How Can You Manage Stage 3 Melanoma
Managing stage 3 melanoma can be challenging. With technological and medical advances, this diagnosis may not be as severe as it once was.
After your surgery or if youre unable to undergo surgery, you may need adjuvant treatment to prevent the cancer from coming back. There is adjuvant radiation therapy and adjuvant immunotherapy. These therapies help reduce the risk of melanoma returning, but they dont increase your survival rate.
Certain Factors Affect Prognosis And Treatment Options
The prognosis and treatment options depend on the following:
- The thickness of the tumor and where it is in the body.
- How quickly the cancer cells are dividing.
- Whether there was bleeding or ulceration of the tumor.
- How much cancer is in the lymph nodes.
- The number of places cancer has spread to in the body.
- The level of lactate dehydrogenase in the blood.
- Whether the cancer has certain mutations in a gene called BRAF.
- The patients age and general health.
Treating Stage Iv Melanoma
Stage IV melanomas have already spread to distant lymph nodes or other areas of the body. Skin tumors or enlarged lymph nodes causing symptoms can often be removed by surgery or treated with radiation therapy.
Metastases in internal organs are sometimes removed, depending on how many there are, where they are, and how likely they are to cause symptoms. Metastases that cause symptoms but cannot be removed may be treated with radiation, immunotherapy, targeted therapy, or chemotherapy.
The treatment of widespread melanomas has changed in recent years as newer forms of immunotherapy and targeted drugs have been shown to be more effective than chemotherapy.
Immunotherapy drugs called checkpoint inhibitors such as pembrolizumab or nivolumab are typically the first drugs tried, especially in people whose cancer cells do not have BRAF gene changes. These drugs can shrink tumors for long periods of time in some people. Ipilimumab , a different type of checkpoint inhibitor, is not typically used by itself as the first treatment, although it might be combined with nivolumab or pembrolizumab. This slightly increase the chances that the tumor will shrink, although itâs also more likely to result in serious side effects, which needs to be considered carefully. People who get any of these drugs need to be watched closely for serious side effects..
Itâs important to carefully consider the possible benefits and side effects of any recommended treatment before starting it.
Read Also: Squamous Cell Carcinoma Skin Metastasis
What Is Stage Iii Melanoma
Stage III melanomas are tumors that have spread to regional lymph nodes or have developed in-transit deposits of disease, but there is no evidence of distant metastasis. Stage III melanoma is regional melanoma, meaning it has spread beyond the primary tumor to the closest lymph nodes, but not to distant sites. There are four subgroups of Stage III melanoma: IIIA, IIIB, IIIC, IIID. Stage III is invasive melanoma.
- Subgroups are IIIA, IIIB, IIIC, IIID
- Stage III melanoma is defined by four primary characteristics
- Important distinction within Stage III: whether the spread to lymph nodes can be detected microscopically or macroscopically
- Microscopically, also called clinically occult = seen by pathologist during biopsy or dissection
- Macroscopically, also called clinically detected = seen by naked eye or felt by hand or seen on CT scans or ultrasound
- Risk: Intermediate to high for regional or distant spread
Targeted Therapies Currently Available
Currently, there are three targeted therapy regimens that are approved for use in Australia in patients with a BRAF mutation. These regimens combine a drug that targets the BRAF gene mutation with a drug that blocks the MEK gene .
The combination of a BRAF inhibitor and a MEK inhibitor has been found to be more effective for shrinking melanoma tumours than using either type of drug on its own.
The combinations are:
- a BRAF inhibitor called dabrafenib and a MEK inhibitor called trametinib
- a BRAF inhibitor called vemurafenib and a MEK inhibitor called cobimetinib
- a BRAF inhibitor called encorafenib and a MEK inhibitor called binimetinib.
There are currently no therapies approved specifically to treat NRAS-mutant or cKIT-mutant melanomas, although some are being tested in clinical trials.
Don’t Miss: Metastatic Basal Cell Carcinoma Survival Rate
Biological Therapies And Melanoma
Biological therapies are treatments using substances made naturally by the body. Some of these treatments are called immunotherapy because they help the immune system fight the cancer, or they occur naturally as part of the immune system. There are many biological therapies being researched and trialled, which in the future may help treat people with melanoma. They include monoclonal antibodies and vaccine therapy.
There Are Three Ways That Cancer Spreads In The Body
Cancer can spread through tissue, the lymph system, and the blood:
- Tissue. The cancer spreads from where it began by growing into nearby areas.
