What Is The Outcome For Melanoma In Situ
Patients with melanoma in situ have the same life expectancy as the general population. Further problems are rare from melanoma in situ because the malignant cells within the epidermis have no metastatic potential. However, a small focus of invasive disease may have beeen missed due to the impracticability of evaluating every part of a large skin lesion.
Melanoma in situ occasionally recurs at the same site, requiring further surgery.
How Is Melanoma In Situ Of Skin Diagnosed
A thorough history and a complete physical exam by a physician are crucial for the diagnosis of Melanoma In Situ of Skin. This is followed by some tests which include:
- Biopsy of skin: A sample of the skin, from any suspected area found on physical examination, is taken and examined under a microscope for signs of cancer by a pathologist. The types of biopsy performed include:
- Excisional biopsy: After numbing the area with a local anesthetic, the entire mole is removed with a small border of surrounding skin. Where possible, this is the generally preferred method
- Punch biopsy: After numbing the area with a local anesthetic, a circular blade is pressed into the skin around the suspicious area, and a round piece of skin removed. This type of biopsy is carried out, when the lesion is large in size
- Incisional biopsy: After numbing the area with a local anesthetic, a portion of the tumor is removed using a surgical knife
According to the American Joint Committee on Cancer TNM system, Melanoma In Situ is categorized as Stage 0-Tis N0 M0, meaning that the tumor is confined to the epidermis and there is no involvement of lymph nodes, or other distant organs.
Many clinical conditions may have similar signs and symptoms. Your healthcare provider may perform additional tests to rule out other clinical conditions to arrive at a definitive diagnosis.
Treatments For Stage I Melanoma
Your doctor will most likely treat stage 1 melanoma with surgery called wide excision, which cuts out the melanoma along with a margin of healthy surrounding skin. The amount of healthy skin removed is determined by the location and the thickness of the melanoma being treated.
While wide excision surgery is often the only treatment necessary, in some cases a doctor may also choose to check for cancer in nearby lymph nodes by performing a sentinel lymph node biopsy. If cancer cells are found in the lymph nodes, further treatment will become necessary, such as a lymph node dissection , chemotherapy, immunotherapy, or targeted therapies.
Recommended Reading: What Are The Forms Of Skin Cancer
What Is A Pathology Report
A pathologist is a doctor who diagnoses diseases by looking at tissue from the body. Samples of your melanoma tissue, removed during surgery or biopsy, will be sent to them for review. The pathology report is a result of their findings. This report contains important information about the tumor which is used to make treatment decisions. You should ask for a copy of this report and keep it in your personal medical files.
Who Gets Melanoma In Situ Of Skin
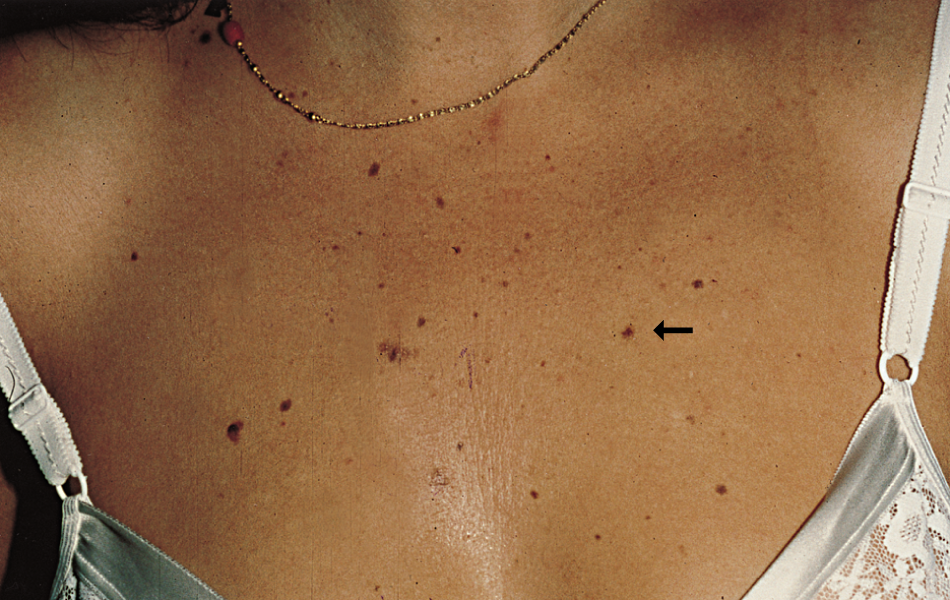
- Melanoma In Situ of Skin can occur in young, as well as old individuals, and is one of the most common cancers in people younger than 30 years
- In the United States, it has been observed that women are at increased risk before the age of 40 years, while men are at a higher risk after the age of 40 years
- Cutaneous Melanoma also occurs more frequently in Caucasians, as compared to other races
You May Like: Does Skin Cancer Burn And Itch
Surgical Treatment Of Stage I Melanoma
The standard treatment of stage I melanoma is surgical removal with pathologically confirmed negative margins. Efforts been made to reduce the amount of normal skin removed without compromising the cure rate achieved with surgery. A melanoma greater than 1 millimeter appears to require a greater surgical margin to reduce the rate of recurrence at the site of origin. Most surgeons recommend a surgical margin of 2 centimeters surrounding the entire cancer for melanomas greater than 1 mm. The need for skin grafting occurs in approximately 10% of patients. Surgical margins greater than 2 cm are no more effective and require skin grafting in a higher fraction of patients .
