Treatment Of Squamous Cell Carcinoma
-
Usually locally destructive techniques
Treatment of squamous cell carcinoma is similar to that for basal cell carcinoma and includes curettage and electrodesiccation, surgical excision, cryosurgery, topical chemotherapy and photodynamic therapy, or, occasionally, radiation therapy. Treatment and follow-up must be monitored closely because of the greater risk of metastasis compared with a basal cell carcinoma.
Squamous cell carcinoma on the lip or other mucocutaneous junction should be excised at times, cure is difficult.
Recurrences and large tumors should be treated aggressively with Mohs microscopically controlled surgery, in which tissue borders are progressively excised until specimens are tumor-free , or by a team approach with surgery and radiation therapy. Because tumors with perineural invasion are aggressive, radiation therapy should be considered after surgery.
Metastatic disease is responsive to radiation therapy if metastases can be identified and are isolated. Widespread metastases do not respond well to chemotherapeutic regimens. For inoperable advanced disease or metastatic disease, programmed death receptor 1 inhibitors are now an option.
What Causes Squamous Cell Cancer
Skin cancer is caused by mutations that occur in skin cell DNA. These changes cause abnormal cells to multiply out of control. When this occurs in the squamous cells, the condition is known as SCC.
UV radiation is the most common cause of the DNA mutations that lead to skin cancer. UV radiation is found in sunlight as well as in tanning lamps and beds.
While frequent exposure to UV radiation greatly increases your risk of skin cancer, the condition can also develop in people who dont spend much time in the sun or in tanning beds.
These people may be genetically predisposed to skin cancer, or they may have weakened immune systems that increase their likelihood of getting skin cancer.
Those who have received radiation treatment may also be at greater risk of skin cancer.
Risk factors for SCC include:
- having fair skin
- having light-colored hair and blue, green, or gray eyes
- having long-term exposure to UV radiation
- living in sunny regions or at a high altitude
- having a history of multiple severe sunburns, especially if they occurred early in life
- having a history of being exposed to chemicals, such as arsenic
Treating Squamous Cell Carcinoma Of The Skin
Treatment options for squamous cell skin cancer depend on the risk of the cancer coming back, which is based on factors like the size and location of the tumor and how the cancer cells look under a microscope, as well as if a person has a weakened immune system.
Most squamous cell skin cancers are found and treated at an early stage, when they can be removed or destroyed with local treatment methods. Small squamous cell cancers can usually be cured with these treatments. Larger squamous cell cancers are harder to treat, and fast-growing cancers have a higher risk of coming back.
In rare cases, squamous cell cancers can spread to lymph nodes or distant parts of the body. If this happens, treatments such as radiation therapy, immunotherapy, and/or chemotherapy may be needed.
Don’t Miss: How To Know If You Have Skin Cancer
How Serious Is A Squamous Cell Skin Cancer
Squamous cell carcinomaskinSquamous cell carcinomaskinsquamous cell carcinomaskinserious
Though not as common as basal cell , squamous cell is more serious because it is likely to spread . Treated early, the cure rate is over 90%, but metastases occur in 1%5% of cases.
One may also ask, what does squamous cell carcinoma look like? Squamous cell carcinomas may appear as flat reddish or brownish patches in the skin, often with a rough, scaly, or crusted surface. They tend to grow slowly and usually occur on sun-exposed areas of the body, such as the face, ears, neck, lips, and backs of the hands. Normal moles also develop from these skin cells.
Subsequently, question is, how do you know if squamous cell skin cancer has spread?
A biopsy is the only way to tell for sure if you have skin cancer and what kind it is. In rare cases basal and squamous cell skin cancer can spread to the nearby lymph nodes Ask your doctor if your lymph nodes will be tested.
Is squamous cell carcinoma a fast growing cancer?
Squamous Cell Carcinoma SCC is generally a slow growing tumor that tends to grow without physical symptoms. However, some forms of this cancer may be fast growing and painful, especially when the lesions are large. They may become irritated and bleed.
