Basal Cell Carcinoma Recurrence
The rate of basal cell carcinoma recurrence is about 40%, which means theres definitely a chance of this type of skin cancer coming back after its been removed. If BCC does recur, it will usually return to a different spot on the body.
After treatment for BCC, its a good idea to see a dermatologist once or twice a year for a complete skin examination. Basal cell carcinoma may recur more than five years after treatment. So if youve had BCC, youll probably want to have a complete skin examination once a year for the rest of your life, just to be safe. You can also ask your dermatologist how often they think you should come in, as risk factors vary for different people.
In general, youre more likely to experience recurring BCC if you have a weakened immune system, if you have fair skin, or if youre exposed to strong sunlight. Thats why its important to wear sunscreen, hats, and clothing that protects your body from the sun.
The size and location of tumors can also play a role in whether or not BCC recurs. When tumors are large, grow quickly, develop around a nerve, or have unclear borders, the risk of recurrent BCC increases. This is also the case if a tumor has already recurred once, or if it develops at the site where youve previously had radiation therapy. Tumors are less likely to come back after Mohs surgery or excision.
How Does The Doctor Know I Have Skin Cancer
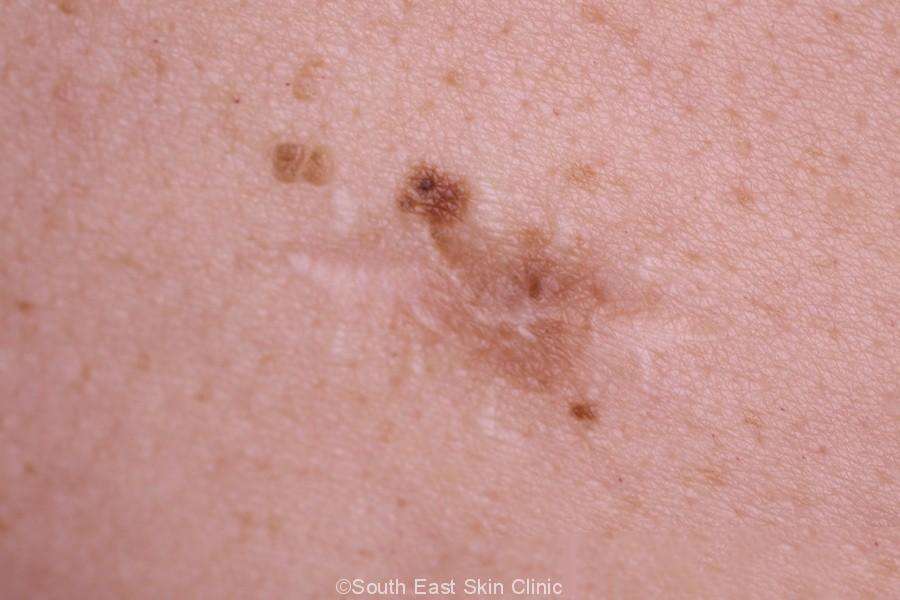
Basal and squamous skin cancer may look like:
- Flat, firm, pale or yellow areas that look a lot like a scar
- Raised reddish patches that might itch
- Rough or scaly red patches, which might crust or bleed
- Small, pink or red, shiny, pearly bumps, which might have blue, brown, or black areas
- Pink growths or lumps with raised edges and a lower center
- Open sores that dont heal, or that heal and then come back
- Wart-like growths
You May Like: What Is The Deadliest Type Of Skin Cancer
The Importance Of The Follow
Attending regular follow-up appointments with a doctor or dermatologist is key to catching any recurring melanomas early before they have a chance to spread or worsen.
A doctor will advise follow-up appointment timing based on the specifics of each individual patient, but the frequency of follow-up appointments are usually based on the stage the melanoma was in when it was treated.
DermNet New Zealand provides an overview:
· Stage I melanoma follow-up visit every year for the next 10 years
· Stage II melanoma depending on the severity of melanoma in this stage, follow-up every 46 months for 23 years and then once every year up to 10 years
· Stage III melanoma every 3 months in the first year, every 4 months in the second year, every 6 months until year 5, and then once a year until year 10
· Stage IV melanoma as for Stage III but with additional visits as required
Taking the proper precautions by staying out of the sun and wearing sunscreen and protective clothing is the other key to help prevent melanoma from returning.
Read more about Skin cancer symptoms what to look out for, with pictures, to help you know what to look out for.
