Resources For More Information:
Skin Cancer Foundation
Strive to educate the public and medical professionals about the dangers of skin cancer, prevention methods, and sun protection. Provides information on skin cancer and treatment.
Melanoma Research Foundation
Committed to the support of medical research in finding effective treatments, the MRF also educates patients about the prevention, diagnosis and treatment of melanoma. Provides a web based support community as well.
Melanoma International Foundation
Help patients and caregivers understand pathology reports, prognosis, and therapy options, including clinical trials, as well as where to get the best possible care.
Levine A. et al. Introduction to reflectance confocal microscopy and its use in clinical practice. JAAD Case Rep. 2018.
NCCN Guidelines Version 2.2021 Melanoma. Found at: https://www.nccn.org/professionals/physician_gls/pdf/cutaneous_melanoma.pdf
Saranga-Perry V, Ambe C, Zager J & Kudchadkar RR. Recent Developments in the Medical and Surgical Treatment of Melanoma. A Cancer Journal for Clinicians. 64:171-185, 2014 May/June.
Shah GD. Chapman PB. Adjuvant therapy of melanoma. Cancer Journal. 13:217-22, 2007 May-Jun.
Skin Cancer Foundation. Melanoma Treatments. 2019. Found at:
Diagnosis And Staging What It Means For You
How is melanoma diagnosed?
To diagnose melanoma, a dermatologist biopsies the suspicious tissue and sends it to a lab, where a dermatopathologist determines whether cancer cells are present.
After the disease is diagnosed and the type of melanoma is identified, the next step is for your medical team to identify the stage of the disease. This may require additional tests including imaging such as PET scans, CT scans, MRIs and blood tests.
The stage of melanoma is determined by several factors, including how much the cancer has grown, whether the disease has spread and other considerations. Melanoma staging is complex, but crucial. Knowing the stage helps doctors decide how to best treat your disease and predict your chances of recovery.
Carcinoma In Situ Vs Precancerous Cells Vs Dysplasia
There are many terms describing the spectrum of normal cells and invasive cancer cells. One of these is dysplasia. Dysplasia can run the spectrum from mild dysplasia in which the cells are barely abnormal appearing, to carcinoma in situ, which some pathologists describe as severe dysplasia involving the full thickness of the epithelium. The term precancerous cells may also be used to describe cells on this continuum between normal and cancer cells.
These terms are also used in different ways depending on the sample analyzed. For example, cells visualized on a pap smear may show dysplasia , but since the cells are “loose,” nothing can be said about whether carcinoma in situ is present or not. With cervical dysplasia, a biopsy is required before the diagnosis of CIS is made. A biopsy sample provides a view of the cells as they occur in relation to the basement membrane and other cells, and is needed to understand if abnormal cells seen on a pap smear are concerning.
Recommended Reading: Cancer Spread All Over Body
Cdkn2a And Cdk: A Clinical Perspective
To date, several clinical trials are ongoing, attempting to find a way to modulate this pathway . With regard to CDKN2A alterations, drugs on study include: ilorasertib , a potent and ATP-competitive multitargeted kinase inhibitor that inhibits Aurora C, Aurora B, and Aurora A and that suppresses RET tyrosine kinase, PDGFR and Flt1 palbociclib and SHR6390, two selective inhibitor of the cyclin-dependent kinases CDK4 and CDK6.
Phase I trial with ilorasertib showed two clinical responses among 58 treated patients, and confirmed a good tolerability and safety profile of the drug . Palbociclib, together with abemaciclib and ribociclib, have already been approved for the treatment of metastatic breast cancer, after several studies showing their activity in a spectrum of solid tumors including melanoma. Palbociclib is currently under investigation among patients affected by acral melanoma with documented gene aberrations in cell cycle pathways, including CDK4 amplification and/or CCND1 amplification and/or CDKN2A loss. Finally, SHR6390 showed a promising activity in preclinical studies performed on cell lines and human tumor xenograft models.
Considering CDK4/6 alterations, several drugs are being testing.
Ribociclib also showed some activity in melanomas with activating mutations of BRAF or NRAS.
Recurrence In Other Parts Of The Body
Melanoma can also come back in distant parts of the body. Almost any organ can be affected. Most often, the melanoma will come back in the lungs, bones, liver, or brain. Treatment for these recurrences is generally the same as for stage IV melanoma . Melanomas that recur on an arm or leg may be treated with isolated limb perfusion/infusion chemotherapy.
Melanoma that comes back in the brain can be hard to treat. Single tumors can sometimes be removed by surgery. Radiation therapy to the brain may help as well. Systemic treatments might also be tried.
As with other stages of melanoma, people with recurrent melanoma may want to think about taking part in a clinical trial.
