How To Protect Yourself From Melanoma
Fortunately, most melanomas are diagnosed in early, localized stages, says Dr. González, and most patients treated for melanoma make a full recovery. But we do have patients that have ignored that funny looking mole for way too long, and its not uncommon to see cases that have metastasized to other organs, she adds.
Melanoma tends to a very aggressive form of cancer, and it can progress quickly from one stage to another. Says Dr. González: As soon as you see something unusual you should get it checked out, and as soon as you get a diagnosis, you need to be on top of the appropriate treatment.
Risk factors for melanoma include ultraviolet light exposure , having fair skin and light hair, and having a close relative whos also had melanoma. But monitoring skin for abnormal growths and changes is important for everyone, whether or not they are predisposed to skin cancer.
Going to see your board-certified dermatologist yearly and doing regular skin exams may not seem that important, Dr. González says, but these are the things that could save your life.
Stage 4 Peritoneal Mesothelioma
There is no official stage 4 for peritoneal mesothelioma. This type of the cancer accounts for roughly 20% of all mesothelioma cases. It is generally accepted that peritoneal patients with extensive tumor spreading are classified as stage 4.
For people who can try surgery, heated intraperitoneal chemotherapy is the most promising option. It combines surgery and heated chemotherapy circulated throughout the abdomen.
What Is The Prognosis For People With Inflammatory Breast Cancer
IBC usually develops quickly and spreads to other tissues outside the breast. Early diagnosis and treatment are key to managing the condition as effectively as possible.
Doctors use a system made up of four stages to diagnose all types of cancer. IBC is stage III or stage IV when it is diagnosed.
Because IBC is aggressive, and because it is found later than other cancers, the outlook for people with this condition is generally not as good as for other types of breast cancer. Still, some people have lived many years after an IBC diagnosis. Your doctor can explain your individual prognosis to you.
Also Check: Is Breast Cancer Considered Internal Cancer
Also Check: Merkel Cancer Prognosis
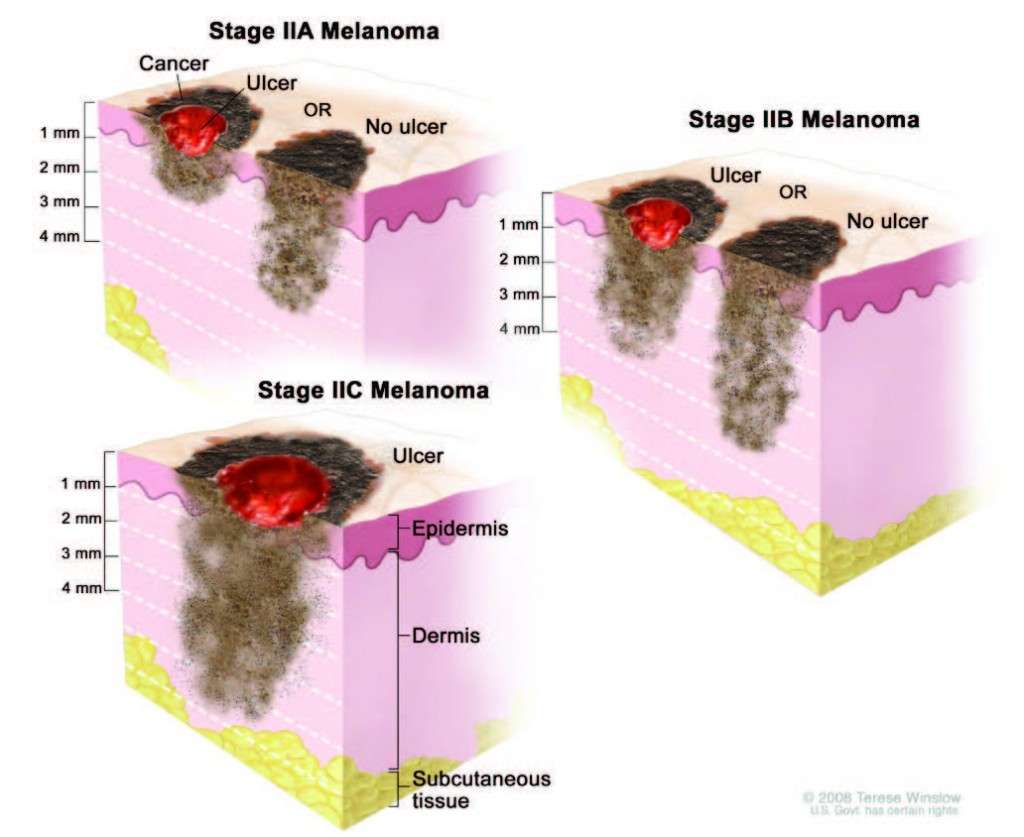
How Is Melanoma Staged
Melanoma stages are assigned using the TNM system.
