Standard Treatment Options For Stage I Bladder Cancer
Patients with stage I bladder tumors are unlikely to die from bladder cancer, but the tendency for new tumor formation is high. In a series of patients with Ta or T1 tumors who were followed for a minimum of 20 years or until death, the risk of bladder recurrence after initial resection was 80%. Of greater concern than recurrence is the risk of progression to muscle-invasive, locally-advanced, or metastatic bladder cancer. While progression is rare for low-grade tumors, it is common among high-grade cancers.
One series of 125 patients with TaG3 cancers followed for 15 to 20 years reported that 39% progressed to more advanced stage disease, while 26% died of urothelial cancer. In comparison, among 23 patients with TaG1 tumors, none died and 5% progressed. Risk factors for recurrence and progression include the following:
- High-grade disease.
TUR with fulguration followed by an immediate postoperative instillation of intravesical chemotherapy
TUR and fulguration are the most common and conservative forms of management. Careful surveillance of subsequent bladder tumor progression is important. Because most bladder cancers recur after TUR, one immediate intravesical instillation of chemotherapy after TUR is widely used. Numerous randomized, controlled trials have evaluated this practice, and a meta-analysis of seven trials reported that a single intravesical treatment with chemotherapy reduced the odds of recurrence by 39% .
TUR with fulguration
Evidence :
Relevance Of The International Bcg Shortage To The Aua Guidelines
The global shortages in TICE BCG that occurred in 2014 and 2019 led the AUA to recommend several management strategies to maintain high quality care for patients with NMIBC. These recommendations may supersede the guideline statements below. In particular, the BCG shortage impacts guideline statements 17, 20, and 21. The AUA Statement on the BCG Shortage is available at .
Carcinogenesis And Risk Factors
Increasing age is the most important risk factor for most cancers. Other risk factors for bladder cancer include the following:
- Use of tobacco, especially cigarettes.
- Family history of bladder cancer.
- HRAS mutation .
- Rb1 mutation.
There is strong evidence linking exposure to carcinogens to bladder cancer. The most common risk factor for bladder cancer in the United States is cigarette smoking. It is estimated that up to half of all bladder cancers are caused by cigarette smoking and that smoking increases a persons risk of bladder cancer two to four times above baseline risk. Smokers with less functional polymorphisms of N-acetyltransferase-2 have a higher risk of bladder cancer than other smokers, presumably because of their reduced ability to detoxify carcinogens.
You May Like: Does Melanoma Blanch When Pressed
Morphologic Variants Of Urothelial Carcinoma
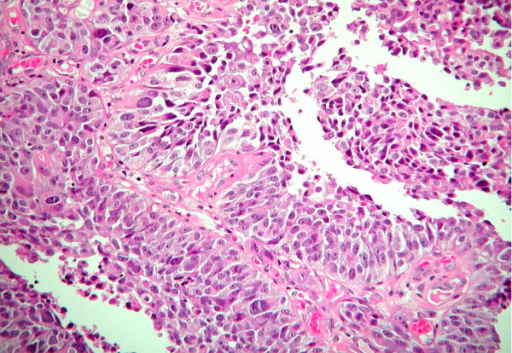
Some cases of urothelial carcinoma show morphologic patterns that are recognized as variants morphology. Those include nested variant, micropapillary, lymphoepithelioma-like, sarcomatoid, small cell carcinoma, and adenocarcinoma. These are frequently under-recognized in bladder biopsies and could have therapeutic implications with different criteria for surgery and different chemotherapy regimens.
Genetic Factors In Pathogenesis
Divergent, yet interconnected and overlapping, molecular pathways are likely responsible for the development of noninvasive and invasive bladder tumors. Somatic mutations in fibroblast growth receptor3 and tumor protein p53 in tumor cells appear to be important early molecular events in the noninvasive and invasive pathways, respectively.
FGFR-3, Ras, and PIK3CA mutations occur with high frequency in noninvasive tumors, leading to upregulation of Akt and mitogen-activated protein kinase . Loss of heterozygosity on chromosome 9 is among the most frequent genetic alterations in bladder tumors and is considered an early event.
Large numbers of genomic changes have been detected using karyotyping and comparative genomic hybridization analysis in urothelial carcinoma. Numerically common are losses of 2q, 5q, 8p, 9p, 10q, 18q, and Y. Gains of 1q, 5p, 8q, and 17q are frequently present, and high-level amplifications can be found however, the target genes in the regions of amplifications have not been conclusively identified.
