What Are The Risk Factors For Basal Cell Carcinoma
Basal cell carcinoma, squamous cell carcinoma and melanoma are all skin cancers caused by exposure to damaging ultraviolet raysfrom natural and artificial sunlight. There’s also a genetic condition called basal cell nevus or Gorlin syndrome, which can cause people to develop hundreds of basal cell skin cancers, but it’s extremely rare, says Dr. Christensen.
People at the highest risk for basal cell carcinoma tend to have fair or light-colored skin, a history of sun exposure and a tendency to sunburn quickly. Fair-skinned people have a 50 percent risk of developing basal skin cancer at some point in their lives, Dr. Christensen says. The cancer is the result of cumulative damage of years spent in the sun, and may take 20 years to manifest.
Although it’s often more common in older people, it can occur in younger adults, too.
Basal cell carcinoma spreads very slowly and very rarely will metastasize, Dr. Christensen says. But if it’s not treated, basal cell carcinoma can continue to grow deeper under the skin and cause significant destruction to surrounding tissues. It can even become fatal. For example, an untreated basal cell carcinoma on the face can grow into the bones and, over time, directly into the brain, Dr. Christensen says.
How Can I Prevent Basal Cell Carcinoma
The most important modifiable risk factor for skin cancer is reducing ultraviolet light exposure. A few studies have linked intermittent, intense sun exposure during childhood and adolescence with developing BCC.2 This is the kind of sun exposure you might have during a summer day at the beach or pool. People who live close to the equator have more UV exposure and are more likely to develop BCC than people at higher latitudes.2Indoor tanning increases the risk of BCC by approximately 40%.2
Luckily, there are many ways to reduce your UV exposure, including:
- Using a broad spectrum sunscreen with sun protection factor 15 or higher.
- Seeking shade between 10 am and 2 pm.
- Wearing long sleeves, long pants, wide-brimmed hats, and sunglasses.
- Avoiding indoor tanning beds.
There are other risk factors for BCC that you cannot change. These include light skin color, tendency to burn, freckling, medical history, age, and gender. People at high risk of skin cancer can take steps to detect cancer early when it is easiest to treat.
Basal Cell Cancer Of The Head And Neck Treatment
Surgery is the preferred method of treatment for basal cell cancer. Radiation is an alternative when surgery is not desirable because of cosmetic concerns or medical reasons. Many early stage small basal cell cancers can be removed by Mohs surgery, which is a technique that spares normal tissue through repeated intraoperative margin testing, removing only the cancer and leaving adjacent normal tissue. Excision, curettage and desiccation, and cryosurgery can also be used to remove the cancer while sparing normal tissue. Large tumors and tumors with nerve or lymph node involvement are not suitable for Mohs surgery and require a multimodality approach to treatment with formal surgical resection and adjuvant radiation or chemotherapy. Larger tumors require reconstruction, which can be done at the time of surgery if margin status is clear.
Patients with high-risk tumors should meet with a radiation therapist to discuss postoperative radiation. In patients with high-risk tumors who are not surgical candidates, systemic treatment with chemotherapy that inhibits the Hedgehog pathway of tumor progression has been shown to be effective. Such cases require multidisciplinary care by a team of surgeons, radiation oncologists and medical oncologists.
Johns Hopkins Head and Neck Cancer Surgery
Don’t Miss: Squamous Cell Carcinoma Skin Metastasis
How Serious Is Basal Cell Skin Cancer
Basal cell skin cancer, also called basal cell carcinoma, is usually very curable, but it can cause disfigurement and complications if it’s not treated. In the majority of cases, basal cell carcinoma is very treatable.
It is unusual for basal cell carcinoma to cause death. Approximately 2,000 people in the U.S. die each year from basal and squamous skin cancers. In most cases, people who die from these types of skin cancer tend to be older, immunosuppressed, or have been diagnosed at a very late stage.
Skin: Condition: Infomation Mohs Micrographic Surgery
This surgical procedure is used to treat more complex BCCs such as those present at difficult anatomical sites or recurrent BCCs. The procedure involves excision of the affected skin and examination of the skin removed under the microscope straight away to see if all of the BCC has been removed. If any residual BCC is left at the edge of the excision further skin is excised from that area and examined under the microscope and this process is continued until all of the BCC is removed. The site is then often closed with a skin graft. This is a time consuming process and is only undertaken when simple surgery may not be suitable.