The stage of the disease indicates how much the cancer has progressed by taking into account the size of the tumor, whether its spread to lymph nodes, and whether its spread to other parts of the body.
A doctor can identify a possible melanoma during a physical exam and confirm the diagnosis with a biopsy, where the tissue is removed to determine if its cancerous.
But more sophisticated technology, such as PET scans and sentinel lymph node biopsies, are necessary to determine the cancers stage or how far its progressed.
There are five stages of melanoma. The first stage is called stage 0, or melanoma in situ. The last stage is called stage 4. Survival rates decrease with later stages of melanoma.
Its important to note that survival rates for each stage are just estimates. Each person with melanoma is different, and your outlook can vary based on a number of different factors.
What Are The Treatments For Metastatic Melanoma
Ideally, melanoma is diagnosed and treated surgically while it is still small and thin and before it has had the chance to metastasize. The prognosis and survivability of metastatic melanoma remain poor compared to other types of cancer. Metastatic melanoma is less responsive to radiation therapy and traditional forms of chemotherapy than other forms of cancer.
Immunotherapy in which the body’s own immune system is used to fight the tumor has been a focus of research for decades and immune system “stimulants” such as interferon-alpha and interleukin-2 have also been tried for many years.
A variety of newer medications target different points in the biologic pathways of melanoma growth and spread. The following are drugs currently in use, or being actively investigated. More should be available shortly.
- Inhibition of kinase enzymes needed in cell reproduction like MEK: cobimetinib , trametinib
- Target cell growth signals from abnormal BRAF genes: dabrafenib , vemurafenib , nivolumab
- Improve immune response to the tumor: pembrolizumab , ipilimumab
As monotherapy , these drugs have not been shown to dramatically improve survival even if they did improve disease-free time. The hope is that combinations of medications targeting more than one part of the melanoma growth and metastasis pathway will provide more encouraging results.
Also Check: What Is The Survival Rate For Invasive Lobular Carcinoma
Tools That Can Help You Find Melanoma On Your Skin
To help you find melanoma early, the American Academy of Dermatology developed the following:
Melanoma can look different on a childs skin. Taking this short quiz can help you hone your skills at finding childhood melanoma.
ImagesImages 1,3,4,5,6,7,8,10: Images used with permission of the American Academy of Dermatology National Library of Dermatologic Teaching Slides.
Image 2: Developed by the American Academy of Dermatology
Image 9: Used with permission of the Journal of the American Academy of Dermatology.
ReferencesBarnhill RL, Mihm MC, et al. Malignant melanoma. In: Nouri K, et al. Skin Cancer. McGraw Hill Medical, China, 2008: 140-167.
Gloster HM Jr, Neal K. Skin cancer in skin of color. J Am Acad Dermatol 2006 55:741-60.
National Comprehensive Cancer Network. NCCN guidelines for patients: Melanoma. 2018. Last accessed February 12, 2019.
Treatment For Desmoplastic Melanoma
Desmoplastic melanoma is highly curable when diagnosed early. The goals for treatment of desmoplastic melanoma are to:
- cure the cancer
- preserve the appearance of your skin
- prevent the cancer from coming back
The extent and depth of the melanoma guides your care plan. Treatment often involves surgery to remove the melanoma. MSK doctors have particular expertise in removing these cancers, which usually occur in important and sensitive areas of the body.
If the melanoma is more advanced and has spread to other parts of the body, such as the lymph nodes or internal organs, immunotherapy, targeted therapy, chemotherapy, radiation, surgery, or a combination of therapies may be used to shrink the tumor.
You May Like: Stage Iiia Melanoma Prognosis
Systemic Adjuvant Treatment Of Stage Iii Melanoma
Systemic therapy is any treatment directed at destroying cancer cells throughout the body. Many patients with stage III melanoma are at high risk for disease recurrence because undetectable cancer cells referred to as micrometastases have already broken away from the primary cancer and traveled through the lymph and blood system to other locations in the body. The delivery of systemic cancer treatment following surgery is referred to as adjuvant therapy.
