Outstanding Issues That Warrant Research
The radiologic discrimination of benign, indolent and aggressive malignant renal masses remains the diagnostic challenge of high clinical relevance. The current need for tissue-based diagnosis and prevalent treatment pattern of nearly non-discriminatory extirpation encourage key areas for research in imaging evaluation of the small renal mass. These key areas include reliable diagnosis of the most common benign lesions, and ability to predict tumor aggressiveness in malignancies. Positive findings in these areas have been reported in relatively small studies with highly variable imaging techniques, limiting application of the evidence at this time. The incremental value of recently developed quantitative techniques, such as diffusion-weighted imaging including intravoxel incoherent motion, or arterial spin labeling , warrant larger studies as morphologic characteristics and quantitative assessment derived from conventional imaging have been well-studied and have not performed reliably in distinguishing benign and malignant tumors. Larger, multi-institutional studies would better establish the performance of CT and MRI and address these questions of high clinical relevance.
Medical History And Physical Exam
If you have any signs or symptoms that suggest you might have kidney cancer, your doctor will want to take your complete medical history to check for risk factors and to learn more about your symptoms.
A physical exam can provide information about signs of kidney cancer and other health problems. For example, the doctor may be able to feel an abnormal mass when he or she examines your abdomen .
If symptoms or the results of the physical exam suggest you might have kidney cancer, more tests will probably be done. These might include lab tests,imaging tests, or biopsies of the kidney.
Review Of Key Questions
AHRQ posted the key questions on the Effective Health Care Website for public comment. The EPC refined and finalized the key questions after review of the public comments, and input from Key Informants and the Technical Expert Panel . This input is intended to ensure that the key questions are specific and relevant.
You May Like: What Is The Worst Skin Cancer To Have
Summary Of Protocol Amendments
|
After elimination of articles captured by the search at title-abstract level, article level, we were left with over 250 articles eligible for data abstraction. After going through and categorizing these studies by study design, we think we have enough controlled studies to address KQ3a and 3b.
There may not be any controlled study for active surveillance. It’s not a surgical treatment. This approach is most often used to identify patients who might safely avoid or defer surgery. The existing literature on active surveillance consists solely of uncontrolled studies |
F Grading The Strength Of Evidence For Major Comparisons And Outcomes
At the completion of our review, two reviewers will independently grade the strength of evidence on key outcomes, including oncologic efficacy, renal functional outcomes, quality of life, and overall survival by adapting an evidence grading scheme recommended by the Methods Guide for Conducting Comparative Effectiveness Reviews. Conflicts will be resolved through consensus or third-party adjudication
We will consider the five required domains: study limitations, directness, consistency, precision, and reporting bias of the evidence body. Additional domains will be considered if applicable.
We will grade the strength of evidence addressing management studies using the evidence grading scheme recommended in the Methods Guide.40
For the diagnostic studies, we will use the grading method recommended in the AHRQ Methods Guide for Diagnostic Tests to rate each domain .41
The evidence pertaining to the KQs classify into four basic categories: 1) high grade; 2) moderate grade; 3) low grade; and 4) insufficient grade. Table 6 defines each strength of evidence grade.
Recommended Reading: What Is The Main Cause Of Skin Cancer
Serum And Urine Biomarkers
With the rapid expansion of therapeutic options for mRCC, there is a need to prospectively select patients most likely to respond to a particular treatment. Cytokines and angiogenic factors are a promising area of investigation with the potential to identify easy-to-obtain and clinically meaningful biomarkers. Urine biomarkers and âliquid biopsyâ with circulating tumor DNA are also areas of active investigation.
Ct Assessment Of Renal Masses
The renal mass protocol, when performed with CT, varies by institution, but standard imaging includes a non-contrast phase followed by contrast-enhanced images in the nephrographic phase at approximately 90 seconds after contrast injection. The American College of Radiology provides CT as the most important technique for evaluating the indeterminate renal mass, but recognizes both CT and MRI as appropriate initial studies with comparable performance in identifying surgical lesions . The nephrographic phase serves best for detection of a renal mass, and also suffices for detection of enhancing components. The corticomedullary and urographic phases are also often acquired to provide additional anatomic information for pre-surgical planning and to assess proximity to or involvement of the collecting system. Useful imaging characteristics at CT include the detection of bulk fat, lesion density, and enhancement. However, multiple studies have been performed to assess the performance of enhancement characteristics derived from multiphase imaging in differentiation of renal tumors with limited success . A general diagnostic algorithm is presented for CT evaluation this includes potential circumstances where MRI may provide additional information for management decisions .
