Metastatic Behavior In Melanoma: Timing Pattern Survival And Influencing Factors
Faruk Tas
1Institute of Oncology, Istanbul University, 34390 Istanbul, Turkey
Abstract
Metastatic melanoma is a fatal disease with a rapid systemic dissemination. This study was conducted to investigate the metastatic behavior, timing, patterns, survival, and influencing factors in MM. 214 patients with MM were evaluated retrospectively. Distant metastases were the most frequent for patients initially metastatic. The median and 1-year survival rates of initially MM patients were 10 months and 41%, respectively. The median time to metastasis for patients with localized disease was 28 months. The timing of appearance of metastases varied minimally; however, times to metastases for distant organs varied greatly. For the first metastatic pathway, more than half of the primary metastases were M1A . These findings were in contrast to the results compared with those with metastatic in diagnosis . The median and 1-year survival rates of all patients were 12 months and 49%, respectively. Outcome was higher in M1A than visceral metastases . In conclusion, the fact that over half of all recurrences/metastases occurred within 3 years urges us to concentrate follow-up in the early time periods following diagnosis. Because the clinical behavior of MM is variable, the factors for survival consisting of site and number of metastases should be emphasized.
1. Introduction
2. Material and Methods
3.1. Metastases at Presentation
3.2. Metastases during Follow-Up
| From |
4. Discussion
Risk Factors For Metastatic Melanomas
You cannot get metastatic melanoma without first having melanoma, though the primary melanoma may be so small its undetectable. Major risk factors for melanomas include:
- Light skin, light-colored hair or light-colored eyes
- Skin prone to burning easily
- Multiple blistering sunburns as a child
- Family history of melanoma
- Frequent exposure to sun or ultraviolet radiation;
- Certain genetic mutations
- Exposure to environmental factors, such as radiation or vinyl chloride
Other factors have been connected with increased metastasis. In a 2018 study in the Anais Brasileiros de Dermatologia and a 2019 study in the Journal of the National Cancer Institute, the following factors were associated with higher levels of metastasis:
- Male gender
- Primary tumor thickness of more than 4 mm
- Nodular melanoma, which is a specific subtype that a care team would identify
- Ulceration of the primary tumor
What Causes Metastatic Melanoma
Anyone can get melanoma, but most cases of melanoma are caused by UV radiation from sunlight; some studies even put incidences of skin cancer caused by sun exposure at around 95%. The UV rays from the sun damage skin cells ability to repair DNA. When this happens, gene mutations can occur and the risk of cancer increases.
The risk of melanoma is higher in fair-skinned people as they have less melanin in their skin to protect from the suns rays. Risk is also higher if there is a history of melanoma in the family as gene mutations are often passed down from one generation to the next.
Read Also: Does Skin Cancer Itch And Burn
What Will Happen After Treatment
Youll be glad when treatment is over. For years after treatment, you will see your cancer doctor. Be sure to go to all of these follow-up visits. You will have exams, blood tests, and maybe other tests to see if the cancer has come back.
At first, your visits may be every few months. Then, the longer youre cancer-free, the less often the visits are needed. After 5 years, they may be done once a year.
Having cancer and dealing with treatment can be hard, but it can also be a time to look at your life in new ways. You might be thinking about how to improve your health. Call us at 1-800-227-2345 or talk to your cancer care team to find out what you can do to feel better.
You cant change the fact that you have cancer. What you can change is how you live the rest of your life making healthy choices and feeling as good as you can.
Many Melanomas Dont Require Immediate Treatment
Many people have this concept that all melanomas are extremely rapidly growing cancers, says Dr. Marghoob. They think that waiting even one day after the diagnosis of melanoma can be fatal.
While some subtypes of melanoma do grow extremely fast, says Dr. Marghoob, most early melanomas dont require immediate treatment, allowing ample time to detect, treat, and cure them. Dr. Marghoob advises checking your skin on a monthly basis. If you notice a changing spot on your skin, dont delay in getting it checked out by a dermatologist, he says. And if your doctor does think you may have a melanoma, know that for most people its not necessary to rush to treatment. Most people can take the time they need to meet with doctors and understand their options.
You May Like: What Are The Chances Of Getting Skin Cancer
The 4 Stages Of Melanoma
Two main things determine the stage of melanoma: The thickness or depth of the tumor and how far it has spread when its diagnosed, explains David Polsky, M.D., dermatologist at NYU Langone Medical Center in New York City. In stages 0, 1, and 2, the melanoma is limited to the skin. In stage 3, its spread to the lymph nodes, small structures throughout your body that help filter fluids and fight infection. In the most advanced stage, stage 4, melanoma cells have broken away from the original tumor, traveled through the body and formed a new tumor somewhere else.
