The Risks The Causes What You Can Do
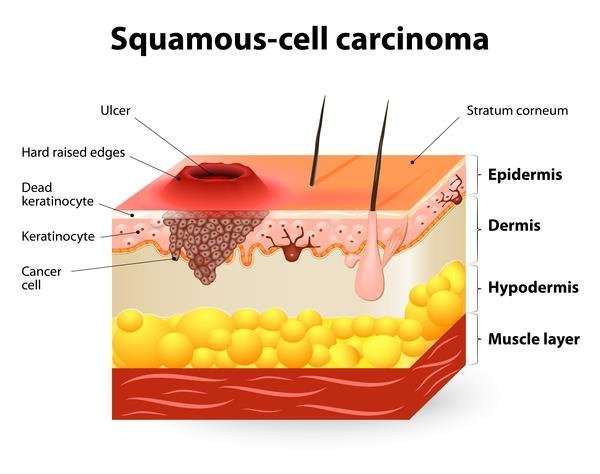
Squamous cell carcinoma of the skin is caused by DNA damage that leads to abnormal changes in the squamous cells in the outermost layer of skin.
Understanding what causes this damage and the factors that increase your risk of developing SCC can help you detect the disease early or prevent it from happening in the first place.
These factors increase your SCC risk:
- Unprotected exposure to ultraviolet radiation from the sun or tanning beds.
- Weakened immune system due to illness or certain immunosuppressive medications.
- History of skin cancer including basal cell carcinoma .
- Age over 50: Most SCCs appear in people over age 50.
- Fair skin: People with fair skin are at an increased risk for SCC.
- Gender: Men are more likely to develop SCC.
- Sun-sensitive conditions including xeroderma pigmentosum.
- Chronic infections and skin inflammation from burns, scars and other conditions.
Supplementary Figure 5 Identification Of Znf750 As A Novel Recessive Cancer Gene In Escc
Box plot showing relative ZNF750 mRNA levels in 947 human cancer cell lines across 21 cancer types analyzed from CCLE database . Number in the parentheses indicates the number of cell lines analyzed. Summary of somatic mutations affecting ZNF750 across different tumor types including mutation data reported by The Cancer Genome Atlas and Catalogue Of Somatic Mutations In Cancer . Number in the parentheses indicates the number of cases sequenced. Concerning C-Mel/CSCC, in TCGA pathological reports, several cutaneous melanoma patients with ZNF750 mutations also had cutaneous squamous cell carcinoma . UASCC, upper aerodigestive squamous cell carcinoma HNSCC, head and neck squamous cell carcinoma CRC, colon and rectum adenocarcinoma LG Glioma, lower grade glioma AML, acute myeloid leukemia GBM, glioblastoma multiforme AG, autonomic ganglia carcinoma. Squamous cell carcinomas were highlighted with Orange Square. Upper panel, mRNA expression of indicated terminal differentiation-related genes quantified with q-PCR in EC109 and KYSE180 cells transfected with either siRNAs against ZNF750 or control siRNA , as well as infected with lentivirus encoding either of ZNF750 protein or GFP . WB results showing ZNF750 protein level in indicated samples. -Actin was used as a loading control. Value represent mean ± s.d. N = 5. Short-term cell proliferation assay of ESCC cells treated with control medium or TPA for 5 days. N = 3. **, P< 0.01 *, P< 0.05.
Incidence Prevalence And Mortality
Global incidence of head and neck squamous cell carcinoma.
The estimated age-standardized rate of HNSCC incidence worldwide is shown for men and women combined. Data from GLOBOCAN, 2018 . Map was generated using the GLOBOCAN website mapping tool by selecting the hypopharynx, larynx, lip, oral cavity, nasopharynx and oropharynx cancer sites.
You May Like: Lobular Breast Cancer Stage 3
Selecting Focal Somatic Copy Number Alterations
We filtered the segmented copy number data by amplitude and level of support to create a short list of focal amplifications or deletions. Specifically, we selected amplicons with log2 values above 0.9 or deep deletions with log2 values below 1 We also required these segments to have at least 20 supporting probes. We then required amplicons to show evidence of allelic imbalance data to further remove technical artifacts. Finally, we manually curated and have plotted the completed list . As part of our manual inspection, when there was more than one gene within a copy number alteration, we nominated the gene we suspected to be the driver of each copy number event. For each gene that was nominated, we revisited copy number data from other samples and identified some additional examples that were previously missed with our filtering criteriafor example, we identified an extremely focal deletion of CDKN2A that was not supported by 20 probes. The supporting data for each copy number alteration, highlighted in this manuscript, are shown in Supplementary Figs. and .
