The 4 Stages Of Melanoma
Two main things determine the stage of melanoma: The thickness or depth of the tumor and how far it has spread when its diagnosed, explains David Polsky, M.D., dermatologist at NYU Langone Medical Center in New York City. In stages 0, 1, and 2, the melanoma is limited to the skin. In stage 3, its spread to the lymph nodes, small structures throughout your body that help filter fluids and fight infection. In the most advanced stage, stage 4, melanoma cells have broken away from the original tumor, traveled through the body and formed a new tumor somewhere else.
Recognizing The Signs And Symptoms
The most noticeable sign of melanoma is the appearance of a new mole or a change in an existing mole or birthmark. People should be aware of any pigmented areas on the skin that appear abnormal in color, shape, size, or texture.
People with stage 4 melanoma may also have ulcerated skin, which is skin with tiny breaks on the surface. These ulcerations can bleed.
Another sign is swollen or hard lymph nodes, which a doctor can confirm by carrying out a physical examination. Other tests include blood tests and imaging scans to confirm the presence of cancer and check how much it has spread.
Red Flag #: Headaches Or Visual Changes
Just like the liver, not everyone will notice symptoms of melanoma spreading to the brain. But when symptoms do show up, its usually in the form of headaches, problems with eyesight, paralysis on one side of the body, or seizures. If someone simply has a headache, that doesnt mean they have advanced stage melanoma, Dr. Yushak says. But if its a headache thats not going away after a week, and you never have headaches, then thats something that definitely needs to be checked out.
Read Also: Can You Die From Basal Cell Skin Cancer
Survival And Clinical Outcome
Fifty-nine patients had died of melanoma progression at the time of the analysis, among which 32 died with progressing brain metastases. The median overall survival duration from the time of initial brain metastasis was 12.8 months , and the median overall survival duration from the time of initial melanoma diagnosis was 60.5 months for all 79 patients. The median overall survival durations from the time of craniotomy and stereotactic radiosurgery were 17.3 months and 15.4 months , respectively. The median survival durations of patients who received anti-CTLA-4 antibody, anti-PD-1 antibody and BRAF inhibitor after the diagnosis of brain metastasis were 19.2 months , 37.9 months and 12.7 months , respectively. Tables and describe the outcomes of the entire cohort as well as specific subsets of patients. Figures and illustrate the Kaplan-Meier curves of overall survival for all patients and for those who were treated with or without anti-PD-1 therapy, respectively.
Fig. 1
How Is Metastasis Detected
If your doctor suspects that your melanoma may have spread, there are several tools available to verify the diagnosis. These include a blood test for lactate dehydrogenase , which increases when melanoma metastasizes, and imaging studies, such as chest X-ray, computed tomography , magnetic resonance imaging , positron emission tomography and ultrasound.
The doctor may also need to take a sample of your lymph nodes, using a procedure called “sentinel lymph node mapping.” If confirmed, there are many treatments available, including chemotherapy, immunotherapy, radiation therapy and surgery.
Read Also: What Is Stage 2 Melanoma Skin Cancer
Symptoms If Cancer Has Spread To The Lymph Nodes
Lymph nodes are part of a system of tubes and glands in the body that filters body fluids and fights infection.
The most common symptom if cancer has spread to the lymph nodes is that they feel hard or swollen. Swollen lymph nodes in the neck area can make it hard to swallow.
Cancer cells can also stop lymph fluid from draining away. This might lead to swelling in the neck or face due to fluid buildup in that area. The swelling is called lymphoedema.
How Melanoma Moves From Its Original Site
When a tumor gets too big, it requires more oxygen and nutrients to survive. This is when the tumor sends out signals that cause new blood vessels to grow into the tumor , bringing the nutrients and oxygen to it.
Read more about: What is melanoma?
After angiogenesis occurs, cancer cells are now able to break off and enter the bloodstream. They can also break off and spread through the lymphatic system . When this happens, the cancer cells can now settle and take root in a new area of the body.
According to the American Cancer Society, three things need to happen in order for the cancer cells to metastasize in a new area.
One: they need to attach to the wall of a blood or lymph vessel and move through it into a new organ.
Two: they need to have the necessary nutrients to grow on the new site.
Three: They must resist attacks from the immune system.
If the cancer cells manage to do all of these things, then a new tumor will develop. Typically, it will look slightly different from the cancer cells in the original tumor as a result of its journey.
You May Like: What Is The Survival Rate For Invasive Ductal Carcinoma
I’ve Been Diagnosed With Melanomawhat Happens Next
Doctors use the TNM system developed by the American Joint Committee on Cancer to begin the staging process. Its a classification based on three key factors:
T stands for the extent of the original tumor, its thickness or how deep it has grown and whether it has ulcerated.
