Treatment For Stage 0 Melanoma
The standard treatment for Stage 0 melanoma is surgery.
The purpose of the surgery is to remove any cancer remaining after the biopsy. This procedure is called a wide local excision. The surgeon removes any remaining tumor from the biopsy site, the surgical margin , and the underlying subcutaneous tissue, to make certain the whole tumor has been removed. This procedure may be done in a doctors office under local anesthetic. The width of the margin taken depends upon the thickness of the primary tumor. The surgical margin for in situ melanoma is 0.5 to 1.0 cm, based on National Comprehensive Cancer Network guidelines.
Melanoma In Situ Treatment Options
Fortunately, stage 0 melanomas are, most often, easy to treat because they are the least invasive when compared to the other stages of melanoma. Typically, all that is required is excision of the affected cells and surrounding healthy tissue this type of outpatient treatment is often found to be successful. Of note, however, repeated surgical treatment may be required until all margins of the area in concern are clear.
Excision may not be ideal in the cases of malignant melanoma in situ of the head and neck due to the risk of disfiguration. Researchers at the University of Connecticut Health Center and School of Medicine have reported that the use of the 5% strength topical cream, imiquimod, healed patients suffering from facial melanoma in situ. Thus, imiquimod was found to be an effective treatment without the normal disfiguring results of excision.
A Healthy Diet May Prevent Melanoma Recurrence
IF YOURE Amelanoma survivor, you know that early detection and treatment are critical, since the five-year-survival rate for people with melanoma thats detected early is about 98 percent, according to the Skin Cancer Foundation. In addition to watching your sun exposure, you can decrease your risk of developing skin cancer or its recurrence through healthy eating. Here, the best foods to reach for
Read Also: Invasive Ductal Carcinoma Breast Cancer Survival Rates
Stage I And Stage Ii Melanoma
Stage I and stage II melanoma describe invasive cancer that has grown below the epidermis to the next layer of skin, the dermis. It has not reached the lymph nodes.
Two major factors help determine the seriousness of stage I melanoma and stage II melanoma: Breslow depth and ulceration.
Breslow depth is a measurement that doctors use to describe the depth of an invasive melanoma in millimeters. It measures how far melanoma cells have reached below the surface of the skin. The thinner the melanoma, the better the chances for a cure.
Ulceration means that there is broken skin covering the melanoma. This breakage can be so small that it can only be seen under a microscope. Ulceration is an important factor in staging. A melanoma with ulceration may require more aggressive treatment than a melanoma of the same size without ulceration.
Melanoma is considered stage 1A when:
- the tumor is less than or equal to 1 millimeter thick in Breslow depth
Melanoma is considered stage IB when:
- the tumor is 1.1 to 2 millimeters thick in Breslow depth without ulceration
Melanoma is considered stage IIA when:
- the tumor is 1.1 to 2 millimeters thick in Breslow depth with ulceration
- the tumor is 2.1 to 4 millimeters thick in Breslow depth without ulceration
Melanoma is considered stage IIB when:
- the tumor is 2.1 to 4 millimeters thick in Breslow depth with ulceration
- the tumor is more than 4 millimeters in Breslow depth without ulceration
Melanoma is considered stage IIC when:
What Are The Clinical Features Of Melanoma In Situ
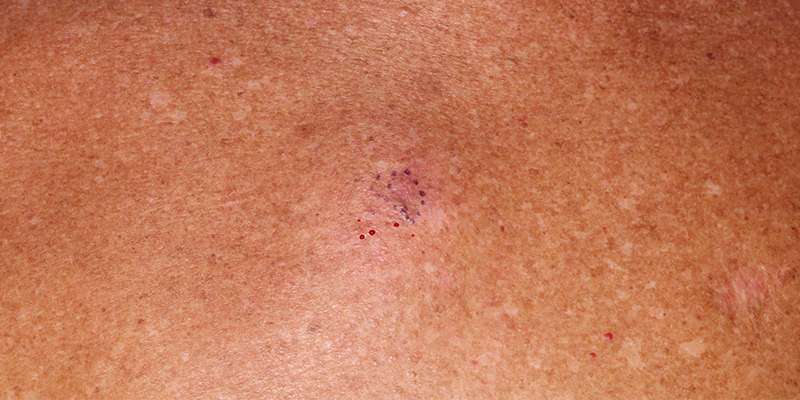
Typically, melanoma in situ is an irregular pigmentedpatch of skin. It often has the ABCDE criteria:
ABCDE
The body site and other clinical features of melanoma in situ depend on the subtype of melanoma . In general terms, melanoma in situ is macular . However, in about 8% of cases, melanoma in situ is thickened and can be scaly due to reactive thickening of the epidermis .
