What Is The Prognosis Of Squamous Cell Carcinoma Of Tongue
- In general, Squamous Cell Carcinoma of Tongue is an aggressive form of cancer. If metastasis is observed, then the prognosis is guarded or unpredictable
- Tumors in their early stage with complete excisional treatment typically have good prognosis
- In cases of metastasis, its prognosis depends upon a set of several factors that include:
- Stage of tumor: With lower-stage tumors, when the tumor is confined to site of origin, the prognosis is usually excellent with appropriate therapy. In higher-stage tumors, such as tumors with metastasis, the prognosis is poor
- The surgical respectability of the tumor
- Overall health of the individual: Individuals with overall excellent health have better prognosis compared to those with poor health
- Age of the individual: Older individuals generally have poorer prognosis than younger individuals
- Whether the tumor is occurring for the first time, or is a recurrent tumor. Recurring tumors have a poorer prognosis compared to tumors that do not recur
- Response to treatment: Tumors that respond to treatment have better prognosis compared to tumors that do not respond so well to treatment
Treating Advanced Squamous Cell Cancers
Lymph node dissection:Removing regional lymph nodes might be recommended for some squamous cell cancers that are very large or have grown deeply into the skin, as well as if the lymph nodes feel enlarged and/or hard. The removed lymph nodes are looked at under a microscope to see if they contain cancer cells. Sometimes, radiation therapy might be recommended after surgery.
Immunotherapy: For advanced squamous cell cancers that cant be cured with surgery or radiation therapy, one option might be using an immunotherapy drug such as cemiplimab or pembrolizumab . However, these drugs havent been studied in people with weakened immune systems, such as people who take medicines for autoimmune diseases or who have had an organ transplant, so the balance between benefits and risks for these people isnt clear.
Systemic chemotherapy and/or targeted therapy:Chemotherapy and targeted therapy drugs might be other options for patients with squamous cell cancer that has spread to lymph nodes or distant organs. These types of treatment might be combined or used separately.
Can Squamous Cell Carcinoma Be Prevented
The best way to prevent SCC is to avoid sunburn. Avoid going outin the sun when the UV Index is higher than 3, such as in the middle of theday. Seek shade, wear a hat, sunglasses and clothing that protects you from thesun, and always use an SPF30+ sunscreen. Do not go to tanningsalons.
If you are at very high risk of developing another skin cancer, yourdoctor may prescribe you specific vitamins.
Also Check: Does Amelanotic Melanoma Blanch When Pressed
Treating Squamous Cell Carcinoma Of The Skin
Treatment options for squamous cell skin cancer depend on the risk of the cancer coming back, which is based on factors like the size and location of the tumor and how the cancer cells look under a microscope, as well as if a person has a weakened immune system.
Most squamous cell skin cancers are found and treated at an early stage, when they can be removed or destroyed with local treatment methods. Small squamous cell cancers can usually be cured with these treatments. Larger squamous cell cancers are harder to treat, and fast-growing cancers have a higher risk of coming back.
In rare cases, squamous cell cancers can spread to lymph nodes or distant parts of the body. If this happens, treatments such as radiation therapy, immunotherapy, and/or chemotherapy may be needed.
