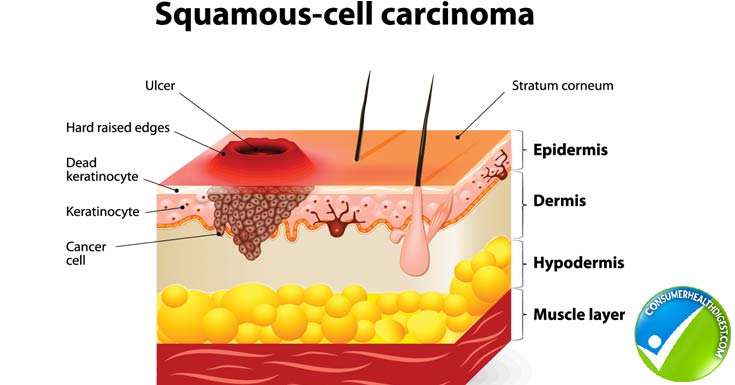
Symptoms Of Squamous Cell Carcinoma
Squamous cell carcinoma is characterized by its thick, scaly, irregular appearance, but it can have various appearances, and a doctor may be suspicious of any sores on sun-exposed surfaces that do not heal.
Squamous cell carcinoma begins as a red area with a scaly, crusted surface. As it grows, the tumor may become somewhat raised and firm, sometimes with a wartlike surface. Eventually, the cancer becomes an open sore and grows into the underlying tissue.
Squamous cell carcinomas can have various appearances. This photo shows one that is raised, scaly, and crusted.
This red, irregular area on the arm was diagnosed as squamous cell carcinoma after a biopsy.
Squamous cell carcinomas can have various appearances. This photo shows an area that is scaly, crusted, and darker than the surrounding skin. It was diagnosed as squamous cell carcinoma after a biopsy.
This squamous cell carcinoma on the lip shows excess build up of keratin that has broken down to form an open sore.
What Is The Outlook For Someone Who Has Squamous Cell Carcinoma Of The Skin
When found early, this cancer is highly treatable. Left untreated, however, SCC can spread deep into the skin and travel to other parts of the body, making treatment difficult.
While treatment can remove the cancer, its important to know that this cancer can return. You also have a greater risk of developing another skin cancer.
Thats why self-care becomes so important after treatment for SCC of the skin. Youll find the self-care that dermatologists recommend at, Squamous cell carcinoma of the skin: Self-care.
ImagesGetty Images
ReferencesAlam M, Armstrong A, et al. Guidelines of care for the management of cutaneous squamous cell carcinoma. J Am Acad Dermatol 2018 78:560-78.
Anadolu-Brasie R, Patel AR, et al., Squamous cell carcinoma of the skin. In: Nouri K, et al. Skin Cancer. McGraw Hill Medical, China, 2008: 86-114.
Marrazzo G, Zitelli JA, et al. Clinical outcomes in high-risk squamous cell carcinoma patients treated with Mohs micrographic surgery alone. J Am Acad Dermatol 2019 80:633-8.
Que SKT, Zwald FO, et al. Cutaneous squamous cell carcinoma: Management of advanced and high-stage tumors. J Am Acad Dermatol 2018 78:249-61.
Ribero S, Stucci LS, et al. Drug therapy of advanced cutaneous squamous cell carcinoma: Is there any evidence? Curr Opin Oncol. 2017 29:129-35.
U.S. Food and Drug Administration. FDA approves cemiplimab-rwlc for metastatic or locally advanced cutaneous squamous cell carcinoma. New release issued 9/28/2018. Last accessed 1/13/2020.