Alterations in the TP53 gene are noted in approximately 60% of invasive bladder cancers. Progression-free survival is significantly shorter in patients with TP53 mutations and is an independent predictor of death among patients with muscle-invasive bladder cancer.
Read Also: What Is Squamous Cell Carcinoma Of The Head And Neck
What Is An Urothelial Neoplasm
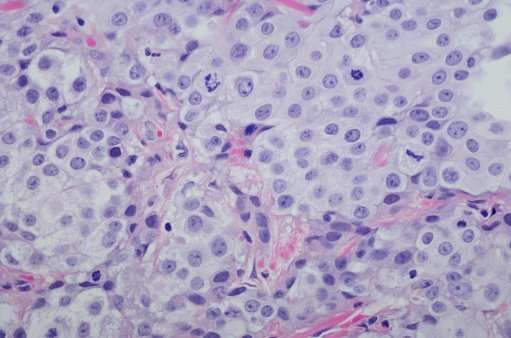
Urothelial neoplasia is a unique cancer in that is consists of a spectrum of tumors with different biologic behaviors. The most common urothelial neoplasm is the low grade superficial papillary carcinoma or papilloma which may recur numerous times but does not result in significant morbidity or mortality.
Treatment Management And Survivorship
Total excision of the ureterwith a bladder cuff, renal pelvis, and kidney is recommended in an attempt toprovide the greatest likelihood of cure.
References
Also Check: Is Stage 3 Melanoma Curable
Standard Treatment Options For Stage Iv Bladder Cancer
Standard treatment options for patients with T4b, N0, M0 disease
Treatment options for patients with T4b, N0, M0 disease include the following:
Chemotherapy alone or as an adjunct to local treatment
Cisplatin-based combination chemotherapy regimens are the standard of care for first-line therapy for stage IV bladder cancer in patients who can tolerate it. The only chemotherapy regimens that have been shown to result in longer survival in randomized controlled trials are MVAC, dose-dense MVAC, and CMV. GC was compared with MVAC in a randomized controlled trial and neither regimen was associated with a statistically significant difference in response rate or survival. The two regimens are generally considered equivalent, but they have never been compared in a noninferiority trial. Of note, patients with good performance status and lymph node-only disease have a low but significant rate of achieving a durable complete remission with MVAC or GC. In the large, randomized, controlled trial comparing MVAC with GC, for example, 5-year OS in patients with lymph node-only disease was 20.9%. Dose-dense MVAC and standard-dose MVAC were compared in a randomized controlled trial, and dose-dense MVAC was associated with longer survival.
Ongoing studies are evaluating new chemotherapy combinations.
Evidence :
Ongoing studies are evaluating new chemotherapy combinations.
Immunotherapy
Donât Miss: Can You Die From Basal Cell Skin Cancer
Treatment Strategy For Newly Diagnosed T1 High
- Zachary KlaassenAffiliationsDivision of Urology, Department of Surgery, University Health Network, Princess Margaret Cancer Centre, University of Toronto, Toronto, ON, Canada
- Bas W.G. van RhijnAffiliationsDepartment of Surgical Oncology, Division of Urology, Netherlands Cancer Institute Antoni van Leeuwenhoek Hospital, Amsterdam, The Netherlands
- These authors share co-senior authorship.James W.F. Catto These authors share co-senior authorship.Affiliations
- These authors share co-senior authorship.Girish S. KulkarniCorrespondenceCorresponding author. Division of Urology, Department of Surgery, Institute for Clinical Evaluative Sciences, University Health Network, Princess Margaret Hospital, 610 University Avenue, Suite 3-130, Toronto, ON M5G 2M9, Canada. Tel. +1 416 946 2246. These authors share co-senior authorship.AffiliationsDivision of Urology, Department of Surgery, University Health Network, Princess Margaret Cancer Centre, University of Toronto, Toronto, ON, Canada
- These authors share co-senior authorship.
Also Check: Melanoma 3b
Localized Transitional Cell Cancer Of The Renal Pelvis And Ureter
Standard treatment options:
Treatment options under clinical evaluation:
The development of new instrumentation for endourological treatment of uppertract transitional cell cancer has provided new options for regional managementof these cancers. Introduction of electrofulguration and resection instrumentsor laser probes either transureterally or percutaneously may permit destructionof a primary cancer. Introduction of cytotoxic agents has also been employed. Although a biopsy can be taken for staging purposes, the accuracy of thisremains to be determined. The efficacy of treatment by these maneuvers has notbeen established.