How Do Dermatologists Diagnose Squamous Cell Carcinoma Of The Skin
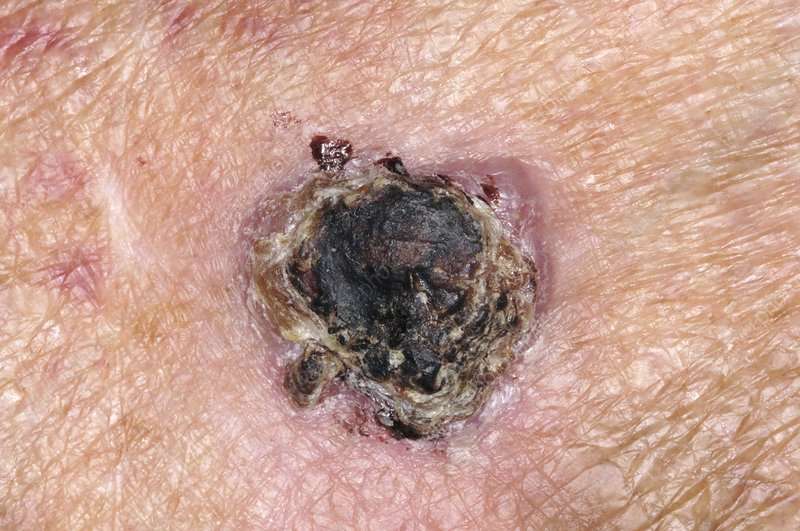
Because this cancer begins on the skin, its possible to find it early when its highly treatable.
When you see a board-certified dermatologist, your dermatologist will examine your skin carefully.
If your dermatologist finds a spot on your skin that could be any type of skin cancer, your dermatologist will first numb the area and then remove all of it. This can be done during an office visit and is called a skin biopsy. This is a simple procedure, which a dermatologist can quickly, safely, and easily perform.
Having a skin biopsy is the only way to know for sure whether you have skin cancer.
What your dermatologist removes will be examined under a high-powered microscope. Your dermatologist or a doctor who has in-depth experience diagnosing skin growths, such as a dermatopathologist, is best qualified to examine the removed tissue under a microscope.
After examining the removed tissue, the doctor writes a biopsy report. Also called a pathology report, this report explains what was seen under the microscope, including whether any skin cancer cells were seen.
If you have squamous cell carcinoma of the skin, the report will contain the following information when possible:
-
Type of SCC
-
Whether the cancer has any features that make it aggressive
Also Check: How Does Skin Cancer Feel
Skin Cancer Types: Squamous Cell Carcinoma Overview
All content solely developed by the American Academy of Dermatology
The American Academy of Dermatology gratefully acknowledges the support from Sanofi Genzyme and Regeneron.
Squamous cell carcinoma of the skin
What is squamous cell carcinoma of the skin?A common type of skin cancer, squamous cell skin cancer can develop from a pre-cancerous skin growth called an actinic keratosis .
Is it contagious? No
Skin Cancer Support Groups And Counseling
Living with skin cancer presents many new challenges for you and for your family and friends. You will probably have many worries about how the cancer will affect you and your ability to “live a normal life,” that is, to care for your family and home, to hold your job, and to continue the friendships and activities you enjoy.
Many people with a skin cancer diagnosis feel anxious and depressed. Some people feel angry and resentful others feel helpless and defeated. For most people with skin cancer, talking about their feelings and concerns helps. Your friends and family members can be very supportive. They may be hesitant to offer support until they see how you are coping. Don’t wait for them to bring it up. If you want to talk about your concerns, let them know.
Continued
Some people don’t want to “burden” their loved ones, or prefer talking about their concerns with a more neutral professional. A social worker, counselor, or member of the clergy can be helpful. Your dermatologist or oncologist should be able to recommend someone.
Many people with cancer are profoundly helped by talking to other people who have cancer. Sharing your concerns with others who have been through the same thing can be remarkably reassuring. Support groups for people with cancer may be available through the medical center where you are receiving your treatment. The American Cancer Society also has information about support groups throughout the U.S.
