Melanoma Treatment Health Professional Version
On This Page
Melanoma is a malignant tumor of melanocytes, which are the cells that make the pigment melanin and are derived from the neural crest. Although most melanomas arise in the skin, they may also arise from mucosal surfaces or at other sites to which neural crest cells migrate, including the uveal tract. Uveal melanomas differ significantly from cutaneous melanoma in incidence, prognostic factors, molecular characteristics, and treatment.
Prevalence Of Malignant Melanoma In Brown Bullhead From
Raised black lesions observed in 30 percent of the brown bullhead collected from two sites in Lake Memphremagog from 2014 through 2017 were identified microscopically as malignant melanoma. Malignant melanoma in freshwater fishes has been reported before, but this cancer occurrence cluster is raising questions about the cause of the tumors and the
Where Are Nodular Melanoma Growths Found
The most common growth sites for nodular melanoma are the neck, head, and trunk of the body. Unlike some other types of skin cancer, nodular melanomas typically begin as a new growth, rather than developing within a preexisting mole.
It can take as little as 3 months for this type of cancer to spread internally. Nodular melanoma can quickly progress to an advanced stage. Advanced stages of nodular melanoma are more difficult to treat than earlier stages of the disease.
Also Check: Life Expectancy Metastatic Melanoma
How Nodular Melanoma Is Treated
If found early, nodular melanoma can usually be treated and oftentimes cured. However, because of this type of cancers fast-growing nature, it is often only discovered once the condition is advanced.
Nodular melanoma is an aggressive form of skin cancer that grows faster than other kinds of melanoma.
Treatment is focused on curing cancer, preserving skin appearance, and preventing cancer from returning. Treatment options may include surgery, chemotherapy, immunotherapy, radiation therapy, and targeted therapy.
Learn more about the different kinds of treatment for nodular melanoma.
Treatment For Nodular Melanoma
Nodular melanoma is highly curable when diagnosed early. However, because nodular melanoma grows so quickly, it is often found at a more advanced stage. The goals for treatment of nodular melanoma are to:
- cure the cancer
- preserve the appearance of your skin
- prevent the cancer from coming back
The extent and depth of the melanoma guides your care plan. Treatment often involves surgery to remove the melanoma. If the melanoma is more advanced and has spread to other parts of the body, such as the lymph nodes or internal organs, then immunotherapy, targeted therapy, chemotherapy, radiation, surgery, or a combination of therapies may be used to shrink the tumor.
Don’t Miss: What Is The Survival Rate For Invasive Ductal Carcinoma
What Is The Clark Level Of Invasion
The Clark level indicates the anatomic plane of invasion.
| Level | |
|---|---|
| Melanoma has invaded the reticular dermis | |
| Level 5 | Melanoma has invaded subcutaneous tissue |
The deeper the Clark level, the greater the risk of metastasis . It is useful in predicting outcome in thin tumours and less useful for thicker ones in comparison to the value of the Breslow thickness.
Tests For Melanoma Skin Cancer
Biopsies of melanoma that may have spread. Biopsies of areas other than the skin may be needed in some cases. For example, if melanoma has already been diagnosed on the skin, nearby lymph nodes may be biopsied to see if the cancer has spread to them. Rarely, biopsies may be needed to figure out what type of cancer someone has.
You May Like: What Is The Survival Rate For Invasive Ductal Carcinoma
What Are The Risk Factors For Nodular Melanoma
Anyone who has skin that burns easily is more likely to get nodular melanoma. Moreover, it is also seen more often in men and in people who have already had another type of melanoma. If you are a person who has numerous moles, then there is a chance for nodular melanoma to grow in your body.
People with the following factors may also face an increased risk of having nodular melanoma:
- Previous history of having melanoma
- Having many moles
- Having one or more moles that do not look like normal moles in the body
- Fair skin
- The normal tissue around the melanoma
- Measure of how speedily the cells are increasing or growing
- Growth patterns and type of cells
- Inflammatory response
Treatment By Stage Of Melanoma
Different treatments may be recommended for each stage of melanoma. General descriptions by stage are below. Your doctor will recommend a specific treatment plan for you based on the stage and other factors. Detailed descriptions of each type of treatment are provided earlier on this page. Clinical trials may also be a treatment option for each stage.
Stage 0 melanoma
Stage 0 melanoma is almost always treated with surgery alone, usually a wide excision.
Stage I melanoma
Stage I melanoma is usually treated with surgical removal of the tumor and some of the healthy tissue around it. The doctor may recommend lymph node mapping, and some lymph nodes may be removed.