Also Check: Does Skin Cancer Itch And Burn
Treatment Of Basal Cell Carcinoma
-
Usually with local methods
Treatment of basal cell carcinoma should be done by a specialist.
The clinical appearance, size, site, and histologic subtype determine choice of treatmentcurettage and electrodesiccation, surgical excision, cryosurgery, topical chemotherapy and photodynamic therapy, or, occasionally, radiation therapy.
Recurrent or incompletely treated cancers, large cancers, cancers at recurrence-prone sites , and morphea-like cancers with vague borders are often treated with Mohs microscopically controlled surgery, in which tissue borders are progressively excised until specimens are tumor-free .
If patients have metastatic or locally advanced disease and are not candidates for surgery or radiation therapy , vismodegib and sonidegib may be given. Both drugs inhibit the hedgehog pathway .
What Are The Risk Factors For Superficial Basal Cell Carcinoma Of Skin
The risk factors that contribute to Superficial Basal Cell Carcinoma of Skin formation include:
- Prolonged sun exposure, exposure to ultraviolet light
- Use of tanning beds, tanning parlors
- Arsenic exposure
- Ionizing radiation
- Smoking
- The presence of certain genetic syndromes such as basal cell nevus syndrome increases the risk
- Caucasians are more vulnerable compared to other darker-toned individuals