How Long Does It Take For Melanoma To Spread To Brain
Ask U.S. doctors your own question and get educational, text answers â it’s anonymous and free!
Ask U.S. doctors your own question and get educational, text answers â it’s anonymous and free!
HealthTap doctors are based in the U.S., board certified, and available by text or video.
Don’t Miss: Where Does Skin Cancer Start
How Long Does Melanoma Take To Spread
Ask U.S. doctors your own question and get educational, text answers â it’s anonymous and free!
Biological Therapies And Melanoma
Biological therapies are treatments using substances made naturally by the body. Some of these treatments are called immunotherapy because they help the immune system fight the cancer, or they occur naturally as part of the immune system.;There are many biological therapies being researched and trialled, which in the future may help treat people with melanoma. They include monoclonal antibodies and vaccine therapy.;
You May Like: What Does Stage 4 Skin Cancer Look Like
Clinical Considerations In Melanoma Metastasis
Improvements in awareness have increased detection of melanoma, such that many melanomas are diagnosed early in disease progression . Though surgical excision is generally thought to be curative in these patients, a subset will develop recurrent disease. While melanomas rarely recur locally at the site of excision, they often recur as metastases at distant sites . Even in Stage IA melanoma patients, who have a 20-year survival rate of at least 90%, recurrences of disease still occur, often a decade or more after the removal of the primary tumor .
Melanoma metastasis cause the vast majority of morbidity and mortality associated with this disease. The presence of metastasis to visceral sites predicts poor outcome in melanoma . The one-year survival rates in melanoma patients with clinically apparent metastasis to one, two, or three different visceral sites is: 36%, 13%, and 1%, respectively . The most important tumor intrinsic variable that can predict metastatic recurrence in early melanomas is the thickness of the tumor . Prognosis is inversely proportional to tumor thickness. Strikingly, differences of only 12 mm in the thickness can alter prognosis substantially .
Early Detection Prevents Melanoma From Spreading
While there are still many mysteries when it comes to why and how melanoma develops, it is certain that the sooner melanoma is discovered, the lower the chances of it spreading and becoming deadly. Thats why its essential to perform regular skin checks and know the symptoms of melanoma so you can catch it early.
Also Check: How Bad Is Basal Cell Carcinoma
Prevalence And Risk Factors
The incidence of melanoma is increasing across all ages, including a more than 600% increase in young adults from 1970 to 2009 . Melanoma is the sixth most common cancer in men and women and the second most common cancer in women ages 20 to 29 in the United States.
Based on the most recent US data, there will be about 178,560 new cases of melanoma in 2018: 87,290 in situ and 91,270 invasive. At current rates, 1 in 27 white men and 1 in 42 white women will develop an invasive melanoma over a lifetime. An estimated 9,320 people will die of melanoma in 2018: 5,990 men and 3,330 women. Apart from these statistics, if melanoma is detected and treated before it invades the deeper layers of skin, the 5-year survival rate is 99%.2,3
The primary risk factor for melanoma is exposure to UV radiation . Most melanomas arise in previously normal skin, and only 20% to 30% arise from pre-existing nevi. Although there are several genetic syndromes that predispose individuals to melanoma, these account for less than 15% of melanomas. These syndromes include xeroderma pigmentosa and familial atypical mole-melanoma syndrome .2,3
Does Ocular Melanoma Spread To The Brain
However, it is found that ocular melanoma can spread to any organ in the body. After the liver, common sites where eye cancer cells can travel are the lung, brain, and bones. Around 50% of ocular melanoma patients will develop metastasis within 15 years of their original medical diagnosis. Once the liver is involved, cancer becomes incurable. However, if metastatic disease is detected in the early phase, there are a few localized and systemic treatment procedures available that may improve the life expectancy of the patient and help in the improvement of the lifestyle for patients.
Regardless of the treatment options selected, ocular melanoma may represent lasting complications, even for patients who have a good prognosis with cancer. Patients can develop glaucoma as its complication, which is caused by the pressure of tumors within the eye, leading to pain. If surgery is conducted to remove these cancer cells, patients may have the risk of full or segmented vision loss as the function of the cranial nerves that control the muscles around the eye may be lost. If the ocular melanoma spreads beyond the eye, the treatment depends on the site it has traveled. It gets more complicated to treat. While it most often affects the liver, in a few cases of metastasis, it can also go to the brain, which becomes more complicated to treat.