Evaluation of the regional lymph nodes by performing a sentinel lymph node biopsy as a staging procedure for patients with a primary melanoma greater than 1 mm is recommended. SLNB should also be considered in patients with thin melanomas and adverse prognostic factors, such as vertical growth phase, Clark Level IV, regression, and ulceration.
The surgical treatment of stage I melanoma typically involves a single procedure in which a local excision of the cancer is performed as well as a SLNB. Approximately 15% of patients undergoing SLNB have a positive SLN . Ninety-five percent of patients with a confirmed negative sentinel node are free of cancer and require no additional treatment.
Treating Stage Iv Melanoma
Stage IV melanomas have already spread to distant lymph nodes or other areas of the body. Skin tumors or enlarged lymph nodes causing symptoms can often be removed by surgery or treated with radiation therapy.
Metastases in internal organs are sometimes removed, depending on how many there are, where they are, and how likely they are to cause symptoms. Metastases that cause symptoms but cannot be removed may be treated with radiation, immunotherapy, targeted therapy, or chemotherapy.
The treatment of widespread melanomas has changed in recent years as newer forms of immunotherapy and targeted drugs have been shown to be more effective than chemotherapy.
Immunotherapy drugs called checkpoint inhibitors such as pembrolizumab or nivolumab are typically the first drugs tried, especially in people whose cancer cells do not have BRAF gene changes. These drugs can shrink tumors for long periods of time in some people. Ipilimumab , a different type of checkpoint inhibitor, is not typically used by itself as the first treatment, although it might be combined with nivolumab or pembrolizumab. This slightly increase the chances that the tumor will shrink, although itâs also more likely to result in serious side effects, which needs to be considered carefully. People who get any of these drugs need to be watched closely for serious side effects..
Itâs important to carefully consider the possible benefits and side effects of any recommended treatment before starting it.
Read Also: How To Identify Basal Cell Carcinoma
Lentigo Maligna And Melanoma In Situ
What are lentigo maligna and melanoma in situ?
Lentigo maligna and melanoma in situ are the very earliest stage of a skin cancer called melanoma.
The word melanoma comes from the Greek word melas, meaning black. Melanin is the dark pigment that gives the skin its natural colour.
Melanin is made in the skin by pigment cells called melanocytes. After our skin is exposed to sunlight, the melanocytes make more melanin, and so the skin becomes darker.
Melanocytes sometimes grow together in harmless groups or clusters, which are known as moles. Most people have between 10 and 50 moles and often they are darker than the surrounding skin.
Melanomas can arise in or near to a mole, but can also appear on skin that looks quite normal. They develop when the skin pigment cells become cancerous and multiply in an uncontrolled way. They can then invade the skin around them and may also spread to other areas such as the lymph nodes, liver and lungs.
In situ means that the cancer cells have not had the opportunity to spread to anywhere else in the body. There are cancer cells in the top layer of the skin but they are all contained in the area in which they began to develop. They have not started to spread or grow into deeper layers of the skin and have not become invasive. This is why some doctors call in situ cancers pre cancer. The prognosis is excellent.
What causes lentigo maligna and melanoma in situ?
Some people are more likely to get a melanoma than others:
Stages Of Melanoma Skin Cancer
Staging describes or classifies a cancer based on how much cancer there is in the body and where it is when first diagnosed. This is often called the extent of cancer. Information from tests is used to find out the size of the tumour, which parts of the skin have cancer, whether the cancer has spread from where it first started and where the cancer has spread. Your healthcare team uses the stage to plan treatment and estimate the outcome .
The most common staging system for melanoma skin cancer is the TNM system. For melanoma skin cancer there are 5 stages stage 0 followed by stages 1 to 4. Often the stages 1 to 4 are written as the Roman numerals I, II, III and IV. Generally, the higher the stage number, the more the cancer has spread. Talk to your doctor if you have questions about staging.