Adjuvant treatment of stage III melanoma with newer precision cancer medicines and immunotherapy drugs is the standard of care because they delay the time to cancer recurrence and prolong survival.
Dont Miss: What Type Of Skin Cancer Spreads The Fastest
Red Flag #: Swollen Lymph Nodes
If melanoma spreads, it often goes to the lymph nodes first, says Melinda L. Yushak, M.D., assistant professor of hematology and medical oncology at Emory University School of Medicine in Atlanta. The cancer cells will first travel to the nodes closest to the original tumor, she says. Lymph nodes are located throughout your entire body, but large clusters are found in the neck, underarms, chest, abdomen, and groin. If the cancer has made its way to the lymph nodes, it usually wont be painful, but theyll feel swollen or even hard to the touch, Dr. Zaba says.
Read Also: Invasive Ductal Breast Cancer Survival Rate
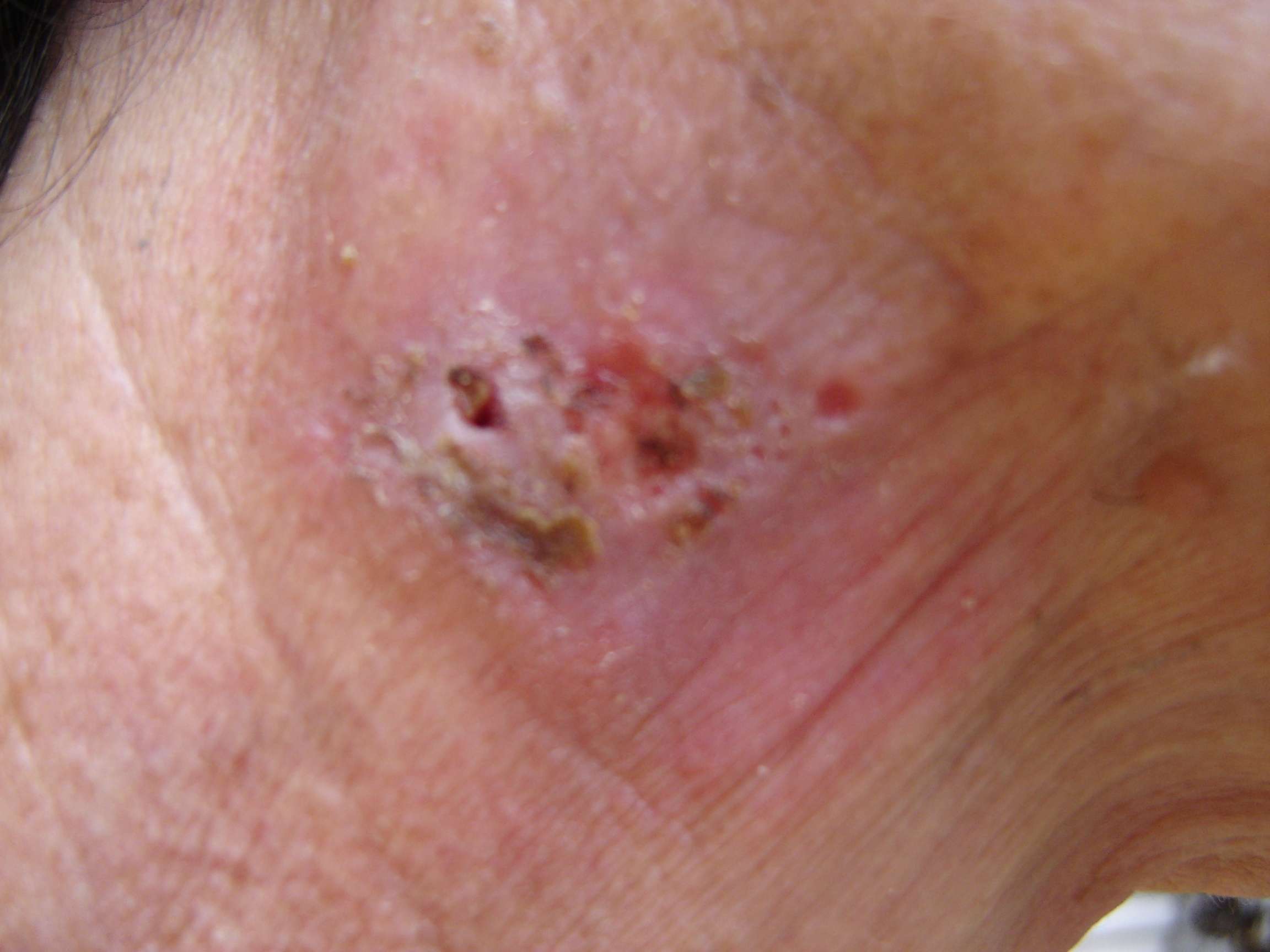
What Do Stage 4 Tumors Look Like
A change to an existing mole or normal skin can be the first sign that the cancer has spread. But the physical symptoms of stage 4 melanoma arent the same for everyone. A doctor will diagnose stage 4 melanoma by looking at the primary tumor, the spread to nearby lymph nodes, and whether the tumor has spread to different organs. While your doctor wont base their diagnosis only on what your tumor looks like, part of their diagnosis involves looking at the primary tumor.
