Squamous Cell Carcinoma Recurrence
Recommended follow-up. After treatment for local squamous cell carcinoma , national guidelines recommend a complete skin examination by your dermatologist every 3 to 12 months for the first 2 years.4 The reason for this frequent follow-up schedule is that most SCC recurrences happen within 2 years.1 Follow-up should continue every 6 to 12 months for 3 more years. After that, the guidelines call for yearly skin examinations for the rest of your life.
You may need more frequent follow-up visits if the initial SCC had spread beyond the skin. Ask your doctor what she or he recommends for you.
Treatment Options For Recurrent Scc
A recurrent skin tumor is treated the same way as a high-risk primary tumor.4 Mohs surgery is the preferred option. Wide excision, radiation therapy, and chemotherapy are alternatives. Your doctor may recommend adjuvant therapy with radiation therapy or additional surgery.
If the cancer recurs in the lymph nodes or distant organs, treatment options include surgery, radiation therapy, and chemotherapy. Treatment options for advanced SCC are limited. Your doctor may recommend participating in a clinical trial.
Amount Of Exposure To Sunlight
The damaging effects of ultraviolet radiation accumulate over the years. In general, the risk of developing skin cancer increases with the amount of time spent under the sun and the intensity of radiation. The intensity of radiation varies according to the season of the year, time of day, geographic location , elevation above sea level, reflection from surfaces , stratospheric ozone, clouds, and air pollution.
Recent studies have focused on the effects of intermittent sun exposure in comparison to chronic exposure. It appears that the type of exposure may influence the type of cancer that develops. For example, intermittent solar exposure may be an important factor leading to the onset of basal cell carcinoma of the skin. Childhood sun exposure may also play an important part in the development of these cancers later in adult life. The pattern for cutaneous melanoma is similar to that for basal cell carcinoma.
In contrast, the relationship between squamous cell carcinoma and solar UVR appears to be quite different. For squamous cell tumours, high levels of chronic occupational sunlight exposure, especially in the 10 years prior to diagnosis, results in an elevated risk for this cancer in the highest exposure group.
Don’t Miss: Whats Cancer Look Like
What Are Some Of The Lesser
Some of the less common skin cancers include the following:
Kaposi sarcoma is a rare cancer most commonly seen in people who have weakened immune systems, those who have human immunodeficiency virus /AIDS and people who are taking immunosuppressant medications who have undergone organ or bone marrow transplant.
Signs and symptoms of Kaposi sarcoma are:
- Blue, black, pink, red or purple flat or bumpy blotches or patches on your arms, legs and face. Lesions might also appear in your mouth, nose and throat.
Merkel cell carcinoma
Merkel cell carcinoma is a rare cancer that begins at the base of the epidermis, the top layer of your skin. This cancer starts in Merkel cells, which share of the features of nerve cells and hormone-making cells and are very close to the nerve ending in your skin. Merkel cell cancer is more likely to spread to other parts of the body than squamous or basal cell skin cancer.
Signs and symptoms of Merkel cell carcinoma are:
- A small reddish or purplish bump or lump on sun-exposed areas of skin.
- Lumps are fast-growing and sometimes open up as ulcers or sores.
Sebaceous gland carcinoma
Sebaceous gland carcinoma is a rare, aggressive cancer that usually appears on your eyelid. This cancer tends to develop around your eyes because theres a large number of sebaceous glands in that area.
Signs and symptoms of sebaceous gland carcinoma are:
- A painless, round, firm, bump or lump on or slightly inside your upper or lower eyelid.
Dermatofibrosarcoma protuberans
Knowledge Is Your Best Defense
What Is Skin Cancer?
Skin cancer is the out-of-control growth of abnormal cells in the epidermis, the outermost skin layer, caused by unrepaired DNA damage that triggers mutations. These mutations lead the skin cells to multiply rapidly and form malignant tumors. The main types of skin cancer are basal cell carcinoma , squamous cell carcinoma , melanoma and Merkel cell carcinoma .