Stage II melanoma
The standard treatment for stage II melanoma is surgery to remove the tumor and some of the healthy tissue around it. While this surgery is being done, lymph node mapping and sentinel lymph node biopsy may also be done. In some people with stage II melanoma, treatment with interferon may be recommended after surgery to lower the chances of the cancer coming back. Treatment in a clinical trial for stage II melanoma may also be an option. Ask your doctor about what clinical trials may be available for you.
Stage III melanoma that can be removed with surgery
Advanced melanoma
-
The persons age and overall health
-
The locations and number of metastases
-
How fast the disease is spreading
-
The presence of specific genetic mutations in the tumor
-
The patients preferences
Treating brain metastases
Don’t Miss: Skin Cancer Perineural Invasion
How Does A Doctor Know The Stage Of A Patient’s Melanoma
When your dermatologist found a spot on your skin that looked like a skin cancer, your dermatologist performed a skin biopsy. This involved giving you an injection to numb the area and then removing all the spot.
The skin that your dermatologist removed was then sent to a lab, where another doctor looked at it under a microscope. This doctor saw melanoma cells.
When a doctor, who is either a dermatopathologist or pathologist, sees melanoma cells, this doctor also tries to determine the stage of the melanoma. When its possible to figure out the stage, the doctor includes this information in your biopsy report. This is a report that the doctor writes and sends to your dermatologist. It explains what the doctor saw under the microscope.
Because the doctor sees only the skin that your dermatologist removed, your dermatologist also uses the findings from your complete skin exam and physical to help determine the stage of the melanoma.
Sometimes, more information is needed to determine the stage.
Metastatic Malignant Melanoma: A Case Study
During melanoma follow-up, patients are clinically monitored to detect a relapse and to recognize additional skin tumors, especially a second melanoma, as early as possible. 8% of all melanoma patients develop a secondary melanoma within 2 years of their initial diagnosis. Melanoma patients also have increased risks for other skin tumors.
You May Like: Small Blue Cell Tumor Prognosis
Treatment Option Overview For Melanoma
| Stage | Standard Treatment Optionsa |
|---|---|
| aClinical trials are an important option for patients with all stages of melanoma because advances in understanding the aberrant molecular and biologic pathways have led to rapid drug development. Standard treatment options are available in many clinical trials. Information about ongoing clinical trials is available from the NCI website. | |
| Stage 0 melanoma | |
| Palliative local therapy |
Stage Information For Melanoma
Clinical staging is based on whether the tumor has spread to regional lymph nodes or distant sites. For melanoma that is clinically confined to the primary site, the chance of lymph node or systemic metastases increases as the thickness and depth of local invasion increases, which worsens the prognosis. Melanoma can spread by local extension and/or by hematogenous routes to distant sites. Any organ may be involved by metastases, but lungs and liver are common sites.
The microstage of malignant melanoma is determined on histologic examination by the vertical thickness of the lesion in millimeters and/or the anatomic level of local invasion . The Breslow thickness is more reproducible and more accurately predicts subsequent behavior of malignant melanoma in lesions thicker than 1.5 mm and should always be reported.
Accurate microstaging of the primary tumor requires careful histologic evaluation of the entire specimen by an experienced pathologist.
Don’t Miss: Stage 4 Basal Cell Carcinoma Life Expectancy
What If The Skin Changes Are Rapid Or Dramatic
Guideline # 4: The more rapid and dramatic the change, the less serious the problem.
When changes such as pain, swelling, or even bleeding come on rapidly, within a day or two, they are likely to be caused by minor trauma, often a kind one doesn’t remember . If a spot changes rapidly and then goes back to the way it was within a couple of weeks, or falls off altogether, it is not likely to represent anything serious. Nevertheless, this would be a good time to say once again: Nobody can diagnose him- or herself. If one sees a spot that looks as though it is new or changing, show it to a doctor. If one see a spot that doesn’t look like one’s other spots, it should be evaluated.
Signs And Symptoms Of Melanoma
The most common sign of melanoma is the appearance of a new mole or a change in an existing mole.
This can happen anywhere on the body, but the most commonly affected areas are the back in men and the legs in women.
Melanomas are uncommon in areas that are protected from sun exposure, such as the buttocks and the scalp.
In most cases, melanomas have an irregular shape and are more than 1 colour.
The mole may also be larger than normal and can sometimes be itchy or bleed.
Look out for a mole that gradually changes shape, size or colour.
Superficial spreading melanoma are the most common type of melanoma in the UK.
