Upper Tract Urothelial Cancer: What You Need To Know Summary:
Raoul S. Concepcion, MD, FACS, provides an overview of the epidemiology of upper tract urothelial carcinoma . He discusses the most recent efforts in improving management for the disease, particularly focusing on neoadjuvant chemotherapy when treating high-grade tumors and nonsurgical ways to combat low-grade UTUC.
Optimisation Of Ct Urography Technique
There are three main protocols for the intravenous administration of contrast medium which depend on the number of boluses of contrast used, single, double or triple bolus.38
The single bolus protocol is optimised for patients with haematuria at high risk of UTUC, renal masses and stones. This protocol consists of three series of image acquisition: an unenhanced series optimised for detecting stones, a nephrographic series optimised for detecting renal masses and an excretory series optimised for detecting UTUC.
The double bolus protocol involves a slightly lower radiation dose than the single bolus protocol. It uses less contrast medium than the single bolus protocol for demonstration of the nephrographic and excretory phases and so may not produce such an intense nephrogram for demonstration of renal cell carcinoma or excretory series for diagnosing UTUC. If the unenhanced series is excluded, and the enhanced nephrographic and excretory phases are acquired in one series, a low-dose protocol is achieved which is commonly used for the follow-up of patients with known bladder cancer or UTUC.32,39,40
Cellular Classification Of Transitional Cell Cancer Of The Renal Pelvis And Ureter
The majority of upper tract uroepithelial tumors are of transitional cellhistology. Squamous cell cancer of the urinary tract constitutes less than 15%of the tumors of the renal pelvis and a smaller percentage of ureteral tumors, and SCC is often associated with chronic calculus disease and infection.
Grade of transitional cell cancer of the upper tract has generally been foundto correlate with stage. Superficial tumors are generally grade I or II,whereas the majority of infiltrative tumors are grades III and IV. Prognosisis worse for patients with high-grade tumors than for thosewith low-grade tumors.
Read Also: Does Skin Cancer Burn And Itch
Role Of Metastasectomy In Utuc
In selected patients metastasectomy can be advantageous, however it is rarely performed. In a large German retrospective study in 15 different uro-oncological centres between 1991 and 2008, only 44 patients with distant metastases of the bladder or upper urinary tract underwent complete resection of all detectable metastases and were analysed. Resected metastatic sites were the following: retroperitoneal lymph nodes , distant lymph nodes , lung , bone , adrenal gland , brain , small intestine and skin . Systemic chemotherapy was administered in 35 of 44 patients before and/or after metastasectomy surgery. Median survival from initial diagnosis of metastases and subsequent resection was as follows: overall survival, 35 months and 27 months CSS, 38 months and 34 months and progression-free survival, 19 months and 15 months. Overall 5-year survival from metastasectomy for the entire cohort was 28%. Seventeen patients were still alive without progression at a median follow up of 8 months. Seven patients without disease progression survived for > 2 years and remained free from tumour progression at a median follow up of 63 months. No significant prognostic factors could be determined due to the limited patient numbers .
Chemotherapy followed by retroperitoneal LND for isolated retroperitoneal recurrence after nephroureterectomy for upper UTUC was feasible and safe treatment that may be potentially therapeutic in selected patients .