Diagnostic and management algorithm for small renal mass using CT.
Renal Mass Attenuation
Detection of Fat
Lesion Density
Qualitative and Quantitative Enhancement
Read Also: What Is Squamous Cell Carcinoma
What Is The Most Common Renal Mass
What is the most common renal mass? Renal Cell Carcinomas .These are the most common malignant kidney tumors. They are found in the lining of the small tubes in the kidney. RCC may form as a single tumor within a kidney. It can also form two or more tumors in one kidney.
What is considered a large renal mass?;Every year in the U.S., more than 67,000 new cases of renal cancer are diagnosed, the majority of which are small masses . However, large renal masses 4 cm still account for a significant number of cases.
What percentage of renal masses are cancerous?;About 20-30% of suspicious kidney tumors when removed prove to be benign! These benign growths include cysts, oncocytomas, angiomyolipomas, and mixed epithelial stromal tumors. Thus, 70-80% of these small kidney tumors are cancers and fortunately the majority are well behaved cancers.
What is the most common renal tumor?;Renal cell carcinoma , also known as renal cell cancer or renal cell adenocarcinoma, is the most common type of kidney cancer. About 9 out of 10 kidney cancers are renal cell carcinomas.
What Is A Renal Adenoma
A renal adenoma is a benign solid tumor in or around the kidneys, arising in glandular tissue. The incidence of these growths in the general population is not known, as they often go undiagnosed and may only be noted incidentally on autopsy findings in patients who die of other conditions. Usually a doctor identifies a renal adenoma when a medical imaging study of the kidneys is requested for an unrelated reason, and the growth appears as a finding on that study.
This type of growth tends to be slow, although there is a potential for differentiation into an aggressive and cancerous tumor. Superficially, renal adenomas can look like renal cell carcinoma, a malignancy, and a doctor will usually request a biopsy to evaluate the cells under a microscope and learn more about the tumor. If the growth is an adenoma, the doctor will not recommend treatment beyond monitoring the patient for any signs of changes.
You May Like: Do You Need Chemo For Melanoma
Having Certain Hereditary Syndromes Can Increase The Risk Of Kidney Cancer
Most of the time, kidney cancer is not passed down from parent to child. Kidney cancer that affects multiple generations of a family is called hereditary kidney cancer. Hereditary kidney cancer is rare and accounts for only 5% to 8% of all kidney cancers. It is usually linked to a hereditary syndrome. A hereditary syndrome is a set of signs and symptoms or conditions that occur together and is caused by certain changes in the genes that can be passed down from a parent to a child. Hereditary syndromes are sometimes called geneticsyndromes or family cancer syndromes. People with the hereditary syndromes described in this summary have an increased risk of getting kidney cancer.
The four hereditary syndromes described in this summary are:
Advanced Or Recurrent Kidney Cancer Treatment
For people with advanced kidney cancer that has spread to other parts of the body, treatment with a drug may be recommended along with surgery, or instead of surgery. Some of these drugs are given to you as a pill that you take by mouth; others are given as an injection.; Much progress has been made in recent years, and people with advanced kidney cancer are living much longer than ten years ago.
- Medicine is often used for advanced kidney cancer that has spread to other parts of the body or where surgery cannot be done.
- Immunotherapy uses the bodys defense system to stop or slow the growth of cancer cells
- Monoclonal antibodies attack a specific part of cancer cells
- Checkpoint inhibitors help the immune system recognize and attack cancer cells
- Vaccines give an overall boost to the immune system
Recommended Reading: Is Renal Cell Carcinoma Hereditary
Renal Oncocytoma Mimicking Renal Cell Carcinoma
Olubunmi Oladunjoye, MD, MPH1 Adeolu Oladunjoye, MD, MPH2 Anish Paudel, MD1 Ronald Herb, DO1
AFFILIATIONS:1Department of Internal Medicine, Tower Health Reading Hospital, West Reading, Pennsylvania2Department of General Pediatrics, Division of Medical Critical Care, Boston Childrens Hospital, Boston, Massachusetts
CITATION:Oladunjoye O, Oladunjoye A, Paudel A, Herb R. Renal oncocytoma mimicking renal cell carcinoma. Consultant.;2021;61:e38-e40.;doi:10.25270/con.2020.11.00009
Received July 17, 2020. Accepted October 25, 2020.;Published online November 9, 2020.
DISCLOSURES:The authors report no relevant financial relationships.