What Is Breslow depth?
Breslow depth is a measurement from the surface of the skin to the deepest component of the melanoma.
Tumor thickness: Known as Breslow thickness or Breslow depth, this is a significant factor in predicting how far a melanoma has advanced. In general, a thinner Breslow depth indicates a smaller chance that the tumor has spread and a better outlook for treatment success. The thicker the melanoma measures, the greater its chance of spreading.
Tumor ulceration: Ulceration is a breakdown of the skin on top of the melanoma. Melanomas with ulceration are more serious because they have a greater risk of spreading, so they are staged higher than tumors without ulceration.
N indicates whether or not the cancer has already spread to nearby lymph nodes. The N category also includes in-transit tumors that have spread beyond the primary tumor toward the local lymph nodes but have not yet reached the lymph nodes.
M represents spread or metastasis to distant lymph nodes or skin sites and organs such as the lungs or brain.
After TNM categories are identified, the overall stage number is assigned. A lower stage number means less progression of the disease.
What Kind Of Treatment Will I Need
There are many ways to treat melanoma. The main types of treatment are:
- Surgery
Most early stage melanomas can be treated with surgery alone. More advanced cancers need other treatments.
The treatment plan thats best for you will depend on:
- The stage of the cancer
- The results of lab tests on the cancer cells
- The chance that a type of treatment will cure the melanoma or help in some way
- Your age
- Other health problems you have
- Your feelings about the treatment and the side effects that come with it
Don’t Miss: Small Blue Cell Tumor Prognosis
Clinical Considerations In Melanoma Metastasis
Improvements in awareness have increased detection of melanoma, such that many melanomas are diagnosed early in disease progression . Though surgical excision is generally thought to be curative in these patients, a subset will develop recurrent disease. While melanomas rarely recur locally at the site of excision, they often recur as metastases at distant sites . Even in Stage IA melanoma patients, who have a 20-year survival rate of at least 90%, recurrences of disease still occur, often a decade or more after the removal of the primary tumor .
Melanoma metastasis cause the vast majority of morbidity and mortality associated with this disease. The presence of metastasis to visceral sites predicts poor outcome in melanoma . The one-year survival rates in melanoma patients with clinically apparent metastasis to one, two, or three different visceral sites is: 36%, 13%, and 1%, respectively . The most important tumor intrinsic variable that can predict metastatic recurrence in early melanomas is the thickness of the tumor . Prognosis is inversely proportional to tumor thickness. Strikingly, differences of only 12 mm in the thickness can alter prognosis substantially .
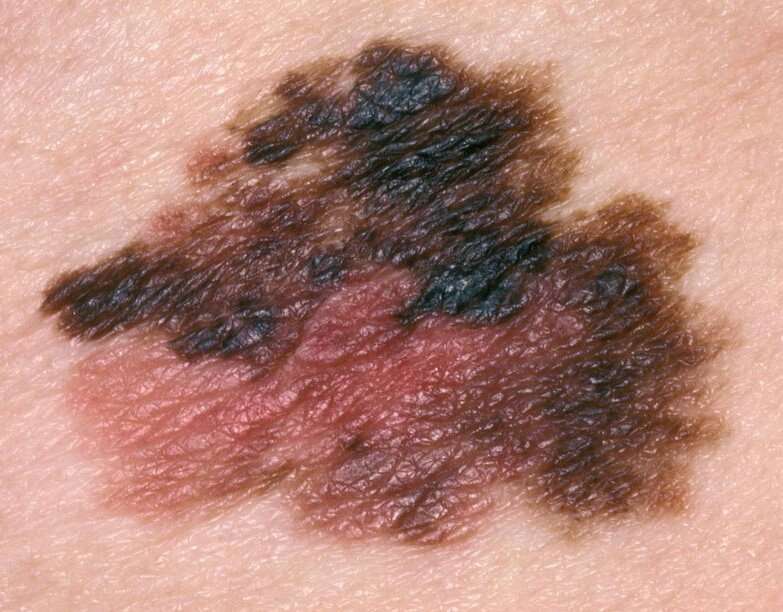
What Are The Symptoms Of Metastatic Melanoma
Many people find out they have melanoma when symptoms prompt them to visit the doctor.
They may be concerned about a mole that is painful, itchy, or bleeding that oozes or becomes scaly or lumpy or that shows other troubling signs.
Doctors looks for evidence of cancer in moles using whats called the ABCDE method:
- A It is asymmetrical.