What Are The Survival Rates For Scc
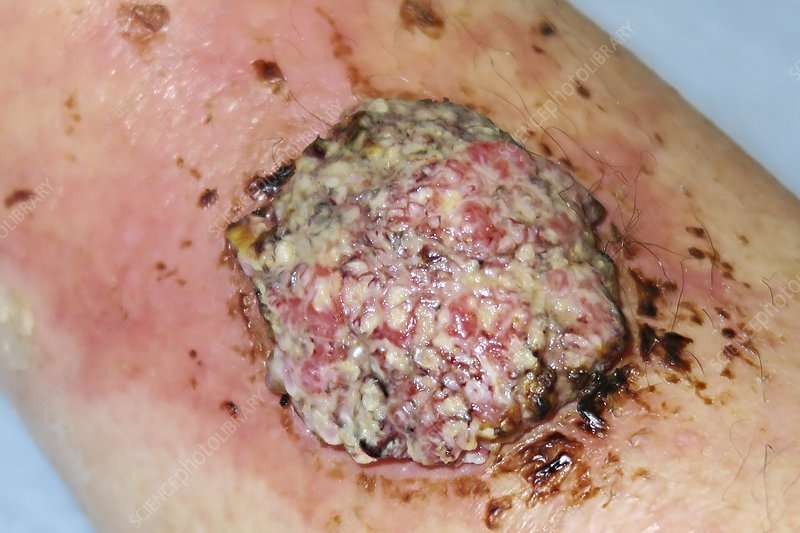
The vast majority of SCC is cured. Only about 2 percent to 5 percent of SCC cases grow back or spread. Unfortunately, because cases of SCC are not reported to the U.S. cancer registry it is hard to estimate survival rates. It is clear that metastatic SCC is very difficult to treat. . In large groups of people studied who have distant metastatic SCC, about 70 percent died from their disease.14,15
You May Like: Lobular Breast Cancer Stage 3
Obtaining Some Cancer Cells
There are a few ways your doctor can obtain these cells. They may take a sputum sample. If there is any fluid around your lungs, it will usually have some cancer cells, too. Your doctor may obtain a sample with a needle inserted through your skin . Then, your cells are examined under a microscope for signs of cancer.
Treatment Of Oral Squamous Cell Carcinoma
-
Surgery, with postoperative radiation or chemoradiation as needed
For most oral cavity cancers, surgery is the initial treatment of choice. Radiation or chemoradiation is added postoperatively if disease is more advanced or has high-risk features.
Selective neck dissection is indicated if the risk of nodal disease exceeds 15 to 20%. Although there is no firm consensus, neck dissections are typically done for any lesion with a depth of invasion > about 3.5 mm.
Routine surgical reconstruction is the key to reducing postoperative oral disabilities procedures range from local tissue flaps to free tissue transfers. Speech and swallowing therapy may be required after significant resections.
Radiation therapy is an alternative treatment. Chemotherapy is not used routinely as primary therapy but is recommended as adjuvant therapy along with radiation in patients with advanced nodal disease.
Treatment of squamous cell carcinoma of the lip is surgical excision with reconstruction to maximize postoperative function. When large areas of the lip exhibit premalignant change, the lip can be surgically shaved, or a laser can remove all affected mucosa. Mohs surgery can be used. Thereafter, appropriate sunscreen application is recommended.
Also Check: Metastatic Skin Cancer Pictures
How Common Is Squamous Cell Carcinoma
Over 1 million people are diagnosed with SCC in the US each year. The incidence of SCC has risen about 200 percent over the past 30 years. There are more than 15,000 deaths each year in the US from SCC. Excluding head and neck SCC and CSCC in situ, about 200,000-400,000 new cases of SCC are diagnosed in the US every year, resulting in about 3,000 deaths.
Men are about two times more likely than women to develop SCCs. People over the age of 50 are most likely to get SCCs, but the incidence has been rising in younger people.
What Survival Rates Mean
The survival rate is the percentage of people who live for a certain period of time with this cancer. The number is based on research done on large groups of people with the same stage of cancer.
Experts dont know the exact survival numbers for late-stage SCC, because cancer registries dont track statistics for this cancer. However, your doctor may be able to give you an estimate of your prognosis.
When it comes to surviving cancer, everyone is different. Your outcome will depend on the specific treatments you have and how well you respond to them. Talk to your doctor about your outlook and what it means.
Read Also: What Is Clear Cell Carcinoma
How Are Skin Cancer Survival Rates Measured
Cancer survival is measured in many different ways, including:1
- Five-year overall survival rate is the percentage of people who are still alive 5 years after diagnosis or treatment. If the 5-year overall survival rate after diagnosis is 85 percent, that means that 5 years after being diagnosed with melanoma, 85 of 100 people are still alive. Some of those people may still have cancer, others do not.
- Disease-free survival is how long a person survives after treatment without any sign of that cancer.
- Median overall survival is the average length of time from treatment that half the study population is still alive. For example, consider 100 people who are treated with a medication and 3.1 years later, 50 have died and 50 are alive. The median overall survival is 3.1 years.