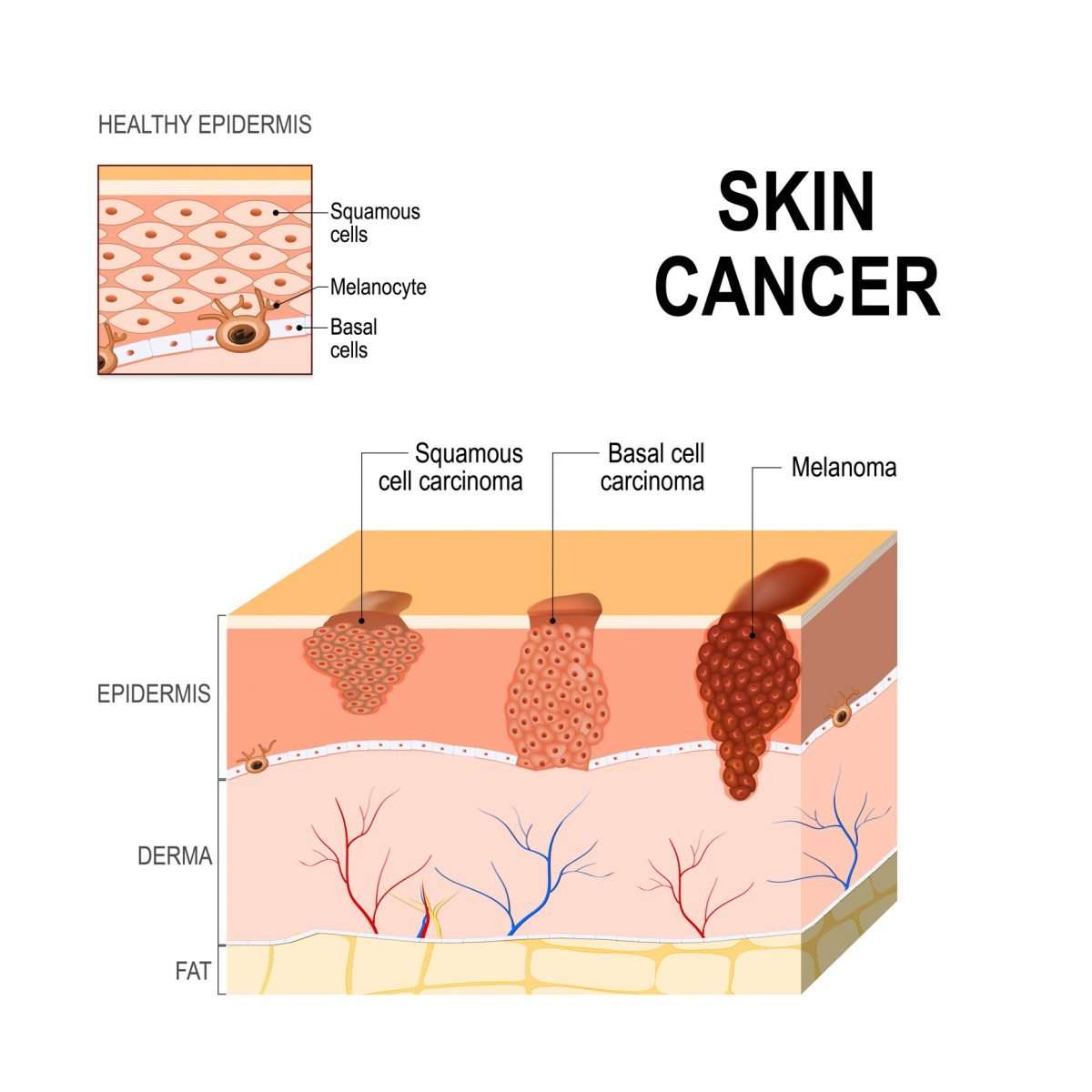
What Are The Different Types Of Skin Cancer
Your skin has multiple layers. The outer, protective layer of the skin is known as the epidermis. The epidermis is made up of squamous cells, basal cells, and melanocytes. These cells are constantly shedding to make way for fresh, new skin cells.
However, when certain genetic changes occur in the DNA of any of these cells, skin cancer can occur. The main types of skin cancer are squamous cell carcinoma, basal cell carcinoma, and malignant melanoma.
Recommended Reading: Invasive Ductal Carcinoma Survival Rate Stage 1
Mcc Stages: Making Sense Of It All
After testing is finished, your medical team will try to pinpoint how far the disease has progressed. This process is known as staging. Staging is a way to understand how much the cancer has grown and how far it has spread. This helps determine how to best treat it, and the risk of it coming back.
The TNM system is frequently used to stage MCC. Its a classification based on three factors:
- T represents the size of the original tumor, its growth rate and other factors.
- N indicates whether the cancer has spread to the local lymph nodes and to what extent.
- M stands for the spread or metastasis to distant lymph nodes and organs.
Once the patients TNM categories have been established, the overall stage number is assigned. As a rule, the lower the stage number, the less the disease has progressed.
MCC Staging
Stage 0
Tumor has not advanced beyond the outermost layer of skin. This stage is also called carcinoma in situ, which means in its original place.
Stage III
Tumor cells have advanced beyond the original tumor and may have traveled as far as the nearby lymph nodes, but not beyond.
Stage I and II
Tumor has not spread to nearby lymph nodes. Stage I includes smaller tumors and stage II includes larger and/or higher-risk tumors.