Also Check: Well Differentiated Squamous Cell Carcinoma Prognosis
There Are Different Types Of Cancer That Start In The Skin
There are two main forms of skin cancer: melanoma and nonmelanoma.
Melanoma is a rare form of skin cancer. It is more likely to invade nearby tissues and spread to other parts of the body than other types of skin cancer. When melanoma starts in the skin, it is called cutaneous melanoma. Melanoma may also occur in mucous membranes . This PDQ summary is about cutaneous melanoma and melanoma that affects the mucous membranes.
The most common types of skin cancer are basal cell carcinoma and squamous cell carcinoma. They are nonmelanoma skin cancers. Nonmelanoma skin cancers rarely spread to other parts of the body.
How To Protect Yourself From Melanoma
Fortunately, most melanomas are diagnosed in early, localized stages, says Dr. González, and most patients treated for melanoma make a full recovery. But we do have patients that have ignored that funny looking mole for way too long, and its not uncommon to see cases that have metastasized to other organs, she adds.
Melanoma tends to a very aggressive form of cancer, and it can progress quickly from one stage to another. Says Dr. González: As soon as you see something unusual you should get it checked out, and as soon as you get a diagnosis, you need to be on top of the appropriate treatment.
Risk factors for melanoma include ultraviolet light exposure , having fair skin and light hair, and having a close relative whos also had melanoma. But monitoring skin for abnormal growths and changes is important for everyone, whether or not they are predisposed to skin cancer.
Going to see your board-certified dermatologist yearly and doing regular skin exams may not seem that important, Dr. González says, “but these are the things that could save your life.”
Don’t Miss: Invasive Ductal Carcinoma Stage 3 Survival Rate
What Are The Signs Of Melanoma
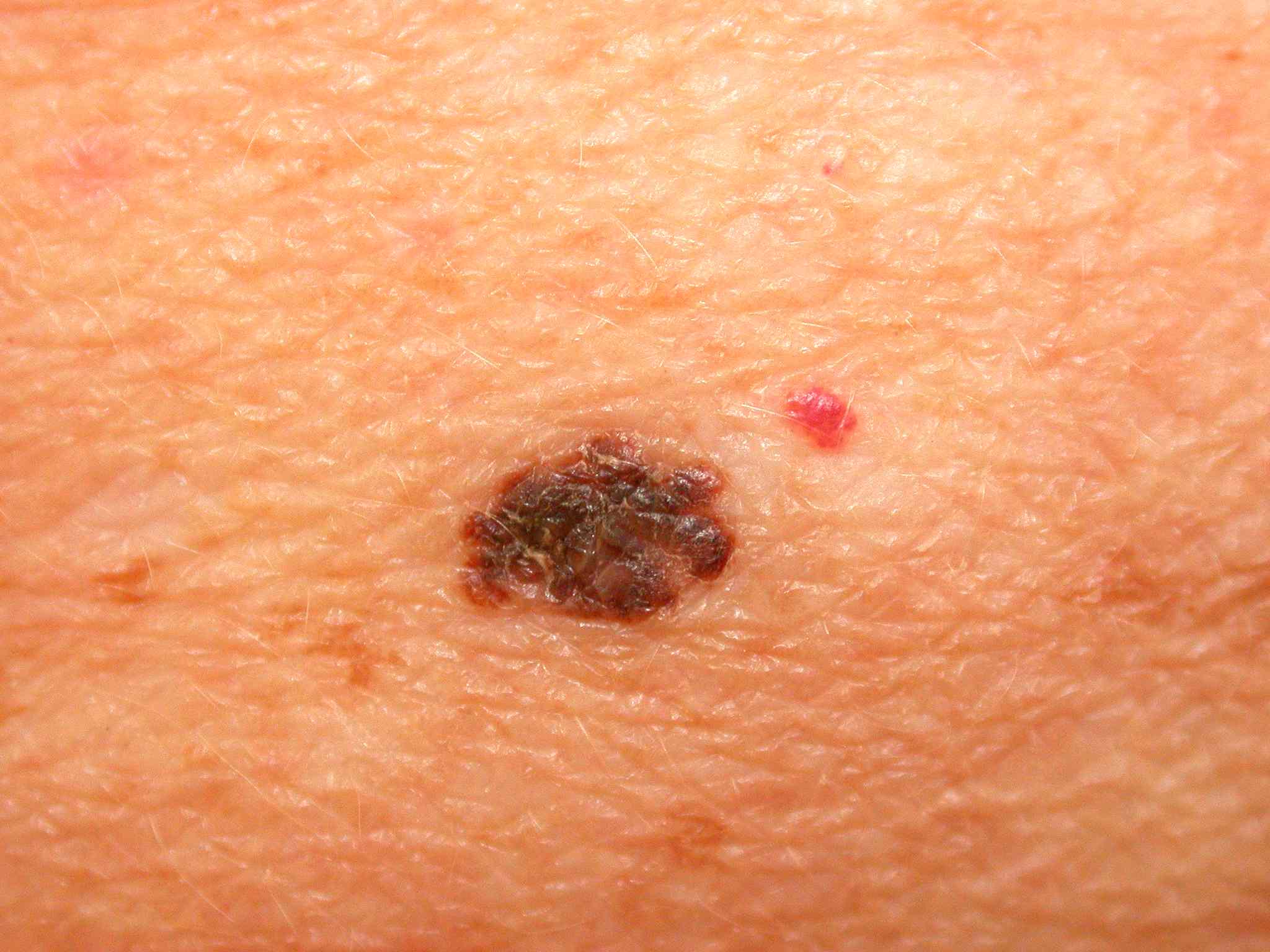
Knowing how to spot melanoma is important because early melanomas are highly treatable. Melanoma can appear as moles, scaly patches, open sores or raised bumps.
Use the American Academy of Dermatologys ABCDE memory device to learn the warning signs that a spot on your skin may be melanoma:
- Asymmetry: One half does not match the other half.
- Border: The edges are not smooth.
- Color: The color is mottled and uneven, with shades of brown, black, gray, red or white.
- Diameter: The spot is greater than the tip of a pencil eraser .
- Evolving: The spot is new or changing in size, shape or color.
Some melanomas dont fit the ABCDE rule, so tell your doctor about any sores that wont go away, unusual bumps or rashes or changes in your skin or in any existing moles.