SkinVision Customer Stories
Recommended Reading: Prognosis Of Skin Cancer
Where Does Melanoma Return
It may come back in the same place or on the same area of your body. This is most common.
Melanoma can also return far from where you had the first one. For example, if you had a melanoma on your back, it could return on your arm.
It can also show up inside your body. If melanoma appears inside the body, its most likely to show up in the lymph nodes, lungs, liver, brain, bone, or gastrointestinal tract.
How Quickly Should Melanoma Be Removed
Hypothesis-based, informal guidelines recommend treatment within 46 weeks. In this study, median surgical intervals varied significantly between clinics and departments, but nearly all were within a 6-week frame. Key words: melanoma, surgical interval, treatment time, melanoma survival, time factors.
Read Also: Melanoma Stage 3 Survival Rate
How Fast Does Melanoma Grow
Some types of melanoma can grow very quickly, becoming life-threatening in as little as six weeks. If left untreated it can spread to other parts of the body.
Nodular melanoma is a highly dangerous form of melanoma that looks different from common melanomas and can grow in just a few weeks. Raised and even in color, nodular melanoma are often red, pink, brown, or black. It can be life-threatening if not detected and removed quickly. See your doctor immediately if you notice any of these changes.
Its also important to note that while sun exposure is a major risk factor in melanoma, the disease can develop in parts of the body that get little or no sun exposure.
Recommended Reading: How Aggressive Is Merkel Cell Carcinoma
How Is Melanoma Detected
Melanomas are visible so cancer which is potentially identified early. Melanoma may not necessarily evidence as a new growth or change in fresh unblemished skin, it can manifest as an alteration to the appearance of an existing mole or birthmark. Glance at these pictures to familiarise yourself with the identity of melanoma.
Recommended Reading: Skin Cancer Prognosis
What Kind Of Treatment Will I Need
There are many ways to treat melanoma. The main types of treatment are:
- Surgery
Most early stage melanomas can be treated with surgery alone. More advanced cancers need other treatments.
The treatment plan thats best for you will depend on:
- The stage of the cancer
- The results of lab tests on the cancer cells
- The chance that a type of treatment will cure the melanoma or help in some way
- Your age
Read Also: What Is Soft Tissue Carcinoma
Can I Lower My Risk Of The Melanoma Progressing Or Coming Back
If you have melanoma, you probably want to know if there are things you can do that might lower your risk of the cancer coming back, or of getting a new skin cancer.
At this time, not enough is known about melanoma to say for sure if there are things you can do that will be helpful. We do know that people who have had melanoma are at higher risk for developing another melanoma or other type of skin cancer. Because of this, its very important to limit your exposure to UV rays and to continue to examine your skin every month for signs of melanoma coming back or possible new skin cancers. Skin cancers that are found early are typically much easier to treat than those found at a later stage.
Adopting healthy behaviors such as not smoking, eating well, being active, and staying at a healthy weight might help as well, but no one knows for sure. However, we do know that these types of changes can have positive effects on your health that can extend beyond your risk of melanoma or other cancers.
Read Also: What Is The Survival Rate For Invasive Ductal Carcinoma
Risk Of Further Melanomas
Most people treated for early melanoma do not have further trouble with the disease. However, when there is a chance that the melanoma may have spread to other parts of your body, you will need regular check-ups. Your doctor will decide how often you will need check-ups everyone is different. They will become less frequent if you have no further problems. After treatment for melanoma it is important to limit exposure to the suns UV radiation. As biological family members usually share similar traits, your family members may also have an increased risk of developing melanoma and other skin cancers. They can reduce their risk by spending less time in the sun and using a combination of sun protection measures during sun protection times. It is important to monitor your skin regularly and if you notice any changes in your skin, or enlarged lymph glands near to where you had the cancer, see your specialist as soon as possible.
What Are The Stages Of Melanoma
Very rapid skin changes are often far less concerning than those materialising over the passage of time. Actual confirmation of melanoma is undertaken via biopsy. A tiny segment is removed for specialist analysis. A positive corroboration is accompanied by a benchmark of severity simply referred to as Stages I-IV, the latter being the most serious. Stage labelling allows the doctor to understand the progression of the disease and determine the most efficacious interventions. The first three stages refer to the depth of melanoma within the skin, size and possible ulceration. Only Stage IV indicates that the illness has spread to other organs.
Recommended Reading: Immunotherapy For Malignant Melanoma
Where To Find Support For Stage 3 Melanoma
With a melanoma diagnosis, its important to reach out to those close to you during your treatment. In addition to family and friends, there are many support groups and resources who can help answer questions or provide a listening ear.
