After Melanoma Has Been Diagnosed Tests May Be Done To Find Out If Cancer Cells Have Spread Within The Skin Or To Other Parts Of The Body
The process used to find out whether cancer has spread within the skin or to other parts of the body is called staging. The information gathered from the staging process determines the stage of the disease. It is important to know the stage in order to plan treatment.
For melanoma that is not likely to spread to other parts of the body or recur, more tests may not be needed. For melanoma that is likely to spread to other parts of the body or recur, the following tests and procedures may be done after surgery to remove the melanoma:
The results of these tests are viewed together with the results of the tumor biopsy to find out the stage of the melanoma.
Will Immunotherapy Be The End Of Cancer
Immunotherapy has been called a great hopeand a great hype. As a patient facing devastating odds, our writer bet her life on it.
In September of 2011, I did the worst Google search of my life. A year after a seemingly manageable melanoma diagnosis and surgery, I learned that my cancer had appeared again, this time moving aggressively into my lungs and soft tissue. Naturally, the first thing I did was open my laptop and type “stage 4 melanoma life expectancy.” Then I cried. The results were terrifying.
On the website of MD Anderson, one of the most prestigious cancer centers in the world, I found a January 2011 article on metastatic melanoma. There was a telling quote from Michael Davies, MD, of the centers Melanoma Medical Oncology Department: “The average survival for patients with stage 4 metastatic melanoma is 6 to 10 months, and this hasnt changed for 30 years.”
I still get chills when I recall my prognosis not so very long ago, a prognosis that looked likely to wipe my presence from my two young daughters childhoods. Yet a month after my diagnosis, I became one of the first dozen patients in a new clinical trial at the Memorial Sloan Kettering Cancer Center in New York City, receiving a type of treatment known as immunotherapy, which harnesses the bodys natural defenses to fight cancer. Three months later, I was declared cancer-free, and I have been ever since. I had not only been granted a futureI had seen a glimpse of it. Welcome to the next era of medicine.
Giving Thanks And Giving Back
Fighting metastatic melanoma was a long, hard road, and I was extremely fortunate. But more than anything, I had an incredible team by my side, including:
- Thomas Froehlich, M.D. oncology, internal medicine
- Sheeba Cantanelli, P.A.-C.
- Stephanie Savory, M.D. melanoma, dermatology
- And countless nurses and other expert providers
I am convinced that I survived because Dr. Froehlich and my other doctors were always on the cutting edge of new treatments for this terrible disease. I always felt that I was getting the best and most innovative treatments. I never had any doubt we were proceeding correctly. I had, and continue to have, complete faith in the dedicated doctors and medical personnel at UT Southwestern who saved my life.
Since February 2018, Ive been feeling great and I continue to be cancer-free. I now find great joy in connecting with people who are going through experiences similar to mine. I am proud to be an original member of the patient family advisory board at UT Southwestern, which helps shape aspects of patient care.
I’ve also helped set up a partnership with Imerman Angels, an international program that enables one-on-one support among cancer fighters, survivors, and caregivers. Ive mentored many great people through this program and offered ideas and perspectives to stay mentally strong through treatment.
Different things work for different people. One of my mentees finds strength through meditation. You have to find what works for you.
You May Like: What Causes Renal Cell Carcinoma Cancer
How Effective Is Immunotherapy
Success rates for any cancer treatment, including immunotherapy, depend on individual factors, including the cancer type and stage. In general, immunotherapy is effective against many cancers. While some cancers are more immunogenic than others, in general, immunotherapy is effective across a wide variety of cancers. Immunotherapy can produce durable responses unlike chemotherapy or radiation, however, these occur only in around 25% patients.
Some research suggests that the immune system may remember cancer cells after immunotherapy ends.
What Are Cancer Vaccines
A cancer vaccine can also help your body fight disease. A vaccine exposes your immune system to a foreign protein, called an antigen. This triggers the immune system to recognize and destroy that antigen or related substances. There are 2 types of cancer vaccine: prevention vaccines and treatment vaccines.
In general, immunotherapy is an important approach to find new treatments for cancer. The examples above do not include every type of immunotherapy treatment. Researchers are studying many new drugs. You can learn more about immunotherapy in each cancer-specific section on Cancer.Net; Look at the “Types of Treatment” and “Latest Research” pages for specific information about immunotherapy for that type of cancer. You can also learn about the latest immunotherapy research on the Cancer.Net Blog.