Management Of Distal Ureter And Bladder Cuff
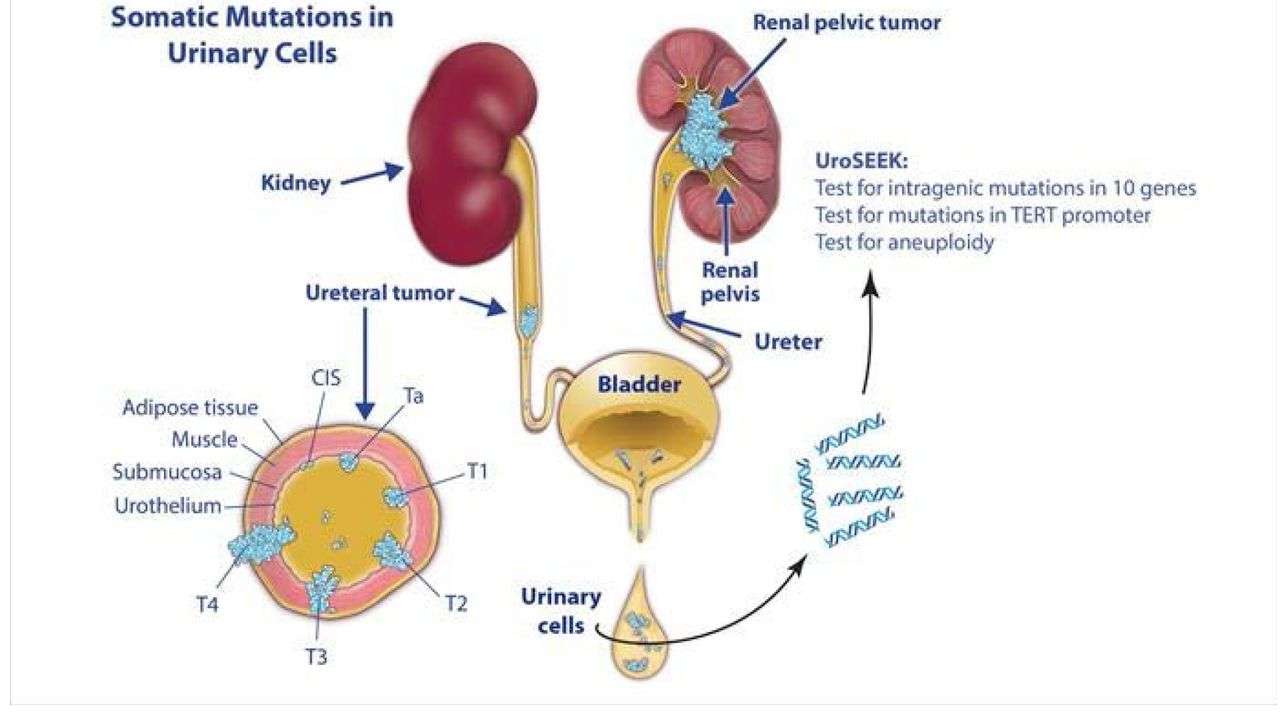
Although there is minimal controversy regarding the role of laparoscopic nephroureterectomy, the management of the distal ureter and bladder cuff with laparoscopy varies among many surgeons. Techniques include 1) open excision, 2) transvesical laparoscopic detachment and ligation technique, 3) laparoscopic stapling of the distal ureter and bladder cuff, and 4) the pluck technique. These techniques were recently reviewed by Steinberg and Matin.
Also Check: Basaloid Tumor
Upper Tract Urothelial Carcinoma
Urothelial cancer refers to a cancer of the lining of the urinary system. While the majority of urothelial cancers arise in the bladder, upper tract urothelial cancers arise in the lining of the kidney or the ureter .
In addition to the signs of bladder cancer, individuals with UTUC may also experience pain in the upper abdomen or mid-back in the region of the kidney. UTUCs can block the ureter or kidney, causing blockage of the kidney , and they can even affect kidney function in some patients.
Like bladder cancers, UTUCs can develop as low- or high-grade tumours.
In general, low-grade tumors are not invasive and very rarely spread from the kidney or ureter to other sites. However, they often recur in the kidney, ureter and bladder. Management involves biopsy and ablation of the tumour through a camera that is passed into the ureter through the bladder. It is important to try to preserve the kidney, but the kidney does have to be removed if the tumour is too extensive.
High-grade UTUC has the potential to spread from the kidney or ureter to lymph nodes, lung and bone. It is most often treated with surgical removal of the kidney and ureter an operation called radical nephrouretectomy.
GET IN TOUCH
Diagnosis Of Upper Tract Urothelial Carcinoma
Often times a CT scan, usually a CT urogram is done. Somtimes depending on the kidney function, a MR urogram, which is MRI test, can be used instead. Somtimes the urologist has to diagnose UTUC by looking into the ureter and kidney.