- Lymph system. The cancer spreads from where it began by getting into the lymph system. The cancer travels through the lymph vessels to other parts of the body.
- Blood. The cancer spreads from where it began by getting into the blood. The cancer travels through the blood vessels to other parts of the body.
Read Also: Does Amelanotic Melanoma Blanch When Pressed
How Dangerous Is Melanoma
Melanoma is usually curable when detected and treated early. Once melanoma has spread deeper into the skin or other parts of the body, it becomes more difficult to treat and can be deadly.
- The estimated five-year survival rate for U.S. patients whose melanoma is detected early is about 99 percent.
- An estimated 7,180 people will die of melanoma in the U.S. in 2021.
What Is Melanoma Of The Head And Neck
Melanoma is a cancer that arises from melanocytes, the cells that give skin its pigment or color. Melanoma most commonly occurs in skin cells, but can rarely also occur in mucous membranes of the respiratory, gastrointestinal, genital or urinary organs. Melanoma arising in skin cells is caused by ultraviolet radiation from exposure to the sun and tanning beds.
Melanoma is the least common form of skin cancer, but it is responsible for more deaths per year than all other skin cancers combined. Melanoma is also more likely than other skin cancers to spread, and may be harder to control. However, approximately 75% of melanomas are found before they have spread, and can be cured with treatment. Mucosal melanomas make up 1% of all melanomas, and are more likely to spread to other sites
Read Also: Does Skin Cancer Make You Lose Hair
The Following Stages Are Used For Melanoma:
Stage 0
Stage I
- Stage IA: The tumor is not more than 1millimeter thick, with or without ulceration.
- Stage IB: The tumor is more than 1 but not more than 2 millimeters thick, without ulceration. Enlarge Stage I melanoma. In stage IA, the tumor is not more than 1 millimeter thick, with or without ulceration . In stage IB, the tumor is more than 1 but not more than 2 millimeters thick, without ulceration. Skin thickness is different on different parts of the body.
Stage II
- Stage IIA: The tumor is either:
- more than 1 but not more than 2 millimeters thick, with ulceration or
- more than 2 but not more than 4 millimeters thick, without ulceration. Enlarge Stage IIA melanoma. The tumor is more than 1 but not more than 2 millimeters thick, with ulceration OR it is more than 2 but not more than 4 millimeters thick, without ulceration. Skin thickness is different on different parts of the body.
Stage III
Stage III is divided into stages IIIA, IIIB, IIIC, and IIID.
Treatments For Advanced Melanoma
In most cases, treatment can’t cure advanced melanoma. But some can help you live longer and feel better. The goal of any therapy you get will be to shrink or remove your tumor, keep the cancer from spreading further, and ease your symptoms.
Surgery. This is the main way to remove melanoma from the skin and lymph nodes. You might also have an operation on organs where the cancer has spread. Thereâs no guarantee your surgeon will get all of it. Some melanoma is too small to see, even with high-tech scans.
Radiation. Your doctor might recommend radiation to kill any cancer cells that have been left behind after surgery or if melanoma spreads to your brain or bones. It can also relieve pain from the disease or treat melanoma that comes back over and over.
Immunotherapy or biologic therapy. These drugs help your immune system find and attack cancer cells. Depending on the ones you take, you might have to go in for treatment every 2, 3, or 4 weeks.
Your doctor might want you to take more than one drug. Some studies show that people who do have fewer side effects.
The flip side of immunotherapy is that sometimes these drugs cause your immune system to attack healthy organs. Then youâd need to stop melanoma treatment and take drugs to stop the attack.
Chemo can shrink the cancer, but chances are it will start growing again after a few months and youâll need more treatment. Immunotherapy and targeted therapy usually work better.
Other side effects include:
Also Check: Soderstrom Skin Cancer Screening
What Is The Outlook For Patients With Melanoma Affecting The Nail Unit
The main factor associated with the risk of spread of melanoma and death is the thickness of the melanoma at the time of complete excision of the primary tumour. Delay in diagnosis is common with subungual melanoma, particularly when it affects the toe, and some of these tumours have already spread at the time of diagnosis.
The 5-year survival rate ranges widely from 16% to 87%, depending on the series, with two larger series in the 51% to 55% range .