The treatment information given here is not official policy of the American Cancer Society and is not intended as medical advice to replace the expertise and judgment of your cancer care team. It is intended to help you and your family make informed decisions, together with your doctor. Your doctor may have reasons for suggesting a treatment plan different from these general treatment options. Don’t hesitate to ask him or her questions about your treatment options.
Also Check: How To Identify Basal Cell Carcinoma
Characteristics Of Stage 0 Melanoma
Stage 0 melanoma is a tumor limited to the epidermis. There are no subgroups for Stage 0 melanoma. In the TNM system , its described as TisN0M0:
- Tis: means Tumorin situ cancer cells are found only in the outer layer of skin , not the second layer of skin
- N0: means melanoma has not spread to the lymph nodes
- M0: means melanoma has not spread to distant sites
Risk: Patients with Stage 0 melanoma are considered at very low risk for local recurrence or for regional and distant metastases.
Is Stage 2 Melanoma Serious
All stages of melanoma are serious, but stage 2 melanoma is when the cancer becomes relatively more serious. When detected in stage 2, the cancerous mole or growth has spread from the epidermis deep into the dermis and potentially into the underlying fat and tissue. In some cases, cancerous cells may have started to spread to other parts of the body. Generally, surgical removal of the growth and surrounding tissue will get rid of the melanoma and generally has a five-year survival rate of 50% to 80%, which means that about 50% to 80% of people with this surgery will still be alive five years later. However, once the disease has spread from the skin to other parts of the body, it may become fatal. That being said, it’s very important to see a doctor if you notice any changes in existing moles or any new skin growths, since the chance for recovery is better the earlier you treat it.
Important: This content reflects information from various individuals and organizations and may offer alternative or opposing points of view. It should not be used for medical advice, diagnosis or treatment. As always, you should consult with your healthcare provider about your specific health needs.
You May Like: What Is The Survival Rate For Invasive Ductal Carcinoma
What Is Melanomain Situ
Melanoma in situ is an early form of primary melanoma in which the malignant cells are confined to the tissue of origin, the epidermis. It is also known as in-situ melanoma and level 1 melanoma.
As melanoma in situ has no associated mortality, early detection of melanoma in an in-situ phase increases survival from melanoma and leads to less morbidity and decreased costs compared to that associated with more advanced melanoma .
Management of melanoma is evolving. For up to date recommendations, refer to Australian Cancer Council Clinical practice guidelines for the diagnosis and management of melanoma.
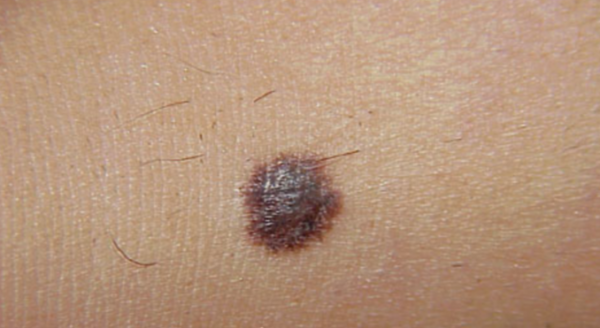
Melanoma in situ
See more images of melanoma in situ.
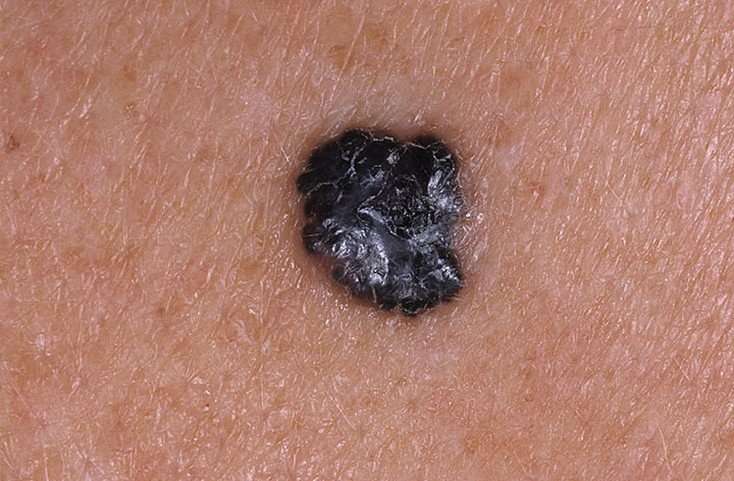
What Is Superficial Spreading Melanoma
Superficial spreading melanoma is the most common type of melanoma, a potentially serious skin cancer that arises from melanocytes along the basal layer of the epidermis.
Superficial spreading melanoma is a form of melanoma in which the malignant cells tend to stay within the epidermis for a prolonged period . At first, superficial spreading melanoma grows horizontally in the skin this is known as the radial growth phase, presenting as a slowly-enlarging flat area of discoloured skin.