Retrograde pyelogram is where a urologist takes the patient to the operating roomand uses a tiny camera passed up the urethra into the bladder and up into the ureter. Then some contrast dye is injected into the ureter, which then fills up the collecting system and can demonstrate a tumor.
A simple urine sample called a urine cytology is often helpful. The pathologist looks under the microscope and tells us that these are cancerous cells that are coming from the urinary system.
Its not a very sensitive test but it is a specific test. So see if a tumor is there then we have to use a camera and a very small scope to go and look at the ureter and the renal pelvis and try to get a biopsy.
You May Like: How Fast Does Cancer Kill
Localized Transitional Cell Cancer Of The Renal Pelvis And Ureter
Standard treatment options:
Treatment options under clinical evaluation:
The development of new instrumentation for endourological treatment of uppertract transitional cell cancer has provided new options for regional managementof these cancers. Introduction of electrofulguration and resection instrumentsor laser probes either transureterally or percutaneously may permit destructionof a primary cancer. Introduction of cytotoxic agents has also been employed. Although a biopsy can be taken for staging purposes, the accuracy of thisremains to be determined. The efficacy of treatment by these maneuvers has notbeen established.
Causes Of Upper Tract Urothelial Cancer
The cause of UTUC is not known in most cases. However, there are several risk factors:
-
smoking tobacco
-
a history of long-term inflammation of the ureter or kidney
-
exposure to certain chemicals over time, such as those used to make plastics, textiles, rubber, paint and dyes
-
exposure to arsenic
-
prior chemotherapy or radiation therapy for another cancer
-
long-term use of large quantities of painkillers
-
family history of bladder cancer
-
having Lynch syndrome or Balkan nephropathy .
Also Check: Non Invasive Breast Cancer Survival Rate
Stage Information For Transitional Cell Cancer Of The Renal Pelvis And Ureter
Though comparable in many respects to staging systems described for bladdercancer, unique structural aspects of the renal pelvis and ureter have led toseveral differences in the classification schema of tumors that involve theupper tracts. Clinical staging is based on a combination of radiographicprocedures and,more recently, ureteroscopy and biopsy.
The advent of rigid and flexible ureteroscopic techniques has permittedendoscopic access to the ureter and renal pelvis. This may permit greateraccuracy in preoperative definition of the stage and grade of an upper tractneoplasm. In addition, fulguration and endourological access permit resectionor laser coagulation of highly selected low-stage, low-grade lesions of theureters. However, this approach is still under clinical evaluation becausethere is the possibility of inaccurate assessment of the stage and extent ofdisease, and the adequacy and risks of such treatment have not yet beendefined.
Because of the inaccessibility of ureteral and pelvic anatomy, accurate stagingrequires pathologic analysis of the surgically excised specimen.
Distribution Of Upper Tract Urothelial Cell Carcinoma
Rates of distribution for UTUC are as follows:
- Renal pelvis: 58%
- Ureter: 35%
- Both renal pelvis and ureter: 7%
- Bilateral: 2-5%
Clinical manifestations of uurothelial tumors of the renal pelvis and ureters include the following:
- Gross or microscopic hematuria – 75% of patients the most common clinical finding
- Flank pain – 20% of patients results from gradual obstruction/distention of the collecting system or, in cases of acute colic, from obstruction by a blood clot
- Dysuria or irritative voiding symptoms – 6% of patients
- Weight loss, anorexia, flank mass, or bone pain – manifestations of advanced disease that manifest in a minority of patients
Recommended Reading: Melanoma 3b
Analysis Of Risk Factors Of Postoperative Bc Recurrence
Among the 439 patients, 89 had BC recurrence, and their data were analyzed using the binary logistic regression model. We found that advanced tumor stage, presence of a high-grade tumor, preoperative ureteroscopy, DM without metformin use, and UUC were risk factors of postoperative BC recurrence. Patients with 1 or more than 1 of the risk factors were more likely to experience BC recurrence. Furthermore, regular postoperative bladder perfusion chemotherapy was a protective factor for recurrent BC. The results of the analysis of high risk factors for postoperative BC recurrence are shown in Table .