High Intratumor Genetic Heterogeneity Is Related To Worse Outcome In Patients With Head And Neck Squamous Cell Carcinoma
Department of Otolaryngology, University of Pittsburgh Cancer Institute, Pittsburgh, Pennsylvania
Department of Radiation Oncology, University of Pittsburgh Cancer Institute, Pittsburgh, Pennsylvania
Department of Immunology, University of Pittsburgh Cancer Institute, Pittsburgh, Pennsylvania
Center for Cancer Research and Department of Surgery, Massachusetts General Hospital, Boston, Massachusetts
Department of Otolaryngology, Massachusetts Eye and Ear Infirmary, Harvard Medical School, Boston, Massachusetts
Corresponding author
Department of Otolaryngology, University of Pittsburgh Cancer Institute, Pittsburgh, Pennsylvania
Department of Radiation Oncology, University of Pittsburgh Cancer Institute, Pittsburgh, Pennsylvania
Department of Immunology, University of Pittsburgh Cancer Institute, Pittsburgh, Pennsylvania
Center for Cancer Research and Department of Surgery, Massachusetts General Hospital, Boston, Massachusetts
Department of Otolaryngology, Massachusetts Eye and Ear Infirmary, Harvard Medical School, Boston, Massachusetts
Corresponding author
Also Check: Metastatic Basal Cell Carcinoma Survival Rate
Sample Collection P16 Staining And Dna Extraction
Ethical approval for this study was granted by the UCL/UCLH Ethics Committee with informed consent obtained where required. Based on the results of a power analysis and taking into account gender and age-matching requirements we selected 20 HPV+ and 20 HPV- oropharyngeal carcinomas , all formalin fixed paraffin-embedded . Our power analysis suggested that by choosing the described number of samples there was a just under 90% chance of detecting moderate differences in the proportion of mutations between HPV+ and HPV- HNSCC samples .
Table 1 Patient characteristics of selected HPV+ and HPV- HNSCC samples.Figure 1
Workflow of FFPE sample preparation and selection. Eighty-two FFPE blocks were stained for p16 of which eight samples were excluded from further analysis, showing mixed p16 staining. Eight samples were excluded after the LCM step, yielding insufficient amounts or quality of DNA and two further samples were excluded due to inconsistent or borderline results in repeat E6 qPCR measurements. In total, 22 confirmed HPV+ and 34 HPV- samples were suitable for further analysis. Following age and gender matching, 20 HPV+ HNSCC samples and 20 HPV- HNSCC samples were then selected for the final analysis sequencing).
Tp53 And Cdkn2a/rb1 Genes
TP53 mutations are the most frequently identified somatic mutations in SCCs from all body sites . Missense âhot spotsâ mutations are very common, which result in dominant negative and/or gain-of-function properties through three possible mechanisms . The first relates to the tetramer complex formation of p53 and its ability to interact, in either wild type or mutated forms, with the two other family members, p63 and p73, affecting their function. The second involves modulation of gene expression by mutant p53 mediated by its association with other transcriptional factors. The third results from altered DNA binding specificity of mutant p53. As a result, a whole range of deregulated genes has been identified with pro-survival, pro-invasive and pro-tumorigenic functions . The different impact on tumorigenesis of missense versus loss of function TP53 mutations is best appreciated in mouse models, with âknock-inâ missense mutations resulting in a shift towards epithelial-derived cancers ).
Suppression of p105-Rb activity by loss-of-function mutations of the CDK inhibitor CDKN2A is also very common in SCCs, while mutations of the RB1 gene itself have been found less frequently except in ESCC . Interestingly, putative cancer driver mutations in many genes including TP53 are already frequent in normal photo-exposed skin, with the notable exception of CDKN2A mutations, suggesting that these may be a critical trigger of cancer development .
Don’t Miss: Does Amelanotic Melanoma Blanch When Pressed
Supplementary Figure 3 Substitution Composition Of Smokers And Non
Comparison of the average substitution rates at non-CpG dinucleotides and at CpG dinucleotides between smokers and non-smokers. Most of the excessive substitution of C> T over C> A/G occurred at CpG dinucleotides. Comparison of the average rates of all possible single-base substitutions between ESCC smokers and non-smokers . Error bars indicate s.e.m. No significant difference was found between smokers and non-smokers.
Clinical Presentation Of Skin Cancers
While the appearance of any one skin cancer can vary, there are general physical presentations that can be used in screening. BCCs most commonly have a pearly rim or can appear somewhat eczematous . They often ulcerate . SCCs frequently have a thick keratin top layer . Both BCCs and SCCs are associated with a history of sun-damaged skin. Melanomas are characterized by dark pigment with asymmetry, border irregularity, color variation, a diameter of more than 6 mm, and evolution . Photographs representing typical clinical presentations of these cancers are shown below.