Find a melanoma support group. The American Melanoma Foundation maintains a list of support groups throughout the country find them by .
Join an online support group. If you feel more comfortable participating in an online support group, the AIM at Melanoma Foundation offers a support community as well as counseling.
Seek financial assistance, if needed. The Melanoma Research Foundation has developed a central resource for patient assistance programs and government entities that offer financial assistance for those with melanoma. For more information, please .
Sign up for a mentoring program. Olympic figure skater Scott Hamiltons charity, 4th Angel, offers a mentoring program for those with cancer. This telephone-based program is designed to provide support and encouragement to those with cancer.
Many organizations provide professional and supportive services when youve been diagnosed with melanoma. Other organizations that provide support for those with skin cancer include the:
Notes Regarding The Recommendations

The recommendations given above are based on the best evidence currently available, but it is acknowledged that this is low-level evidence. Individual patients may prefer more frequent follow-up for reassurance, while others may prefer less frequent follow-up because of the anxiety provided by the follow-up visits or the time and expense associated with attendance for follow-up. Routine radiological follow up for stage IIC and III melanoma may detect recurrence sooner, possibly leading to better outcome by allowing treatment with drugs, such as immunotherapy drugs, to start earlier. However, while early drug treatment of recurrent melanoma might improve survival, there is currently no evidence showing this. Thus, the recommendations are a reasonable compromise which, reinforced by good patient education, should ensure that most melanoma recurrences are detected promptly and new primary melanomas are diagnosed early.
Don’t Miss: Lobular Carcinoma Survival Rate
What Is Melanoma In Situ
4.5/5Melanoma in situmelanomamelanomasituthe answer
Prognosis: Stage 0 melanoma, or melanoma in situ, is highly curable. There is very little risk for recurrence or metastasis. The 5-year survival rate as of 2018 for local melanoma, including Stage 0, is 98.4%. Click here to learn more about melanoma survival rates.
Also, how serious is melanoma in situ? In situ melanomas don’t spread to other parts of the body or cause death, but if the tumor has an opportunity to grow even one millimeter deep into the skin, it can lead to more involved treatment and greater danger. If left untreated, it can metastasize and even become life-threatening.
Also question is, what does melanoma in situ look like?
What They Look Like. Melanomas in situ tend to be flat and asymmetric with irregular borders. They can be black, brown, tan, gray or even pink if the person has very fair skin.
Does melanoma in situ come back?
Yes, the outlook for melanoma in situ is excellent. It is very rare for them to come back if they are removed completely. Furthermore, because they were ‘in situ‘, they will not have had an opportunity to spread elsewhere in the body.
| 99.9% 5-year survival 98.9% 10-year survival | |
| I/II | 89 to 95% 5-year survival |
| II | 45 to 79% 5-year survival |
| III |
What Is The Importance Of Sentinel Lymph Node Biopsy For Breast Cancer Diagnosis
What is the importance of sentinel lymph node biopsy for breast cancer diagnosis? Sentinel node biopsy is a surgical procedure used to determine whether cancer has spread beyond a primary tumor into your lymphatic system. Its used most commonly in evaluating breast cancer and melanoma. The sentinel nodes are the first few lymph nodes into which a tumor drains.
Is sentinel lymph node biopsy necessary for breast cancer? Sentinel lymph node biopsy might be needed. Lymph node surgery is often done as part of the main surgery to remove the breast cancer, but in some cases it might be done as a separate operation.
What is the importance of sentinel lymph node? Sentinel lymph nodes are an important part of the immune system, and they contain the cells that monitor foreign substances, like bacteria, viruses and cancer. Sentinel lymph node mapping helps to identify the lymph nodes that are at highest risk for containing cancer.
Where are the sentinel nodes located and why are these important in a patient with breast cancer? Sentinel refers to the first lymph node in the armpit on the same side of the body as the breast cancer. Since specific lymph nodes handle drainage from the breast, this node is the most likely place tumor cells will metastasize if some cells have left the original tumor by the time of surgery.
Read Also: How To Identify Skin Cancer
Read Also: Idc Breast Cancer Survival Rate
How Long Do Grey Horses Live
Other Signs of Aging in Horses
Older horses begin to show signs of aging by the time they hit their teenage years, usually starting around 15. They will sometimes sprout gray hairs around their eyes and muzzle. These can be difficult to spot on a horse that is light-colored or already gray. What is this?