Stage IV
Tumor cells have spread to distant body areas, lymph nodes or organs.
These stages are each further broken down, from lowest to highest risk, depending on different characteristics of the original tumor and the areas where it has spread.
What Causes This Type Cancer
The reason why a particular dog may develop this, or any cancer, is not straightforward. Very few cancers have a single known cause. Most seem to be caused by a complex mix of risk factors, some environmental and some genetic or hereditary.
As with SCC in humans, exposure to ultraviolet rays/sunlight has been attributed to the development of these tumors. Exposure to papilloma-like viruses appears to contribute to multicentric SCC in the mouth and other areas of the skin where squamous cells are present.
Certain breeds are known to have an increased incidence of SCC, including Scottish Terriers, Pekingese, Boxer Dogs, Poodles, and Norwegian Elkhounds. SCC of the skin is also more common in dogs that are sparsely haired and have light-colored hair and skin . In contrast, large-breed dark-coated dogs are more prone to SCC of the toes .
Also Check: Skin Cancer Metastasis To Lymph Nodes
Perineural And Intravascular Invasion
Perineural invasion is associated with a poor prognosis including increased risk of local recurrence, distant metastasis and disease-specific death . Debate exists regarding the importance of the size of the nerve involved. Perineural invasion of named nerves is accepted as significant disease with poor prognosis. The significance of small caliber nerve invasion is controversial. In a retrospective cohort of 48 patients with perineural invasion, involvement of nerves > 0.1 mm had higher rates of local recurrence, nodal metastases, distant metastases and disease-specific death . A retrospective cohort study examining 114 cases of perineurally invasive SCC showed that tumors with large nerve invasion were significantly more likely to have other risk factors leading to recurrence and metastasis . Sixty-eight tumors had perineural invasion of small nerves . One tumor with perineural invasion of small caliber nerves had a single local recurrence. On univariate analysis, large nerve invasion was associated with increased risk of nodal metastasis and death from disease . When perineural invasion was combined with other risk factors such as lymphovascular invasion, invasion beyond subcutaneous fat, and tumor diameter greater than 2 cm, overall prognosis was poor. Tumors with multiple high-risk features are more likely to have a poor prognosis.
Treatment Of Stage Ii Paranasal Sinus And Nasal Cavity Cancer
For information about the treatments listed below, see the Treatment Option Overview section.
- If cancer is in the maxillary sinus, treatment is usually high-dose radiationtherapy before or after surgery.
- If cancer is in the ethmoid sinus, treatment is usually radiation therapy and/or surgery.
- If cancer is in the sphenoid sinus, treatment is the same as for nasopharyngeal cancer, usually radiation therapy with or without chemotherapy. for more information.)
- If cancer is in the nasal cavity, treatment is usually surgery and/or radiation therapy.
- For inverting papillomas, treatment is usually surgery with or without radiation therapy.
- For melanomas and sarcomas, treatment is usually surgery with or without radiation therapy and chemotherapy.
- For midline granulomas, treatment is usually radiation therapy.
- If cancer is in the nasal vestibule, treatment is usually surgery or radiation therapy.
Use our clinical trial search to find NCI-supported cancer clinical trials that are accepting patients. You can search for trials based on the type of cancer, the age of the patient, and where the trials are being done. General information about clinical trials is also available.
Don’t Miss: Cell Cancer Symptoms
What Is Metastatic Squamous Cell Carcinoma Of Skin
- Metastatic Squamous Cell Carcinoma of Skin is the advanced form of squamous cell carcinoma of skin a common malignant skin tumor that typically affects elderly men and women. In this condition, the skin cancer has already metastasized to the lymph nodes and various parts of the body
- Prolonged exposure to the suns ultraviolet rays may result in damage of skin DNA, causing squamous cell carcinoma. Other factors that may influence its development include skin tanning, radiation treatment for other reasons, previous burn injuries, and exposure to coal tar and arsenic
- Squamous cell carcinoma of skin may appear as slow-growing skin lesions, commonly on the sun-exposed areas, such as the face, neck, hands, and even the chest. The lesions may ulcerate and cause scarring of skin
- The treatment may include surgical procedures followed by radiation therapy or chemotherapy, as decided by the healthcare provider. Targeted therapy medications may also be used to destroy the tumor cells
- The prognosis of Metastatic Squamous Cell Carcinoma of Skin depends upon many factors including the health status of the affected individual it is generally guarded
Read Also: Invasive Ductal Breast Cancer Prognosis
Do You Need Chemotherapy For Squamous Cell Carcinoma
Because just about all squamous cell carcinoma is usually localized it is typically not treated with chemotherapy. Chemotherapy is used for widespread cancer cell eradication, not localized growths. Chemotherapy could be used for a very small percentage of these cases, typically if the cancer has spread.
