Symptoms If Cancer Has Spread To The Brain
You might have any of the following symptoms if your cancer has spread to your brain:
- headaches
- weakness of a part of the body
- fits
- personality changes or mood changes
- eyesight changes
-
J Tobias and D HochhauserJohn Wiley and Sons Ltd
-
TNM Staging ChartsLippincott Williams and Wilkins, 2009
-
Improving supportive and palliative care for adults with cancerNational Institute for Clinical Excellence , 2004
-
Oxford Textbook of Palliative MedicineEds D Doyle and othersOxford Universty Press, 3rd edition 2005
-
Cancer and its Management J Tobias and D HochhauserWiley Blackwell, 2015
Surgery For Melanoma Skin Cancer
Most people with melanoma skin cancer will have surgery. The type of surgery you have depends mainly on where the cancer is located and the risk that the cancer will come back . When planning surgery, your healthcare team will also consider other factors, such as your age, your overall heath and how surgery will affect how you look.
Surgery may be done for different reasons. You may have surgery to:
- completely remove the tumour
- repair or rebuild the area where the cancer was removed
- remove lymph nodes
- reduce pain and relieve any symptoms
The following types of surgery are used to treat melanoma skin cancer. You may also have other treatments before or after surgery.
Medical Treatment For Skin Cancer
Surgical removal is the mainstay of skin cancer treatment for both basal cell and squamous cell carcinomas. For more information, see Surgery.People who cannot undergo surgery may be treated by external radiation therapy. Radiation therapy is the use of a small beam of radiation targeted at the skin lesion. The radiation kills the abnormal cells and destroys the lesion. Radiation therapy can cause irritation or burning of the surrounding normal skin. It can also cause fatigue. These side effects are temporary. In addition, topical chemotherapy creams have been FDA approved for the treatment of certain low-risk nonmelanoma skin cancers. Patients with advanced or many basal cell carcinomas are sometimes prescribed oral pills to block the growth of these cancers. Side effects include muscle spasms, hair loss, taste changes, weight loss and fatigue.
In advanced cases of melanoma, immune therapies, vaccines, or chemotherapy may be used. These treatments are typically offered as clinical trials. Clinical trials are studies of new therapies to see if they can be tolerated and work better than existing therapies.
Read Also: What Is The Most Aggressive Skin Cancer
What Are Basal And Squamous Cell Skin Cancers
Basal and squamous cell skin cancers are the most common types of skin cancer. They start in the top layer of skin , and are often related to sun exposure.
Cancer starts when cells in the body begin to grow out of control. Cells in nearly any part of the body can become cancer cells. To learn more about cancer and how it starts and spreads, see What Is Cancer?
Symptoms If Cancer Has Spread To The Bone
You might have any of the following symptoms if your cancer has spread to the bones:
- pain from breakdown of the bone the pain is continuous and people often describe it as gnawing
- backache, which gets worse despite resting
- weaker bones they can break more easily
- raised blood calcium , which can cause dehydration, confusion, sickness, tummy pain and constipation
- low levels of blood cells blood cells are made in the bone marrow and can be crowded out by the cancer cells, causing anaemia, increased risk of infection, bruising and bleeding
Cancer in the spinal bones can cause pressure on the spinal cord. If it isn’t treated, it can lead to weakness in your legs, numbness, paralysis and loss of bladder and bowel control . This is called spinal cord compression. It is an emergency so if you have these symptoms, you need to contact your cancer specialist straight away or go to the accident and emergency department.
Read Also: What Do Skin Cancer Marks Look Like
What Is Skin Cancer
There are 2 main types of skin cancer: Non melanoma skin cancer and melanoma skin cancer.
This section is about non melanoma skin cancer.
Non melanoma skin cancers tend to develop most often on skin that’s exposed to the sun. There is a high cure rate for these cancers. It is important that you check your skin regularly.