How Often Does Skin Cancer Return
A huge majority of adults today spent their early years exposed to sunshine without any protection. While our understanding of the dangers of UV exposure has come a long way over the last several decades, damage done before sun safety became commonplace cant be erased.
Skin cancer diagnoses are higher than ever. After a positive diagnosis and treatment, its critical to work with your doctors to manage risk and stay informed about when and how skin cancer may return. At Desert Bloom, our goal is to ensure every patients safety by providing all the necessary information to support long-term health.
Dr. Wallin is a board certified reconstructive surgeon with extensive experience repairing wounds caused by skin cancers after MOHS surgery. At Desert Bloom Plastic Surgery, we have helped patients of all ages, genders, and skin tones. Dr. Wallin has several treatment methods available to address varying tumor depths and locations. Our patients are strongly encouraged to continue seeing their dermatologist regularly to ensure the detection of potential cancer recurrences and the presence of new lesions.
Also Check: Invasive Ductal Breast Cancer Prognosis
Survival And Clinical Outcome
Fifty-nine patients had died of melanoma progression at the time of the analysis, among which 32 died with progressing brain metastases. The median overall survival duration from the time of initial brain metastasis was 12.8 months , and the median overall survival duration from the time of initial melanoma diagnosis was 60.5 months for all 79 patients. The median overall survival durations from the time of craniotomy and stereotactic radiosurgery were 17.3 months and 15.4 months , respectively. The median survival durations of patients who received anti-CTLA-4 antibody, anti-PD-1 antibody and BRAF inhibitor after the diagnosis of brain metastasis were 19.2 months , 37.9 months and 12.7 months , respectively. Tables and describe the outcomes of the entire cohort as well as specific subsets of patients. Figures and illustrate the Kaplan-Meier curves of overall survival for all patients and for those who were treated with or without anti-PD-1 therapy, respectively.
Fig. 1
Skin Exam And Physical
You may have had a complete skin exam during your last dermatology appointment. Dermatologists often perform this exam when a patient has a suspicious spot on their skin that could be skin cancer.
During a complete skin exam, your dermatologist examines you head to toe. This exam includes a look at all of your skin, including the skin on your scalp, face, genitals, and the bottoms of your feet. Your dermatologist will also examine your nails and look inside your mouth.
If you did not have a complete skin exam before being diagnosed with melanoma, youll have one at your next appointment.
During a complete skin exam, your dermatologist may use a device called a dermatoscope
This device provides a closer look at the spots on your skin.
At your next appointment, youll receive a physical. During your physical, your dermatologist will ask how youre feeling and about your health, illnesses, and injuries. Your dermatologist will also want to know what diseases run in your family and the medications you take.
During your physical, your dermatologist will check your lymph nodes to find out if any feel swollen. There are many reasons for swollen lymph nodes. For example, if you have an infection or recently received a vaccination, lymph nodes can feel swollen. When you have melanoma, the swelling might be a sign that the cancer has spread.
If youre unsure what diseases your close blood relatives have had, try to find out
Dont Miss: Show Me What Skin Cancer Looks Like
Also Check: Invasive Ductal Carcinoma Stage 3 Survival Rate
New Melanomas Likely To Recur At Same Rate
byCharles Bankhead, Senior Editor, MedPage Today August 9, 2014
CHICAGO — A diagnosis of in situ or invasive melanoma conferred a similar long-term risk of invasive melanoma recurrence, a 40-year retrospective review showed.
For the first 2 years after initial diagnosis, invasive melanoma had a greater risk of invasive recurrence, as compared with an initial diagnosis of in situ disease. Thereafter, the risk of invasive recurrence remains the same, regardless of the initial diagnosis, Hyemin Pomerantz, MD, of Brown University in Providence, R.I., reported here at the American Academy of Dermatology summer meeting.
Action Points
- Note that this study was published as an abstract and presented at a conference. These data and conclusions should be considered to be preliminary until published in a peer-reviewed journal.
“The findings suggest that follow-up after diagnosis of in situ or invasive melanoma should be the same,” Pomerantz told MedPage Today. “Because the incidence of melanoma in situ is increasing, surveillance for recurrence in this patient population could help improve outcomes for melanoma.”
To compare recurrence risk associated with the initial diagnosis, investigators reviewed data from the Surveillance, Epidemiology, and End Results program for 1973 to 2011. They identified all patients with a first diagnosis of melanoma and no history of other types of cancer and determined the classification of the initial diagnosis .
Disclosures
Primary Source