About 95 percent of squamous cell carcinomas are detected early, and this makes them easy to treat. All treatment options are highly successful, but Mohs micrographic surgery is the most successful while taking the least amount of healthy skin.
Recommended Reading: Melanoma Cancer Prognosis
Diagnosing Squamous Cell Carcinoma
The main way to diagnose squamous cell carcinoma is with a biopsy. This involves having a small piece of tissue removed from the suspicious area and examined in a laboratory.
In the laboratory, a pathologist will examine the tissue under a microscope to determine if it is a skin cancer. He or she will also stage the cancer by the number of abnormal cells, their thickness, and the depth of penetration into the skin. The higher the stage of the tumor, the greater the chance it could spread to other parts of the body.
Squamous cell carcinoma on sun-exposed areas of skin usually does not spread. However, squamous cell carcinoma of the lip, vulva, and penis are more likely to spread. Contact your doctor about any sore in these areas that does not go away after several weeks.
Does Fluorouracil Work On Squamous Cell Carcinoma
4.6/5fluorouracilsquamous cellcancersisdoes
Likewise, people ask, what is the best treatment for squamous cell carcinoma?
Squamous Cell Skin Cancer Treatment
- Mohs Surgery. Mohs surgery has the highest cure rate of all therapies for squamous cell carcinomas.
- Curettage and Electrodessication. This very common treatment for squamous cell carcinoma is most effective for low-risk tumors.
- Cryosurgery.
- Laser Surgery.
Secondly, is Squamous Cell Carcinoma an aggressive cancer? Squamous cell carcinoma of the skin is usually not life-threatening, though it can be aggressive. Untreated, squamous cell carcinoma of the skin can grow large or spread to other parts of your body, causing serious complications.
In this regard, what type of chemo is used for squamous cell carcinoma?
One drug that is commonly used for topical chemotherapy to treat squamous cell carcinoma is fluorouracil .
What is the survival rate for squamous cell carcinoma?
The 5-year survival rates were 62% for patients with stage I disease, 80% for patients with stage II disease, 42% for patients with stage III, and 19% for patients with stage IV disease.
Don’t Miss: Skin Cancer Pictures Mayo Clinic
Squamous Cell Carcinoma Warning Signs
At the Bondi Junction Skin Cancer Clinic we use the adage The faster a Squamous Cell Carcinoma grows the faster it needs to go.
Faster growing Squamous Cell Carcinoma are more likely to be
- aggressive,
- Invade and potentially penetrate the skin
- spread .
If they do spread this high growth rate is often maintained leading to a rapidly progressive clinical course which is associated with higher fatality rates.
Any rapidly growing lump or change in a pre-existing or new skin growth, should prompt an immediate visit to a Bondi Junction Skin Cancer Clinic.
Squamous Cell Skin Cancer Of The Head And Neck Treatment
Surgery is the preferred management method for the majority of squamous cell skin cancers. Low-risk, early stage, small squamous cell cancers can be removed by Mohs surgery, which is a technique that spares normal tissue through repeated intraoperative margin testing, removing only the cancer and leaving adjacent normal tissue. Excision, curettage and desiccation, and cryosurgery can also be used to remove the cancer while sparing normal tissue. Radiation alone is an alternative for low-risk tumors when surgery is not desirable because of cosmetic concerns or medical reasons.
Large tumors and tumors with nerve or lymph node involvement are not suitable for Mohs surgery and require removal of at least 5-millimeter margins of normal tissue around the cancer and neck dissection for involved lymph nodes. Larger tumors require reconstruction, which can be done at the time of surgery if margin status is clear. Reconstruction should be staged when margins status is not clear.
Patients with high-risk tumors should meet with a radiation therapist to discuss postoperative radiation. Chemotherapy may be added to radiation for extensive lymph node involvement or positive margins that cannot be cleared with additional surgery. In patients with high-risk tumors who are not surgical candidates, systemic treatment with both radiation and chemotherapy is used. Such cases require multidisciplinary care by a team of surgeons, radiation oncologists and medical oncologists.