When looking at a skin cancer survival rate, it is important to know what group was studied. Survival rates can differ greatly by cancer stage, age at diagnosis, gender, and race/ethnicity. The most accurate numbers about skin cancer survival are about melanoma because cases of melanoma are tracked in national cancer registries.
What Is Squamous Cell Carcinoma Of Esophagus
- Squamous Cell Carcinoma of Esophagus is a highly-malignant tumor of the epithelium. The esophagus is a part of the upper gastrointestinal tract and is also known as the food-pipe
- The risk factors for Squamous Cell Carcinoma of Esophagus include smoking and alcohol consumption, dietary habits that exclude fresh fruits and vegetables, radiation treatment for breast cancer, and certain genetic conditions
- The cause of the condition is generally unknown, but numerous genetic abnormalities and gene involvement are noted. Squamous Cell Carcinoma of Esophagus is observed at a higher incident rate in certain geographical areas such as parts of China, Central Asia, and South Europe
- Most tumors are diagnosed at a later stage . Superficial tumors may be painless and asymptomatic, while advanced cases present swallowing difficulties and chest and upper abdominal pain
- The treatment of choice is a surgical excision with clear margins followed by radiation therapy/chemotherapy. In case of spread of cancer to other regions, a combination of treatments may be considered by the healthcare provider
- The prognosis depends upon a set of several factors including the stage of the tumor, extent of tumor spread, overall health of the patient, and many other factors. In general, the prognosis of Squamous Cell Carcinoma of Esophagus is poor
There are different subtypes of Esophageal Squamous Cell Carcinoma and these include:
- Verrucous Carcinoma
- Basaloid Squamous Cell Carcinoma
Read Also: Well Differentiated
What Is Squamous Cell Carcinoma Of Tongue
- Squamous Cell Carcinoma of Tongue is a common malignant tumor that typically affects elderly men and women. It is more aggressive than conventional squamous cell carcinoma affecting other body regions
- The cause of the condition is unknown, but genetic mutations may be involved. Factors that may influence its development include smoking and chewing of tobacco, radiation treatment for other reasons, and exposure to coal tar and arsenic
- The squamous cell carcinoma may appear as slow-growing skin lesions. The lesions may ulcerate and cause scarring of the tongue. It may be difficult to eat, swallow food, or even to speak
- The treatment of choice is a surgical excision with clear margins followed by radiation therapy or chemotherapy, as decided by the healthcare provider. In majority of the cases, the prognosis is good with appropriate treatment
- Nevertheless, the prognosis of Squamous Cell Carcinoma of Tongue depends upon many factors including the stage of the tumor and health status of the affected individual. There is a possibility of local or regional metastasis, which can involve the lymph nodes. This may dictate the course of the condition
Metastatic Squamous Cell Carcinoma
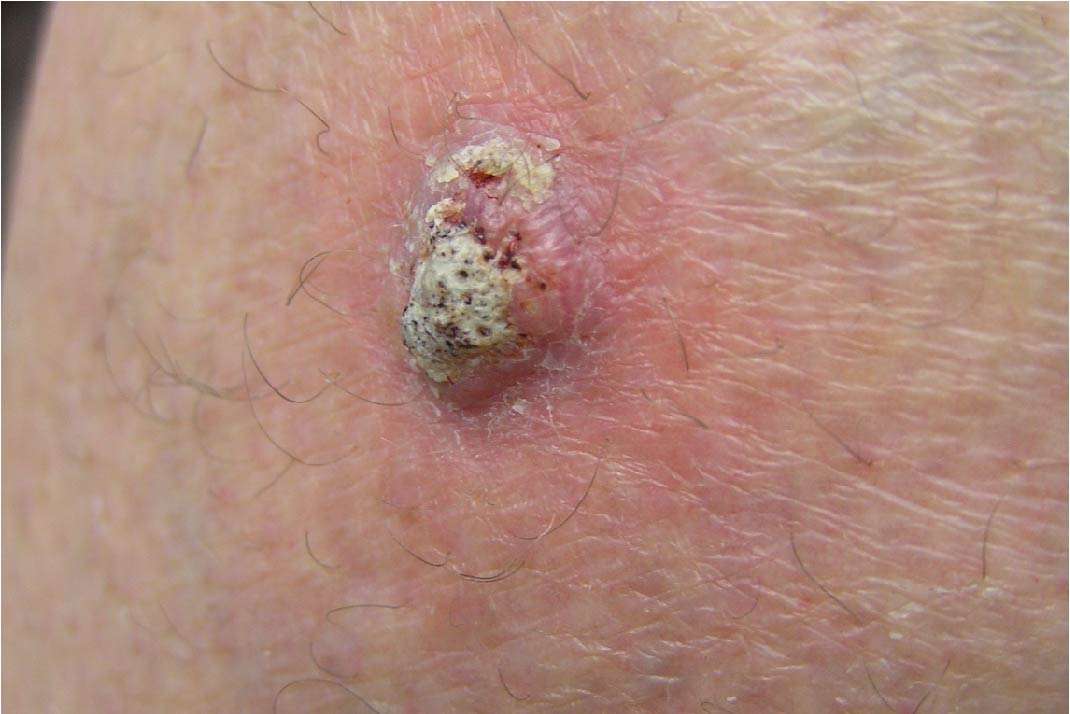