Recommended Reading: What Are The Three Types Of Skin Cancer
Expert Treatment For Squamous Cell Carcinoma
Squamous cell carcinoma is a highly treatable form of cancer, especially when detected early. At ColumbiaDoctors Dermatology we offer a full range of treatments, which include surgery, radiation therapy, and cyrosurgery. Our physicians will help you develop the best treatment plan for your specific set of circumstances. Treatments include:
What Patients And Caregivers Need To Know Abo
This the most important factor in determining treatment and probable outcome. What patients and caregivers need to know abo. There are different staging guidelines for basal and squamous cell cancer and melanoma. The aad’s coronavirus resource center will help you find information about how you can continue to care for your skin, hair, and nails. Some types of skin cancer are more dangerous than others, but if you have a spot. Being armed with information is vital to begin the fight. Skin cancer is the most common type of cancer in the united states by a pretty large margin, and it does not discriminate. A cancer diagnosis can leave you unable to comprehend anything else your doctor says, but it’s important to pay attention to what stage of cancer you have. The stage of a basal or squamous cell skin cancer is a description of how widespread the cancer is. Not only does the stage tell you how serious the disease is, but it can help you and. According to the american cancer society, just over 100,000 new cases of skin cancer are diagnosed in the united states each year. The aad’s coronavirus resource center will help you find information about how you can continue to care for your skin, hair, and nails. Cancer stages describe the size of the primary tumor and how far cancer has spread.
Read Also: How To Tell If You Have Skin Cancer
Tumour Staging For Cutaneous Scc
TX: Th Primary tumour cannot be assessed
T0: No evidence of a primary tumour
Tis: Carcinoma in situ
T1: Tumour 2cm without high-risk features
T2: Tumour 2cm or Tumour 2 cm with high-risk features
T3: Tumour with the invasion of maxilla, mandible, orbit or temporal bone
T4: Tumour with the invasion of axial or appendicular skeleton or perineural invasion of skull base
After Skin Cancer Treatment
Most skin cancer is cured surgically in the dermatologist’s office. Of skin cancers that do recur, most do so within three years. Therefore, follow up with your dermatologist as recommended. Make an appointment immediately if you suspect a problem.
If you have advanced malignant melanoma, your oncologist may want to see you every few months. These visits may include total body skin exams, regional lymph node checks, and periodic chest X-rays and body scans. Over time, the intervals between follow-up appointments will increase. Eventually these checks may be done only once a year.
Recommended Reading: When Squamous Cell Carcinoma Spreads
Basal Cell Carcinoma Stages
There are certain features that are considered to make the cancer at higher risk for spreading or recurrence, and these may also be used to stage basal cell carcinomas. These include:
- Greater than 2 mm in thickness
- Invasion into the lower dermis or subcutis layers of the skin
- Invasion into the tiny nerves in the skin
- Location on the ear or on a hair-bearing lip
After the TNM components and risk factors have been established, the cancer is given a stage. For basal cell carcinoma staging, the factors are grouped and labeled 0 to 4. The characteristics and stages of basal cell carcinoma are:
Stage 0: Also called carcinoma in situ, cancer discovered in this stage is only present in the epidermis and has not spread deeper to the dermis.
Stage 1 basal cell carcinoma: The cancer is less than 2 centimeters, about 4/5 of an inch across, has not spread to nearby lymph nodes or organs, and has one or fewer high-risk features.
Stage 2 basal cell carcinoma: The cancer is larger than 2 centimeters across, and has not spread to nearby organs or lymph nodes, or a tumor of any size with 2 or more high-risk features.
Stage 3 basal cell carcinoma: The cancer has spread into facial bones or 1 nearby lymph node, but not to other organs.
Stage 4 basal cell carcinoma: The cancer can be any size and has spread to 1 or more lymph nodes which are larger than 3 cm and may have spread to bones or other organs in the body.