How Do I Decrease My Risk
Similar to the amount of variation in recurrence or new primary melanoma development rates, theres also no clear way of preventing these events from happening. Creating a survivorship care plan with your healthcare team that includes a set of guidelines and timelines for future follow-up appointments, exams, tests, and screenings, and following these instructions, is a great way to help monitor for recurrence or new primary melanomas. Your healthcare team or survivorship care plan may also have information on what signs and symptoms to look for at home between appointments, as well as tips on how to perform self-exams of your skin and lymph nodes. Additionally, eliminating or reducing cancer risk-increasing behaviors, such as smoking, obesity, lack of exercise, and poor diet, may help reduce your overall risk of developing another cancer, both recurrent or new.1
If you are concerned about your risk for recurrence or the development of a new primary melanoma after youve been treated for melanoma skin cancer, contact your healthcare team and ask what your risk profile looks like, and what steps you can do to lower your chances of developing melanoma again.
Read Also: Are There Stages Of Basal Cell Carcinoma
After Skin Cancer Treatment
Most skin cancer is cured surgically in the dermatologist’s office. Of skin cancers that do recur, most do so within three years. Therefore, follow up with your dermatologist as recommended. Make an appointment immediately if you suspect a problem.
If you have advanced malignant melanoma, your oncologist may want to see you every few months. These visits may include total body skin exams, regional lymph node checks, and periodic chest X-rays and body scans. Over time, the intervals between follow-up appointments will increase. Eventually these checks may be done only once a year.
I’ve Been Diagnosed With Melanomawhat Happens Next
Doctors use the TNM system developed by the American Joint Committee on Cancer to begin the staging process. Its a classification based on three key factors:
T stands for the extent of the original tumor, its thickness or how deep it has grown and whether it has ulcerated.
What Is Breslow depth?
Breslow depth is a measurement from the surface of the skin to the deepest component of the melanoma.
Tumor thickness: Known as Breslow thickness or Breslow depth, this is a significant factor in predicting how far a melanoma has advanced. In general, a thinner Breslow depth indicates a smaller chance that the tumor has spread and a better outlook for treatment success. The thicker the melanoma measures, the greater its chance of spreading.
Tumor ulceration: Ulceration is a breakdown of the skin on top of the melanoma. Melanomas with ulceration are more serious because they have a greater risk of spreading, so they are staged higher than tumors without ulceration.
N indicates whether or not the cancer has already spread to nearby lymph nodes. The N category also includes in-transit tumors that have spread beyond the primary tumor toward the local lymph nodes but have not yet reached the lymph nodes.
M represents spread or metastasis to distant lymph nodes or skin sites and organs such as the lungs or brain.
After TNM categories are identified, the overall stage number is assigned. A lower stage number means less progression of the disease.
You May Like: How To Identify Basal Cell Carcinoma
What’s My Risk Of Developing A New Primary Melanoma
As far as developing new cancers, it has been estimated that individuals with melanoma have a 9-fold increase in risk in developing new, primary melanomas, as well as a 28% overall increase in risk of developing a new primary cancer that isnt melanoma, also referred to as a second cancer. Specifically, individuals with melanoma are at a higher risk of developing second cancers in the prostate gland, breasts, salivary glands, kidneys, and thyroid glands, as well as a higher risk of developing leukemia and non-Hodgkin lymphoma.4
Factors that contribute to the development of a new primary melanoma include gender, genetics, age, and original melanoma location. For example, the younger an individual is at original diagnosis, the greater their risk is of developing a new melanoma. This could be due to a genetic tendency to developing melanomas, since melanoma diagnosed in individuals 30 years old or younger is often due to genetic factors. Also, women who have had an original melanoma on the head or neck region are at a higher risk of developing subsequent primary melanomas. Additionally, the risk of developing a new primary melanoma decreases each year after diagnosis and treatment, however, individuals with melanoma are a higher risk of developing a new melanoma than the general population for up to 20 years.4
How Is Melanoma Diagnosed
Your doctor will check your skin to look for melanoma. If your doctor thinks that you have melanoma, he or she will remove a sample of tissue from the area around the melanoma. Another doctor, called a pathologist, will look at the tissue to check for cancer cells.
If your biopsy shows melanoma, you may need to have more tests to find out if it has spread to your lymph nodes.
Recommended Reading: How Many Types Of Skin Cancer Exist
Stages Of Melanoma Skin Cancer
Staging describes or classifies a cancer based on how much cancer there is in the body and where it is when first diagnosed. This is often called the extent of cancer. Information from tests is used to find out the size of the tumour, which parts of the skin have cancer, whether the cancer has spread from where it first started and where the cancer has spread. Your healthcare team uses the stage to plan treatment and estimate the outcome .