How Can I Take Care Of Myself While Living With Metastatic Breast Cancer
Living with metastatic breast cancer can be challenging. Your care team can help provide physical and emotional support. Talk to them about how you can:
- Eat the most nutritious diet for your needs.
- Exercise regularly.
- Get emotional support, including finding support groups.
- Reach out for help from friends, family and loved ones.
- Find mental health services.
Recommended Reading: Scalp Melanoma Stages
What Are Some Of The Cancer Type
Breast and prostate cancers are the most common types of cancer that have their own grading systems.
Breast cancer. Doctors most often use the Nottingham grading system for breast cancer . This system grades breast tumors based on the following features:
- Tubule formation: how much of the tumor tissue has normal breast duct structures
- Nuclear grade: an evaluation of the size and shape of the nucleus in the tumor cells
- Mitotic rate: how many dividing cells are present, which is a measure of how fast the tumor cells are growing and dividing
Each of the categories gets a score between 1 and 3 a score of 1 means the cells and tumor tissue look the most like normal cells and tissue, and a score of 3 means the cells and tissue look the most abnormal. The scores for the three categories are then added, yielding a total score of 3 to 9. Three grades are possible:
- Total score = 35: G1
- Gleason X: Gleason score cannot be determined
- Gleason 26: The tumor tissue is well differentiated
- Gleason 7: The tumor tissue is moderately differentiated
- Gleason 810: The tumor tissue is poorly differentiated or undifferentiated
What About Other Treatments I Hear About
When you have cancer you might hear about other ways to treat the cancer or treat your symptoms. These may not always be standard medical treatments. These treatments may be vitamins, herbs, special diets, and other things. You may wonder about these treatments.
Some of these are known to help, but many have not been tested. Some have been shown not to help. A few have even been found to be harmful. Talk to your doctor about anything youre thinking about using, whether its a vitamin, a diet, or anything else.
Don’t Miss: Invasive Ductal Carcinoma Stage 3 Survival Rate
Red Flag #: Bone Pain Or Fractures
The bones are considered a late-stage site of melanoma metastasestypically, it doesnt spread to the bones until its already spread to another area of the body first. Melanoma can cause pain in the bones where its spread, and some peoplethose with very little body fat covering their bonesmay be able to feel a lump or mass. Metastatic melanoma can also weaken the bones, making them fracture or break very easily. This is most common in the arms, legs, and spine. If you feel any sharp, sudden, or new pains that wont go away, talk to your doctor.
What Are The Prognosis And Survival Rates For Metastatic Melanoma
The prognosis for thin melanomas completely removed by surgery remains quite good although patients require long-term monitoring to watch for both new melanomas as well as evidence of late recurrence and previously undiagnosed metastasis of the original one. Survival rates for melanoma, especially for metastatic melanoma, vary widely according to many factors, including the patient’s age, overall health, location of the tumor, particular findings on the examination of the biopsy, and the depth and stage. Survival statistics are generally based on five-year survival. Much of the success reported for the targeted therapies focus on “disease free” time because, in many cases, the actual five-year survival is not affected. It is hoped that combination therapy with two or more agents targeting different stages of the melanoma cell cycle will change that.
- For stage 1 , five-year survival is near 100%.
- For stage 2 , five-year survival is 80%-90%.
- For stage 3 , five-year survival is around 50%.
- For stage 4 , five-year survival is 10%-25% depending upon sex and other demographic factors.
Recommended Reading: How Do Carcinomas Spread
S To Consider After A Stage 4 Diagnosis
- Get a second opinion from a mesothelioma specialist.
- Find financial assistance available to offset potential monetary burden.
- Enroll in a clinical trial. Consult with your doctor to determine if you are eligible.
- Try alternative and complementary treatment options.