Basal cell carcinomas
Squamous cell carcinomas
Melanomas
References
Recommended Reading: Carcinoma Cancer Symptoms
Initiating And Early Events
HPV-negative HNSCC.
Tobacco consumption is the primary risk factor for development of HPV-negative HNSCC. Tobacco consists of over 5,000 different chemicals, of which dozens have been shown to have carcinogenic activity. The chemicals thought to be most responsible for the cancer-causing effects of tobacco are polycyclic aromatic hydrocarbons , including benzopyrene, and nitrosamines, including 4–1–1-butanone and N-nitrosonornicotine ,. In smokeless tobacco, nitrosamines are the dominant carcinogen, whereas the carcinogens in areca nut and betel quid are poorly defined. Tobacco-derived carcinogens, including PAHs and nitrosamines, undergo metabolic activation, with detoxication enzymes and pathways promoting excretion . However, many of the reactive metabolites of these carcinogens can also form covalent DNA adducts, which, if not properly repaired, lead to mutations and other genetic abnormalities. The propensity for tobacco carcinogens to promote genetic changes and neoplastic transformation likely depends on the balance between metabolic activation versus detoxification and DNA repair . The use of tobacco products is also associated with inflammation in the exposed tissues. Coincident with inflammation is the local production of cytokines, chemokines and growth factors that can have an important role in promoting proliferation, angiogenesis and, ultimately, carcinogenesis.
Development of carcinogen-associated, HPV-negative HNSCC.
HPV-positive HNSCC.
Supplementary Figure 6 Fat Gene Mutations And Loss Of Heterozygosity
Summary of somatic mutations affecting FAT1, FAT2 and FAT3 across different tumor types from COSMIC. Number in the parentheses indicates the number of cases sequenced. Inactivation of both alleles of FAT1 in two ESCC cases. Upper panel, SNP-array data showing FAT1 loss of heterozygosity in both tumors . Blue line, total gene dosage Green and red line, alleles-specific gene dosage. The number on the left indicates log2 tumor/reference ratio. Lower panel, Sanger sequencing signals confirmed the somatic mutations of FAT1 in both cases. Arrows indicate the beginning of frameshift mutation bases in tumor DNA and the corresponding bases in germline DNA.
Also Check: Basal Skin Cancer Survival Rates
Supplementary Figure 2 Intratumoral Clonality Analysis
Intratumoral clonality plots of four representative ESCC cases from Discovery Cohort. ESCC-D13, D15, D17 tumors were developed bi-clonaly whereas ESCC-D14 tumor showed multi-clonal structure. Variant allele frequency was calculated with copy-number neutral variants, which was further used to plot intratumoral clonal architectures.
What Are The Signs And Symptoms Of Squamous Cell Carcinoma Of Oral Cavity
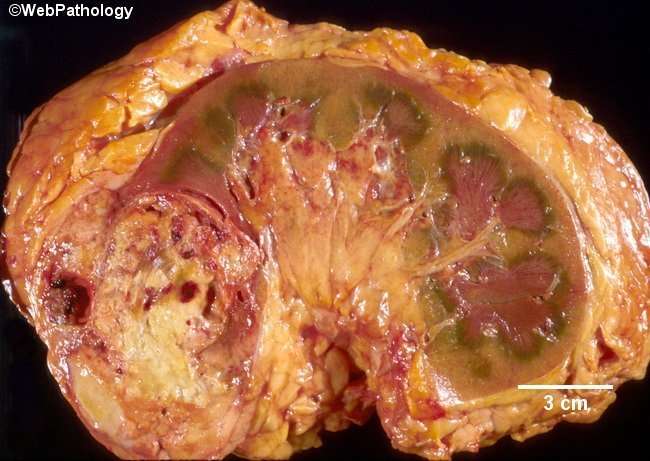
The signs and symptoms of Squamous Cell Carcinoma of Oral Cavity include:
- In majority of the cases, the condition is asymptomatic and does not present any signs or symptoms
- Generally, squamous cell carcinomas are slow-growing tumors though SCC of Oral Cavity is an aggressive form of cancer
- The mouth parts affected may include the cheek, hard and soft palate, gums, etc.
- The skin lesions may appear as crusted ulcer, plaques, and nodules
- It may ulcerate and bleed. Occasionally, after the ulcer heals, it may become ulcerated again
- The size of the lesions range from 1-10 cm average size is usually less than 3 cm
- Individuals with immunocompromised states have more aggressive tumors
- Due to the presence of the lesion on the oral mucosa, it may be difficult for the individual to consume food and drink. Also, speaking may be difficult and painful
Also Check: Stage 3 Basal Cell Carcinoma Survival Rate
What Causes Basal And Squamous Cell Skin Cancers
While many risk factors for basal and squamous cell skin cancers have been found, its not always clear exactly how these factors might cause cancer.