Recommended Reading: Can You Die From Basal Cell Skin Cancer
How Does Immunotherapy Work
Different types of immunotherapy work differently to fight melanoma. Immunotherapy can be systemic or local.
Systemic;treatments travel through the bloodstream to reach all parts of the body. Cancer physicians use systemic immunotherapy to treat metastatic cancer, which is cancer that has spread from its original location to other areas of the body.
Local;treatments are applied, usually by injection, directly to melanoma lesions. Local immunotherapy treatments work by infecting and killing melanoma cells in the treated lesions. They may also produce an immune response.
Watch Dr. Evan J. Lipson of Johns Hopkins Medicine discuss more on immunotherapy.
The Future Of Immunotherapy
Terry’s story shows the powerful effects, as well as the challenges, associated with immunotherapy. It is a relatively new treatment, and we continue to refine it and use it in new ways. Weve seen how it works against melanoma, as well as kidney cancer and lung cancer.
And while immunotoxicities are not what we want, there is some data to suggest that patients who get them are more likely to respond to the treatment. We dont know exactly why, and through clinical trials we are working to prevent side effects while continuing to reap the benefits of immunotherapy.
Clinical trials offer gold standard of care plus the newest available treatments, often at little to no cost to patients. These studies help us advance treatment options for more patients.
If you or a loved one is diagnosed with metastatic melanoma, ask your doctor about immunotherapy. Find an academic medical center that has teams of experts in place not only to manage your care, but also the potential side effects of treatment.
Weve only scratched the surface of what immunotherapy can offer cancer patients. But at UT Southwestern and Simmons Cancer Center we are determined to continue improving it to help more patients like Terry beat this disease and lead longer, healthier lives.
To find out whether you or a loved one might benefit from immunotherapy, call or request an appointment online.
Don’t Miss: How Is Basal Cell Carcinoma Removed From The Nose
How Do Immune Checkpoint Inhibitors Work Against Cancer
Immune checkpoints are a normal part of the immune system. Their role is to prevent an immune response from being so strong that it destroys healthy cells in the body.
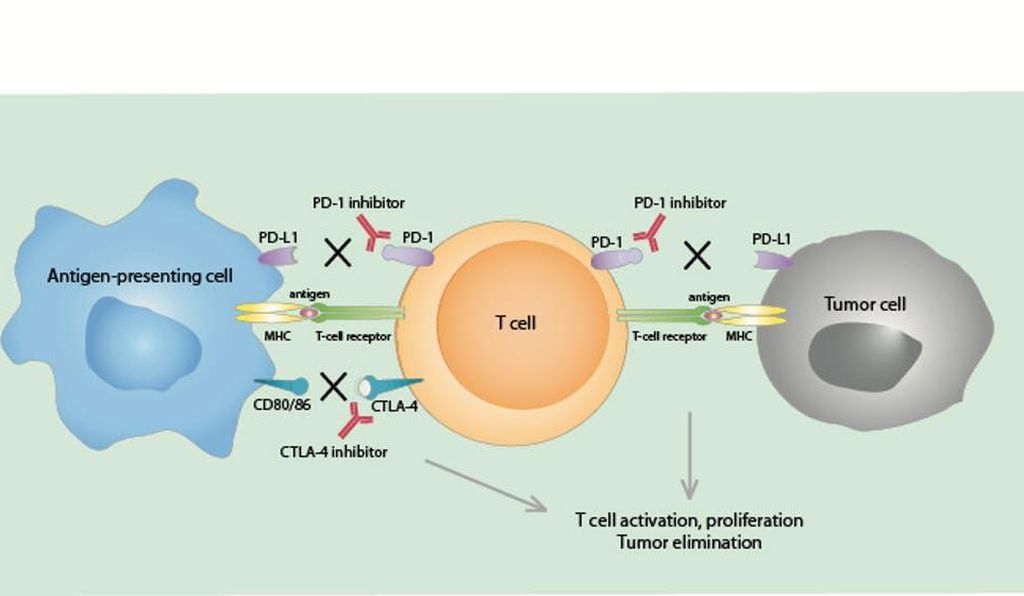
Immune checkpoints engage when proteins on the surface of immune cells called T cells recognize and bind to partner proteins on other cells, such as some tumor cells. These proteins are called immune checkpoint proteins. When the checkpoint and partner proteins bind together, they send an off signal to the T cells. This can prevent the immune system from destroying the cancer.