- B It has an irregular border.
- C It contains more than one color or is an unusual color.
- D Its diameter is unusually big.
- E It evolves, changing size, color, shape, or another characteristic.
These are all traits that distinguish a cancerous mole from a benign one.
Its possible that by the time a physician diagnoses melanoma on the skin, cancer cells have already spread to other parts of the body. Melanoma can also appear in a different part of the body after initial diagnosis and treatment.
People with metastatic melanoma may feel tired or unwell in general. They also may have specific symptoms based on where in the body the cancer cells have spread. Some parts of the body that may be affected by metastatic melanoma include:
You May Like: What Is Melanoma In The Brain
Complementary And Alternative Treatments
It’s common for people with cancer to seek out complementary or alternative treatments. When used alongside your conventional cancer treatment, some of these therapies can make you feel better and improve your quality of life. Others may not be so helpful and in some cases may be harmful. It is important to tell all your healthcare professionals about any complementary medicines you are taking. Never stop taking your conventional treatment without consulting your doctor first.All treatments can have side effects. These days, new treatments are available that can help to make many side effects much less severe than they were in the past.
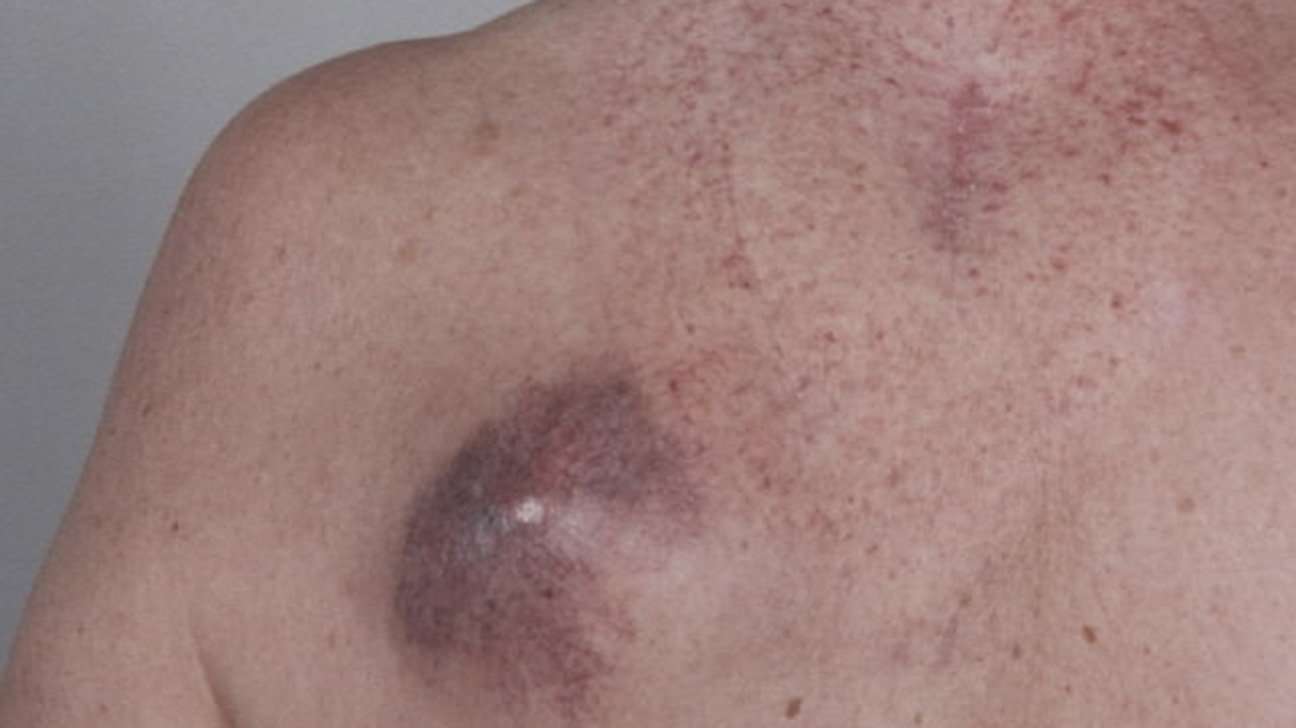
What Are The Possible Complications Of Metastatic Squamous Cell Carcinoma Of Skin
The possible complications due to Metastatic Squamous Cell Carcinoma of Skin could be:
- The metastasis can occur to any part of the body
- Large lesions may ulcerate and bleed resulting in superimposed bacterial or fungal infections
- Tumors that invade into nerves have higher chances of recurrence and metastasis
- Severely infiltrated or metastasized tumors may affect many body functions, depending on their location
Recommended Reading: Stage 5 Cancer Symptoms
Mouse Models Mimic Metastasis Of Human Melanoma
Metastasis is a highly inefficient process in that the vast majority of cancer cells that try to migrate die before they ever have an opportunity to form a tumor, Dr. Morrison said.