They’re more common in people with pale skin and freckles, and much less common in people with darker skin.
They initially tend to grow outwards rather than downwards, so they do not pose a problem.
But if they grow downwards into the deeper layers of skin, they can spread to other parts of the body.
You should see a GP if you have a mole that’s getting bigger, particularly if it has an irregular edge.
Read Also: Does Melanoma Blanch When Pressed
Diagnostic Excision Of A Lesion Suspicious Of Nodular Melanoma
If the skin lesion is suspected to be a nodular melanoma, it should be urgently cut out . A small biopsy is best avoided, except in unusually large lesions. An incisional or punch biopsy could be misleading.
The pathological diagnosis of melanoma can be challenging. Nodular melanomas have little or no spread of malignant cells within the epidermis the melanoma cells are found within the dermis or subcutaneous fat. Extra tests using immunohistochemical stains may be necessary.
What Are The Symptoms Of Nodular Melanoma
Most skin cancer screening guidelines tell you to check for the ABCDE symptoms of skin cancer. But there are additional warning signs that can alert you to possible nodular melanoma.
Also, unlike some other types of skin cancer, nodular melanomas typically begin as a new growth, rather than developing within a preexisting mole.
Don’t Miss: Stage 2 Invasive Ductal Carcinoma Survival Rate
Surgical Removal Of Melanomas
Superficial melanoma can be removed with a surgery called a wide excision. This can be done with local anesthesia . Usually, it is done as a surgery under general anesthesia . If you are having surgery, your nurse will give you the resource Getting Ready for Surgery to help prepare you for it.