- Exercise and maintain a healthy diet to improve mood and quality of life.
- Join a support group to connect with others coping with mesothelioma.
- Make time for hobbies and activities that bring you joy.
- Read stories about other mesothelioma survivors for hope and inspiration.
Treating Stage 0 Melanoma
Stage 0 melanoma has not grown deeper than the top layer of the skin . It is usually treated by surgery to remove the melanoma and a small margin of normal skin around it. The removed sample is then sent to a lab to be looked at with a microscope. If cancer cells are seen at the edges of the sample, a second, wider excision of the area may be done.
Some doctors may consider the use of imiquimod cream or radiation therapy instead of surgery, although not all doctors agree with this.
For melanomas in sensitive areas on the face, some doctors may use Mohs surgery or even imiquimod cream if surgery might be disfiguring, although not all doctors agree with these uses.
Read Also: Melanoma 3c
Clinical Characteristics Of The Patients With Brain Metastasis
A total of 79 patients were identified for this analysis. The demographic and baseline characteristics of the patients are described in Table . The median time from primary melanoma diagnosis to brain metastasis was 3.2 years , and the median time from stage IV diagnosis to brain metastasis was 2 months . Forty patients had prior extracranial metastasis at the time of initial brain metastasis 28 had concurrent extracranial metastasis at the time of brain metastasis and 5 patients developed extracranial metastasis subsequently, defined as at least 1 month after initial diagnosis of brain metastasis. Six patients had brain metastasis as the only site of distant metastasis until death or at the time of the analysis.
Table 1 Patient characteristics and treatment
The cerebrum was the most common site of brain metastasis , and 21.5% and 8.9% patients had metastasis to the cerebellum and pons, respectively. Thirty-nine had a solitary brain metastasis at the initial brain metastasis diagnosis, and the largest size of the initial brain metastasis was 10 mm or less in 31.7%. Thirty-six patients had neurological symptoms associated with brain metastasis. Forty-nine of the 79 patients had received systemic therapy prior to or at the time of brain metastasis, including checkpoint inhibitors, targeted drugs, cytotoxic chemotherapy and/or cytokine therapy.
Also Check: Grade 3 Cancer Treatment
Skin Exam And Physical
You may have had a complete skin exam during your last dermatology appointment. Dermatologists often perform this exam when a patient has a suspicious spot on their skin that could be skin cancer.
During a complete skin exam, your dermatologist examines you head to toe. This exam includes a look at all of your skin, including the skin on your scalp, face, genitals, and the bottoms of your feet. Your dermatologist will also examine your nails and look inside your mouth.
If you did not have a complete skin exam before being diagnosed with melanoma, youll have one at your next appointment.
During a complete skin exam, your dermatologist may use a device called a dermatoscope
This device provides a closer look at the spots on your skin.
At your next appointment, youll receive a physical. During your physical, your dermatologist will ask how youre feeling and about your health, illnesses, and injuries. Your dermatologist will also want to know what diseases run in your family and the medications you take.
During your physical, your dermatologist will check your lymph nodes to find out if any feel swollen. There are many reasons for swollen lymph nodes. For example, if you have an infection or recently received a vaccination, lymph nodes can feel swollen. When you have melanoma, the swelling might be a sign that the cancer has spread.
If youre unsure what diseases your close blood relatives have had, try to find out
Don’t Miss: Grade 3 Cancer Treatment
Who Is More Likely To Develop Lobular Breast Cancer
Risk factors for developing lobular breast cancer are the same as those for developing breast cancer in general. These include:
- Older age. The risk of breast cancer increases with age. Most breast cancers are diagnosed after age 50.
- Being diagnosed with lobular carcinoma in situ. This means you have abnormal cells confined within the lobules of your breast. Although this is not considered cancer, it does increase your risk of developing breast cancer.
- Family history of breast cancer. Having a mother, sister, or daughter who has had breast cancer.
- Early puberty/late menopause. Starting your period at an early age or experiencing late menopause .
- Not having children/later childbirth. Not having children or having your first child after the age of 35.
- Postmenopausal hormone use. Using the female hormones estrogen and progesterone for more than 5 years to manage menopause symptoms.
- Exposure to radiation. Receiving radiation to the breast or chest to treat cancer before the age of 30.
- Having genetic mutations for certain types of breast cancer. Being a carrier of the familial breast cancer genes, BRCA1 and BRCA2.
- Being overweight.
- Drinking alcohol. Compared with nondrinkers, women who consume one alcoholic drink a day have a 10% increase in risk. The risk increases the more you drink.