Recommended Reading: What Are The Symptoms Of Melanoma Skin Cancer
Diagnosis And Staging What It Means For You
How is melanoma diagnosed?
To diagnose melanoma, a dermatologist biopsies the suspicious tissue and sends it to a lab, where a dermatopathologist determines whether cancer cells are present.
After the disease is diagnosed and the type of melanoma is identified, the next step is for your medical team to identify the stage of the disease. This may require additional tests including imaging such as PET scans, CT scans, MRIs and blood tests.
The stage of melanoma is determined by several factors, including how much the cancer has grown, whether the disease has spread and other considerations. Melanoma staging is complex, but crucial. Knowing the stage helps doctors decide how to best treat your disease and predict your chances of recovery.
Melanoma Can Go Away On Its Own
Melanoma on the skin can spontaneously regress, or begin to, without any treatment. Thats because the bodys immune system is able launch an assault on the disease thats strong enough to spur its retreat. Unfortunately, sometimes this happens only after the disease has spread to other parts of the body, such as the liver, lungs, bones, or brain.;
The observation that the immune system can cause melanoma to regress was one of the key insights that led to the development of immunotherapy as a successful treatment for melanoma, explains Dr. Marghoob. The thinking went, if the immune system can get rid of melanoma on its own, there must also be a way to enhance the immune systems natural ability to fight melanoma. This eventually led researchers to develop drugs designed to enhance the immune systems ability to successfully fight melanoma that has spread.
Don’t Miss: When Squamous Cell Carcinoma Spreads
Immunotherapies Targeting Melanoma Post Encouraging Results New Data Show
Most cancer cells die when they leave the primary tumor and enter the bloodstream. For unknown reasons, the journey causes severe oxidative stress , biologist Sean Morrison of the Childrens Medical Center Research Institute at the University of Texas Southwestern Medical Center found in a 2015 study. Oxidative stress kills them, said Morrison, who also led the new research. The vast majority of cells die before they have an opportunity to grow at a distant site.
Vast majority is not all, however, and it takes only a few cancer cells to seed a potentially fatal metastasis. If scientists could discover what separates tumor cells that die en route from those that reach their destination, Morrison figured, it might be possible to prevent metastasis, which is responsible for more than 90 percent of all cancer deaths.
Although immunotherapies are more successful against metastatic melanoma than most other cancers, only about one-quarter of patients respond, and melanoma will kill more than 7,000 people in the U.S. this year.
How Fast Melanoma Spreads
Some forms of melanoma can spread quickly, though the exact timeline will depend on your individual health situation. The timeline can be impacted by factors like your age, family history, any underlying medical conditions you may have, as well as what kind of melanoma you have.
During the diagnosis process, your dermatologist will determine what stage your cancer is at. The stage of your melanoma indicates what kind of treatment youll need.
Melanoma can spread quickly and be difficult to treat at later stages, so its important to seek treatment immediately after diagnosis, even if youre only at Stage 0 or Stage 1.
Protect the skin youre in.
Skincare is healthcare
Read Also: Can You Die From Basal Cell Skin Cancer
What Are The Melanoma Stages And What Do They Mean
Early melanomas
Stage 0 and I are localized, meaning they have not spread.
- Stage 0: Melanoma is localized in the outermost layer of skin and has not advanced deeper. This noninvasive stage is also called melanoma in situ.
- Stage I: The cancer is smaller than 1 mm in Breslow depth, and may or may not be ulcerated. It is localized but invasive, meaning that it has penetrated beneath the top layer into the next layer of skin. Invasive tumors considered stage IA are classified as early and thin if they are not ulcerated and measure less than 0.8 mm.
Find out about treatment options for early melanomas.
Intermediate or high-risk melanomas
Localized but larger tumors may have other traits such as ulceration that put them at high risk of spreading.
- Stage II: Intermediate, high-risk melanomas are tumors deeper than 1 mm that may or may not be ulcerated. Although they are not yet known to have advanced beyond the primary tumor, the risk of spreading is high, and physicians may recommend a sentinel lymph node biopsy to verify whether melanoma cells have spread to the local lymph nodes. Thicker melanomas, greater than 4.0 mm, have a very high risk of spreading, and any ulceration can move the disease into a higher subcategory of stage II. Because of that risk, the doctor may recommend more aggressive treatment.
Learn more about;sentinel lymph node biopsy;and melanoma treatment options.
Advanced melanomas
Has Anyone Survived Melanoma 4
Prognosis: Stage IV melanoma is very difficult to cure as it has already spread to other parts of the body. However, a small number of people respond well to treatment, achieve No Evidence of Disease , and survive for many years following diagnosis.