Who Is Most Likely To Have A Squamous Cell Carcinoma
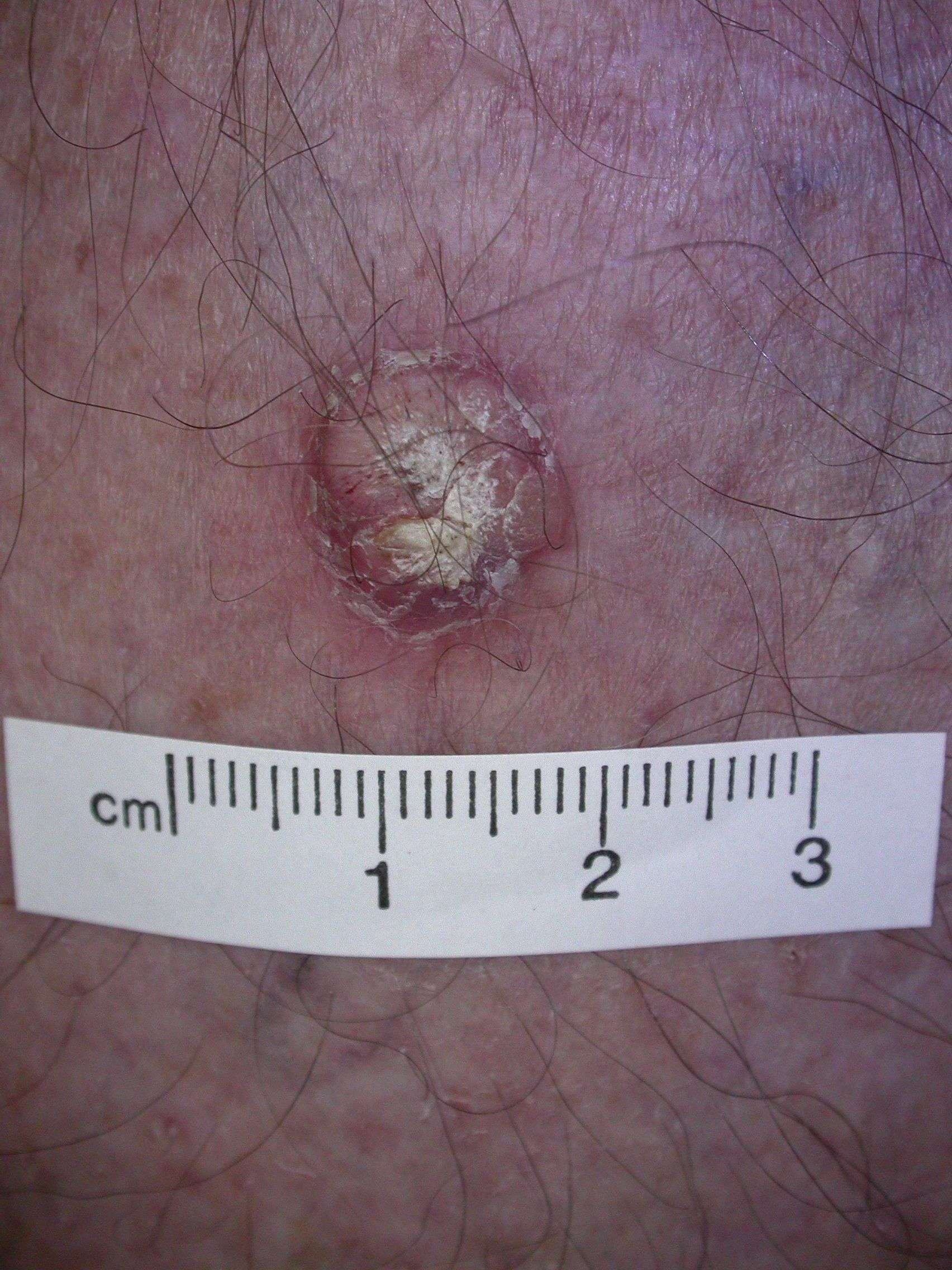
The following groups of people are at greater risk of developing SCC:
- Immunosuppressed individuals either due to medical treatment, such as methotrexate, ciclosporin and azathioprine, or due to diseases which affect immune function, including inherited diseases of the immune system or acquired conditions such as leukaemia or HIV
- Patients who have had an organ transplant because of the treatment required to suppress their immune systems to prevent organ rejection
- People who are more susceptible to sunburn
- People who have had significant cumulative ultraviolet light exposure, for example:
- people who have lived in countries near to the equator, or who have been posted to work in these countries, e.g. military personnel, construction workers
- outdoor workers, such as builders, farmers
- people of advanced years, who have had a lifetime of frequent sun exposure
Don’t Miss: What Is The Leading Cause Of Skin Cancer
What Are The Symptoms Of Squamous Cell Skin Cancer Of The Head And Neck
Squamous cell skin cancers usually present as an abnormal growth on the skin or lip. The growth may have the appearance of a wart, crusty spot, ulcer, mole or a sore that does not heal. It may or may not bleed and can be painful. If you have a preexisting mole, any changes in the characteristics of this spot such as a raised or irregular border, irregular shape, change in color, increase in size, itching or bleeding are warning signs. Pain and nerve weakness are concerning for cancer that has spread. Sometimes a lump in the neck can be the only presenting sign of skin cancer that has spread to lymph nodes, particularly when there is a history of previous skin lesion removal.