The most common staging system for melanoma skin cancer is the TNM system. For melanoma skin cancer there are 5 stages stage 0 followed by stages 1 to 4. Often the stages 1 to 4 are written as the Roman numerals I, II, III and IV. Generally, the higher the stage number, the more the cancer has spread. Talk to your doctor if you have questions about staging.
When describing the stage, doctors often use the words early stage, locoregional or metastatic.
Early stage means that the cancer is only in where it started and has not spread to other parts of the body. It includes stage 0, stage 1A, stage 1B, stage 2A, stage 2B and stage 2C melanoma skin cancers.
Locoregional means the cancer has spread to nearby lymph nodes, or it has spread to nearby areas of skin or lymph vessels. It includes stage 3 melanoma skin cancer.
Metastatic means that the cancer is in a part of the body farther from where it started. It includes stage 4 melanoma skin cancer.
Find out more about .
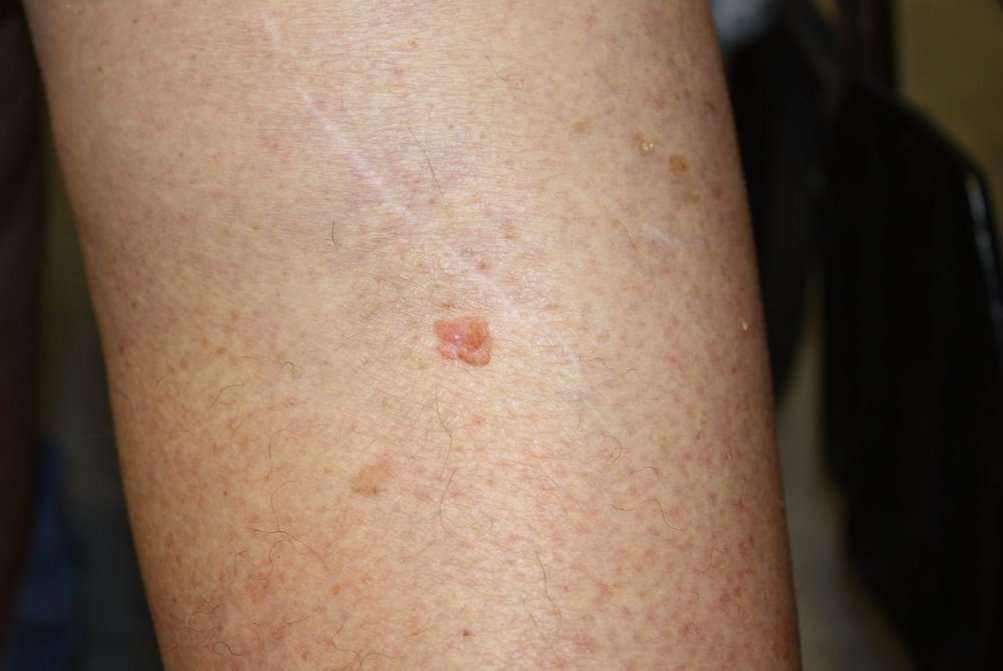
Possible Signs And Symptoms Of Melanoma
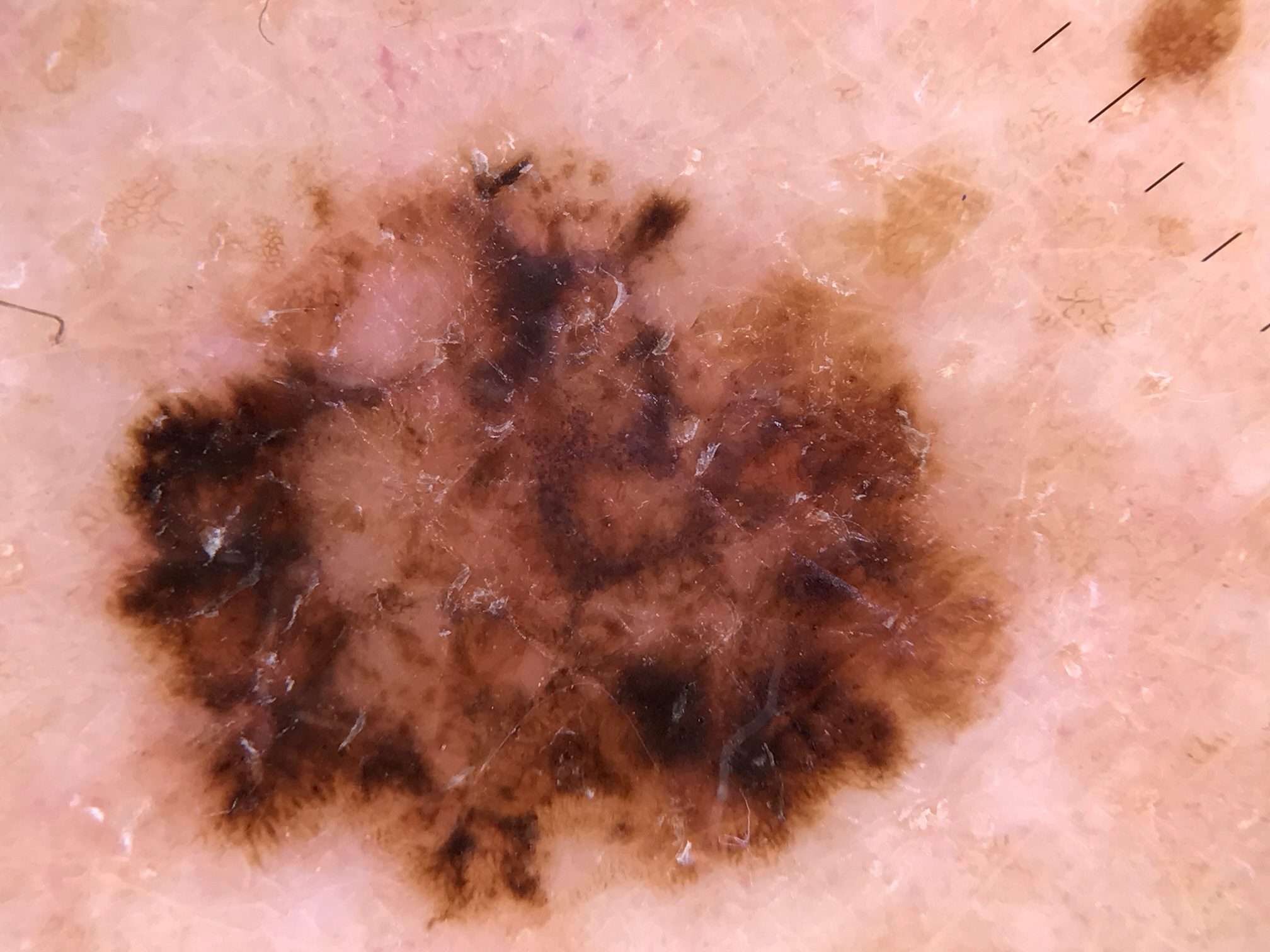
The most important warning sign of melanoma is a new spot on the skin or a spot that is changing in size, shape, or color.
Another important sign is a spot that looks different from all of the other spots on your skin .
If you have one of these warning signs, have your skin checked by a doctor.