Treating Stage Iv Melanoma
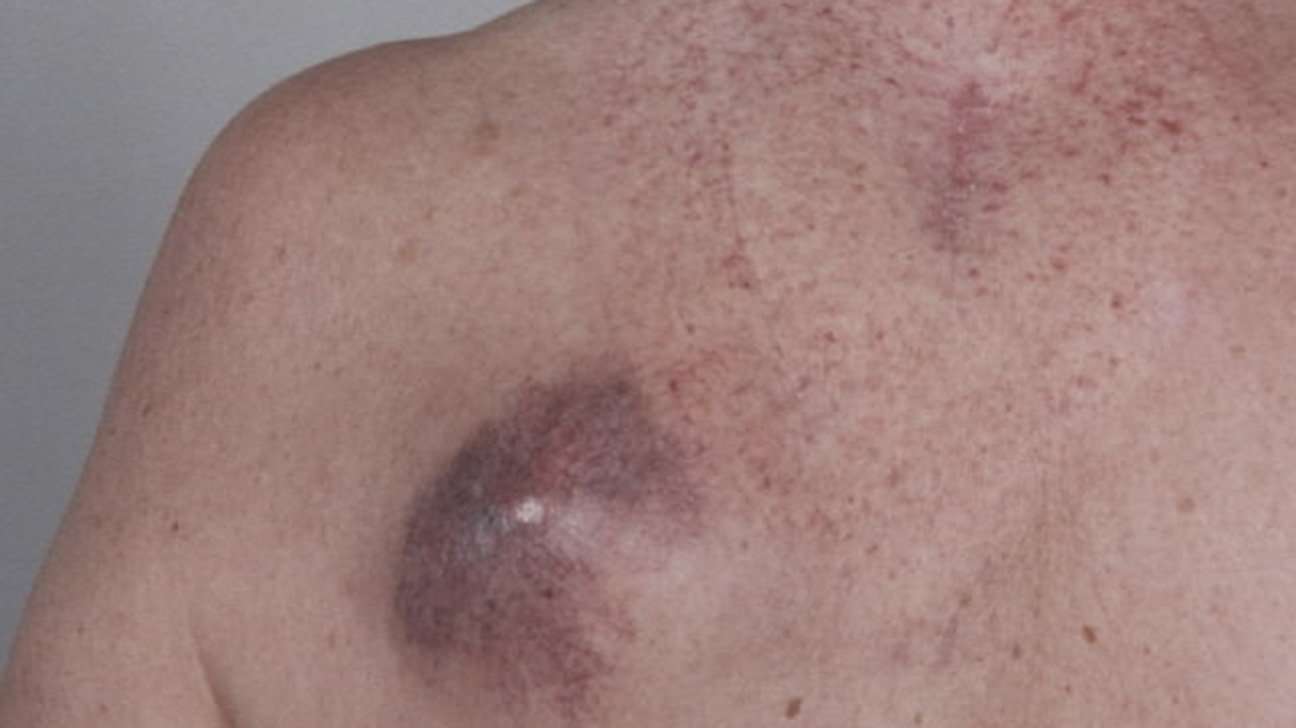
Stage IV melanomas have already spread to distant lymph nodes or other areas of the body. Skin tumors or enlarged lymph nodes causing symptoms can often be removed by surgery or treated with radiation therapy.
Metastases in internal organs are sometimes removed, depending on how many there are, where they are, and how likely they are to cause symptoms. Metastases that cause symptoms but cannot be removed may be treated with radiation, immunotherapy, targeted therapy, or chemotherapy.
The treatment of widespread melanomas has changed in recent years as newer forms of immunotherapy and targeted drugs have been shown to be more effective than chemotherapy.
Immunotherapy drugs called checkpoint inhibitors such as pembrolizumab or nivolumab are typically the first drugs tried, especially in people whose cancer cells do not have BRAF gene changes. These drugs can shrink tumors for long periods of time in some people. Ipilimumab , a different type of checkpoint inhibitor, is not typically used by itself as the first treatment, although it might be combined with nivolumab or pembrolizumab. This slightly increase the chances that the tumor will shrink, although itâs also more likely to result in serious side effects, which needs to be considered carefully. People who get any of these drugs need to be watched closely for serious side effects..
Itâs important to carefully consider the possible benefits and side effects of any recommended treatment before starting it.
Recommended Reading: Invasive Ductal Carcinoma Survival Rate Stage 1