Don’t Miss: Is Squamous Cell Carcinoma Treatable
Why Are Brain Metastases So Difficult To Treat
There are several potential reasons:
- There is growing evidence that brain tumors are very different from tumors in other parts of the body and may need to be treated differently.
- The brain looks familiar. Melanocytes arise from the same part of the early embryo as the brain, so the brain might be a very natural environment for melanoma tumors to grow in.
- Often, by the time a patient first exhibits symptoms, s/he already has multiple lesions, not just one.
- Brain metastases tend to be very aggressive and even a small increase in their size can cause more symptoms.
- The brain has many defenses to reduce the penetration of harmful substances. This system is called the blood-brain-barrier, and also it prevents many medications from entering the brain.
- Treatment options may damage surrounding normal tissue and have significant impact on the quality of life.
What Else Should I Know About Treatment For Advanced Melanoma
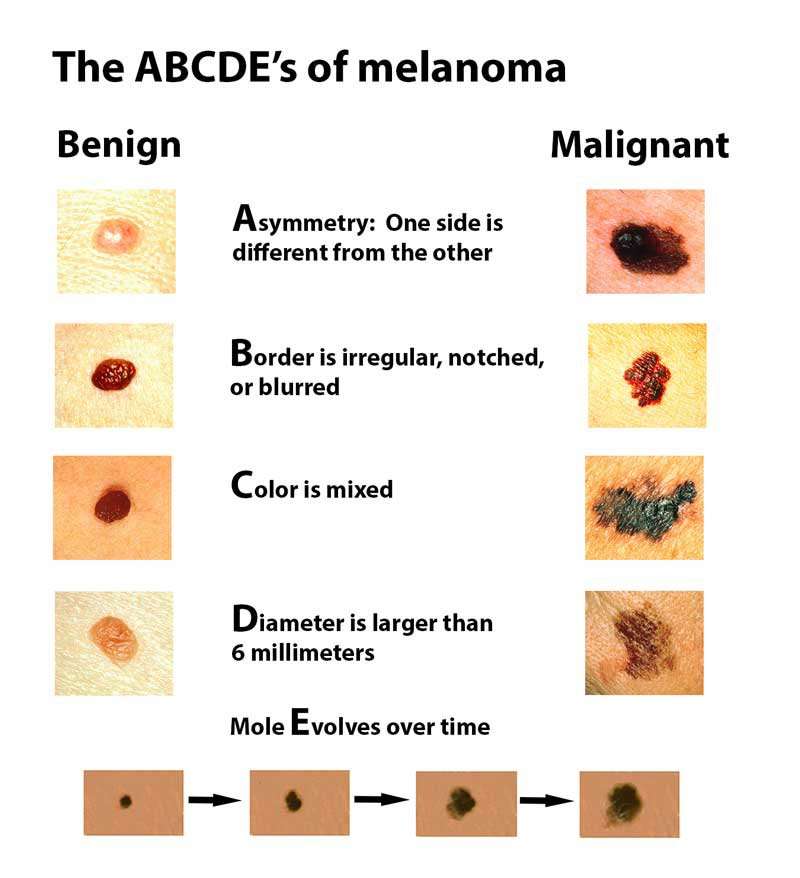
Thanks to research breakthroughs, more patients diagnosed with advanced melanoma are living longer some for years.
Because these breakthrough are relatively recent, its important to:
-
Work with a team of melanoma specialists.
-
Ask your melanoma specialists if any of the newer treatments are appropriate for you.
-
Realize that no one treatment works for everyone, so you may need to try different treatments or combine treatments.
Researchers continue to study advanced melanoma, and next-generation treatments are now being studied in clinical trials. If you want to know whether you are a match for a trial, you can find out if there are any relevant trials at, Clinical Trial Finder.
Related AAD resources
ReferencesChukwueke U, Batchelor T, et al. Management of brain metastases in patients with melanoma. J Oncol Pract. 2016; 12:536-42.
Emory Medical Center. A year in the life: Jimmy Carter shares his cancer experience. Posted July 11, 2016. Last accessed March 26, 2018.
Podlipnik S, Carrera C, et al. Performance of diagnostic tests in an intensive follow-up protocol for patients with American Joint Committee on Cancer stage IIB, IIC, and III localized primary melanoma: A prospective cohort study. J Am Acad Dermatol. 2016; 75:516-24.
Nordmann N, Hubbard M, et al. Effect of gamma knife radiosurgery and programmed cell death 1 receptor antagonists on metastatic melanoma. Cureus. 2017; 9: e1943.
Also Check: What Does Skin Cancer Look Like On Your Skin