When Should I Call My Doctor
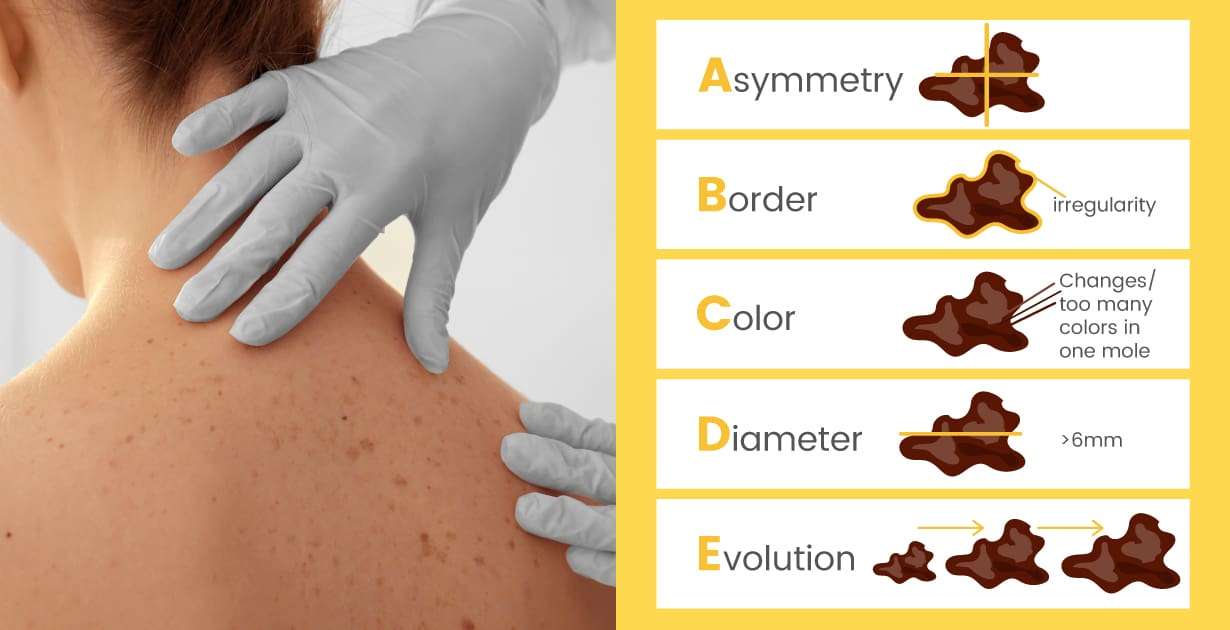
You should have a skin examination by a doctor if you have any of the following:
- A personal history of skin cancer or atypical moles .
- A family history of skin cancer.
- A history of intense sun exposure as a young person and painful or blistering sunburns.
- New or numerous large moles.
- A mole that changes in size, color or shape.
- Any mole that itches, bleeds or is tender.
A note from Cleveland Clinic
Receiving a diagnosis of melanoma can be scary. Watch your skin and moles for any changes and seeing your doctor regularly for skin examinations, especially if youre fair-skinned, will give you the best chances for catching melanoma early when its most treatable.
Last reviewed by a Cleveland Clinic medical professional on 06/21/2021.
References
Read Also: Amelanotic Melanoma Blanch
Abcdef Guidelines For Pigmented Nail Lesions
Levit et al described ABCDEF guidelines to assess pigmented nail lesions .
- A: Age 4070 years of age African, Japanese, Chinese, and Native American heritage
- B: Brown-black band 3mm with variegated borders
- C: Change or lack of change in the nail band or nail morphology
- D: Digit most commonly involved
- E: Extension of discolouration into the skin surrounding the nail
- F: Family or personal history of melanoma
Risk Of Further Melanomas
Most people treated for early melanoma do not have further trouble with the disease. However, when there is a chance that the melanoma may have spread to other parts of your body, you will need regular check-ups. Your doctor will decide how often you will need check-ups everyone is different. They will become less frequent if you have no further problems. After treatment for melanoma it is important to limit exposure to the sun’s UV radiation. As biological family members usually share similar traits, your family members may also have an increased risk of developing melanoma and other skin cancers. They can reduce their risk by spending less time in the sun and using a combination of sun protection measures during sun protection times. It is important to monitor your skin regularly and if you notice any changes in your skin, or enlarged lymph glands near to where you had the cancer, see your specialist as soon as possible.
Don’t Miss: Etiology Of Basal Cell Carcinoma
Getting Regular Checkups Vital
The main key to combating a melanoma recurrence is early detection.