When describing the stage, doctors often use the words early stage, locoregional or metastatic.
Early stage means that the cancer is only in where it started and has not spread to other parts of the body. It includes stage 0, stage 1A, stage 1B, stage 2A, stage 2B and stage 2C melanoma skin cancers.
Locoregional means the cancer has spread to nearby lymph nodes, or it has spread to nearby areas of skin or lymph vessels. It includes stage 3 melanoma skin cancer.
Metastatic means that the cancer is in a part of the body farther from where it started. It includes stage 4 melanoma skin cancer.
Find out more about .
Also Check: What Is The Survival Rate For Invasive Ductal Carcinoma
Putting It All Together
Some pieces of the report are used to determine the stage of the cancer and other pieces play a role in deciding what treatment is needed. By understanding the basics of the report, you will be better able to discuss your treatment options with your healthcare team. Your provider will be able to explain any questions you have about your report.
Melanoma In Situ Of The Skin
What is melanoma in situ?
Melanoma in situ is a type of early, non-invasive skin cancer. The tumour is made up of specialized cells called melanocytes. Another name for melanoma in situ is lentigo maligna. In melanoma in situ, the abnormal melanocytes are only found in the top layer of the skin called the epidermis. If left untreated, this tumour can change over time into a type of cancer called invasive melanoma.
Skin
Skin is made up of three layers: epidermis, dermis, and subcutaneous fat. The surface and the part you can see when you look at your skin is called the epidermis. The cells that make up the epidermis include squamous cells, basal cells, melanocytes, Merkel cells, and cells of the immune system. The squamous cells in the epidermis produce a material called keratin which makes the skin waterproof and strong and protects us from toxins and injuries.
The dermis is directly below the epidermis. The dermis is separated from the epidermis by a thin layer of tissue called the basement membrane. The dermis contains blood vessels and nerves. Below the dermis is a layer of fat called subcutaneous adipose tissue.
Melanocytes
Melanocytes are small cells that produce melanin, a dark pigment that helps protect our skin from the suns ultraviolet rays. The amount of melanin normally found in our skin determines our skin colour. People with very light skin produce very little melanin while people with very dark skin produce a lot of melanin.
You May Like: What Is Braf Melanoma
How Is Melanoma Staged
Melanoma stages are assigned using the TNM system.
The stage of the disease indicates how much the cancer has progressed by taking into account the size of the tumor, whether its spread to lymph nodes, and whether its spread to other parts of the body.
A doctor can identify a possible melanoma during a physical exam and confirm the diagnosis with a biopsy, where the tissue is removed to determine if its cancerous.
But more sophisticated technology, such as PET scans and sentinel lymph node biopsies, are necessary to determine the cancers stage or how far its progressed.
There are five stages of melanoma. The first stage is called stage 0, or melanoma in situ. The last stage is called stage 4. Survival rates decrease with later stages of melanoma.
Its important to note that survival rates for each stage are just estimates. Each person with melanoma is different, and your outlook can vary based on a number of different factors.
Available Evidence On Histologic Clearance Margins In Mis
Thirty-two articles were identified that met the inclusion criteria for this review . The majority of the articles were reviews of single-surgeon or single-institution experiences using MMS or SE for surgical treatment of MIS and/or LM. No RCTs were identified. It should be noted that a subset of studies of LM included patients with lentigo maligna melanoma we focused our review on the subcohort of patients with LM only. As previously mentioned, if the analysis did not separate in situ from invasive lesions, the study was excluded.
Don’t Miss: Is Melanoma Cancer Curable
What Are The Signs And Symptoms Of Melanoma In Situ Of Skin
Melanoma In Situ of Skin can develop from an existing mole or appear as a new spot. The signs and symptoms may include:
- A pigmented area that is Asymmetrical in shape, whose Borders are irregular or ragged
- A pigmented area that is not Colored uniformly, unlike a benign mole, which has an even distribution of shades
- Any suspicious looking spot, whose Diameter is more than ¼ inches
- Any suspicious looking spot that is Evolving, or changing in shape/color
These signs are often collectively referred to as the âABCDE characteristicsâ of melanoma, by physicians.
- A suspicious looking spot or a âpotential melanomaâ often differs in appearance from other benign moles on the body. This variability is sometimes called the ugly duckling sign by physicians
- A suspicious pigmented area/spot showing a spread of color to the surrounding skin and with any swelling, redness or itching . Such areas may also be scaly, or exhibit some oozing of fluid, or bleeding
What Is Melanoma In Situ Of Skin
- A melanoma is a type of cancer that develops from cells, called melanocytes. Melanocytes are cells that produce melanin the pigment that gives skin its color
- Normal skin is composed of three layers:
- Epidermis – the outermost protective layer
- Dermis – the middle layer containing blood vessels, sweat glands, hair follicles, and nerves
- Subcutis – composed of fat and a protein called collagen
The epidermis and dermis are separated by a layer, called the basement membrane.