Immunotherapy drugs called immune checkpoint inhibitors work by blocking checkpoint proteins from binding with their partner proteins. This prevents the off signal from being sent, allowing the T cells to kill cancer cells.
One such drug acts against a checkpoint protein called CTLA-4. Other immune checkpoint inhibitors act against a checkpoint protein called PD-1 or its partner protein PD-L1. Some tumors turn down the T cell response by producing lots of PD-L1.
Immune Checkpoint Inhibitors
Learn about immune checkpoint inhibitors, one type of immunotherapy used to treat cancer.
What Should I Expect After Immunotherapy
Unlike chemotherapy, immunotherapy may not always cause tumor shrinkage. Rarely, tumors temporarily swell or get bigger as immune cells attack the cancer even when patients are feeling great. This phenomenon is known as pseudoprogression. The term means that a tumor only appears to be worsening and patients may still be deriving benefit.
Youll need to see your healthcare provider often to track treatment response. You may have frequent physical exams, blood tests and imaging scans.
Read Also: What Is Non Small Cell Carcinoma
Treating Stage 1 To 2 Melanoma
Treating stage 1 melanoma involves surgery to remove the melanoma and a small area of skin around it. This is known as surgical excision.
Surgical excision;is usually;done;using local anaesthetic, which means you’ll be awake, but the area around the melanoma will be numbed, so you will not feel pain. In some cases, general anaesthetic is used, which means you’ll be unconscious during the procedure.
If a surgical excision is likely to leave a significant scar, it may be done in combination with a skin graft. However, skin flaps are now more commonly used because the scars are usually less noticeable than those resulting from a skin graft.
Read more about flap surgery.
In most cases, once the melanoma has been removed there’s little possibility of it returning and no further treatment should be needed. Most people are monitored for 1 to 5 years and are then discharged with no further problems.
A Sense Of Empowerment
Our online research of melanoma yielded an interesting fact. A series of new treatments had gone through clinical trials and been approved by the U.S. Food and Drug Administration for the treatment of metastatic melanoma. They were called immunotherapy drugs, and they were showing amazing results in certain people with melanoma, including former U.S. President Jimmy Carter. We had no idea whether I would benefit from these drugs or if my insurance would pay for them, but we kept hearing more about their successes in both clinical trials and the real world.;
The moment I was approved for treatment with nivolumab and ipilimumab was when hope came alive for Elvira and me. We had never really lost hope, but we knew the odds were stacked against us. Now, we felt that I had a chance against this diagnosis.
Immunotherapy is so powerful because it does not fight the cancer directly. Instead, it prompts the patients own immune system to recognize and destroy the cancer cells. Once those drugs were coursing through my system, my immune system was actually doing the hard work. It was incredibly empowering to realize that my own body was no longer a bystander in my cancer treatment.; It was working with a singular purpose: to rid my body of cancer cells.
Read Also: How Fast Does Subungual Melanoma Grow
Certain Factors Affect Prognosis And Treatment Options
The prognosis and treatment options depend on the following:
- The thickness of the tumor and where it is in the body.
- How quickly the cancer cells are dividing.
- Whether there was bleeding or ulceration of the tumor.
- How much cancer is in the lymph nodes.
- The number of places cancer has spread to in the body.
- The level of lactate dehydrogenase in the blood.
- Whether the cancer has certain mutations in a gene called BRAF.
- The patients age and general health.
What Are Monoclonal Antibodies And Tumor
When your immune system detects something harmful, it makes antibodies. Antibodies are proteins that fight infection by attaching to antigens, which are molecules that start the immune response in your body.
Monoclonal antibodies are made in a laboratory to boost your bodys natural antibodies or act as antibodies themselves. Monoclonal antibodies can help fight cancer in different ways. For example, they can be used to block the activity of abnormal proteins in cancer cells. This is also known as a targeted therapy, or cancer treatment that targets a cancers specific genes, proteins, or the tissue environment that helps the tumor grow and survive.
Other types of monoclonal antibodies boost your immune system by inhibiting or stopping immune checkpoints. An immune checkpoint is normally used by the body to naturally stop the immune systems response and prevent it from attacking healthy cells. Cancer cells can find ways to hide from the immune system by activating these checkpoints. Checkpoint inhibitors stop the ability of cancer cells to stop the immune system from activating, and in turn, amplify your bodys immune system to help destroy cancer cells. Common checkpoints that these inhibitors affect are the PD-1/PD-L1 and CTLA-4 pathways.