Irocker Blackfin Paddle Board Xl
Functionality, swiftness, and stableness make this set of our most preferred boards. If you like paddling at speed, with add-ons to entertain, then this board is created you.
For taller riders over 5 8 the Blackfin XL iSUP maneuvers completely through any type of water environment and is great for natural buffs who intend to fish as well as bring camping gear along for the tripexpedition}.
It has an array of attributes, transforming to a dual kayak and integrated fishing installs. Adventure applicants and adventure enthusiasts, its time to enhance the means you paddle.
Donât Miss: How Do You Know If Squamous Cell Carcinoma Has Spread
You May Like: Invasive Ductal Carcinoma Grade 1 Survival Rate
Treatment For Hg Pt1 Bladder Cancer With Pt2 Or More Histology At Second Tur
There is no doubt about the need to perform radical cystectomy for patients with muscle-invasive disease at the second TUR. Most of these tumors are understaged at the initial TURBT due to technical problems, and may not be large or bulky like muscle-invasive tumors that are diagnosed at the initial TURBT and/or with computed tomography or magnetic resonance imaging. The discussion on the treatment strategies for these tumors does not include whether cystectomy should be performed but whether neoadjuvant chemotherapy and/or extended lymph node dissection should be performed.
Several randomized Phase III trials and meta-analyses demonstrated the survival benefit of cisplatin-based neoadjuvant chemotherapy for patients with MIBC. However, whether neoadjuvant chemotherapy prolongs the survival of patients with T1 cancer at the initial TURBT and with muscle-invasive disease detected by a second TUR is unclear. Neoadjuvant chemotherapy offers potential advantages in tumor downstaging and eradication of micrometastases, so this therapy should be indicated for patients who have risk factors for locally advanced disease or nodal metastasis.
Other Squamous Cell Carcinoma Risk Factors
Having bladder diverticula may increase an individuals chance of developing SCC. Rarely, bacillus Calmette-Guerin treatment for CIS has been reported to lead to development of SCC. Development of bladder cancer at a younger age has been associated with bladder exstrophy. SCC has also been described in urachal remnants.
Coffee consumption does not increase the risk of developing bladder cancer. Early studies of rodents and a minority of human studies suggested a weak connection between artificial sweeteners and bladder cancer however, most recent studies show no significant correlation.
Don’t Miss: Stage 3 Melanoma Survival Rate
Grading Of A Bladder Cancer
Grading of a bladder cancer is assessing how aggressive it is in terms of howabnormal its cells look under a microscope. Those that are very abnormal growmore quickly. Grade can be divided into low or high orcan be scored from 1 to 3. Often this number has a G as a prefix toshow it represents the grade, e.g. G1, G2 or G3.
Urothelial Carcinoma With Trophoblastic Differentiation
More than 30 cases of urothelial carcinoma with areas of trophoblastic differentiation have been reported and a small subset has had symptoms related to excess human chorionic gonadotropin production including gynecomastia., , , , Although some of the early reports have described tumors that apparently were composed solely of tissue resembling choriocarcinoma, most tumors reported in the last three decades or so have been composed of a mixture of urothelial carcinoma with trophoblastic elements. A single case of micropapillary carcinoma with trophoblastic elements has been reported.
Figure 11
Also Check: Can Merkel Cell Carcinoma Be Cured
Also Check: Melanoma Bone Cancer Symptoms
Treating Stage Iv Bladder Cancer
These cancers have reached the pelvic or abdominal wall , may have spread to nearby lymph nodes , and/or have spread to distant parts of the body . Stage IV cancers are very hard to get rid of completely.
Chemotherapy is usually the first treatment if the cancer has not spread to distant parts of the body . The tumor is then rechecked. If it appears to be gone, chemo with or without radiation or cystectomy are options. If there are still signs of cancer in the bladder, chemo with or without radiation, changing to another kind of chemo, trying an immunotherapy drug, or cystectomy may be recommended.
Chemo is typically the first treatment when bladder cancer has spread to distant parts of the body . After this treatment the cancer is rechecked. If it looks like it’s gone, a boost of radiation to the bladder may be given or cystectomy might be done. If there are still signs of cancer, options might include chemo, radiation, both at the same time, or immunotherapy.
