Reducing Your Skin Cancer Risk
You can take steps to reduce your risk of skin cancer from exposure to UV radiation.
Use a combination of the 5 sun protection measures during the daily sun protection times to reduce your risk, including:
- Slip on sun-protective clothing that covers as much skin as possible.
- Slop on SPF30 broad-spectrum, water-resistant sunscreen. Apply sunscreen 20 minutes before you go outdoors and reapply it every 2 hours . Never use sunscreen on its own or to extend the time you spend in the sun.
- Slap on a broad-brimmed hat that protects the face, head, neck and ears.
- Seek shade.
- Slide on wrap-around sunglasses. Make sure they meet Australian/New Zealand Standard AS/NZS 1067. Optometry Australia recommends using eye protection all year.
UV levels are most intense during the middle of the day.
SunSmart and the Bureau of Meteorology issue daily sun protection times whenever UV index levels are 3 or higher. This is available as a free SunSmart app, or online at SunSmart, in the weather section of newspapers, or as a free website widget.
Winter activities such as skiing or snowboarding also pose a high risk of skin damage and sunburn. UV radiation is more intense at high altitude than at sea level. This is because the air is clearer and there is less atmosphere to absorb harmful UV rays. Read more about sun protection at the snow.
Sign Up For Our Newsletter Here
Examples include the armpits, around the base of the neck, underneath the breasts, and along the inguinal crease where the upper thigh meets the body. Skin tags may also be found on the eyelids.
Hormones may also play a role in developing skin tags as these growths seem to increase in pregnant women. And as with many medical conditions, there may be a genetic predisposition because skin tags often run in families.
Other articles by this author:
Q: How Might You Know If Melanoma Runs In Your Family
A: We are currently studying people who have had two or more melanomas in one person or in their family. People should consider joining this study if they have melanoma and have family members with other cancers like breast or kidney cancer.
My guess is that melanoma is going to end up being like the canary in the coal mine. Its the bell that rings, alerting you to a family with a higher predisposition for having a number of cancers especially in fairer-skinned Caucasian populations.
Read Also: Lobular Breast Cancer Survival Rate
How Do Cdkn2a Gene Mutations Cause Melanoma
CDKN2A encodes two distinct proteins:
Mutations in CDKN2A can disrupt the functions of either or both of these proteins.
INK4A inhibits the G1 phase of the cell cycle which is mediated by the G1 cyclin-dependent kinases 4/6 which phosphorylate and inactivate the retinoblastoma protein , thereby allowing entry into the S-phase of the cell cycle. The G1 cell cycle arrest phase must be bypassed before cell division.
Loss of INK4A function through mutation prevents the binding of INK4A to CDK4 and promotes RB activation through hyperphosphorylation resulting in unconstrained cell cycle progression.
ARF protein has been shown to promote the stabilisation of p53, a critical tumour suppressor and proapoptotic protein by preventing Mdm2 -mediated degradation of p53.
Inactivation of ARF leads to degradation of the p53 protein and rite of passage to unrestrained cell multiplication.
Families with ARF mutations appear to develop cutaneous melanoma and neural system tumours, whereas, in families with INK4 mutations, cutaneous melanoma and pancreatic cancer often cluster in the same pedigree.
A Dermatologist Can Tell You About Your Risks
If youre still wondering whether you should have genetic testing for melanoma, you may want to talk with your dermatologist. By talking about your concerns and risks, your dermatologist can help you decide whether this test would be helpful.
If genetic testing may be an option for you, your dermatologist can refer you to a qualified genetic counselor. A genetic counselor can talk with you about the benefits and limitations of testing.
1Swetter SM, Tsao H, et al. Guidelines of care for the management of primary cutaneous melanoma. J Am Acad Dermatol. 201. Articles in press.
ImagesGetty Images
ReferencesLeachman SA, Carucci J, et al. Selection criteria for genetic assessment of patients with familial melanoma. J Am Acad Dermatol. 2009 Oct 61:677e1-14.
National Comprehensive Cancer Network. NCCN Guidelines Melanoma. Last accessed March 27, 2017.
Ransohoff KJ, Jaju PD, et al. Familial skin cancer syndromes: Increased melanoma risk. J Am Acad Dermatol. 2016 74:423-34.