The ABCDE rule is another guide to the usual signs of melanoma. Be on the lookout and tell your doctor about spots that have any of the following features:
- A is for Asymmetry: One half of a mole or birthmark does not match the other.
- B is for Border:The edges are irregular, ragged, notched, or blurred.
- C is for Color:The color is not the same all over and may include different shades of brown or black, or sometimes with patches of pink, red, white, or blue.
- D is for Diameter:The spot is larger than 6 millimeters across , although melanomas can sometimes be smaller than this.
- E is for Evolving: The mole is changing in size, shape, or color.
Some melanomas dont fit these rules. Its important to tell your doctor about any changes or new spots on the skin, or growths that look different from the rest of your moles.
Other warning signs are:
- A sore that doesnt heal
- Spread of pigment from the border of a spot into surrounding skin
- Redness or a new swelling beyond the border of the mole
- Change in sensation, such as itchiness, tenderness, or pain
- Change in the surface of a mole scaliness, oozing, bleeding, or the appearance of a lump or bump
Recommended Reading: How Do You Know If Melanoma Has Spread
Tools That Can Help You Find Melanoma On Your Skin
To help you find melanoma early, the American Academy of Dermatology developed the following:
Melanoma can look different on a childs skin. Taking this short quiz can help you hone your skills at finding childhood melanoma.