An unknown proportion of superficial spreading melanoma become invasive, that is, the melanoma cells cross the basement membrane between the epidermis and dermis and malignant melanocytes enter the dermis. A rapidly-growing nodular melanoma can arise within superficial spreading melanoma and proliferate deeply within the skin.
Management of melanoma is evolving. For up to date recommendations, refer to Australian Cancer Council Clinical practice guidelines for the diagnosis and management of melanoma.
Also Check: What Are The Forms Of Skin Cancer
Squamous Cell Carcinoma Treatment
Squamous cell carcinomas detected at an early stage and removed promptly are almost always curable and cause minimal damage. However, left untreated, they may grow to the point of being very difficult to treat.
A small percentage may even metastasize to distant tissues and organs. Your doctor can help you determine if a particular SCC is at increased risk for metastasis and may need treatment beyond simple excision.
Fortunately, there are several effective ways to treat squamous cell carcinoma. The choice of treatment is based on the type, size, location, and depth of penetration of the tumor, as well as the patients age and general health. Squamous cell carcinoma treatment can almost always be performed on an outpatient basis.
What Is The Outcome For Melanoma In Situ
Patients with melanoma in situ have the same life expectancy as the general population. Further problems are rare from melanoma in situ because the malignant cells within the epidermis have no metastatic potential. However, a small focus of invasive disease may have beeen missed due to the impracticability of evaluating every part of a large skin lesion.
Melanoma in situ occasionally recurs at the same site, requiring further surgery.
Recommended Reading: What Is The Survival Rate For Invasive Ductal Carcinoma
What Are The Complications Of Melanoma In Situ
Untreated, melanoma in situ slowly enlarges. Some in-situ melanomasdevelop foci or a more potentially dangerous, invasive form of melanoma.
- It is thought that less than 5% of lentigo maligna and lentiginous melanoma transform into invasive melanoma.
- The risk of melanoma in situ evolving into invasive melanoma over time is greater in superficial spreading melanoma, acral lentiginous melanoma and other forms of melanoma, but the exact risk is unknown.
Carcinoma In Situ Vs Cancer
A million-dollar question lately, especially with controversy over the treatment of ductal carcinoma in situ or in situ breast cancer, is whether or not carcinoma in situ is really cancer. The answer is that it depends on who you talk to. Some physicians classify carcinoma in situ as non-invasive cancer and others may prefer calling it pre-cancer. The distinction would lie in knowing whether or not the CIS would progress to invasive cancer, and that, by definition, is not known. Nor are we apt to get answers soon, as it wouldn’t be ethical to simply watch large numbers of carcinoma in situ’s to see if they became invasive cancer and spread.
Read Also: Invasive Ductal Carcinoma Grade 3 Survival Rate
What Are The Melanoma Stages And What Do They Mean
Early melanomas
Stage 0 and I are localized, meaning they have not spread.
- Stage 0: Melanoma is localized in the outermost layer of skin and has not advanced deeper. This noninvasive stage is also called melanoma in situ.
- Stage I: The cancer is smaller than 1 mm in Breslow depth, and may or may not be ulcerated. It is localized but invasive, meaning that it has penetrated beneath the top layer into the next layer of skin. Invasive tumors considered stage IA are classified as early and thin if they are not ulcerated and measure less than 0.8 mm.
Find out about treatment options for early melanomas.
Intermediate or high-risk melanomas
Localized but larger tumors may have other traits such as ulceration that put them at high risk of spreading.
- Stage II: Intermediate, high-risk melanomas are tumors deeper than 1 mm that may or may not be ulcerated. Although they are not yet known to have advanced beyond the primary tumor, the risk of spreading is high, and physicians may recommend a sentinel lymph node biopsy to verify whether melanoma cells have spread to the local lymph nodes. Thicker melanomas, greater than 4.0 mm, have a very high risk of spreading, and any ulceration can move the disease into a higher subcategory of stage II. Because of that risk, the doctor may recommend more aggressive treatment.
Learn more about sentinel lymph node biopsy and melanoma treatment options.
Advanced melanomas
Wide Local Excision For Treatment Of Melanoma
If melanoma is caught early, it is highly treatable. Surgery with wide local excision is the main treatment for early melanomas and may be used as part of the treatment approach for advanced melanomas.
Depending on the depth of the melanoma , the margin of normal tissue surrounding the abnormal lesion varies. This is done after the diagnosis is made. This helps reduce the risk of the cancer returning at the primary site.
Read Also: Lobular Breast Cancer Stage 1
Sentinel Lymph Node Biopsy
SLNB is performed to determine whether any cancer cells have spread to the sentinel node, the first lymph node to receive drainage from the primary tumor, and the site where melanomas commonly spread to first. Sentinel lymph node biopsy is recommended for all Stage II tumors regardless of size.