You May Like: How Fast Does Squamous Cell Carcinoma Spread
Can A Squamous Cell Skin Cancer Be Unpredictable
Squamous cell skin cancer can be unpredictable. My first squamous cell area did not hurt, but it bled. My second squamous cell area did not bleed, but it hurt. If you have an area appear suddenly and it doesnt go away within a relatively short period of time, please make an appointment to have it looked at.
You May Like: What Are The 4 Types Of Melanoma
Predictions Based On Doubling Times
Looking at doubling times of tumors is helpful only if the estimated doubling times can be used to predict the growth of a persons tumor. One study looked at predicted survival times of people who had inoperable lung cancers and found that there was a close correlation between survival predicted from doubling time and actual survival.
Recommended Reading: What Does Melanoma In Situ Look Like
What Are The Types Of Squamous Cell Carcinoma
Squamous cell carcinoma develops when the flat cells in the toplayer of skin grow and divide in an uncontrolled way.
You can get an SCC wherever there are squamous cells which is in manydifferent parts of the body. However, typically they appear on parts of theskin that have been exposed to a lot of ultraviolet radiation from the sunor from tanning beds.
An early form of skin cancer, called Bowens disease, which looks like a red, scaly patch, can also develop into an SCC if nottreated.
An SCC can be quite an aggressive cancer if left untreated. If you evernotice a sore, scab or scaly patch of skin that doesnt heal within 2 months,see a doctor.
Also Check: What Does Early Squamous Skin Cancer Look Like
What Causes Squamous Cell Cancer
Skin cancer is caused by mutations that occur in skin cell DNA. These changes cause abnormal cells to multiply out of control. When this occurs in the squamous cells, the condition is known as SCC.
UV radiation is the most common cause of the DNA mutations that lead to skin cancer. UV radiation is found in sunlight as well as in tanning lamps and beds.
While frequent exposure to UV radiation greatly increases your risk of skin cancer, the condition can also develop in people who dont spend much time in the sun or in tanning beds.
These people may be genetically predisposed to skin cancer, or they may have weakened immune systems that increase their likelihood of getting skin cancer.
Those who have received radiation treatment may also be at greater risk of skin cancer.
Risk factors for SCC include:
- having fair skin
- having light-colored hair and blue, green, or gray eyes
- having long-term exposure to UV radiation
- living in sunny regions or at a high altitude
- having a history of multiple severe sunburns, especially if they occurred early in life
- having a history of being exposed to chemicals, such as arsenic
You May Like: Body Cancer Symptoms
Cutaneous Basal Cell Carcinoma With Bone Metastases: An Orthopaedic Case Report
John Strony
1Department of Orthopaedic Surgery, Thomas Jefferson University Hospital, Philadelphia, PA, USA
2Rothman Orthopaedic Institute, Philadelphia, PA, USA
3Department of Pathology, Anatomy, and Cell Biology, Thomas Jefferson University Hospital, Philadelphia, PA, USA
Abstract
Basal cell carcinoma is the most common skin cancer, and its incidence is increasing. Though metastatic BCC is uncommon, the literature demonstrates a 0.0028%-0.55% rate of metastasis. We report on a patient treated at our institution who was found to have mBCC with osseous metastases. To our knowledge, this is the first report of mBCC in the orthopaedic literature. Orthopaedic oncologists should consider mBCC in patients diagnosed with carcinoma of unknown origin, with a known history of BCC, or individuals with light skin pigmentation and age 50 or greater. This can help clinicians make the correct diagnosis and provide the appropriate treatment.
1. Introduction
Cutaneous basal cell carcinoma is the most commonly diagnosed skin cancer, constituting ~80% of nonmelanoma skin cancers and with incidence rising . Rates are highest in elderly white men, and identified risk factors include UV exposure, fair complexion, immunosuppression, and ionizing radiation or arsenic exposure. While most clinicians consider it an indolent and at most locally invasive malignancy, it can in fact metastasize through both lymphatic and vascular means. Incidences of metastasis are estimated at 0.0028% to 0.55% .
How To Tell If Squamous Cell Carcinoma Has Spread
Many doctors will order a PET or CT scan once a squamous cell carcinoma diagnosis has been reached to ensure the cancer has not spread to other parts of the body and is contained within the layers of the skin. Your doctor may also test your lymph nodes near the tumor site.
Diagnostic services, staging services and a comprehensive range of treatments are all available at Moffitt Cancer Center, and referrals are not required. To learn more about squamous cell carcinoma stages and the treatment options for each, call or submit a new patient registration form online.
- BROWSE
Don’t Miss: Large Cell Cancers