Another tool to recognize melanoma is the ugly duckling sign. If one of your moles looks different from the others, its the ugly duckling and should be seen by a dermatologist.
Original Articlerisk Of Second Primary Cancer In Survivors Of In Situ Melanoma
Survivors of invasive melanoma have an increased risk of developing second primary cancers however, similar risks associated with in situ melanoma have not been established. We evaluated 39,872 survivors of first primary in situ melanoma diagnosed from 1982 through 2012 in Queensland, Australia. Relative risk of second nonmelanoma primary cancers was estimated from standardized incidence ratios with 95% confidence intervals. A total of 4,823 in situ melanoma survivors developed a second primary cancer. A small increased risk compared with the general population was found. In those younger than 50 years, risk was increased by 14% for all cancers combined. In situ melanoma survivors had significantly increased risks of developing lip, thyroid, pancreatic, and brain cancers and decreased risks of head and neck, and lung cancers. Male in situ melanoma survivors had a significantly increased risk of prostate cancer female survivors had an increased risk of thyroid cancer and lymphoid leukemia. Findings indicate that in situ melanoma may predict the diagnosis of certain second primary cancers. This altered risk may be due to biological, behavioral, or genetic factors or increased medical surveillance, and it requires further investigation, particularly among people younger than 50 years.
- Previous article in issue
Recommended Reading: Stage 2 Invasive Ductal Carcinoma Survival Rate
Dont Use Tanning Beds Or Sunlamps
Tanning equipment like tanning beds or lamps give off the same damaging UVA and UVB rays as the sun. As a result, people who use tanning equipment have at least a 20% increased risk of melanoma.
In Ontario, the Skin Cancer Prevention Act , 2013 banned the sale and marketing of tanning services to people under 18 years of age.
Medical Treatment For Skin Cancer
Surgical removal is the mainstay of skin cancer treatment for both basal cell and squamous cell carcinomas. For more information, see Surgery.People who cannot undergo surgery may be treated by external radiation therapy. Radiation therapy is the use of a small beam of radiation targeted at the skin lesion. The radiation kills the abnormal cells and destroys the lesion. Radiation therapy can cause irritation or burning of the surrounding normal skin. It can also cause fatigue. These side effects are temporary. In addition, topical chemotherapy creams have been FDA approved for the treatment of certain low-risk nonmelanoma skin cancers. Patients with advanced or many basal cell carcinomas are sometimes prescribed oral pills to block the growth of these cancers. Side effects include muscle spasms, hair loss, taste changes, weight loss and fatigue.