It is important to note that having a risk factor does not mean that one will get the condition. A risk factor increases one’s chances of getting a condition compared to an individual without the risk factors. Some risk factors are more important than others.
Also, not having a risk factor does not mean that an individual will not get the condition. It is always important to discuss the effect of risk factors with your healthcare provider.
You May Like: Amelanotic Melanoma Blanch
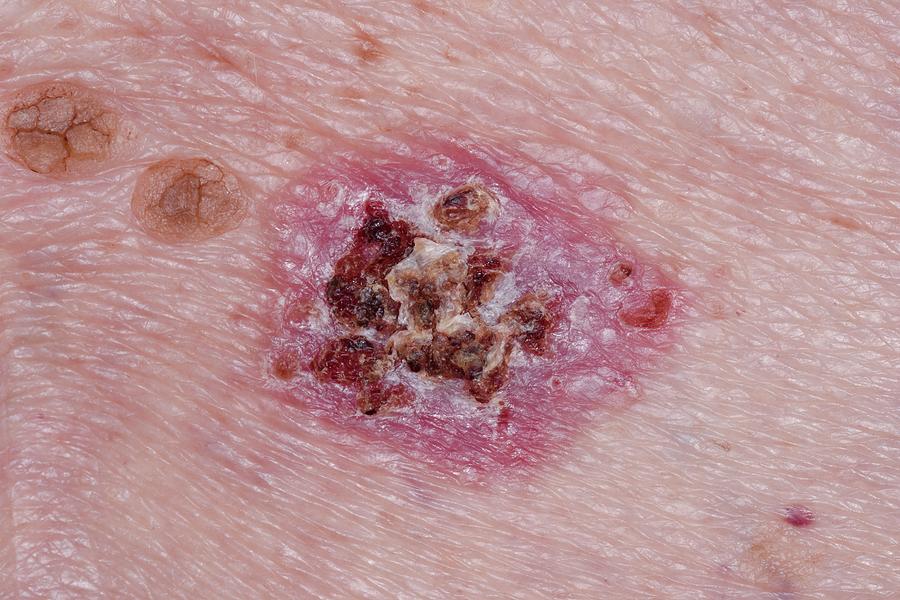
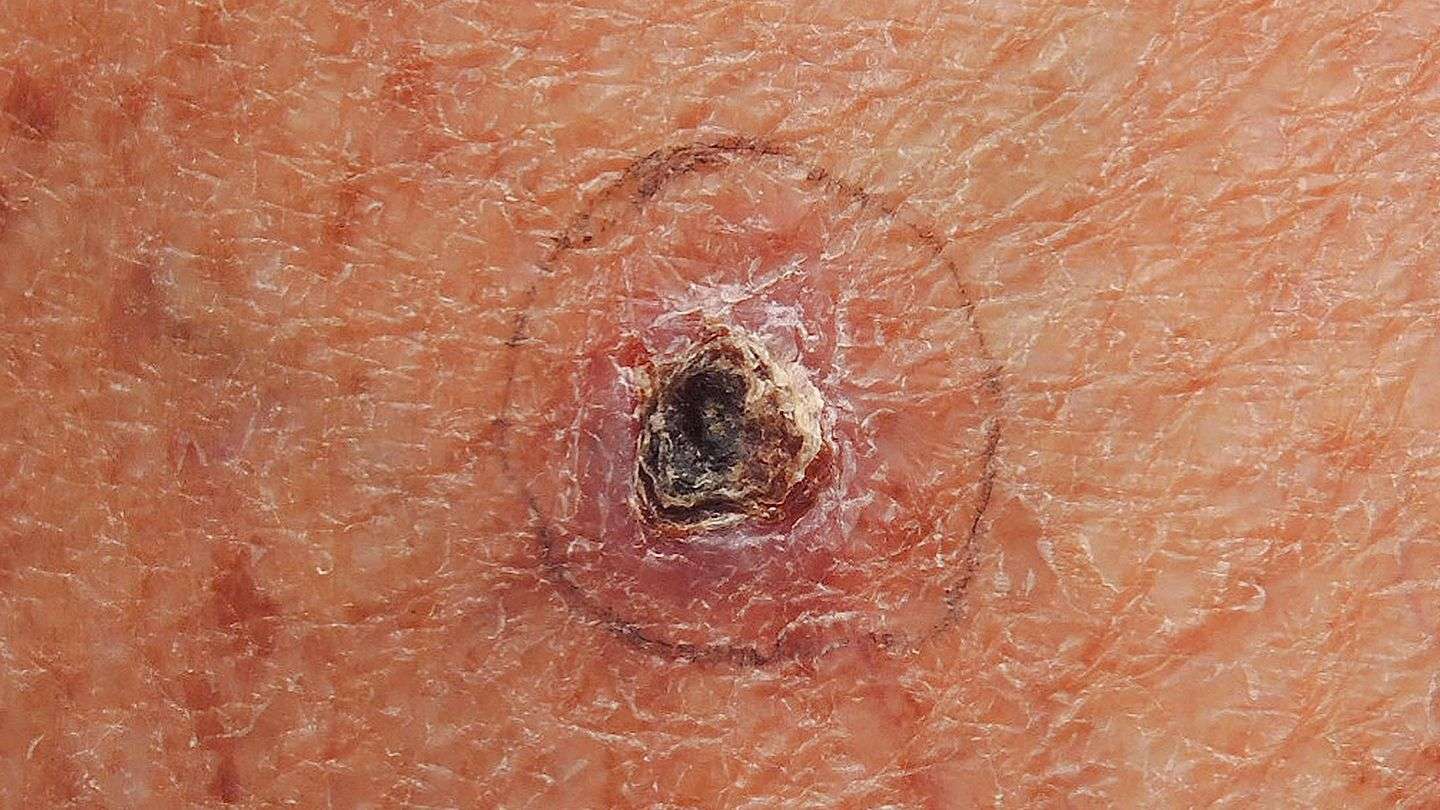
How To Spot A Bcc: Five Warning Signs
Check for BCCs where your skin is most exposed to the sun, especially the face, ears, neck, scalp, chest, shoulders and back, but remember that they can occur anywhere on the body. Frequently, two or more of these warning signs are visible in a BCC tumor.
Please note: Since not all BCCs have the same appearance, these images serve as a general reference to what basal cell carcinoma looks like.
An open sore that does not heal
A reddish patch or irritated area
A small pink growth with a slightly raised, rolled edge and a crusted indentation in the center
A shiny bump or nodule
A scar-like area that is flat white, yellow or waxy in color
How Is Basal Cell Cancer Of The Head And Neck Diagnosed
Diagnosis is made by clinical exam and a biopsy. Basal cell cancers are staged by size and extent of growth. These cancers rarely metastasize to lymph nodes or other organs, but they can grow quite large and invade small nerves and local structures.