ACKNOWLEDGEMENT:We thank the Department of Pathology at Tower Health Reading Hospital for the histology images.
CORRESPONDENCE:Olubunmi Oladunjoye, MD, Department of Internal Medicine, Reading Hospital, 420 S 5th Ave, West Reading, PA 19611
A 61-year-old woman with a history of bladder prolapse and normal kidney function developed complications after a recent laparoscopic sacral colpopexy for urinary incontinence. Computed tomography scans revealed an incidental finding of an enhancing 3.3-cm mass within the right posterior kidney that was concerning for renal cell carcinoma .
Figure 1. CT scan with contrast of the abdomen and pelvis showed a 3.3-cm abdominal mass within the right posterior kidney, concerning for RCC.
Figure 3. Low-power image showing oncocytoma cells with no perinephric or vascular invasion .
REFERENCES:
What Happens To Patients With Renal Cell Carcinoma
Prognosis in patients with renal cell carcinoma
In general, the prognosis and prediction of outcomes after treatment for RCC is generally based on tumor-specific factors and patient-specific factors . Based on large studies of patients with RCC, prognostic scoring systems have been developed and validated.
-
Tumor Node Metastasis staging system
-
Memorial Sloan Kettering Cancer Center ; validated by the Cleveland Clinic Foundation
-
UCLA Integrated Staging System
-
Stage Size Grade and Necrosis scoring system for clear cell RCC; emphasis on histologic/pathologic features of clear cell RCC
-
Fuhrman Nuclear Grading System for RCC
Tumor Node Metastasis staging system:
This system is used to give general prognostic information based on the extent of tumor burden . This system is used to evaluate survival up to 5 years post-diagnosis, based on the stage at the time of diagnosis.
For stages I, II, III, and IV the 1, 2, 3, 4 and 5 year survivals are approximately as follows: respectively.
Memorial Sloan Kettering Cancer Center:
This system is perhaps the most widely used and most well validated scheme for prognostic stratification. This system is based on clinical factors and was developed based on outcomes of patients with advanced RCC. The system has also been validated by the Cleveland Clinic Foundation. Five factors are used to estimate survival in patients with advanced disease:
Based on these five factors, 3 risk categories are determined and correlate with survival data.
Table 2.
Recommended Reading: Can Skin Cancer Be Cured With Cream
Kidney Tumor With Suspicion Of Spread
You may have been told that the kidney cancer has spread. This could be to lymph nodes, the lungs, liver, bone, or even the vena cava â the largest vein in your body.
About 1/3 of patients find that the cancer has spread even without any symptoms.
For those with symptoms, you may have experienced abdominal or back pain, blood in the urine, bone pain, seizures, or even bad headaches. After a full evaluation of the extent of spread a treatment plan should be formulated.
This can get quite complicated and a multidisciplinary team who specialize in kidney cancer would be best to help with this. It is important that an urologist and medical oncologist collaborate in constructing an optimal plan for your care. This multidisciplinary approach is most important for cancers with a high suspicion of spread! This is because today there are numerous options and combinations for patients with metastatic kidney cancer.
These options can include:
Surgery – In certain settings, removal of the kidney even when the cancer has already spread has been shown to improve survival. This can often be done laparoscopically so the patient can recover rapidly and promptly receive additional therapy.
Immunotherapy – IL-2 can be a good option for some patients and can deliver excellent results for some patients. Interferon-alpha is another option.
Where Does Renal Cell Carcinoma Spread
Common sites of metastases include the lung, liver, bone, brain, and adrenal gland, with case reports detailing the capacity of RCC to appear almost anywhere in the body. More than one organ system is often involved in the metastatic process. Metastases may be found at diagnosis or at some interval after nephrectomy.
Recommended Reading: Can Cancer Cause Skin Rash
How Should Patients With Renal Cell Carcinoma Be Managed
Surgery
Laparoscopic or open approach depends on the nature of the tumor and surgeon preference and expertise:
-
Partial nephrectomy- limited resection of the portion of the kidney where the mass is
-
Simple nephrectomy- removal of the kidney without node or adrenal resection
-
Radical nephrectomy- includes a perifascial resection of the kidney, perirenal fat, regional lymph nodes, and ipsilateral adrenal gland
-
Cytoreductive nephrectomy- removal of the kidney in the setting of advanced stage IV disease where cure is not expected to be achieved
Surgical resection of localized disease remains the treatment of choice for either cure or long-term disease-free survival. Nephrectomy is recommended in patients with stage I-III disease. The degree of resection is dictated by the extent of disease and location of the tumor. Historically, partial resection was done in patients with a solitary kidney or severe CKD where a radical nephrectomy would render a patient functionally anephric. With recent data suggesting that nephrectomy-induced CKD is associated with an increased risk of all-cause and cardiovascular death, nephron-sparing procedures should be considered when at all possible.