In advanced cases of melanoma, immune therapies, vaccines, or chemotherapy may be used. These treatments are typically offered as clinical trials. Clinical trials are studies of new therapies to see if they can be tolerated and work better than existing therapies.
Don’t Miss: Lobular Breast Cancer Survival Rates
What Will You Find On A Pathology Report
The report is broken down into a few sections including:
- Some information about the patient.
- Diagnosis if it is known.
- Procedure.
- Description of what the specimen looks like to the naked eye
- Description of what was seen under the microscope
- Where the tissue was taken from.
- Diagnosis of the biopsy.
The pathologist will describe the type of melanoma and some characteristics or features of it that are important for prognosis and treatment. To help you read your report, let’s go through what you may find in your report.
Type of Melanoma
Also called the histologic type or cellular type of melanoma. There are four major subtypes, with a few rare subtypes:
- Superficial Spreading Melanoma: most common of the melanomas.
- Nodular Melanoma: are always vertical growth phase present melanomas. Most commonly found on the chest, back, head or neck.
- Acral Lentiginous: most common type in dark skinned and Asian populations. More frequently occur on soles of feet, palms of hands or under nails.
- Lentigo Maligna Melanoma: tends to occur on sun-exposed areas in older people. Often found on the face or neck.
- Rare subtypes: mucosal melanoma, desmoplastic melanoma, nevoid melanoma
Breslow Depth Classification:
- Melanoma in situ or thin invasive tumors: less than 1.0mm in depth.
- Intermediate risk melanoma: 1mm – 4mm in thickness.
- High risk melanoma: greater than 4.0mm in depth.
Types of Biopsies :
Carcinoma In Situ Vs Cancer
A million-dollar question lately, especially with controversy over the treatment of ductal carcinoma in situ or in situ breast cancer, is whether or not carcinoma in situ is really cancer. The answer is that it depends on who you talk to. Some physicians classify carcinoma in situ as non-invasive cancer and others may prefer calling it pre-cancer. The distinction would lie in knowing whether or not the CIS would progress to invasive cancer, and that, by definition, is not known. Nor are we apt to get answers soon, as it wouldn’t be ethical to simply watch large numbers of carcinoma in situ’s to see if they became invasive cancer and spread.
Don’t Miss: Invasive Breast Cancer Survival Rate
What Is Squamous Cell Cancer
Squamous cell carcinoma of the skin is a common skin cancer that typically develops in chronic sun-exposed areas of your body. This type of skin cancer is usually not nearly as aggressive as melanoma and is uncontrolled growth of cells in the epidermis of your skin.
It can become disfiguring and sometimes deadly if allowed to grow. Squamous cell carcinomas are at least twice as frequent in men as in women. They rarely appear before age 50 and are most often seen in individuals in their 70s.
An estimated 700,000 cases of SCC are diagnosed each year in the United States, resulting in approximately 2,500 deaths.
Dont Miss: Can I Die From Skin Cancer
Scientists Discover Role For Vitamin D In Melanoma
A new study published in Cancer Research on November 6, 2019, from Cancer Research UK suggests that vitamin D may reduce the aggressive nature of melanoma cells, and improve survival rates.
Melanoma is a type of skin cancer that is deadly but relatively rare in the population. This aggressive disease accounts for the majority of deaths due to skin cancer. Each year 16,000 patients are newly diagnosed with melanoma each year in the UK, with about 300 of these being advanced-stage cancer.
With the advancement of treatment methods, the survival rate has doubled over the past 40 years. Despite this, advanced stage melanoma has a 1-year survival rate of just 55%, compared to almost 100% for those whose cancer is picked up very early
Melanoma patients often avoid sunlight, to prevent exposing their skin to solar ultraviolet rays, and are therefore at a higher risk of being vitamin D-deficient. Conversely, a higher level of vitamin D in the blood is linked to smaller tumors and better outcomes.However, the mechanism responsible for this finding is unknown
from Cancer Research UK pointed out that the National Health Service already advises that people take 10 micrograms of vitamin D every day to maintain good muscle and bone health, more particularly during winter when sunlight exposure is low.