In a wide excision, your doctor will remove the melanoma and some healthy skin around it to make sure they get all of the cancer. This tissue will be sent to a pathologist to determine the type of tumor that you have. A pathologist is a doctor who looks at body tissue under a microscope to diagnose disease. The surgical site will closed with sutures . They are removed about a week after your surgery. Certain sutures dissolve on their own. Some people may also have reconstruction if the wound is large. See the Reconstruction of your wound site section for more information.
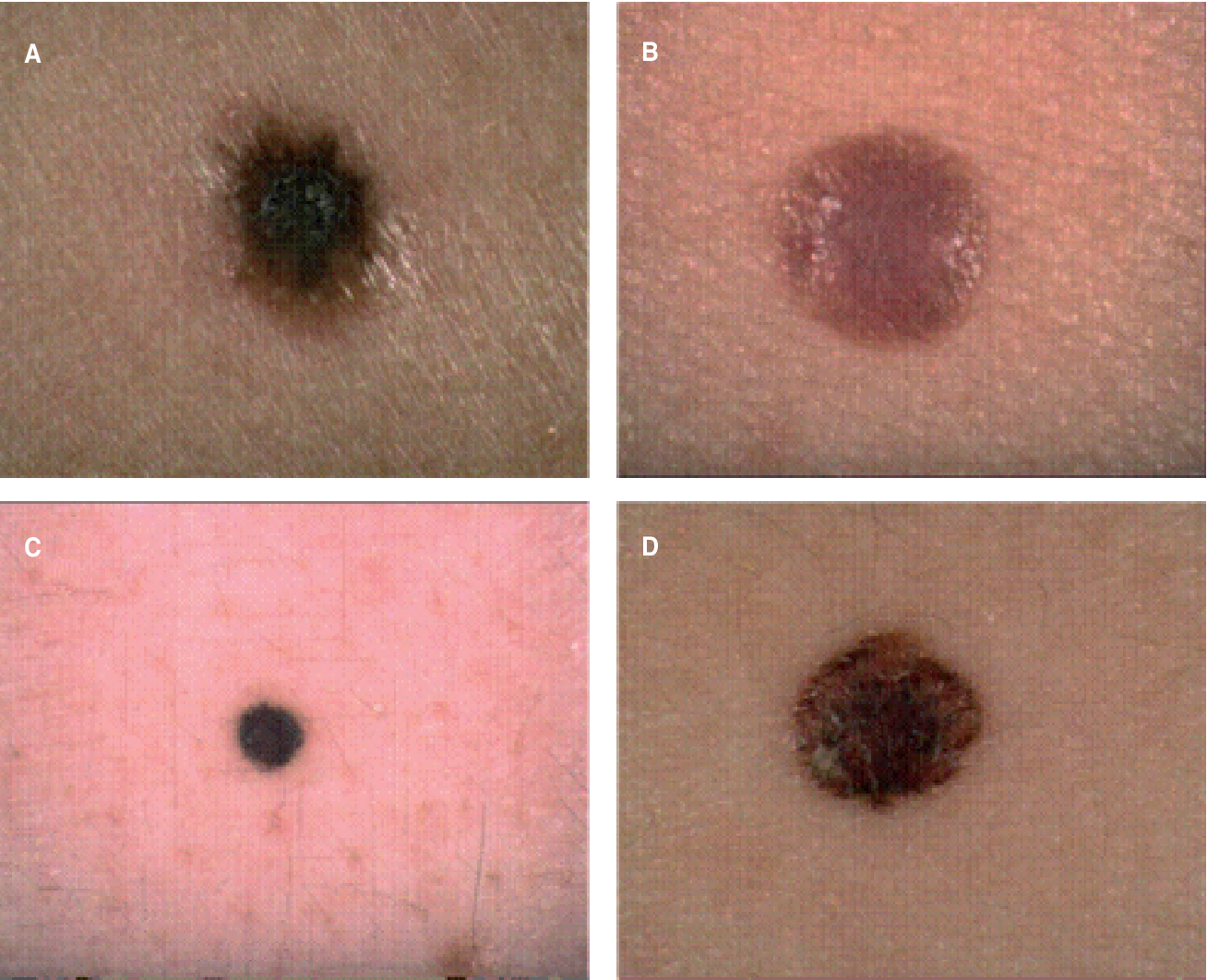
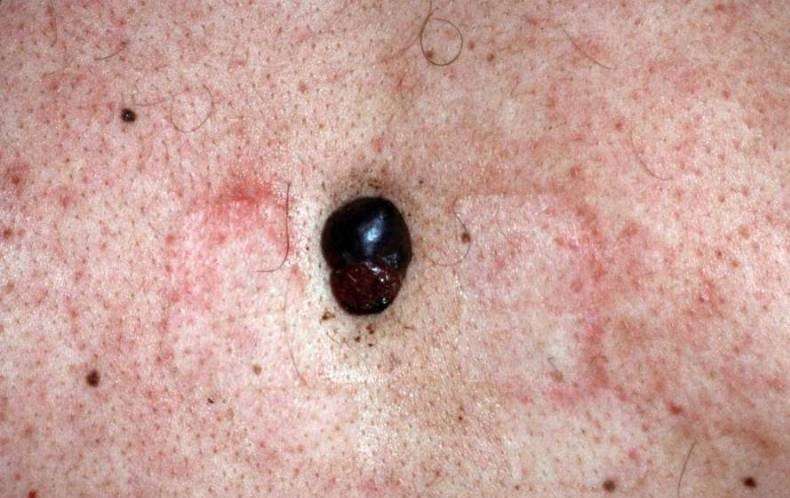
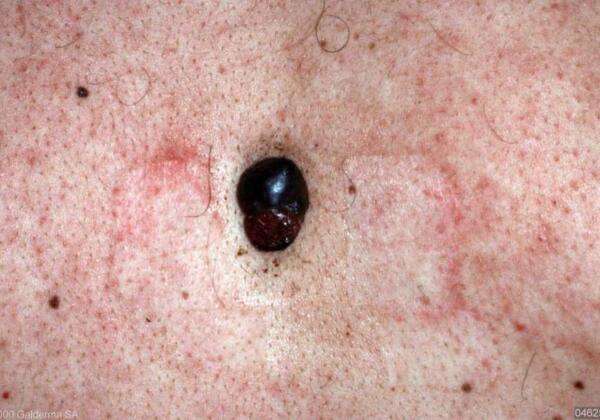
What Does Nodular Melanoma Look Like
Nodular melanoma may arise on any site but is most common on exposed areas of the head and neck.
Nodular melanoma presents as a rapidly enlarging lump . The characteristics of nodular melanoma include:
- Larger size than most moles > 6 mm and often a centimetre or more in diameter at diagnosis
- Dome-shaped, often symmetrical firm lump
- Single colour or variable pigmentation most often black, red or skin coloured
- Smooth, rough, crusted or warty surface
- Ulceration or bleeding
- Itching or stinging
One-third of nodular melanomas are not pigmented. They lack the ABCDE criteria melanoma warning signs. .
Nodular melanoma
Read Also: What Is Stage 2 Squamous Cell Carcinoma
The Stage Of Melanoma Depends On The Thickness Of The Tumor Whether Cancer Has Spread To Lymph Nodes Or Other Parts Of The Body And Other Factors
To find out the stage of melanoma, the tumor is completely removed and nearby lymph nodes are checked for signs of cancer. The stage of the cancer is used to determine which treatment is best. Check with your doctor to find out which stage of cancer you have.