New Diagnostic Tools For Utuc
Nomogram
A nomogram including tumour grade, architecture and location of the tumour achieved 76.6% accuracy in predicting nonorgan-confined UTUC and can be used for designing clinical trials, selecting patients for preoperative systemic therapy and guiding the extent of concomitant lymph node dissection at RNU .
Fluorescence in situ hybridization
Read Also: Tumor Calcification
Effects Of Cox Regression Analysis On The Prognosis Of Utucs
Cox regression analysis was performed to eliminate confounding factors. Eight factors, namely smoking, consumption of Chinese medicine containing aristolochic acid, history of BC, age, tumor stage, tumor grade, tumor size, and LNM, had a significant effect on survival and were identified as prognostic factors . This suggested that smoking, taking Chinese medicine containing aristolochic acid, history of BC, older age, advanced tumor stage, high-grade tumors, larger tumors, and presence of LNM were risk factors of UTUC patients with poor prognosis. Sex, number of tumors, tumor location, DM, and mode of operation had no effect on the prognosis . The results of the analysis of factors influencing survival time and prognosis are shown in Table .
Diagnosis Of Upper Tract Urothelial Cancer
If your doctor thinks you may have UTUC they will take your medical history, perform a physical examination and arrange for you to have a number of tests.
If the results of these tests suggest that you may have UTUC, your doctor will refer you to a specialist called a urologist, who will arrange further tests. These may include:
Also Check: Is A Sore That Doesn T Heal Always Cancer
Role Of Segmental Ureterectomy And Others Rather Than Endoscopic Organ
Jeldres and colleagues showed by analysing SEER data that segmental ureterectomy compared with RNU showed 5-year CSM-free rates for segmental ureterectomy versus nephroureterectomy with bladder cuff removal of 86.6% versus 82.2%, respectively . Thus, segmental resection does not appear to undermine cancer control compared with RNU. However, it is imperative that the results of population-based data analysis be interpreted with caution.
Steffens and colleagues reported in four out of 978 patients a partial nephrectomy and autotransplantation with pyelovesicostomy in solitary kidneys. All patients received mitomycin or bacille CalmetteGuérin instillation therapy after surgery. There were no recurrences or deaths and kidney function was stable .
Guidelines on UTUC stated the following indications for endoscopic treatment:
unifocal tumour
low-grade tumours
no evidence of an infiltrative lesion on computed tomography
understanding the close follow up.
Ethics Approval And Consent To Participate
This research adopted the retrospective analysis based on the principle of safety and fairness. The diagnosis and treatment conducted had no harm on the health of the subjects, and there was no risk for the subjects. All subjects signed the informed consent and their personal information would not be disclosed. Moreover, the research was beneficial and instructive for clinical practice. Based on the discussion of the medical scientific ethical committee of the First affiliated hospital of Zhengzhou University, this study was approved.
Also Check: Infiltrating Ductal Carcinoma Survival Rate
Outcomes After Endoscopic Organ
RNU is the standard treatment for UTUC. Alternative management is considered, because preserving the renal function and/or reducing morbidity of the treatment while having excellent oncological results is attractive. Alternative treatment can be sufficient in selected patients, especially in those with small, low-grade UTUC.
Ishikawa and colleagues underlined that diagnostic ureteroscopy was no risk factor for intravesical recurrence and survival in UTUC patients . Diagnostic ureteroscopy with cytology and biopsies to determine tumour grade as a surrogate marker for the aggressiveness of the underlying tumour should be performed in the case of endoscopic treatment . Large size, broad base and nonpapillary pattern favour tumour invasiveness. If necessary, biopsies can be done with flexible instruments or percutaneously. In a Dutch study, an increasing time trend was found for endoscopic treatment .
With experience, good results can be also achieved with flexible ureteroscopy only. Cornu and colleagues after a median follow up of 30 months reported a recurrence in 21 out of 35 patients . The median survival rate without recurrence was 10 months . Four patients underwent nephroureterectomy during follow up and none of the patients died of disease progression .
There Are Two Kinds Of Upper Tract Urothelial Carcinoma:
- Non-invasive: more than half the people have this type, where the cancer remains in the urothelial cells that line the renal pelvis or ureters.