Biopsy can help determine if the basal cell cancer is a low-risk tumor or a high-risk tumor that requires more aggressive treatment. Low-risk tumors are often nodular and do not have nerve involvement. High-risk tumors in the head and neck are those that involve the central face, nose and eye area, as well as those tumors that are greater than or equal to 10 millimeters on the cheeks, scalp and neck tumors that are recurrent or arising from previously radiated tissue and tumors arising in patients who are immunosuppressed. An aggressive growth pattern on the pathology evaluation and perineural invasion are also features of high-risk basal cell cancers.
Recommended Reading: What Is The Most Aggressive Skin Cancer
How Widespread Is Bcc
Basal cell carcinoma is quite common, and the number of reported cases in the U.S. has steadily increased.
- An estimated 3.6 million Americans are diagnosed with BCC each year.
- More than one out of every three new cancers are skin cancers, and the vast majority are BCCs.
- The diagnosis and treatment of nonmelanoma skin cancers, including BCC and squamous cell carcinoma , increased up to 77 percent between 1994 and 2014.
Reviewed by:
What Are The Symptoms Of Basal Cell Carcinoma
BCCs usually develop on parts of the body that are often exposed to the sun, like the head, face, shoulders, arms and lower legs.
They often start with a subtle change in the skin, like a small bump or a flat red patch.
Signs of a BCC to look for include:
- a pearly spot or lump
- a scaly, dry area that is shiny and pale or bright pink in colour
- a sore that doesnt heal
- a sore that bleeds
See your doctor if you notice any new spots or an existing spot that changes size, shape or colour. Visit the Cancer Councils website for tips on how to check your skin.
Also Check: Stage 3 Basal Cell Carcinoma Survival Rate
Of Basal Cell Carcinoma
Basal cell carcinoma: The most common type of skin cancer, which commonly presents as a sore that seems to get better and then recurs and may start to bleed. Basal cell carcinoma often occurs on the face and neck, where the skin is exposed to sunlight. These tumors are locally invasive and tend to burrow in but not metastasize to distant locations.
©1996-2021 MedicineNet, Inc. All rights reserved. Terms of Use.
MedicineNet does not provide medical advice, diagnosis or treatment. See additional information.
Health Categories
What Is Basal Cell Carcinoma Skin Cancer
Thomas Urban Marron, MD, PhDAlamy
Mark Lebwohl, MD, a professor and the chairman at the Kimberly and Eric J. Waldman Department of Dermatology at Mount Sinai and a spokesperson for the Skin Cancer Foundation, recalls once running into a doctor colleague at work with a scab on his lip.
Crossing paths again weeks later, his colleague had the same scab.
I looked at him and said, You really should have that looked at, and he said, Oh, its just a scab, I keep hitting it when I shave, says Dr. Lebwohl. Ultimately, his colleague did get it looked at by a dermatologist. It was skin cancer, more specifically basal cell carcinoma .
Skin cancer is the most common type of cancer in the United states, and BCC is the most frequently occurring of all forms of cancer, according to the Skin Cancer Foundation. Basal cell carcinoma, which can appear, as in the case of Lebwohls colleague, as a minor irritation, has more than 4 million cases diagnosed annually. And like Lewohl’s colleague, a wound that wont heal is just one possible manifestation of basal cell carcinoma.
RELATED:What Doctors and Specialists Treat Skin Cancer?
Read Also: Does Insurance Cover Skin Cancer Screening
Basal Cell Carcinoma Treatment And Diagnosis
Basal cell carcinoma diagnosis is a frequent and daily occurrence across the UK. Fortunately, the vast majority are very easy to cure and very few people diagnosed with BCC will see it spread from its starting site or suffer serious ill-health. However, this relies on early detection. As described and illustrated above most of these lesions are easy to notice and this usually prompts early medical review and treatment. This limits the number of people that present for basal cell cancer treatment at a late stage.
Diagnosis is often by inspection but sometimes confirmation is required by a simple skin biopsy which is then assessed under a microscope. Lesions in a single site are usually removed with minor surgical procedures. Basal cell carcinoma removal and surgery often only requires local anaesthetic. Some very small lesions can be treated with topical chemotherapy type creams.
Further details of basal cell carcinoma treatment can be foundhere.
Targeted Therapy Or Immunotherapy For Advanced Basal Cell Cancers
In rare cases where basal cell cancer spreads to other parts of the body or cant be cured with surgery or radiation therapy, a targeted drug such as vismodegib or sonidegib can often shrink or slow its growth.