Dr. Morrisons team found previously that one factor limiting the survival of melanoma cells circulating in the blood is that the cells experience a high level of oxidative stress. Oxidative stressan imbalance between free radicals and antioxidants in the bodycauses chemical reactions that can damage proteins, DNA, and lipids in cells and disrupt normal cell processes. However, precisely how oxidative stress kills circulating melanoma cells was not known.
For their studies, the team used a mouse model of metastasis created by transplanting melanoma cells from humans beneath the skin of specially bred mice with weakened immune systems. These mice were used to avoid having the transplanted human cells seen as foreign and attacked by the immune system. The team also used a second mouse model created by transplanting mouse melanoma cells into mice with normal immune systems.
Comparing these two mouse models let the researchers control for potential effects of the immune system on the spread of melanoma, Dr. Salnikow explained.
The study was supported in part by NCIs Patient-Derived Models of Cancer program, which promotes the development of animal models that more closely mirror how tumor cells behave in humans.
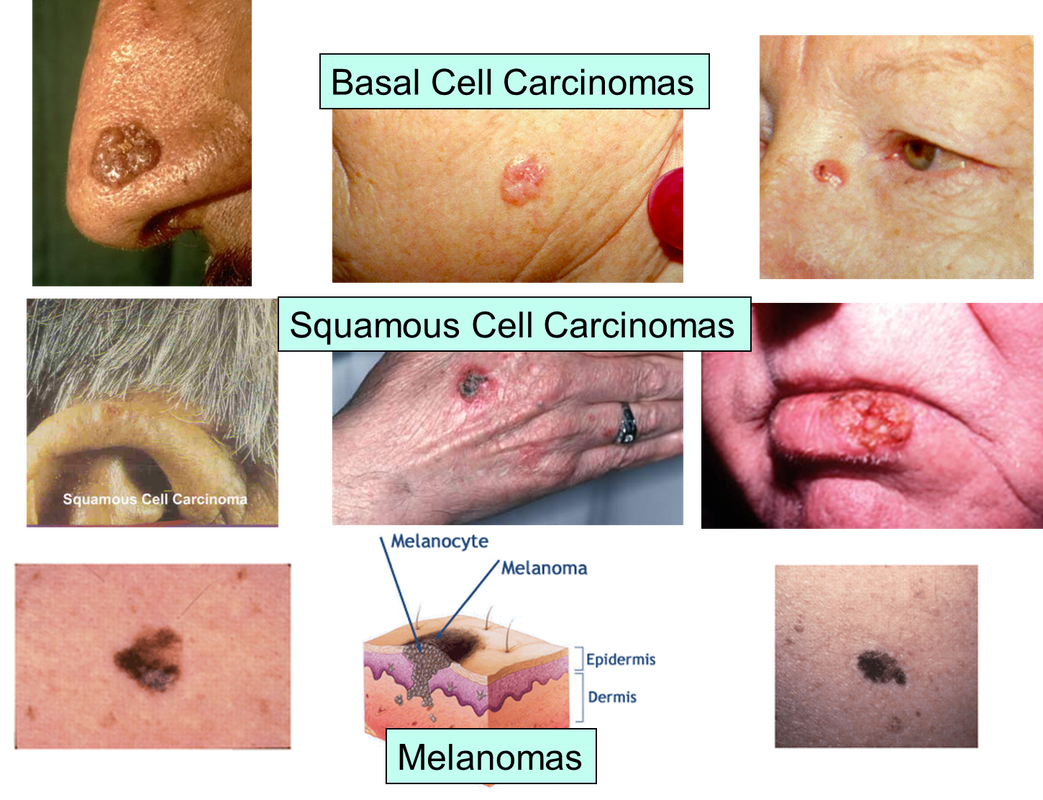
Are There Different Kinds Of Skin Cancer
There are many types of skin cancer. Your doctor can tell you more about the type of skin cancer you have.
Basal cell and squamous cell skin cancers are much more common than melanoma and dont often spread to other parts of the body. Melanoma is more deadly because it is more likely to spread to other parts of the body.
Read Also: How Long Does It Take Melanoma To Metastasize
How Does The Doctor Know I Have Melanoma
A new spot on your skin or a spot thats changing in size, shape, or color may be a warning sign of melanoma. If you have any of these changes, have your skin checked by a doctor.