- Invasive: the rest have this type, where the cancer has grown beyond those urothelial cells. Or it may have spread to other parts of the body.
The grade of the tumor is determined by a pathologist who examines the cells under a microscope. Low grade UTUC is usually not very aggressive and is slow to spread. High grade UTUC can be more aggressive. It may spread to other parts of your urinary tract, or to other parts of your body. The grade of your UTUC is important to know as you and your doctor choose the best treatment for your cancer. Doctors may also use imaging studies to help them stage UTUC. Ask your doctor to explain the details about your diagnosis and pathology report.
This information and assessing your overall health, will help your doctor recommend the best treatment options for your cancer. Depending on the stage, grade and location of your tumor, UTUC can be treated with medications or surgery.
Also Check: Invasive Lobular Carcinoma Grade 2 Survival Rates
Identification Of Prognostic Factors
Prognostic factors are patient characteristics which predict the disease outcome including the chance of recovery or recurrence. Prognostic factors are significant and important in clinical practice as they can guide selection of treatment and the timing of surveillance. Identification of prognostic factors determining which patients can benefit from endoscopic versus radical nephroureterectomy, neoadjuvant or adjuvant chemotherapy and/or lymphadenectomy is urgently needed.
Clinical Nomograms And Predictive Tools
![[Full text] Emerging biomarkers for the diagnosis and ...](https://img.healthyskinworld.com/wp-content/uploads/full-text-emerging-biomarkers-for-the-diagnosis-and.jpeg)
There have been numerous pre-operative and post-operative prognostic markers that have been shown to be associated with survival in UTUC. These are mostly based upon retrospective cohort studies. There have been efforts to use these collectively as predictive tools to aid in clinical management.
Preoperatively, there are 2 models that have been developed. The first nomogram is aimed to predict lymph node involvement in locally advanced UTUC, in order to guide clinicians on whether to perform a lymph node dissection or not. Three variables, namely tumor grade, architecture, and location of tumor were found to be independently associated with non-organ-confined disease. Together these 3 variables achieved 76.6% accuracy in prediction of non-organ confined UTUC. The second model combines imaging and ureteroscopy variables to help select non-organ-confined UTUC which is likely to benefit from RNU. Lastly, a multi-center database was used to develop a preoperative nomogram to help predict disease recurrence to better select patients who can most benefit from RNU.
There exist 5 different postoperative nomograms. They can help to predict survival rates based on standard pathological features, which can be helpful for postoperative follow-up and counseling. Another prognostic nomogram based on 2926 patients which are based on 4 variables has good prognostic accuracy and risk stratification for patients with high-grade UTUC.
Read Also: In Situ Cancer Melanoma
Imaging Upper Tract Urothelial Carcinoma
Diagnostic imaging plays a significant role in diagnosing and staging of UTUC. Previously, multiple imaging investigations were common with ultrasound, excretory urography and retrograde pyelography. Currently, CT urography is the most common imaging technique for imaging UTUC and MR urography is used only when CT urography is contraindicated. Clinical presentation of UTUC is usually with haematuria and so the imaging techniques used must not only be highly accurate for diagnosing UTUC but also be able detect other diseases responsible for haematuria.
Impact Of Radical Nephroureterectomy On Kidney Function
Recent data showed an association between chronic kidney disease and cardiovascular morbidity and mortality after radical treatment of cortical renal tumours leaving a single renal unit . This can be translated also in the radical treatment of UTUC. Kaag and colleagues showed that the estimated glomerular filtration rate is significantly diminished after RNU particularly in the elderly. Preoperatively only about 50% and postoperatively only about 20% of all patients who underwent RNU had eGFR 60ml/min per 1.73cm2 , respectively .
Similar results in a different context were found in another study: median age was 72 years and median preoperative eGFR was 59ml/min/1.73m2. Before nephroureterectomy, only 48% of patients were eligible to receive CBC and this decreased to 22% postoperatively . In the 144 patients with pT2pT4 and/or pN1pN3 disease who are suitable to receive CBC, these proportions were 40% and 24%, respectively .
Also Check: Cell Cancer Symptoms