If these drugs are no longer working , the immunotherapy drug cemiplimab can sometimes be helpful.
Recommended Reading: How To Identify Basal Cell Carcinoma
Nevoid Basal Cell Carcinoma Syndrome
In addition to basal cell carcinoma, this autosomal dominant disorder can result in the early formation of multiple odontogenic keratocysts, palmoplantar pitting, intracranial calcification, and rib anomalies. Various tumors such as medulloblastomas, meningioma, fetal rhabdomyoma, and ameloblastoma also can occur.
Odontogenic keratocysts, palmoplantar pitting, intracranial calcification, and rib anomalies may be seen. Mutations in the hedgehog signaling pathway, particularly the patched gene, are causative.
Go to Nevoid Basal Cell Carcinoma Syndrome to see more complete information on this topic.
Dna Mismatch Repair Proteins
DNA mismatch repair proteins are a group of proteins that physiologically stimulate G2 cell cycle checkpoint arrest and apoptosis. Failure of MMR proteins to detect induced DNA damage results in the survival of mutating cells. MMR protein levels have been found to be higher in nonmelanoma skin cancers than in normal skin, and there is also some evidence of MMR dysregulation.
Read Also: Osteomyoma
Who Is Affected By Basal Cell Carcinoma
Basal cell carcinoma affects slightly more men than women. It occurs more often in older people. People with fair skin and light eyes are more likely to get BCC. It is 19 times more common in whites than blacks, but people of color may still be affected. People who have had BCC once are at higher risk for developing another lesion.
Types Of Basal Cell Carcinoma
There are several types of basal cell carcinoma, including:
- Nodular basal cell carcinoma: Approximately 60-80% of all basal cell carcinomas that present on the face or head are nodular. It is the most common subtype, and it is also known as nodulocystic carcinoma. It presents as a shiny, smooth nodule. It may have a dip in the center, with rolled edges, and blood vessels are often seen to cross its surface.
- Superficial spreading basal cell carcinoma: Most commonly seen on the upper body, back, and shoulders, this type is more common in younger adults. It presents as shallow, scaly, irregular plaques that are pink or a similar color to the skin itself. Almost all superficial spreading basal cell carcinomas are secondary to sun damage.
- Sclerosing basal cell carcinoma : This type can be challenging to diagnose. Most commonly seen on the face, it can look like a small, waxy, white scar that expands over time. It can be more dangerous or disfiguring because it is often not recognized as skin cancer until it has grown.
- Pigmented basal cell carcinoma: Most commonly occurs in people with a darker skin tone, particularly Asians. The pigmentation can be found in the different basal cell carcinoma subtypes and it can appear dark blue, dark brown, or black.
It is possible that you can get more than one type of basal cell carcinoma simultaneously. If you have one type, it increases your risk of getting another. Basal cell carcinoma rarely spreads to other parts of the body.
Also Check: Does Amelanotic Melanoma Blanch When Pressed
How Is Superficial Basal Cell Carcinoma Of Skin Treated
In general, the treatment of Superficial Basal Cell Carcinoma of Skin depends upon a variety of factors including:
- The location of the tumor
- The number of tumors
- The size of the tumor
- Any health considerations of the patient
A number of treatment methods may be used to treat Superficial Basal Cell Carcinoma of Skin. The treatment types may include:
Topical medications can be used to treat Superficial Basal Cell Carcinoma. This is because the thinness of the tumor permits permeation of the active ingredient to the full depth of the carcinoma. The two most frequently used active ingredients are imiquimod and 5-Flurouracil.
- Imiquimod is an immune system signal which calls for the migration of T-cells into the area of the tumor, which actively kill the cancer cells
- 5-Flurouracil is a metabolic agent which toxically kills the more basal cell carcinoma cells. The surrounding normal skin does not absorb the medication and hence is safe from the toxicity
Both these topical applications take at least a few weeks to treat a typically sized lesion, longer for larger lesions. The actions will lead to redness, irritation, sometimes crusting and possibly secondary infection
One advantage of these creams is that it is sometimes possible to treat the Superficial Basal Cell Carcinoma without affecting the underlying skin at all, so after healing, little to no scarring is detectable.
Other techniques to treat this skin cancer may include: