Treatments For Autoimmune Skin Disease
The best way to treat your skin lesions is by treating the underlying cause, which is the autoimmune disorder itself. As symptoms can range from very mild to severe, doctors will usually prescribe medications to alleviate the symptoms and decrease inflammation in order to make patients more comfortable. Here are some common treatment methods for calming down symptoms.
Topical Steroids: These consist of creams aimed at reducing inflammation and irritation of the skin. You can get prescription-strength topical steroids from your doctor or go with a lower strength over-the-counter option such as hydrocortisone.
Oral Steroids and Immunosuppressive Drugs: These medications reduce inflammation by altering the immune response to combat autoimmune diseases. They are more effective than topical steroids, but come with a greater chance of side effects.
IV Immunoglobulin Therapy: Some autoimmune diseases, such as dermatomyositis, will require IVIG therapy. This treatment consists of infusing a combination of antibodies and other soluble proteins to neutralize the immune responses that cause inflammation. If your doctor determines that this is the best course of action, you may need to visit a facility for regular treatments over time.
Sleep: Perhaps the simplest but most ignored remedy for dealing with autoimmune disease is getting adequate sleep. Sleeping for at least 7 to 8 hours a night will reduce stress, inflammation, and cravings for high sugar foods.
Our Blog
What Is An Autoimmune Disorder
Autoimmune conditions occur when the body incorrectly identifies something not native to the body and creates an immune response to reject it. When the immune system works right, it keeps you healthy by fighting off intruding unhealthy organisms and even cancerous cells. But with autoimmune conditions, the body revs up your immune system to fight against its own cells, which causes a multitude of problems.
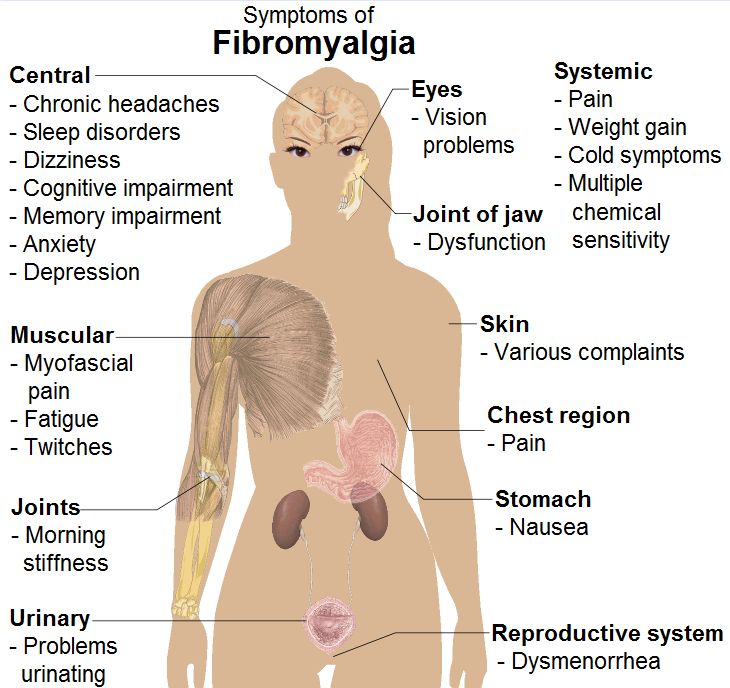
Autoimmune disorders can attack any part of the body. However, some of these become most apparent in how they affect the skin. With most autoimmune disorders of the skin, patients experience both systemic manifestations and symptoms on the skin.
Clinical Phenotypes Of Oral Involvement In Autoimmune Disorders
Autoimmune diseases may manifest on oral mucous membrane as erythema, blisters, erosions, and ulcerations. By far, oral blisters and ulcerations are the most common presenting features of immune-mediated disorders in the oral cavity. Oral blisters erode rapidly and leave behind ulcers associated with moderate to severe pain and discomfort that may interfere with speaking, eating and swallowing. A variety of local and systemic factors and conditions may trigger mucosal ulceration such as trauma,
Also Check: Who Do You See For Skin Cancer Screening
What Causes Common Autoimmune Skin Diseases
Unfortunately, the exact cause of autoimmune diseases is not yet understood. Some research points to a genetic predisposition that may involve a mutation in specific genes and affect mucous membranes, which signal the immune system to attack healthy tissue. There is not one particular gene that causes these autoimmune conditions but rather a combination of several genes. Most clinical dermatology specialists believe that lifestyle and environmental risk factors play a role in bringing these genetic factors to the surface. This includes exposure to certain viruses and bacteria or the use of particular drugs.
Are Autoimmune Skin Diseases Contagious?
We know that autoimmune diseases are not contagious, and therefore, the skin lesions and rashes they cause are not contagious either. Even if you make direct skin-to-skin contact with someone that has a chronic autoimmune disorder, you will not be affected or experience skin rashes yourself. Again, these rare disorders arise from a combination of hereditary and environmental factors, and are not spread from person to person like the common cold.
How Can I Identify an Autoimmune Rash?
What Are The Treatment Options For Autoimmune Disorders
Autoimmune disease treatments may include drugs that suppress your immune system as well as therapies that target the specific organs affected.
The most common drugs used to treat autoimmune disorders include:
- Immunosuppressant drugs
- Nonsteroidal anti-inflammatory drugs , such as ibuprofen and naproxen
- Corticosteroids
Don’t Miss: What Does Basal Skin Cancer Look Like
What Causes Autoimmune Disease
“…some theorize that genetics and/or environmental pollutants play a role.”
The cause or causes of autoimmune disease are not fully understood, although some theorize that genetics and/or environmental pollutants play a role. Ultraviolet exposure is thought to be a predisposing or triggering cause of autoimmune skin diseases in some dogs. Certain drugs have also been reported as potential triggers for pemphigus foliaceus, a common form of autoimmune skin disease in dogs and cats. Early recognition is extremely important. Left untreated, the complications of autoimmune disease are serious and multiple system involvement is common. This can make diagnosis and treatment very challenging and complicated.
How Does Scleroderma Affect The Skin
Scleroderma is a term that just means ‘hard skin.’ Like lupus, patients having scleroderma skin changes have a variable risk for having associated damage to internal organs, especially the kidneys and lungs.
Some patients develop a form of scleroderma that never goes on to cause damage to internal organs. This form of the disease is called localized scleroderma or morphea. However, other patients with scleroderma do develop internal complications relatively soon after the onset of skin problems.
Also Check: How Bad Is Basal Cell Carcinoma
Other Autoimmune Skin Diseases With Oral Manifestations
Oral lesions may less commonly manifest other autoimmune skin diseases such as bullous pemphigoid and dermatitis herpetiformis. Bullous pemphigoid is a subepidermal blistering disease characterized by autoantibodies directed against the basement membrane zone and targeting a 230-kDa protein and a 180-kDa transmembrane protein . Bullous pemphigoid is the most common autoimmune blistering disease in North America and Western Europe, with a recent reported incidence of 4.3 cases per
Common Autoimmune Skin Disorders And Treatments
- Bullous pemphigoid, pemphigus, and epidermolysis bullosa aquisita: These rare disorders cause large fluid-filled blisters to develop on the skin. Treatments may include corticosteroids, immuno-suppressing medications, and anti-inflammatory drugs.
- Dermatomyositis: This conditions can cause a distinct skin rash, discoloration and swelling. It can usually be treated with steroids and other medications.
- Scleroderma: This disorder can cause skin thickening, scarring and inflammation, and can be treated with prescription moisturizers or corticosteroid creams.
- Vasculitis: This condition causes inflammation of the blood vessels, and can affect many parts of the body, including the skin. Treatments include steroids and other medications.