The stage of melanoma depends on the following:
- The thickness of the tumor. The thickness of the tumor is measured from the surface of the skin to the deepest part of the tumor.
- Whether there are:
- Satellite tumors: Small groups of tumor cells that have spread within 2 centimeters of the primary tumor.
- Microsatellite tumors: Small groups of tumor cells that have spread to an area right beside or below the primary tumor.
- In-transit metastases: Tumors that have spread to lymph vessels in the skin more than 2 centimeters away from the primary tumor, but not to the lymph nodes.
What Are The Melanoma Stages And What Do They Mean
Early melanomas
Stage 0 and I are localized, meaning they have not spread.
- Stage 0: Melanoma is localized in the outermost layer of skin and has not advanced deeper. This noninvasive stage is also called melanoma in situ.
- Stage I: The cancer is smaller than 1 mm in Breslow depth, and may or may not be ulcerated. It is localized but invasive, meaning that it has penetrated beneath the top layer into the next layer of skin. Invasive tumors considered stage IA are classified as early and thin if they are not ulcerated and measure less than 0.8 mm.
Find out about treatment options for early melanomas.
Intermediate or high-risk melanomas
Localized but larger tumors may have other traits such as ulceration that put them at high risk of spreading.
- Stage II: Intermediate, high-risk melanomas are tumors deeper than 1 mm that may or may not be ulcerated. Although they are not yet known to have advanced beyond the primary tumor, the risk of spreading is high, and physicians may recommend a sentinel lymph node biopsy to verify whether melanoma cells have spread to the local lymph nodes. Thicker melanomas, greater than 4.0 mm, have a very high risk of spreading, and any ulceration can move the disease into a higher subcategory of stage II. Because of that risk, the doctor may recommend more aggressive treatment.
Learn more about sentinel lymph node biopsy and melanoma treatment options.
Advanced melanomas
Also Check: Melanoma Bone Cancer Life Expectancy
Treating Stage Iii Melanoma
These cancers have already reached the lymph nodes when the melanoma is first diagnosed. Surgical treatment for stage III melanoma usually requires wide excision of the primary tumor as in earlier stages, along with lymph node dissection.
After surgery, adjuvant treatment with an immune checkpoint inhibitor or with targeted therapy drugs may help lower the risk of the melanoma coming back. Other drugs or perhaps vaccines may also be recommended as part of a clinical trial to try to reduce the chance the melanoma will come back. Another option is to give radiation therapy to the areas where the lymph nodes were removed, especially if many of the nodes contain cancer.
If melanoma tumors are found in nearby lymph vessels in or just under the skin , they should all be removed, if possible. Other options include injections of the T-VEC vaccine , Bacille Calmette-Guerin vaccine, or interleukin-2 directly into the melanoma radiation therapy or applying imiquimod cream. For melanomas on an arm or leg, another option might be isolated limb perfusion or isolated limb infusion . Other possible treatments might include targeted therapy , immunotherapy, or chemotherapy.
Some people with stage III melanoma might not be cured with current treatments, so they may want to think about taking part in a clinical trial of newer treatments.
How Do Dermatologists Diagnose Melanoma
When you see a board-certified dermatologist, your dermatologist will:
-
Examine your skin carefully
-
Ask questions about your health, medications, and symptoms
-
Want to know if melanoma runs in your family
If any spot on your skin looks like skin cancer, your dermatologist will first numb the area and then remove all of it. This can be done during an office visit and is called a skin biopsy. This is a simple procedure, which a dermatologist can quickly, safely, and easily perform.
Having a skin biopsy is the only way to know for sure whether you have skin cancer.
The tissue that your dermatologist removes will be sent to a lab, where a doctor, such as a dermatopathologist, will examine it under a high-powered microscope. The doctor is looking for cancer cells.
What this doctor sees while looking at your tissue will be explained in the pathology report, including whether cancer cells were seen. If melanoma cells are seen, the report will include many important details, including:
-
The type of melanoma
-
How deeply the melanoma tumor has grown into the skin
-
How quickly the melanoma cells are growing and dividing
If its possible to tell the stage of the melanoma, the report will include this information.
Stages of melanoma
Heres an explanation of what each stage of melanoma means:
Stages of melanoma
Stage 0
The melanoma has spread to either: One or more nearby lymph node Nearby skin
Once the stage is known, the next step is treatment.
Don’t Miss: Melanoma Stage 3 Survival Rate