Read Also: Stage 3 Invasive Ductal Carcinoma Survival Rate
Be Aware Of Products That Increase Sun Sensitivity
Some medications or products can make your skin more sensitive to the sun . When you start a new prescription, over-the-counter medication or herbal remedy, read the product information and talk with your pharmacist. Ask if this product has been reported to make people more sensitive to the sun. If it has, you should be careful to protect yourself whenever you are in the sun.
Transplant patients have special sun protection needs. You can learn more at the Kidney Foundation of Canada.
Recommended Reading: How To Identify Basal Cell Carcinoma
Characteristics Of Stage 0 Melanoma
Stage 0 melanoma is a tumor limited to the epidermis. There are no subgroups for Stage 0 melanoma. In the TNM system , its described as TisN0M0:
- Tis: means Tumorin situ cancer cells are found only in the outer layer of skin , not the second layer of skin
- N0: means melanoma has not spread to the lymph nodes
- M0: means melanoma has not spread to distant sites
Risk: Patients with Stage 0 melanoma are considered at very low risk for local recurrence or for regional and distant metastases.
- detect any evidence of the melanoma returning or spreading to other organs, and
- identify new melanomas.
If the original melanoma returns, it is likely to be in the first 1-2 years after diagnosis . People who have had a melanoma have an increased risk â as much as 5 to 10 fold â of developing a new melanoma in future. This increased risk persists lifelong .
The usual follow-up for a patient with melanoma in situ is:
- full body skin cancer check for melanoma and other skin cancers, plus examination of lymph nodes and abdomen for signs of spread: 6-monthly for two years, then 12-monthly for the next three years and then
- a full body skin cancer check for melanoma and other skin cancers every year for life .
Read Also: What Is The Survival Rate For Invasive Ductal Carcinoma
What Are The Melanoma Stages And What Do They Mean
Early melanomas
Stage 0 and I are localized, meaning they have not spread.
- Stage 0: Melanoma is localized in the outermost layer of skin and has not advanced deeper. This noninvasive stage is also called melanoma in situ.
- Stage I: The cancer is smaller than 1 mm in Breslow depth, and may or may not be ulcerated. It is localized but invasive, meaning that it has penetrated beneath the top layer into the next layer of skin. Invasive tumors considered stage IA are classified as early and thin if they are not ulcerated and measure less than 0.8 mm.
Find out about treatment options for early melanomas.
Intermediate or high-risk melanomas
Localized but larger tumors may have other traits such as ulceration that put them at high risk of spreading.
- Stage II: Intermediate, high-risk melanomas are tumors deeper than 1 mm that may or may not be ulcerated. Although they are not yet known to have advanced beyond the primary tumor, the risk of spreading is high, and physicians may recommend a sentinel lymph node biopsy to verify whether melanoma cells have spread to the local lymph nodes. Thicker melanomas, greater than 4.0 mm, have a very high risk of spreading, and any ulceration can move the disease into a higher subcategory of stage II. Because of that risk, the doctor may recommend more aggressive treatment.
Learn more about sentinel lymph node biopsy and melanoma treatment options.
Advanced melanomas
Questions To Ask Your Physician
Patients with melanoma of less than 1 millimeter should ask their physicians whether or not their melanoma demonstrated any evidence of ulceration, vertical growth phase, regression, or whether it is Clark level IV. Patients should also inquire about the treatment results achieved at the cancer center or institution where they are considering treatment.
Don’t Miss: How Long Until Melanoma Spreads
Precancer Or Noninvasive Cancer
Some physicians use the terms precancer and noninvasive cancer interchangeably when referring to stage 0 breast cancer, whereas others simply call it cancer. There is great debate over this, but generally, DCIS is considered cancer, while LCIS isnt .
Aside from clinical perspectives that shape their opinion on the proper terminology to use, some physicians consider how hearing cancer will affect a patient.
Learning that your condition is precancerous may make you worry that it will inevitably progress to cancer and that it must be treated as such . On the other hand, people told that they have a noninvasive cancer often lump their condition in with more advanced cases of the disease. In fact, some doctors refer to LCIS as lobular neoplasia simply because it sounds less frightening.
Dont be mistaken: Both DCIS and LCIS are concerning because they have the potential to invade beyond their well-contained sites. Both carcinomas have the cellular appearance of cancer and both might eventually grow and spread beyond their original clumps. But, they also might not. So far, doctors cant say which direction any particular case will go.
While stage 0 breast cancer should be taken seriously, the lower the stage number, the easier the disease is to treat.
Remember that all of these names for stage 0 breast cancer are just different ways to refer to the same thing. Dont get hung up on terms when deciding on treatment.