Also Check: What Is Urothelial Carcinoma In Situ
What Is An Autoimmune Disease
Our bodies have an immune system that protects us from foreign invaders that can cause disease and infection. If you have an autoimmune disease, however, your immune system attacks itself by mistake, causing serious illness. The immune cells fail to distinguish the body’s normal healthy cells from foreign cells, and thus try to destroy the normal tissues. The cause of this “mistake” is not well understood. Autoimmune disease can affect a single system or multiple body systems. Autoimmune diseases can affect skin, connective tissues, nerves, muscles, the endocrine system , red blood cells, and the digestive system. Dogs and cats with autoimmune diseases should not be vaccinated except under certain circumstances your veterinarian can discuss this further with you.
Induction Of Autoimmunity Against Skin Antigens
There are multiple theories that explain how the loss of tolerance to self-antigens initially occurs and it is understood that the majority of AIBDs are a product of several aberrant processes which disrupt skin barrier homeostasis. Genetic factors play an important role, as specific skin blistering diseases have varying prevalence in different populations and inherited human leukocyte antigen types are associated with autoreactivity to specific autoantigens . Multiple HLA alleles have been identified which are associated with pemphigus vulgaris , BP , and EBA . Genetic susceptibility is not limited to HLA types, as pemphigus vulgaris has been associated with mutations in ST18 in certain populations and experimental models of EBA have identified non-HLA murine gene loci that confer susceptibility to disease development , however further studies are required to extrapolate these findings to clinical populations.
Read Also: Is Adenoid Cystic Carcinoma Curable
What Are Autoimmune Skin Diseases
Autoimmune skin diseases are a group of disorders in which the immune system mistakenly attacks healthy tissue. Our immune system functions with the help of antibodies and white blood cells, which are produced to help defend against foreign substances that cause disease. In the case of autoimmune disease, our bodys natural defenses turn and attack its cells instead of an outside invader. There are a variety of autoimmune diseases that affect different parts of the body, and some will affect several parts of the body at once. Common symptoms include disorders of internal organs, joints, muscles, and the skin. In this article, we will look to explore autoimmune skin diseases and provide an understanding of the best ways to keep them under control.
Autoimmune Disease And Your Health
Having lupus, rheumatoid arthritis or psoriatic arthritis raises your risk for heart disease. While taking steps to reduce heart disease is always a good idea, it is even more essential if you have one of these conditions. Talk to your doctor about what you can do to keep your heart healthy and strong. For example, keeping your blood pressure and cholesterol levels within healthy ranges, eating a nutritious diet and exercising regularly can be lifesaving.
These steps can also help reduce the symptoms of autoimmune disease. In serious cases, global immune suppressing drugs are used to restrain the bodys immune response, preventing it from doing further harm. Unfortunately, immunosuppressants render people more susceptible to infections.Orbai admits that making time for healthy living can be hard, given womens fast-paced lives, but she insists that finding the balance is key to living with autoimmune disease.
Its something thats going to involve commitment, and sometimes its going to be tough, she says. But learning to listen to your body and being smart about what triggers your disease is important. Its something you do for yourself.
Don’t Miss: How To Reduce Risk Of Skin Cancer
Other Rare Blistering Diseases
Dermatitis herpetiformis is an itchy blistering skin disease that typically affects the elbows, knees, and buttocks. It is associated with coeliac disease and the symptoms heal with a gluten-free diet . It is characterised by blisters with a subepidermal deposition of immunoglobulin A and a neutrophilicinfiltrate. In dermatitis herpetiformis, the antibodies in the autoimmune response target the coagulationenzyme epidermal transglutaminase .
Linear IgA bullous dermatosis is a very rare autoimmune blistering disorder that can be acquired or drug-induced . The blisters are sometimes arranged in rings . There is a subepidermal deposition of IgA antibodies which target a portion of the BP180 antigen, type VII collagen, or other basement membrane proteins.
Epidermolysis bullosa acquisita is also very rare. In its classical form, blisters and erosions form at areas of minor trauma . In epidermolysis bullosa acquisita, the autoimmune reaction is directed against type VII collagen in the basement membrane zone of the skin and mucosa.
Bullous systemic lupus erythematosus is a rare presentation of subepidermal blistering in a patient with systemic lupus erythematosus.