In addition to a 65-fold higher risk of developing squamous cell carcinoma , SCC that develop in adult transplant recipients are at higher risk for metastasis, 5-7%, compared to the general population, ~2% . ~13% of SCC that occur in pediatric patients metastasize. SCC that occur on the lip of pediatric patients are at particularly high risk .
SCC metastasis is generally associated with a poor prognosis with a 3-year disease-free survival rate in adult patients of 56% . Relapse of SCC is common, with the cumulative relapse rate ~29% within 1-year of treatment.
Clinical Characteristics of Metastatic Squamous Cell Carcinoma
Onset:Few large studies of metastatic cutaneous squamous cell carcinoma are available. One of the largest was performed by Martinez et al 2003 who followed 68 pts with 73 distinct metastatic skin cancers . In this study, the mean onset of metastatic SCC occurred 10.7-years following transplantation. The mean time with which metastatic SCC was detected after diagnosis of the primary SCC lesion was 1.4-years.
Location:The location where metastatic SCC was detected varied. 36% of patients had in-transit metastasis, metastasic foci located between the primary tumor and the closest lymph node region. These usually represent SCC spread along lymphatic vessels and/or nerves. 78% had lymph node metastasis occurring in draining nodal basins, and 35% had distant systemic/visceral metastasis. The most common sites for distant disease were lung and bone.
Don’t Miss: Invasive Ductal Breast Cancer Prognosis
What Are The Survival Rates For Melanoma
The 5-year overall survival rate for melanoma is 92.7 percent, based on the most recent data from the National Cancer Institute from 2010-2016. That means that 5 years after being diagnosed with melanoma of any type, about 92 out of 100 people are still alive. This estimate includes people of both genders, all races, and all stages at diagnosis.4
Cancer stage. One important factor in estimating survival is how far the cancer has spread by the time it is diagnosed. Local melanoma is melanoma that has not spread beyond the original tumor. About 83 percent of melanomas are caught at this early stage. The 5-year survival rate for local melanoma is 99 percent.5
If cancer cells have spread to a nearby lymph node, it is called regional metastasis. In 9 percent of cases, the melanoma has spread to regional lymph nodes at diagnosis. The 5-year survival for regional melanoma is 66.2 percent.5
Distant spread is when cancer cells have traveled to distant parts of the body. About 4 percent of melanoma cases have metastasized to distant locations at the time of diagnosis. The 5-year survival for distant metastatic melanoma is 27.3 percent.5
Gender. Skin cancer survival rates in women are higher than survival rates in men at all ages and stages of cancer. Five years after diagnosis, 92.5 percent of women were alive compared to 87.3 percent of men.4,6
Squamous Cell Carcinoma Complications
If its not treated, squamous cell carcinoma can spread and damage healthy tissue and organs. In rare cases, it can be life-threatening. That can be more likely if:
- The cancer is large or very deep.
- The cancer involves mucous membranes, like your lips.