The two main causes of skin cancer are the suns harmful ultraviolet rays and the use of UV tanning beds. The good news is that if skin cancer is caught early, your dermatologist can treat it with little or no scarring and high odds of eliminating it entirely. Often, the doctor may even detect the growth at a precancerous stage, before it has become a full-blown skin cancer or penetrated below the surface of the skin.
Americans will develop skin cancer by age 70.
Also Check: Rare Cancer Symptoms
How Is Squamous Cell Carcinoma Treated
Although squamous cell carcinomas usually grow slowly, it is important to see a dermatologist quickly. “The sooner you see your doctor and the cancer is diagnosed and treated, the less complicated the surgery to remove it will be, and the faster you will make a complete recovery, Dr. Leffell explains. The treatment for squamous cell cancer varies according to the size and location of the lesion. The surgical options are the same as those for basal cell cancer:
- Surgical excision: Removing a squamous cell lesion is a simple procedure that typically takes place in the dermatologist’s office. After numbing the cancer and the area around it with a local anesthetic, the doctor uses a scalpel to remove the tumor and some of the surrounding skin to make sure all cancer is eliminated. Estimating how much to take requires skill and expertise, Dr. Leffell notes. The risk of taking too little tissue is that some cancer remains taking too much leaves a larger scar than is necessary. Shaped like a football, the wound is stitched together, using plastic surgery techniques. If dissolvable stitches are used, they will disappear on their own as the area heals. Though the procedure leaves some redness and a small scar, it tends to become less noticeable over time. “The cure rate for this type of excision is typically about 90 to 93 percent,” says Dr. Leffell. But, of course, this is dependent on the skill and experience of the doctor.”
When Is A Mole A Problem
If a new or existing mole begins to change shape, color, size, or becomes flaky, crusty, or begins to bleed, it’s time to make an appointment with your dermatologist to get it checked out. A mole can turn into melanoma on rare occasions. In early melanoma, the shape of a mole becomes asymmetrical and uneven.