Swetter SM, Tsao H, et al. Guidelines of care for the management of primary cutaneous melanoma. J Am Acad Dermatol. 201. Articles in press.
Van Voorhees A. What should you know about hereditary melanoma? Dermatology World. 2016 26:20-4.
Recommended Reading: Invasive Ductal Carcinoma Grade 2 Survival Rate
Continue Learning About Skin Cancer Causes & Risk Factors
Important: This content reflects information from various individuals and organizations and may offer alternative or opposing points of view. It should not be used for medical advice, diagnosis or treatment. As always, you should consult with your healthcare provider about your specific health needs.
What Do Family Cancer Clinics Provide
Family cancer clinics provide counselling and information for families with a history of cancer on:
- inheriting cancer
- screening
- cancer risk reduction strategies.
They also provide genetic testing where appropriate. The clinics are conducted through the public hospital system and there is no direct cost to the patient for consultation or genetic testing.
Also Check: Skin Cancer Spreading To Lymph Nodes
How Common Are Cancers Caused By Inherited Faulty Genes
Cancers due to inherited faulty genes are much less common than cancers due to gene changes caused by ageing or other factors. Most cancers develop because of a combination of chance and our environment, not because we have inherited a specific cancer gene fault.
Genetic specialists estimate that between 5 and 10 in every 100 cancers diagnosed are linked to an inherited faulty gene.
Different gene faults increase the risk of different types of cancer. Some faults increase the risk by a small amount and some increase the risk much more.
Genes Mutations And Cancer
Cancer is a disease in which cells grow out of control. This happens because of changes in some of the genes inside cells. Genes are pieces of DNA that control how cells make the proteins the body needs to function, as well as how cells are kept in balance. Your genes affect things such as hair color, eye color, and height. They can also affect your chance of getting certain diseases, such as cancer.
Nearly every cell in your body has all of the genes you were born with. Although all cells have the same genes, different cells may use different genes. For example, muscle cells use different genes than skin cells use. The genes that the cell doesnt need are turned off and not used. The genes that the cell is using are activated or turned on.
An abnormal change in a gene is called a mutation. Mutations in a gene can affect how it functions. For example, a mutation might stop a gene from working. Or it might keep a gene turned on all the time . Either way, these can cause problems inside the cell.
Gene mutations can be either inherited or acquired.
Many family cancer syndromes are caused by inherited mutations in tumor suppressor genes. These are genes that normally keep cells under control by slowing down how often they divide , repairing DNA mistakes, or telling cells to die at the right time.
For more information about gene changes that can lead to cancer, see Genes and Cancer.
Don’t Miss: Whats Cancer Look Like
What Role Do Genes Play In Melanoma
Many cancers begin when one or more genes in a cell are mutated , creating an abnormal protein.
A person may either be born with a genetic mutation in all of their cells or acquire a genetic mutation in a single cell during his or her life sometimes as a result of exposure to environmental factors, such as UV radiation from the sun.
Most melanomas are considered sporadic, meaning that the damage to the genes occurs by chance after a person is born, and there is no risk of passing on the gene to a person’s children.
An increased risk of melanoma occurs when specific gene mutations are passed within a family from generation to generation. Such inherited melanoma is sometimes called familial melanoma.
Inherited risk of melanoma is suspected if two or more first-degree relatives are diagnosed with melanoma.
Many people who have an increased risk of melanoma never develop the disease only 10% of melanoma is familial.
Can Metastasis Be Prevented
Melanoma can spread âsilently,â meaning that you may not experience any symptoms of metastasis. Therefore, if youâve been treated for early-stage melanoma in the past, it is extremely important to perform regular self-examinations of your skin and lymph nodes, to keep all your appointments for checkups, and practice sun safety. There is nothing else an individual can do to prevent metastasis from being very diligent.
Catching a recurrence early greatly increases your chances of successful treatment. If the melanoma does spread, it is important to remain positive: remember that while the average prognosis is poor, some people do survive stage IV melanoma.
Skin Cancer Doctor Discussion Guide
Get our printable guide for your next doctorâs appointment to help you ask the right questions.