Most basal cell and squamous cell skin cancers are caused by repeated and unprotected skin exposure to ultraviolet rays from sunlight, as well as from man-made sources such as tanning beds.
UV rays can damage the DNA inside skin cells. DNA is the chemical in each of our cells that makes up our genes, which control how our cells function. We usually look like our parents because they are the source of our DNA. But DNA affects more than just how we look.
Some genes help control when our cells grow, divide into new cells, and die:
- Genes that help cells grow, divide, and stay alive are called oncogenes.
- Genes that keep cell growth in check by slowing down cell division or causing cells to die at the right time are called tumor suppressor genes.
Cancers can be caused by DNA changes that keep oncogenes turned on, or that turn off tumor suppressor genes. These types of gene changes can lead to cells growing out of control.
Researchers dont yet know all of the DNA changes that result in basal or squamous cell skin cancer, but they have found that in many skin cancers the cells have changes in tumor suppressor genes.
These are not the only gene changes that play a role in the development of skin cancer. There are many others as well.
Risk Factors For Basal Cell Carcinoma
This section focuses on risk factors in individuals at increased hereditary risk of developing BCC.
Sun exposure
Sun exposure is the major known environmental factor associated with the development of skin cancer of all types. There are different patterns of sun exposure associated with each major type of skin cancer .
Pigmentary characteristics
The high-risk phenotype consists of individuals with the following physical characteristics:
- Fair skin that sunburns easily.
- Lightly pigmented irides .
- Presence of freckles in sun-exposed skin.
- Poor ability to tan.
- Blond or red hair color.
Specifically, people with more highly pigmented skin demonstrate lower incidence of BCC than do people with lighter pigmented skin. Individuals with Fitzpatrick type I or II skin were shown to have a twofold increased risk of BCC in a small case-control study. Blond or red hair color was associated with increased risk of BCC in two large cohorts: the Nurses Health Study and the Health Professionals Follow-Up Study. In women from the Nurses Health Study, there was an increased risk of BCC in women with red hair relative to those with light brown hair . In men from the Health Professionals Follow-Up Study, the risk of BCC associated with red hair was not as large and was not significant after adjustment for melanoma family history and sunburn history. Risk associated with blond hair was also increased for both men and women , and dark brown hair was protective against BCC .
Family history
Also Check: Squamous Cell Carcinoma Scalp Prognosis
Risk Factors For Squamous Cell Carcinoma
Sun exposure and other risk factors
Sun exposure is the major known environmental factor associated with the development of skin cancer of all types however, different patterns of sun exposure are associated with each major type of skin cancer. Unlike basal cell carcinoma , SCC is associated with chronic exposure, rather than intermittent intense exposure to ultraviolet radiation. Occupational exposure is the characteristic pattern of sun exposure linked with SCC. Other agents and factors associated with SCC risk include tanning beds, arsenic, therapeutic radiation , chronic skin ulceration, and immunosuppression.
Characteristics of the skin
Like melanoma and BCC, SCC occurs more frequently in individuals with lighter skin than in those with darker skin. A case-control study of 415 cases and 415 controls showed similar findings relative to Fitzpatrick type I skin, individuals with increasingly darker skin had decreased risks of skin cancer . The same study found that blue eyes and blond/red hair were also associated with increased risks of SCC, with crude ORs of 1.7 for blue eyes, 1.5 for blond hair, and 2.2 for red hair.
Immunosuppression
Personal history of BCC, SCC, and melanoma skin cancers
Family history of squamous cell carcinoma or associated premalignant lesions
What Steps Can You Take To Protect Yourself
Even if youre not in a high risk category for skin cancer, its still important to take precautions to protect your skin from sun damage.
If skin cancer runs in your family, or if youre fair-skinned, you should take extra care to protect yourself from the sun.
Regardless of your risk factors, here are some precautions to take:
- Use a broad-spectrum sunscreen. This means the sunscreen has the ability to block both UVA and UVB rays.
- Use sunscreen with a high SPF. The American Academy of Dermatology recommends an SPF of 30 or higher.
- Reapply sunscreen frequently. Reapply every 2 hours or more often if youre sweating, swimming, or exercising.
- Limit your exposure to direct sunlight. Stay in the shade if youre outdoors, especially between 10 a.m. and 3 p.m, when the suns UV rays are strongest.
- Wear a hat. A wide-brimmed hat can provide extra protection for your head, face, ears, and neck.
- Cover up. Clothes can provide protection from the damaging rays of the sun. Wear light, loose-fitting clothing that allows your skin to breathe.
- Get regular skin check-ups. Get your skin screened every year by your doctor or dermatologist. Let your doctor know if you have a family history of melanoma or other skin cancers.
Also Check: How Do You Die From Melanoma