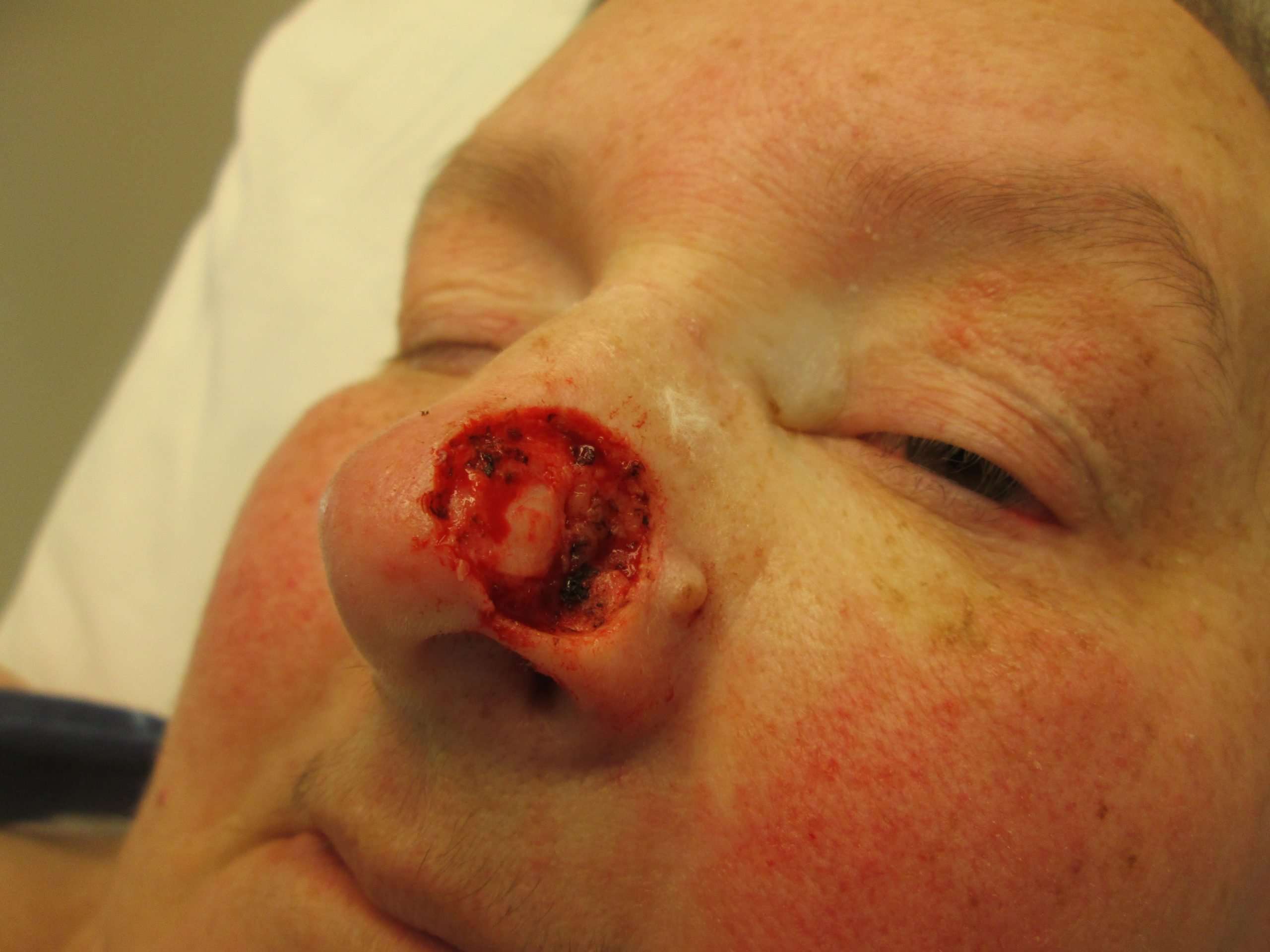
This photo contains content that some people may find graphic or disturbing.
Nodular basal cell carcinoma is a type of skin cancer that is most often found on the head. This type of cancer starts in basal cells, which are tasked with making new skin cells to push the old ones toward the surface of the skin. Nodular basal cell carcinoma is responsible for 60%-80% of all basal cell carcinomas. In the United States, its estimated that 4.3 million cases of basal cell carcinoma are diagnosed every year, with 2.5 to 3.4 million of those cases being nodular basal cell carcinoma.
This type of cancer appears as a pearl-like papule that is round and surrounded by threadlike red lines on the skin made up of tiny blood vessels. The risk of developing nodular basal cell carcinoma can be increased by spending a lot of time out in the sun, living in high-altitude and sunny locations, and radiation therapy.
Other risk factors include:
- Prolonged exposure to arsenic
- Certain rare genetic disorders such as basal cell nevus syndrome
Although this type of cancer is common, it is highly treatable, and the five-year relative survival rate is 100%.
Also Check: Does Skin Cancer Burn And Itch
What Causes Basal And Squamous Cell Skin Cancers
While many risk factors for basal and squamous cell skin cancers have been found, its not always clear exactly how these factors might cause cancer.
Most basal cell and squamous cell skin cancers are caused by repeated and unprotected skin exposure to ultraviolet rays from sunlight, as well as from man-made sources such as tanning beds.
UV rays can damage the DNA inside skin cells. DNA is the chemical in each of our cells that makes up our genes, which control how our cells function. We usually look like our parents because they are the source of our DNA. But DNA affects more than just how we look.
Some genes help control when our cells grow, divide into new cells, and die:
- Genes that help cells grow, divide, and stay alive are called oncogenes.
- Genes that keep cell growth in check by slowing down cell division or causing cells to die at the right time are called tumor suppressor genes.