How Is Squamous Cell Carcinoma Diagnosed
Diagnosis of cutaneous SCC is based on clinical features. The diagnosis and histological subtype are confirmed pathologically by diagnostic biopsy or following excision. See squamous cell carcinoma pathology.
Patients with high-risk SCC may also undergo staging investigations to determine whether it has spread to lymph nodes or elsewhere. These may include:
- Imaging using ultrasound scan, X-rays, CT scans, MRI scans
- Lymph node or other tissue biopsies
Don’t Miss: How To Know If It’s Skin Cancer
The Difference Between Basal Cell Carcinoma And Squamous Cell Carcinoma
Basal cell carcinoma and squamous cell carcinoma are the two most common types of skin cancers. According to the American Cancer Society, over 5 million cases of basal cell and squamous cell cancers are diagnosed every year. Though, basal cell carcinoma occurs more often, taking credit for about 80% of these cases. Other than the disparities in occurrence, what is the difference between basal cell and squamous cell carcinomas? You may also be wondering is squamous cell worse than basal cell, or vice versa. Here is some insight.
What Are Symptoms Of Squamous Cell Carcinoma
Squamous cell carcinoma tends to develop on sun-exposed areas of the body such as the face, lips, ears, scalp, neck, shoulders, backs of the hands, and forearms, though it may occur anywhere on the skin.
Characteristics of squamous cell carcinomas include:
- Raised growths or lumps, which may be depressed in the center
- Rough or scaly red patches, which may crust or bleed
- Open sores that may ooze or crust over, dont completely heal, or that heal and return
- A flat area only slightly different from normal skin
Also Check: How Do You Get Melanoma Cancer
When To Seek Medical Care
If you have developed a new bump on sun-exposed skin, or if you have a spot that bleeds easily or does not seem to be healing, then you should make an appointment with your primary care physician or with a dermatologist. You should also make an appointment if an existing spot changes size, shape, color, or texture, or if it starts to itch, bleed, or become tender.Try to remember to tell your doctor when you first noticed the lesion and what symptoms, if any, it may have . Also be sure to ask your parents, siblings, and adult children whether or not they have ever been diagnosed with skin cancer, and relay this information to your physician.
For More Information About Skin Cancer
National Cancer Institute, Cancer Information Service Toll-free: 4-CANCER 422-6237TTY : 332-8615
Skin Cancer Foundation
Media file 1: Skin cancer. Malignant melanoma.
Media file 2: Skin cancer. Basal cell carcinoma.
Media file 3: Skin cancer. Superficial spreading melanoma, left breast. Photo courtesy of Susan M. Swetter, MD, Director of Pigmented Lesion and Cutaneous Melanoma Clinic, Assistant Professor, Department of Dermatology, Stanford University Medical Center, Veterans Affairs Palo Alto Health Care System.
Media file 4: Skin cancer. Melanoma on the sole of the foot. Diagnostic punch biopsy site located at the top. Photo courtesy of Susan M. Swetter, MD, Director of Pigmented Lesion and Cutaneous Melanoma Clinic, Assistant Professor, Department of Dermatology, Stanford University Medical Center, Veterans Affairs Palo Alto Health Care System.
Media file 5: Skin cancer. Melanoma, right lower cheek. Photo courtesy of Susan M. Swetter, MD, Director of Pigmented Lesion and Cutaneous Melanoma Clinic, Assistant Professor, Department of Dermatology, Stanford University Medical Center, Veterans Affairs Palo Alto Health Care System.
Continued
Media file 6: Skin cancer. Large sun-induced squamous cell carcinoma on the forehead and temple. Image courtesy of Dr. Glenn Goldman.
Don’t Miss: What Is Good For Skin Cancer
Diagnosing Squamous Cell Carcinoma
The main way to diagnose squamous cell carcinoma is with a biopsy. This involves having a small piece of tissue removed from the suspicious area and examined in a laboratory.
In the laboratory, a pathologist will examine the tissue under a microscope to determine if it is a skin cancer. He or she will also stage the cancer by the number of abnormal cells, their thickness, and the depth of penetration into the skin. The higher the stage of the tumor, the greater the chance it could spread to other parts of the body.
Squamous cell carcinoma on sun-exposed areas of skin usually does not spread. However, squamous cell carcinoma of the lip, vulva, and penis are more likely to spread. Contact your doctor about any sore in these areas that does not go away after several weeks.