Examples of immune checkpoint inhibitors are:
-
Ipilimumab
-
Avelumab
-
Durvalumab
Don’t Miss: What Does Skin Cancer On Scalp Feel Like
Vaccination Strategies For Melanoma
Several strategies are currently being explored to find an effective vaccine-based therapy for melanoma, including those that have the capability to target melanoma cells directly, DC-based vaccines, peptide-based vaccines, and vector-based vaccines .
Vaccines targeting melanoma cells are an active, specific immunotherapy based on the use of patients’ own or donors’ melanoma cells from resected tumors .
DCs are antigen-presenting cells with an elevate capacity of inducing T cell immunity through the activation of cytotoxic T cell response and proinflammatory cytokine response. DC-based vaccines have limited efficacy since tumors tend to reside in immunosuppressive microenvironments .
DNA-based vaccines have been shown to be safe and immunogenic in clinical trials; however, to date, they have not shown satisfactory effectiveness .
Unusual Moles Exposure To Sunlight And Health History Can Affect The Risk Of Melanoma
Anything that increases your risk of getting a disease is called a risk factor. Having a risk factor does not mean that you will get cancer; not having risk factors doesn’t mean that you will not get cancer. Talk with your doctor if you think you may be at risk.
Risk factors for melanoma include the following:
- Having a fair complexion, which includes the following:
- Fair skin that freckles and burns easily, does not tan, or tans poorly.
- Blue or green or other light-colored eyes.
- Red or blond hair.
Being White or having a fair complexion increases the risk of melanoma, but anyone can have melanoma, including people with dark skin.
See the following PDQ summaries for more information on risk factors for melanoma:
Recommended Reading: How Can Skin Cancer Kill You
Not A Cure But An Extension: How Immunotherapy Works For Advanced Lung Cancer
May 3, 2018
For nearly five decades, doctors have usedvarious forms of immunotherapy to treat certain cancers. These treatmentsstimulate the patients own immune system to attack a disease, much like itwould a virus or another foreign invader. Promising data have emerged toindicate its effectiveness against many cancers, including lung, kidney,melanoma, and some colon cancers.
Most recently, lung cancer has receivedattention for data released from a studypublished in The New England Journal ofMedicine and featured in The New York Times. In the study,the immunotherapy drug pembrolizumab was combined with chemotherapyto determine whether the dual approach was more effective than chemotherapyalone for metastatic nonsquamous non-small cell lung cancer.;
The results are encouraging: Patients whoreceived the dual therapy lived longer than those who received onlychemotherapy. In fact, the findings suggest that earlier introduction ofimmunotherapy for certain patients might one day become the standard treatment.
But while the data are promising, we must notbe too eager to declare victory. Todays immunotherapy is not a cure forlate-stage lung cancer. However, it can give certain patients more precioustime with family and friends. To provide that, we must carefully selectpatients who will benefit most and determine the most appropriate availabletreatment.; Recent developments havefocused on immune checkpoint inhibitors and on CAR-T cell therapy.
What Is Immunotherapy For Melanoma Cancer
For over 40 years, the Saint Johns Cancer Institute has investigated how tumors evolve in the context of the immune system.
Institute co-founder Donald L. Morton, MD, was an early advocate of finding ways to harness the immune systems power to fight cancer. In the early 1970s, he pioneered a method of injecting Bacilli Calmette-Guérin , a weakened strain of the tuberculosis bacterium, directly into melanoma tumors, which was the first successful use of immunotherapy against metastatic human cancer.;This research commenced in the melanoma research program under the late Dr. Donald L. Morton and continues today.
Read Also: What Does Skin Cancer Look Like On Your Head
How Are They Treated
For most people, steroids can help manage the symptoms and not stop the drugs from working. Topical corticosteroid creams and oral antihistamines can often give quick relief for skin symptoms. Over-the-counter treatments should work for mild diarrhea as well.
High-test steroids like prednisolone or other drugs that suppress your immune system are also the choice to treat most other problems, which you may hear your doctor refer to as adverse events, or AEs.
In addition to steroids, you might have to take permanent hormone supplements after being on this type of treatment. If the symptoms are too severe, your doctor may pause your treatment for a while. But if you have a life-threatening reaction, youâll need to stop treatment.