Cancers can be caused by DNA changes that keep oncogenes turned on, or that turn off tumor suppressor genes. These types of gene changes can lead to cells growing out of control.
Researchers dont yet know all of the DNA changes that result in basal or squamous cell skin cancer, but they have found that in many skin cancers the cells have changes in tumor suppressor genes.
These are not the only gene changes that play a role in the development of skin cancer. There are many others as well.
Skin Pigment And Ability To Tan
Ultraviolet radiation from sunlight affects everybody’s skin to some extent, but the skin’s response varies widely from person to person. Peoples’ sensitivity to the sun varies according to the amount of pigment in the skin and the skin’s ability to tan.
Ultraviolet radiation causes tanning in two different ways: by immediate tanning and by delayed tanning. Immediate tanning causes the skin to darken in response to UVA. This darkening begins during the period of exposure, but fades within a few hours or days. The amount of tanning increases according to the skin’s natural darkness and previous amount of tanning.
Delayed tanning occurs two to three days after exposure to either UVA or UVB. It lasts from several weeks to months, and is maintained by repeated exposure to sunlight. With delayed tanning, the skin increases its production and distribution of dark pigment. The skin also becomes thicker. These changes can follow sunburning or develop gradually over a long period of repeated brief exposures to sunlight.
Some people burn easily after the first hour of sun exposure following winter or any period away from the sun. Other people, especially those with dark skin, rarely burn. This difference in reaction makes it possible to classify skin into one of six different types .
Table adapted from: SunSmart Victoria , Australia
You May Like: Lobular Breast Cancer Stage 1
What Are The Treatment Options
There are varieties of treatments available to treat skin cancer, including surgery, radiation therapy, and chemotherapy. Treatment for skin cancer depends on the type and size of cancer, your age, and your overall health.
Surgery is the most common form of treatment. It generally consists of an office or outpatient procedure to remove the lesion and check the edges, or margins, to make sure all the cancer was removed. For basal cell and squamous cell carcinomas, excision is frequently done using a specific technique called Mohs surgery, which gives the best chance to include all margins, while still minimizing the size of the defect. The site may then be repaired with simple stitches or skin from the same area or a different area of your body.
For melanoma treatment, your ENT specialist might also recommend doing a biopsy of the lymph node with the highest chance of having tiny microscopic metastatic cancer cells called a sentinel lymph node biopsy. If this biopsy is positive, further removal of more lymph nodes might be needed.
Sometimes radiation may be used as definitive therapy or additional treatment after surgery. For non-melanoma skin cancers, chemotherapy is not used as primary therapy, and its use after surgery is controversial. For melanomas, chemotherapy and medications that modulate the immune system may be used in more advanced cases.
css id:
Prognosis For Skin Cancer
It is not possible for a doctor to predict the exact course of a disease. However, your doctor may give you the likely outcome of the disease. If detected early, most skin cancers are successfully treated.
Most non-melanoma skin cancers do not pose a serious risk to your health but a cancer diagnosis can be a shock. If you want to talk to someone see your doctor. You can also call Cancer Council 13 11 20.
Recommended Reading: What Does Melanoma In Situ Look Like
How Do People Find Signs Of Melanoma On Their Own Skin
Performing a skin self-exam as often as recommended by your dermatologist is the best way. While examining your skin, you want to look for the following:
-
Mole that is changing in any way
-
Spot that looks different from the rest of the spots on your skin
-
Growth or spot on your skin that itches, bleeds, or is painful
-
Band of color beneath or around a nail
-
Sore that doesnt heal or heals and returns
The ABCDEs of melanoma can help you find changes to a mole, freckle, or other spot on your skin.
Preparing For Your Appointment
If you have any concerns about the health of your skin, it is important to share them with your doctor. After making an appointment, there are steps you can take to prepare yourself and make the most of your time with your doctor.