The doctor will ask you questions about when the spot on your skin first showed up and if it has changed in size or the way it looks. The rest of your skin will be checked. During the exam your doctor will check the size, shape, color and texture of any skin changes. If signs are pointing to melanoma, more tests will be done.
Stop Tumors In Their Tracks
Every melanoma has the potential to become deadly, but the difference between an in situ melanoma and one that has begun to metastasize cannot be overstated. There is a drastic change in the survival rate for the various stages of tumors, highlighting the importance of detecting and treating melanomas before they have a chance to progress. Its impossible to predict exactly how fast a melanoma will move from stage to stage, so you should be taking action as soon as possible.
To be sure youre spotting any potential skin cancers early, The Skin Cancer Foundation recommends monthly skin checks, and scheduling an annual total-body skin-exam with a dermatologist. These skin exams can help you take note of any new or changing lesions that have the potential to be cancerous, and have them biopsied and taken care of before they can escalate.
Trust your instincts and dont take no for an answer, Leland says. Insist that a doctor biopsy anything you believe is suspicious.
Read Also: What Is The Survival Rate For Invasive Ductal Carcinoma
Signs And Symptoms Of Melanoma
The most common sign of melanoma is the appearance of a new mole or a change in an existing mole.
This can happen anywhere on the body, but the most commonly affected areas are the back in men and the legs in women.
Melanomas are uncommon in areas that are protected from sun exposure, such as the buttocks and the scalp.
In most cases, melanomas have an irregular shape and are more than 1 colour.
The mole may also be larger than normal and can sometimes be itchy or bleed.
Look out for a mole that gradually changes shape, size or colour.
Superficial spreading melanoma are the most common type of melanoma in the UK.
They’re more common in people with pale skin and freckles, and much less common in people with darker skin.
They initially tend to grow outwards rather than downwards, so they do not pose a problem.
But if they grow downwards into the deeper layers of skin, they can spread to other parts of the body.
You should see a GP if you have a mole that’s getting bigger, particularly if it has an irregular edge.
Topical Diphencyprone For Melanoma
Topical diphenylcyclopropenone or diphencyprone in various concentrations in solution or cream may be useful for small cutaneous melanoma metastases. The first application sensitises the patient to the chemical over about 10 days. Further applications applied to the lesions at weekly intervals cause allergic contact dermatitis, which can be very itchy and uncomfortable and may generalise. When effective, existing treated lesions stop enlarging and may shrink or disappear. Dramatic responses have been reported including regression of involved lymph nodes.
Intralesional immunotherapy for melanoma metastases using T-VEC, Allovectin-7® and Rose Bengal is under investigation.
Don’t Miss: Mayo Clinic Skin Cancer
Prevalence And Risk Factors
The incidence of melanoma is increasing across all ages, including a more than 600% increase in young adults from 1970 to 2009 . Melanoma is the sixth most common cancer in men and women and the second most common cancer in women ages 20 to 29 in the United States.
Based on the most recent US data, there will be about 178,560 new cases of melanoma in 2018: 87,290 in situ and 91,270 invasive. At current rates, 1 in 27 white men and 1 in 42 white women will develop an invasive melanoma over a lifetime. An estimated 9,320 people will die of melanoma in 2018: 5,990 men and 3,330 women. Apart from these statistics, if melanoma is detected and treated before it invades the deeper layers of skin, the 5-year survival rate is 99%.2,3
The primary risk factor for melanoma is exposure to UV radiation . Most melanomas arise in previously normal skin, and only 20% to 30% arise from pre-existing nevi. Although there are several genetic syndromes that predispose individuals to melanoma, these account for less than 15% of melanomas. These syndromes include xeroderma pigmentosa and familial atypical mole-melanoma syndrome .2,3
What Will Happen After Treatment
Youll be glad when treatment is over. For years after treatment, you will see your cancer doctor. Be sure to go to all of these follow-up visits. You will have exams, blood tests, and maybe other tests to see if the cancer has come back.
At first, your visits may be every few months. Then, the longer youre cancer-free, the less often the visits are needed. After 5 years, they may be done once a year.
Having cancer and dealing with treatment can be hard, but it can also be a time to look at your life in new ways. You might be thinking about how to improve your health. Call us at 1-800-227-2345 or talk to your cancer care team to find out what you can do to feel better.
You cant change the fact that you have cancer. What you can change is how you live the rest of your life making healthy choices and feeling as good as you can.
Recommended Reading: Can You Die From Basal Cell Skin Cancer