Summary of surgical recommendations based on TNM stage of disease
Ablation Therapy
These procedures are performed by urologists and interventional radiologists. They are generally performed under conscious sedation but may require general anesthesia.
Immunotherapy
Targeted Molecular Therapy
Surveillence
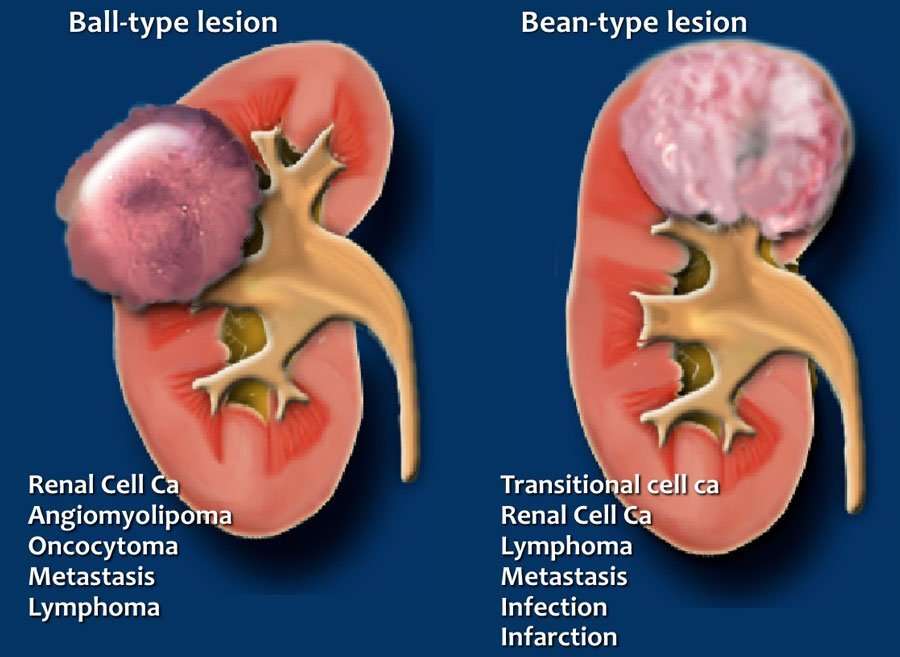
The Ball Versus The Bean
In 2006, David S. Hartman and Pablo R. Ros from the Armed Forces Institute of Pathology designed a strategy for the evaluation of renal masses and developed a concept known as ball-type or bean-type renal masses depending upon the growth pattern.
The ball-type renal masses are more common. The ball-type lesion typically deforms the renal contour, producing a hump or contour bulge. Collecting system elements are displaced. These masses are better seen on nephrographic phase becausethey are more conspicuous against the background of normally enhancing renal parenchyma. The bean-type lesions use the renal tissue as scaffolding for their growth, thus causing enlargement of the kidney, while maintaining its reniform shape. The bean-type masses are invisible on unenhanced images and are best appreciated on nephrographic and excretory phase images. Collecting system elements are destroyed by the bean-type masses . The list of ball and bean type renal masses is detailed in .
Line diagram showing ball and bean-type renal mass
Don’t Miss: Is Skin Cancer Usually Raised
Looking For More Of An Introduction
If you would like more of an introduction, explore these related items. Please note that these links will take you to other sections on Cancer.Net:
-
ASCO Answers Fact Sheet:Read a 1-page fact sheet that offers an introduction to kidney cancer. This free fact sheet is available as a PDF, so it is easy to print.
What Is Renal Cell Carcinoma
It’s the most common type of kidney cancer. Although itâs a serious disease, finding and treating it early makes it more likely that youâll be cured. No matter when youâre diagnosed, you can do certain things to ease your symptoms and feel better during your treatment.
Most people who have renal cell carcinoma are older, usually between ages 50 and 70. It often starts as just one tumor in a kidney, but sometimes it begins as several tumors, or itâs found in both kidneys at once. You might also hear it called renal cell cancer.
Doctors have different ways to treat renal cell carcinoma, and scientists are testing new ones, too. Youâll want to learn as much about your disease as you can and work with your doctor so you can choose the best treatment.
Don’t Miss: How To Treat Melanoma In Nails