After your treatment, its vital to continue to see your dermatologist or physician regularly. Your doctor will base the need for follow-up on your specific case. As time goes by without a relapse, the frequency of visits will gradually decline.
For patients who had melanoma before, we generally recommend seeing your physician every three to six months, Dr. Tarhini says. The higher the stage of melanoma you had, the higher your risk is for relapse.
He recommends seeing your physician every three months for a year. Then, every four to six months for the next year. After that, every six months up to five years.
If there is no evidence of another melanoma or disease relapse at that point, continue your follow-up once a year, he says.
Who Treats Melanoma Skin Cancer
Depending on your options, you may have different types of doctors on your treatment team. These doctors may include:
- A dermatologist: a doctor who treats diseases of the skin
- A surgical oncologist : a doctor who uses surgery to treat cancer
- A medical oncologist: a doctor who treats cancer with medicines such as chemotherapy, immunotherapy, or targeted therapy
- A radiation oncologist: a doctor who treats cancer with radiation therapy
Many other specialists may be involved in your care as well, including physician assistants , nurse practitioners , nurses, psychologists, social workers, rehabilitation specialists, and other health professionals.
Also Check: Basal Skin Cancer Survival Rates
How Immunotherapy Comes Into Play
Immunotherapy helps your natural immune system to attack cancer cells.
One group of immunotherapy drugs in particular has shown great promise for treating advanced-stage melanoma. These drugs are known as checkpoint inhibitors. They help the immune systems T cells recognize and attack melanoma cells.
Studies have found these medications improve survival rates for people with advanced-stage melanoma, report the authors of a review article in the American Journal of Clinical Dermatology. Research published in The Oncologist has also found that people with melanoma can potentially benefit from treatment with these drugs, regardless of their age.
But immunotherapy doesnt work for everyone. According to a research letter published in the journal Nature Medicine, only a portion of people with melanoma benefit from treatment with checkpoint inhibitors. More research is needed to learn which people are most likely to respond well to this treatment.
Adjuvant Treatment May Represent The Best Opportunity To Cure Patients After Surgery And To Prevent Morbidity From Progression
Following surgery for melanoma with a high risk of relapse and death , melanoma patients currently have two treatment options approved by the US Food and Drug Administration: high-dose IFN- and pegylated IFN . The patterns of relapse in this population show that 51% of the relapses occur at distant sites , so treatment to delay relapse can be a significant benefit to patients, even if the therapy does not increase long-term overall survival . Curing patients in this population at high risk for relapse and death ideally would require the pretreatment ability to identify which patients are destined for relapse and, among those at highest risk, who will benefit from a particular adjuvant intervention which may relate to patient, tumor and therapy.
To answer the first question, years of work have been devoted to evaluating clinical and pathologic risk factors related to the primary melanoma, and the presence or absence of tumor in draining lymph nodes, which is the single most important determinant of survival. The current American Joint Committee on Cancer staging system recognizes the importance of ulceration of the primary tumor, mitotic rate, and the number and size of tumor bearing lymph nodes . Further refinement of this system is needed, because even with a full knowledge of all of these factors, many patients defined as high risk by AJCC criteria are likely cured by surgery and may be receiving adjuvant therapy for no benefit.
Recommended Reading: Does Skin Cancer Burn And Itch
What Are The Chances Of Recurrence
The chances of your melanoma coming back depend on its stage.
Those who have had melanoma are at greater risk for developing another melanoma. It can return in the same spot or elsewhere on your body, even 10 years after initial treatment.
Some cancer cells may remain inside your body that screening tests cant detect. If these cells grow into a tumor, its known as a recurrence.
Doctors classify melanoma in one of four stages:
- In Stages 1 and 2, it involves the skin only.
- In Stage 3, it has spread from the skin to the lymph nodes.
- In Stage 4, it has spread from the skin to other organs.
The likelihood of recurrence varies by stage. It is less likely to recur at lower stages, Dr. Tarhini says.
The recurrence rate increases as the stage advances even after successful surgery, he says.
The stage also affects your prognosis. The lower the stage, the higher the likelihood is of curing your melanoma.
At Stage 1, over 90 percent of patients can be cured, says Dr. Tarhini. As the stage progresses, the likelihood of cure is less. However, with recent advancements in immunotherapy and targeted therapy for melanoma, even at Stage 4 , we are very optimistic that we can cure many patients.