition is known as SCC.
UV radiation is the most common cause of the DNA mutations that lead to skin cancer. UV radiation is found in sunlight as well as in tanning lamps and beds.
While frequent exposure to UV radiation greatly increases your risk of skin cancer, the condition can also develop in people who dont spend much time in the sun or in tanning beds.
These people may be genetically predisposed to skin cancer, or they may have weakened immune systems that increase their likelihood of getting skin cancer.
Those who have received radiation treatment may also be at greater risk of skin cancer.
Risk factors for SCC include:
- having fair skin
- having light-colored hair and blue, green, or gray eyes
- having long-term exposure to UV radiation
- living in sunny regions or at a high altitude
- having a history of multiple severe sunburns, especially if they occurred early in life
- having a history of being exposed to chemicals, such as arsenic
Read Also: Invasive Ductal Breast Cancer Survival Rate