In most cases surgery cant remove all of the cancer, so treatment is usually aimed at slowing the cancers growth and spread to help people live longer and feel better. If surgery is a treatment option, it’s important to understand the goal of the operation whether it’s to try to cure the cancer, to help a person live longer, or to help prevent or relieve symptoms from the cancer.
Because treatment is unlikely to cure these cancers, many experts recommend taking part in a clinical trial.
Prognosis And Life Expectancy
In general, papillary urothelial cancers have a better prognosis than other types of bladder cancer. Your specific outlook depends on the stage and grade of your cancer. High-grade cancers can spread. Low-grade papillary cancers are less likely to spread. Papillary cancers can also return after theyve been treated.
You May Like: Lobular Breast Cancer Stage 3
Standard Treatment Options For Stages Ii And Iii Bladder Cancer
The most common treatments for muscle-invasive bladder cancer are radical cystectomy and radiation therapy. There is no strong evidence from randomized controlled trials to determine whether surgery or radiation therapy is more effective. There is strong evidence that both therapies become more effective when combined with chemotherapy. The treatments with the highest level of evidence supporting their effectiveness are radical cystectomy preceded by multiagent cisplatin-based chemotherapy and radiation therapy with concomitant chemotherapy.
Radical cystectomy
Radical cystectomy is a standard treatment option for stage II and stage III bladder cancer, and its effectiveness at prolonging survival increases if it is preceded by cisplatin-based multiagent chemotherapy. Radical cystectomy is accompanied by pelvic lymph node dissection and includes removal of the bladder, perivesical tissues, prostate, and seminal vesicles in men and removal of the uterus, fallopian tubes, ovaries, anterior vaginal wall, and urethra in women. Studies of outcomes after radical cystectomy report increased survival in patients who had more, rather than fewer, lymph nodes resected whether this represents a therapeutic benefit of resecting additional nodes or stage migration is unknown. There are no randomized controlled trials evaluating the therapeutic benefit of lymph node dissection in this setting.
Evidence :
Evidence :
Segmental cystectomy
Cellular Classification Of Bladder Cancer
More than 90% of bladder cancers are transitional cell carcinomas derived from the uroepithelium. About 2% to 7% are squamous cell carcinomas, and 2% are adenocarcinomas. Adenocarcinomas may be of urachal origin or nonurachal origin the latter type is generally thought to arise from metaplasia of chronically irritated transitional epithelium. Small cell carcinomas also may develop in the bladder. Sarcomas of the bladder are very rare.
Pathologic grade of transitional cell carcinomas, which is based on cellular atypia, nuclear abnormalities, and the number of mitotic figures, is of great prognostic importance.
References
You May Like: Body Cancer Symptoms
Low Grade And High Grade
Bladder cancer can also be described as either low grade or high grade.
Low grade bladder cancer means that your cancer is less likely to grow, spread and come back after treatment. High grade means your cancer is more likely to grow spread and come back after treatment.
For example, if you have early bladder cancer but the cells are high grade, youâre more likely to need further treatment after surgery. This is to reduce the risk of your cancer coming back.
Low grade is the same as grade 1. High grade is the same as grade 3. Grade 2 can be split into either low or high grade. Carcinoma in situ tumours are high grade.
You May Like: How Deadly Is Squamous Cell Carcinoma
Turbt/ Repeat Resection: Timing Technique Goal Indication

Guideline Statement 12
12. In a patient with non-muscle invasive disease who underwent an incomplete initial resection , a clinician should perform repeat transurethral resection or endoscopic treatment of all remaining tumor if technically feasible.
Discussion
Incomplete resection is likely a significant contributing factor to what have been described and diagnosed as early recurrences, as tumors have been noted at the first follow-up cystoscopic evaluation in up to 45% of patients. 57 The Panel recognizes specific, albeit rare, circumstances in which transurethral resection is not likely to impact clinical management and may be omitted for patients with incompletely resected non-muscle invasive disease. Examples of such patients include those with large-volume, high-grade tumors not amenable to complete endoscopic resection for whom immediate radical cystectomy is planned. An additional example includes those patients with a tumor diagnosed within a bladder diverticulum and for whom subsequent surgical resection is planned. However, for the majority of patients, complete resection is essential for adequate staging and optimal clinical management. Although surgeons may utilize BLC for this situation, of note, there is insufficient evidence in this repeat transurethral resection setting to support the routine use of enhanced or BLC versus standard WLC, particularly in light of the noted increase in false positive diagnosis with BLC following recent TURBT. 116-118
Discussion
Don’t Miss: Well Differentiated