ImagesImages 1,3,4,5,6,7,8,10: Images used with permission of the American Academy of Dermatology National Library of Dermatologic Teaching Slides.
Image 2: Developed by the American Academy of Dermatology
Image 9: Used with permission of the Journal of the American Academy of Dermatology.
ReferencesBarnhill RL, Mihm MC, et al. Malignant melanoma. In: Nouri K, et al. Skin Cancer. McGraw Hill Medical, China, 2008: 140-167.
Gloster HM Jr, Neal K. Skin cancer in skin of color. J Am Acad Dermatol 2006 55:741-60.
National Comprehensive Cancer Network. NCCN guidelines for patients: Melanoma. 2018. Last accessed February 12, 2019.
Exams And Tests For Skin Cancer
If you think a mole or other skin lesion has turned into skin cancer, your primary care provider will probably refer you to a dermatologist. The dermatologist will examine any moles in question and, in many cases, the entire skin surface. Any lesions that are difficult to identify, or are thought to be skin cancer, may then be checked. Tests for skin cancer may include:
- The doctor may use a handheld device called a dermatoscope to scan the lesion. Another handheld device, MelaFind, scans the lesion then a computer program evaluates images of the lesion to indicate if it’s cancerous.
- A sample of skin will be taken so that the suspicious area of skin can be examined under a microscope.
- A biopsy is done in the dermatologist’s office.
If a biopsy shows that you have malignant melanoma, you may undergo further testing to determine the extent of spread of the disease, if any. This may involve blood tests, a chest X-ray, and other tests as needed. This is only needed if the melanoma is of a certain size.
Continued
Also Check: Can You Get Skin Cancer On Your Scalp
What Is A Melanocyte
Melanocytes are skin cells found in the upper layer of skin. They produce a pigment known as melanin, which gives skin its color. There are two types of melanin: eumelanin and pheomelanin. When skin is exposed to ultraviolet radiation from the sun or tanning beds, it causes skin damage that triggers the melanocytes to produce more melanin, but only the eumelanin pigment attempts to protect the skin by causing the skin to darken or tan. Melanoma occurs when DNA damage from burning or tanning due to UV radiation triggers changes in the melanocytes, resulting in uncontrolled cellular growth.
About Melanin
Naturally darker-skinned people have more eumelanin and naturally fair-skinned people have more pheomelanin. While eumelanin has the ability to protect the skin from sun damage, pheomelanin does not. Thats why people with darker skin are at lower risk for developing melanoma than fair-skinned people who, due to lack of eumelanin, are more susceptible to sun damage, burning and skin cancer.
Recurrent Basal Cell Carcinoma
Basal cell carcinomas are the most common type of skin cancer, according to the American Cancer Society. These cancers develop within the basal cell layer of the skin, in the lowest part of the epidermis.
Patients who have had basal cell carcinoma once have an increased risk of developing a recurrent basal cell cancer. Basal cell cancers may recur in the same location that the original cancer was found or elsewhere in the body. As many as 50 percent of cancer patients are estimated to experience basal cell carcinoma recurrence within five years of the first diagnosis.
Basal cell carcinomas typically grow slowly, and it is rare for them to metastasize or spread to nearby lymph nodes or other parts of the body. But early detection and treatment are important.
After completing treatment for basal cell carcinoma, it is important to perform regular self-examinations of the skin to look for new symptoms, such as unusual growths or changes in the size, shape or color of an existing spot. Skin cancers typically develop in areas of the body that are exposed to the sun, but they may also develop in areas with no sun exposure. Tell your oncologist or dermatologist about any new symptoms or suspicious changes you may have noticed.
- Have a history of eczema or dry skin
- Have been exposed to high doses of UV light
- Had original carcinomas several layers deep in the skin
- Had original carcinomas larger than 2 centimeters
Also Check: How Long Does It Take For Melanoma To Metastasize
When To Seek Medical Care For Skin Cancer
Many people, especially those who have fair coloring or have had extensive sun exposure, periodically check their entire body for suspicious moles and lesions.
Have your primary health care provider or a dermatologist check any moles or spots that concern you.
See your health care provider to check your skin if you notice any changes in the size, shape, color, or texture of pigmented areas .
If you have skin cancer, your skin specialist or cancer specialist will talk to you about symptoms of metastatic disease that might require care in a hospital.