Pyodermatitis Vegetans Pyostomatitis Vegetans Pyodermatitispyostomatitis Vegetans
Pyodermatitis vegetans , a rare skin manifestation of IBD and often regarded as one of clinical forms of PG, has histopathology similar to pyostomatitis vegetans but with treatment similar to PG . PDV occurs mainly in skin folds such as axillary or inguinal area, but can also be present on the trunk or extremities. These lesions are characterized by pustules that quickly rupture, forming erosions with hemorrhagic ground, developing large raised well-demarcated plaques with surrounding pustules .
Pyodermatitis vegetans was first reported by Hallopeau when he described two patients with unusual pustular dermatosis and oral lesions for which he named pyodermite vegetans . McCarthy proposed the term pyostomatitis vegetans after he observed similar lesions isolated in the oral cavity . Recently these two entities are considered to be variants of the same disease termed pyodermatitispyostomatitis vegetans . PDV and PSV are rare cutaneous manifestation of IBD . In general, bowel disease antedate oral involvement by several years . The rash of PPV has been reported to correlate with underlying bowel disease activity . The pathogenesis of PSV, PDV, or PPV is not clear, but has been hypothesized to be due to aberrant immune responses in IBD to cross-reacting antigens in the skin and bowel resulting in mucocutaneous manifestations .
Don’t Miss: Is Transitional Cell Carcinoma Curable
How Is Pemphigus Vulgaris Diagnosed
Blisters also occur with many other common conditions, so pemphigus, which is rare, can sometimes be difficult to diagnose. During the visit, a physician diagnoses based on the medical history and physical examination of the skin and mouth. In addition, the doctor may undergo the following tests:
-
Skin biopsy, in which a piece of tissue from a blister is removed and examined under a microscope.
-
Blood tests help detect and identify antibodies in the blood that are known to be present with pemphigus vulgaris.
-
Endoscopy may be done to look for sore throat by inserting a flexible tube down the throat.
What Do I Do If I Suspect An Autoimmune Disorder Of The Skin
Anytime you experience a persistent skin rash, schedule an appointment with your dermatologist. You may be dealing with a simple topical allergy, eczema, or a more complicated issue like an autoimmune skin disease. A dermatologist is best suited to check the skin for an accurate diagnosis and begin a treatment plan to provide relief to your symptoms right away.
to find an Epiphany provider near you.
Read Also: Hyaluronic Acid For Skin Care
Signs And Symptoms Of A Skin Picking Disorder
Symptoms of skin picking disorder include:
- Recurrent skin picking that leads to skin lesions
- Repeated attempts to stop the behavior
- Significant distress or impairment due to picking
- An urge to pick or physical tension thats relieved by picking
- Unusual sensations
- Beliefs about how the skin should look or feel
To be diagnosed with skin picking disorder, your symptoms cant be better explained by another psychiatric disorder and arent caused by another medical condition, a skin condition, or a substance .
Treatment For Autoimmune Disorders Of The Skin At Penn
Patients who choose or are referred to Penn Dermatology for treatment of autoimmune disorders are assured exceptional and compassionate care. Several of Penns dermatologists serve on boards or participate on committees of distinguished national organizations, including the Rheumatologic Dermatology Society, Lupus Foundation of America, International Pemphigus and Pemphigoid Foundation, the Scleroderma Foundation and the American College of Rheumatology.
Penn dermatologists are frequently listed under local and national listings of Top Docs in the area of autoimmune idsease.
At Penn Dermatology, patients can seek comprehensive treatment for autoimmune conditions that affect the skin including:
- Cutaneous Lupus for patients with skin problems as a result of cutaneous lupus or systemic lupus with skin disease.
- Dermatomyositis for patients diagnosed with this rare disease characterized by inflammation and a skin rash, sometimes associated with muscle or lung inflammation.
- Morphea/Scleroderma for patients with morphea or localized scleroderma affecting the skin or systemic scleroderma affecting the skin and other organs in the body.
- Vasculitis for patients with autoimmune disease affecting the vessels and other organs in the body.