You May Like: Skin Cancer Prognosis
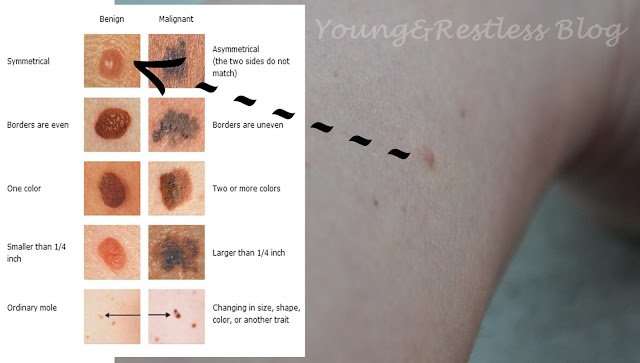
Melanoma Symptoms And Tips For Prevention
Melanoma can develop suddenly on skin that looks normal otherwise, or it may develop in or near a mole. The dermatology experts at Roswell Park suggest that you get in the habit of examining your skin using both a full-length mirror and a hand-held mirror so you can see every part of your body. Contact a dermatologist if you find new moles or if a mole begins bleeding, changes color or becomes itchy or painful. If youre at increased risk for melanoma, schedule routine annual visits with a dermatologist.
The Centers for Disease Control and Prevention recommends easy options for protection from UV radiation:
What Is Metastatic Melanoma
Metastatic melanoma occurs when the cancerous cells from the original tumor get loose, travel through the lymph or blood circulation, and start a new tumor somewhere else. Once it spreads, or metastasizes, the disease is known as metastatic melanoma. This type of melanoma may typically occur during stage III or stage IV. Common sites for metastases include the lymph nodes, lungs, liver, bones and brain.
About 106,110 adults in the United States will be diagnosed with melanoma in 2021, according to the American Society of Clinical Oncology . Approximately 4 percent of people are diagnosed with melanomas that have spread to distant parts of the body, according to the ASCO. This is the most advanced stage of metastatic melanoma.
The percentage of people diagnosed with melanoma that has spread to nearby lymph nodes is 8.5 percent, according to the National Cancer Institute . These cases have a slightly better prognosis.
From 2014 to 2018, the incidence rate of melanoma that had spread to distant parts of the body was 0.9 per 100,000 people, according to the NCI.
Melanoma tumors that have metastasized to other parts of the body are still considered melanoma. For example, melanoma found in the lungs is called metastatic melanoma of the lung or melanoma with lung metastases.
Read Also: Well-differentiated
Don’t Miss: Stage 4 Basal Cell Carcinoma Life Expectancy
Family History And Inherited Cancer Genes
-
Most cancers are caused by gene faults that happen during our lifetime
-
Some people have an increased risk of particular types of cancer because they have inherited a faulty gene
-
Your doctor can refer you to a genetic clinic if you have a strong family history of cancer
This information looks at how inherited faulty genes can cause cancer and what you can do if you have a strong family history of cancer.
Q: How Frequently Does Familial Melanoma Occur
A: Some research shows that about 1 to 2% of melanoma cases are inherited. Some literature says its higher, maybe closer to 12%.
Among my patients, I see two to three each week with cancer that has some kind of familial connection. When you add that up, the number is pretty significant. I would say its anywhere from 10 to 20%.
Don’t Miss: Melanoma On Face Prognosis
What Else Can Increase Your Risk Of Skin Cancer
Many cancers are caused by a combination of genetic and environmental factors. Although your genes can play a role in making you more susceptible to skin cancer, the environment plays a bigger role.
Exposure to ultraviolet radiation from the sun is the primary cause of skin cancer. Tanning beds, booths, and sunlamps also produce UV rays that can be equally harmful to your skin.
According to the National Human Genome Research Institute , skin cancer is related to your lifetime exposure to UV radiation.
Thats why even though the sun can damage your skin from an early age, many cases of skin cancer only appear after age 50.
UV rays from the sun can change or damage the DNA makeup of your skin cells, causing cancer cells to grow and multiply.
People who live in sunny places that get high amounts of UV radiation from the sun are at a higher risk for skin cancer.