- Melanomas that are confined to the epidermis and have not yet penetrated through the basement membrane are called, Melanoma In Situ of Skin. They are usually brown or black in color, but sometimes may be pink, tan, or white
- Although melanomas may occur anywhere on the body, Cutaneous Melanoma In Situ generally occur on sun-exposed areas. Some of the common sites include:
- Chest and back in men
- Legs in women
- Neck and face
You May Like: Squamous Cell Carcinoma Skin Metastasis
What Is Stage 0 Melanoma
In Stage 0 melanoma, the malignant tumor is still confined to the upper layer of the skinthe epidermiswhich means the cancer cells are only in the outer layer of the skin and have not grown into the second layer of skin, called the dermis. Stage 0 melanoma is not considered invasive melanoma the other stages are invasive. In Stage 0 melanoma, there is no evidence the cancer has spread to the lymph nodes or to distant sites . Stage 0 is local melanoma, meaning it has not spread beyond the primary tumor. Another term for Stage 0 melanoma is in situ, which means in place in Latin.
What Is Melanomain Situ
Melanoma in situ is an early form of primary melanoma in which the malignant cells are confined to the tissue of origin, the epidermis. It is also known as in-situ melanoma and level 1 melanoma.
As melanoma in situ has no associated mortality, early detection of melanoma in an in-situ phase increases survival from melanoma and leads to less morbidity and decreased costs compared to that associated with more advanced melanoma .
Management of melanoma is evolving. For up to date recommendations, refer to Australian Cancer Council Clinical practice guidelines for the diagnosis and management of melanoma.
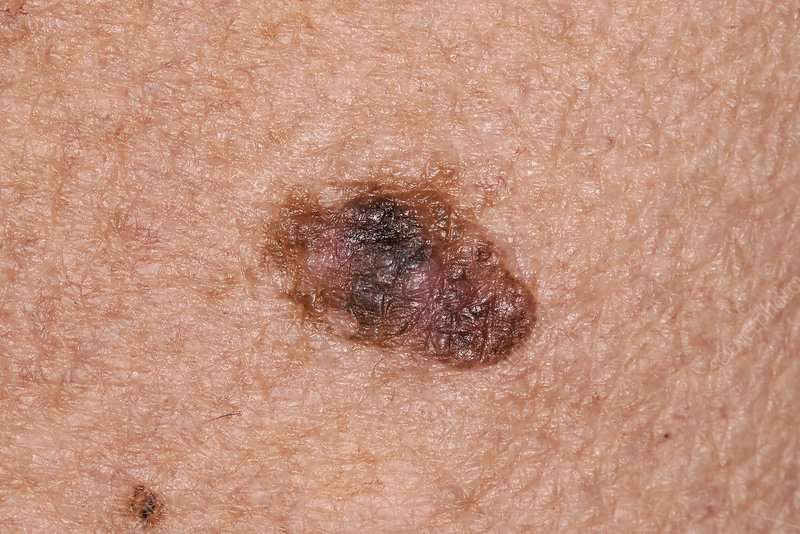
Melanoma in situ
See more images of melanoma in situ.
Also Check: What Is The Survival Rate For Invasive Ductal Carcinoma
Signs Of Melanoma In Situ
According to the American Cancer Society, the most important warning sign of melanoma is an existing mole or spot on the skin that is changing in shape, color, or size. This spot may look vastly different from the other spots on your skin. A new lesion on the skin can also indicate melanoma. If you notice any of these warning signs, see your physician at once.
The ABCDE rule is an easy-to-remember guide to help you identify melanoma. When performing your monthly at home skin check, look for:
- Asymmetry: A birthmark or mole that is not symmetrical. That means that one-half does not match the other.
- Border: Look for edges that are blurred, notched, ragged or otherwise irregular.
- Color: The color may include different shades of black or brown. It will usually not have the same color all over. It may sometimes appear with patches of blue, white or pink.
- Diameter: Any spot or mole larger than about ¼ inch should be checked by a physician.
- Evolving: A spot or mole that is changing in color, shape or size.
If you notice any of the above symptoms, contact a dermatologist right away. Additionally, keep in mind that a dermatologist’s eye is going to be much more advanced at detecting cancers. Keep up with your annual or biannual skin checks for maximum protection.