Here are some things to consider and be prepared to discuss before visiting the clinic or hospital:
-
What symptoms are you experiencing ?
-
When did you first notice your symptoms?
-
Have there been any major changes or stressors in your life recently?
-
What medications and/or vitamins are you taking?
-
What questions do you have for your doctor?
Also Check: Invasive Lobular Breast Cancer Survival Rate
What Is The Outlook For People With Skin Cancer
Nearly all skin cancers can be cured if they are treated before they have a chance to spread. The earlier skin cancer is found and removed, the better your chance for a full recovery. Ninety percent of those with basal cell skin cancer are cured. It is important to continue following up with a dermatologist to make sure cancer does not return. If something seems wrong, call your doctor right away.
Most skin cancer deaths are from melanoma. If you are diagnosed with melanoma:
- The five-year survival rate if its detected before it spreads to the lymph nodes is 99%.
- The five-year survival rate if it has spread to nearby lymph nodes is 66%.
- The five-year survival rate if it has spread to distant lymph nodes and other organs is 27%.
Determining If The Cancer Has Spread
As part of your diagnosis, your doctor will also determine what stage the cancer is in. The different stages refer to whether and how far the cancer has spread in your body, on a Roman numeral scale of I to IV. A stage I cancer is small and contained to the body part where it originated, whereas a stage IV cancer has spread aggressively to other parts of the body.
Depending on the type of skin cancer that a person has, it may be more or less likely that it has spread through the body. For instance, basal cell skin cancer rarely spreads beyond the skin where it starts. However, melanomas and large squamous cell carcinomas are more likely to spread into other regions of the body. Cases of melanoma, in particular, may call for further tests to determine the specific stage theyre in.
Your doctor may evaluate multiple factors in order to stage the cancer. Using biopsies and imaging tests, your doctor may take a look at:
-
The size and thickness of the tumor, and whether it has grown into surrounding tissues
-
Nearby lymph nodes, to check for signs of cancer spread
Don’t Miss: What Does Cancer Tumor Look Like
What Are The Symptoms Of Skin Cancer Of The Head And Neck
Skin cancers usually present as an abnormal growth on the skin. The growth may have the appearance of a wart, crusty spot, ulcer, mole or sore. It may or may not bleed and can be painful. If you have a preexisting mole, any change in the characteristics of this spot – such as a raised or an irregular border, irregular shape, change in color, increase in size, itching or bleeding – are warning signs of melanoma. Sometimes the first sign of melanoma or squamous cell cancer is an enlarged lymph node.
Johns Hopkins Head and Neck Cancer Surgery Specialists
Our head and neck surgeons and speech language pathologists take a proactive approach to cancer treatment. Meet the Johns Hopkins specialists who will work closely with you during your journey.
Infiltrative Basal Cell Carcinoma
This photo contains content that some people may find graphic or disturbing.
DermNet NZ
Infiltrative basal cell carcinoma occurs when a tumor makes its way into the dermis via thin strands between collagen fibers. This aggressive type of skin cancer is harder to diagnose and treat because of its location. Typically, infiltrative basal cell carcinoma appears as scar tissue or thickening of the skin and requires a biopsy to properly diagnose.
To remove this type of basal cell carcinoma, a specific form of surgery, called Mohs, is used. During a Mohs surgery, also called Mohs micrographic surgery, thin layers of skin are removed until there is no cancer tissue left.
This photo contains content that some people may find graphic or disturbing.
DermNet NZ
Superficial basal cell carcinoma, also known as in situ basal-cell carcinoma, tends to occur on the shoulders or the upper part of the torso, but it can also be found on the legs and arms. This type of cancer isnt generally invasive because it has a slow rate of growth and is fairly easy to spot and diagnose. It appears reddish or pinkish in color and may crust over or ooze. Superficial basal cell carcinoma accounts for roughly 15%-26% of all basal cell carcinoma cases.
Recommended Reading: Stage 1 Cancer Symptoms