Tyr Tyrp1 And Asip Genes
Recently, other genes involved with skin pigment have been identified that may also increase susceptibility to inherited melanoma.
These genes encode the following proteins: TYR , TYRP1 , and ASIP .
Tyrosinase is a copper-containing enzyme that catalyses the production of melanin and other pigments and is encoded by the TYR gene.
TYRP1 is a protein involved in melanin production and is encoded by the TYRP1 gene.
Tyrp1 is involved in stabilising the tyrosinase enzyme and modulating its catalytic activity. Tyrp1 also affects melanocyte proliferation and melanocyte cell death.
Agouti signalling protein is a product of the Agouti gene, also called ASIP. ASIP affects the quality of hair pigmentation and act as an inhibitor of the -melanocyte stimulating hormone.
Mutations in TYR, TYRP1 or ASIP genes can result in the production of abnormal proteins and increase melanoma risk.
Also Check: Stage Iiia Melanoma Prognosis
Thyroid Disease Is Often Hereditary
More than 75% of the time, patients with thyroid disease tell me that someone on one side of their family has thyroid disease, says Dr. Nasr.
The more family members that have thyroid disease, the greater the likelihood that there is a hereditary root. And the higher the chances the patient will experience a thyroid problem.
Autoimmune disorders seem to be a genetic link for some of the familial thyroid disorders, he notes. Autoimmune disorders occur when white blood cells go haywire and attack the cells that regulate body functions. The immune systems foul play could cause the thyroid gland to produce too much or too little hormone. So having an autoimmune disease may increase your risk for thyroid disease, Dr. Nasr says.
But this same action the white blood cells attacking bodycells could result in other autoimmune disorders like diabetes, lupus orrheumatoid arthritis, too.
In a family, the same person could have an autoimmunedisorder that causes hypothyroidism and another that causes diabetes, says Dr.Nasr. And you may have a different family member who has diabetes, but notthyroid disease.
The takeaway: Inform your healthcare provider if any autoimmune diseases run in your family, even if there isnt an obvious thyroid connection.
Having A Family History Of Melanoma
Our natural risk of illness depends in part on our genes the instructions that our bodies use to grow and repair themselves.
To decide the risk of illness such as melanoma, to family members, doctors look for signs of high-risk genes within the family.
Those signs are:
- Several cases of melanoma within a family.The more cases of melanoma the more likely there will be a high-risk gene in that family. However, more than one case might occur by chance alone or because the family live somewhere with a high environmental risk . Some families may also have family members with cancer of the pancreas.
- Three of more melanomas in a single family member.When a person develops multiple primary melanomas they may have a high-risk gene, but research has shown that in the absence of a family history of melanoma, most such people do not have a high risk gene such as CDKN2A: it is likely that many of these people have several low risk genes eg those associated with skin which tends to burn in the sun, and they have had quite a lot of sun exposure. In such a case, then the affected family members would be less likely to pass on a significant risk of melanoma to their children.
- Melanoma occurring earlier than usual.Most cases of melanoma are in people aged 50 or older. In families with high-risk genes then melanoma occurs a little earlier on average.
Referral to a specialist
Questions to consider:
What would the clinical geneticist or specialist dermatologist do?
Gene Testing
Recommended Reading: Skin Cancer Metastasis To Lymph Nodes
Diagnosis Of Metastatic Melanoma
Your care team may use several tests to diagnose metastatic melanoma.
If theres evidence of a primary tumor, a biopsy may be taken. For this, a small section of suspected cancerous skin is removed with a razor, scalpel or small punch tool. The removed tissue is examined under a microscope to determine whether its melanoma.
Additional tests are needed to determine whether the cancer is metastatic melanoma, or if theres no visible primary tumor. To test for metastatic melanoma, or melanoma that has spread to lymph nodes or distant parts of the body, your care team may perform the following tests.
- Lymph node mapping and sentinel lymph node biopsy : Your doctor may perform a physical exam of your lymph nodes and check for swelling or physical masses. If no tumors are found , an SLNB may be done. For an SLNB, a radioactive dye is injected to locate the primary tumor. Then, the doctor will remove the lymph nodes that the dye traveled to and check them for melanoma.
Donât Miss: Skin Cancer Perineural Invasion