Recommended Reading: What Does Skin Cancer Look Like On Your Arm
Common Autoimmune Disease Symptoms
Despite the varying types of autoimmune disease, many of them share similar symptoms. Common symptoms of autoimmune disease include:
- Abdominal pain or digestive issues
- Recurring fever
Many women say its hard to get diagnosed, something that Orbai agrees with. Its not black or white, she says. Theres usually no single test to diagnose autoimmune disease. You have to have certain symptoms combined with specific blood markers and in some cases, even a tissue biopsy. Its not just one factor.
Diagnosis can also be difficult because these symptoms can come from other common conditions. Orbai says women should seek treatment when they notice new symptoms.
If youve been healthy and suddenly you feel fatigue or joint stiffness, dont downplay that, she says. Telling your doctor helps him or her to look closer at your symptoms and run tests to either identify or rule out autoimmune disease.
Autoimmune Diseases Of The Skin
Pathogenesis, Diagnosis, Management
You can also search for this editor inPubMed
-
Comprehensive presentation of pathophysiology, clinical diagnosis, and management of cutaneous autoimmune diseases
-
Thoroughly updated with new chapters on inflammatory diseases
-
Presented by world experts in the field
This is a preview of subscription content, access via your institution.
Recommended Reading: How To Get Rid Of Zits Under The Skin
Skin Barrier And Autoimmunitymechanisms And Novel Therapeutic Approaches For Autoimmune Blistering Diseases Of The Skin
- Regenerative Medicine Laboratory, Future Industries Institute, University of South Australia, Adelaide, SA, Australia
One of the most important functions of the skin besides regulating internal body temperature includes formation of the barrier between the organism and the external environment, hence protecting against pathogen invasion, chemical and physical assaults and unregulated loss of water and solutes. Disruption of the protective barrier is observed clinically in blisters and erosions of the skin that form in autoimmune blistering diseases where the body produces autoantibodies against structural proteins of the epidermis or the epidermal-dermal junction. Although there is no cure for autoimmune skin blistering diseases, immune suppressive therapies currently available offer opportunities for disease management. In cases where no treatment is sought, these disorders can lead to life threatening complications and current research efforts have focused on developing therapies that target autoantibodies which contribute to disease symptoms. This review will outline the involvement of the skin barrier in main skin-specific autoimmune blistering diseases by describing the mechanisms underpinning skin autoimmunity and review current progress in development of novel therapeutic approaches targeting the underlying causes of autoimmune skin blistering diseases.
What Are Some Of The Common Autoimmune Skin Diseases In Dogs
Autoimmune skin diseases are relatively rare in dogs. Some of the more common forms of autoimmune skin disease include:
Pemphigus complex
Pemphigus Foliaceus – The term means “leaf-like pemphigus” and this is the most common immune-mediated skin disease of dogs and cats. Pemphigus foliaceus is rarely found in the mouth or at mucocutaneous junctions. In this form of pemphigus, the patient develops crusts and ulcers around the eyes, ears, footpads, groin and bridge of the nose. Breeds more commonly affected included the Chow chow, akita, cocker spaniel, Labrador retriever, dachshund, English bulldog, Finnish spitz, and schipperke. Pemphigus foliaceus usually appears suddenly without a recognized cause. In some cases, however, it may be drug-induced or can be the result of years of chronic skin disease.
Pemphigus erythematosus – The term means “red and inflamed pemphigus” and its most common symptom is redness, crusting, scales and hair loss on the nose. Exposure to ultraviolet light worsens this form of pemphigus. Breed predispositions include the German shepherd dog, collie, and Shetland sheepdog.
Pemphigus vegetans – This form is typified by thick and irregular vegetative lesions or lumps associated with chronic “oozing” and pustules. It is believed to be a more benign form of pemphigus vulgaris. This condition is rare in dogs.
Bullous Pemphigoid
Systemic Lupus Erythematosus
Discoid Lupus Erythematosus
How is autoimmune skin disease diagnosed?
Read Also: What Is Clear Cell Carcinoma Of The Kidney