SLNB is most accurate when the lymph channels around the primary melanoma have not been disturbed by a prior wide local excision. Therefore, in most cases, if you are having an SLNB, your SLNB and wide local excision are performed in succession, with the SLNB performed first.
Further treatment will depend on whether the lymph node biopsy is positive.
Box 1 Modelling Melanoma In Vitro And In Vivo
Traditional 2D cell culture and 3D organoid approaches that incorporate microenvironmental elements allow for investigations of melanoma proliferation following various environmental and therapuetic conditions. Spheroid, skin reconstruct, and endothelial trans-membrane models enable in vitro study of migration, invasive, and metastatic dynamics. The limitations of the above models rests on their ex vivo nature. Tail vein injection and spontaneous metastasis models are in vivo approaches that allow inspection of micro- and macrometastases in target organs . Sphere, organoid, PDX, and xenograft models of melanoma allow for delineation of cellular heterogeneity and plasticity of melanoma cells that only recently can be unbiasedly characterized by scRNAseq and barcoding approaches, however, limitations lie in the absence of an immune system. Co-culture approaches incorporating stromal, endothelial, and immune cell types help overcome this limitation. GEMM, immune- humanized, and autologous adoptive T-cell models currently represent the best approaches to investigate immune dynamics in response to therapy. Limitations for the GEMM and immune-humanized models lie in the lack of human cells and an autologous immune system, respectively. The isolation and expansion of tumor infiltrating leukocytes along with tumor from the same patient tumor material for autologous models is a challenging accomplishment.
You May Like: Can You Die From Basal Cell Skin Cancer
Current Nccn Recommendations For Wide Local Excision
After the primary tumor is removed, the skin area excision is closed with stitches or sometimes a skin graft is needed to cover the site. This can be done either in the clinic or in the operating room. The tissue removed is sent to pathology for examination and a report is usually complete in 5-7 days.
| Breslow Thickness |
|---|
What Is The Follow
Most patients with melanoma in situ will be advised to have follow-up examinations with their specialist or general practitioner. The main focus will be a total body skin examination, because patients with a melanoma in situ have eight times the risk of developing another in-situ or invasive primary melanoma compared to matched individuals without melanoma in situ.
Recommended Reading: Does Amelanotic Melanoma Blanch When Pressed
Carcinoma In Situ Vs Invasive Carcinoma
In contrast to carcinoma, or invasive cancer, carcinoma in situ has not yet invaded the basement membrane, and there is no stromal invasion. Other than thisthe fact that the cells have not yet broken through the supporting structure from which they beganthe cells appear the same as invasive cancer cells would appear under the microscope.
How Is Melanoma In Situ Treated
Melanoma in situ is treated by excision biopsy. A special tissue-sparing technique may be used for a large melanoma in situ, such as Mohs micrographic surgery or staged mapped excisions .
When surgical margins are narrow, a second surgical procedure is undertaken, including a 510mm clinical margin of normal skin, to ensure complete removal of the melanoma. This is known as wide local excision.
Non-surgical options may be considered in selected cases of melanoma in situ where surgery is contraindicated, including imiquimod cream , intralesional interferon-alpha, radiation therapy, and laser therapy. Recurrence rates are high with these second-line treatments.
You May Like: How To Identify Basal Cell Carcinoma
Squamous Cell Carcinoma Stages
There are certain features that are considered to make the cancer at higher risk for spreading or recurrence, and these may also be used to stage squamous cell carcinomas. These include:
- Greater than 2 mm in thickness
- Invasion into the lower dermis or subcutis layers of the skin
- Invasion into the tiny nerves in the skin
- Location on the ear or on a hair-bearing lip
After the TNM components and risk factors have been established, the cancer is assigned to one of the five squamous cell carcinoma stages, which are labeled 0 to 4. The characteristics and stages of squamous cell cancer are:
Stage 0: Also called carcinoma in situ, cancer discovered in this stage is only present in the epidermis and has not spread deeper to the dermis.
Stage 1 squamous cell carcinoma: The cancer is less than 2 centimeters, about 4/5 of an inch across, has not spread to nearby lymph nodes or organs, and has one or fewer high-risk features.
Stage 2 squamous cell carcinoma: The cancer is larger than 2 centimeters across, and has not spread to nearby organs or lymph nodes, or a tumor of any size with 2 or more high risk features.
Stage 3 squamous cell carcinoma: The cancer has spread into facial bones or 1 nearby lymph node, but not to other organs.
Stage 4 squamous cell carcinoma: The cancer can be any size and has spread to 1 or more lymph nodes which are larger than 3 cm and may have spread to bones or other organs in the body.