- Youve had an organ transplant.
- You have a weakened immune system because of certain conditions, like some types of leukemia.
Also Check: Melanoma On Nose Prognosis
How Is Squamous Cell Carcinoma Of Esophagus Diagnosed
A diagnosis of Squamous Cell Carcinoma of Esophagus may involve the following:
- A thorough medical history and physical examination
- X-ray of the chest
- CT or MRI scan of the chest: For advanced cases and to check cancer growth and spread, including lymph node involvement
- Upper GI endoscopy: An endoscopic procedure is performed using an instrument called an endoscope, which consists of a thin tube and a camera. Using this technique, the radiologist can have a thorough examination of the insides of the upper gastrointestinal tract
- Endoscopic ultrasonography: During this procedure, fine needle aspiration biopsy can be performed on the affected area. This is good technique for tumor detection, including tumor invasion parameters, and whether nearby lymph nodes are affected
- Endocytoscopy: It is a non-invasive technique helpful for invasive carcinomas that are located superficially
- Early cancer lesions may be detected using narrow band imaging technique
- Barium swallow
- Whole body PET scans to determine how far the cancer has spread to other organ systems
Although the above modalities can be used to make an initial diagnosis, a tissue biopsy of the tumor is necessary to make a definitive diagnosis to begin treatment. The tissue for diagnosis can be procured in multiple different ways which include:
Tissue biopsy:
What Are The 5 Stages Of Skin Cancer
Staging is an important tool used to treat skin cancer. Your stage helps the medical team determine where the tumor is, how large it is, where it has spread, your prognosis, and the most effective treatment plan.
The five stages of squamous cell carcinoma include:
- Stage 0: Also known as carcinoma in situ, in this stage cancer is present in the epidermis. It has not spread to deeper layers.
- Stage 1: The tumor is smaller than 2 centimeters and has not spread to nearby lymph nodes or other organs. The individual has one or fewer risk factors for spread.
- Stage 2: The tumor is wider than 2 centimeters and has not spread to nearby lymph nodes or other organs. This stage also applies to any sized tumor when the individual has two or more risk factors.
- Stage 3: The tumor has spread into nearby facial bones or one lymph node. It has not spread to other organs.
- Stage 4: The tumor is of any size and has metastasized to one or more of the lymph nodes. It may have spread to the bones and other distant organs.
You May Like: Lobular Breast Cancer Survival Rate
Scc Is Mainly Caused By Cumulative Uv Exposure Over The Course Of A Lifetime
If youve had a basal cell carcinoma you may be more likely to develop a squamous cell skin carcinoma, as is anyone with an inherited, highly UV-sensitive condition such as xeroderma pigmentosum.
Chronic infections, skin inflammation, HIV and other immune deficiency diseases, chemotherapy, anti-rejection drugs used in organ transplantation, and excessive sun exposure can all lead to a risk of squamous cell carcinoma.
Occasionally, squamous cell carcinomas arise spontaneously on what appears to be normal, healthy skin. Some researchers believe the tendency to develop these cancers can be inherited.
SCCs may occur on all areas of the body including the mucous membranes and genitals, but are most common in areas frequently exposed to the sun:
- Ears
- Previous BCC or SCC
- Chronic inflammatory skin conditions or chronic infections
But anyone with a history of substantial sun exposure is at increased risk. Those whose occupations require long hours outside or who spend their leisure time in the sun are also at risk.
Can Squamous Cell Carcinoma Be Cured
The majority of SCC tumors are found early and treated while they are still small. Treatment at an early stage can usually remove SCC.2
SCC is more likely than BCC to invade deeper layers of skin and spread to other parts of the body.2 This is uncommon. However, about 5% to 10% of SCC tumors are considered aggressive.2,4 It is more difficult to treat aggressive SCC. By one estimate, between 3,900 and 8,800 white individuals died from SCC in 2012.1 In the Midwest and southern United States, SCC may cause as many deaths as melanoma.1
Your dermatologist may recommend regular follow up for several years after treating any SCC. Most of the cases that return do so with 2 years of initial treatment.5
Don’t Miss: Invasive Breast Cancer Survival Rate