Melanoma Can Be Tricky
Identifying a potential skin cancer is not easy, and not all melanomas follow the rules. Melanomas come in many forms and may display none of the typical warning signs.
Its also important to note that about 20 to 30 percent of melanomas develop in existing moles, while 70 to 80 percent arise on seemingly normal skin.
Amelanotic melanomas are missing the dark pigment melanin that gives most moles their color. Amelanotic melanomas may be pinkish, reddish, white, the color of your skin or even clear and colorless, making them difficult to recognize.
Acral lentiginous melanoma, the most common form of melanoma found in people of color, often appears in hard-to-spot places, including under the fingernails or toenails, on the palms of the hands or soles of the feet.
The takeaway: Be watchful for any new mole or freckle that arises on your skin, a sore or spot that does not heal, any existing mole that starts changing or any spot, mole or lesion that looks unusual.
Acral lentiginous melanoma is the most common melanoma found in people of color.
Who Gets Skin Cancer And Why
Sun exposure is the biggest cause of skin cancer. But it doesn’t explain skin cancers that develop on skin not ordinarily exposed to sunlight. Exposure to environmental hazards, radiation treatment, and even heredity may play a role. Although anyone can get skin cancer, the risk is greatest for people who have:
- Fair skin or light-colored eyes
- An abundance of large and irregularly-shaped moles
- A family history of skin cancer
- A history of excessive sun exposure or blistering sunburns
- Lived at high altitudes or with year-round sunshine
- Received radiation treatments
When Melanoma Can’t Be Cured
If your cancer has spread and it is not possible to cure it by surgery, your doctor may still recommend treatment. In this case, treatment may help to relieve symptoms, might make you feel better and may allow you to live longer.
Whether or not you choose to have anti-cancer treatment, symptoms can still be controlled. For example, if you have pain, there are effective treatments for this.
General practitioners, specialists and palliative care teams in hospitals all play important roles in helping people with cancer.
Read Also: Invasive Ductal Carcinoma Stage 3 Survival Rate
A Primer On Skin Cancer
Malignant melanoma, especially in the later stages, is serious and treatment is difficult. Early diagnosis and treatment can increase the survival rate. Nonmelanoma skin cancers include basal cell carcinoma and squamous cell carcinoma. Both are common and are almost always cured when found early and treated. People who’ve had skin cancer once are at risk for getting it again they should get a checkup at least once a year.
Should People Have A Doctor Remove A Dysplastic Nevus Or A Common Mole To Prevent It From Changing Into Melanoma
No. Normally, people do not need to have a dysplastic nevus or common mole removed. One reason is that very few dysplastic nevi or common moles turn into melanoma . Another reason is that even removing all of the moles on the skin would not prevent the development of melanoma because melanoma can develop as a new colored area on the skin . That is why doctors usually remove only a mole that changes or a new colored area on the skin.
Don’t Miss: Cancer All Over Body Symptoms
What Is The Clark Level Of Invasion
The Clark level indicates the anatomic plane of invasion.
- Level 1: In situ melanoma
- Level 2: Melanoma has invaded the papillary dermis
- Level 3: Melanoma has filled the papillary dermis
- Level 4: Melanoma has invaded the reticular dermis
- Level 5: Melanoma has invaded the subcutaneous tissue
Deeper Clark levels have a greater risk of metastasis. It is useful in predicting outcome in thin tumours. It is less useful than Breslow thickness for thick tumours.
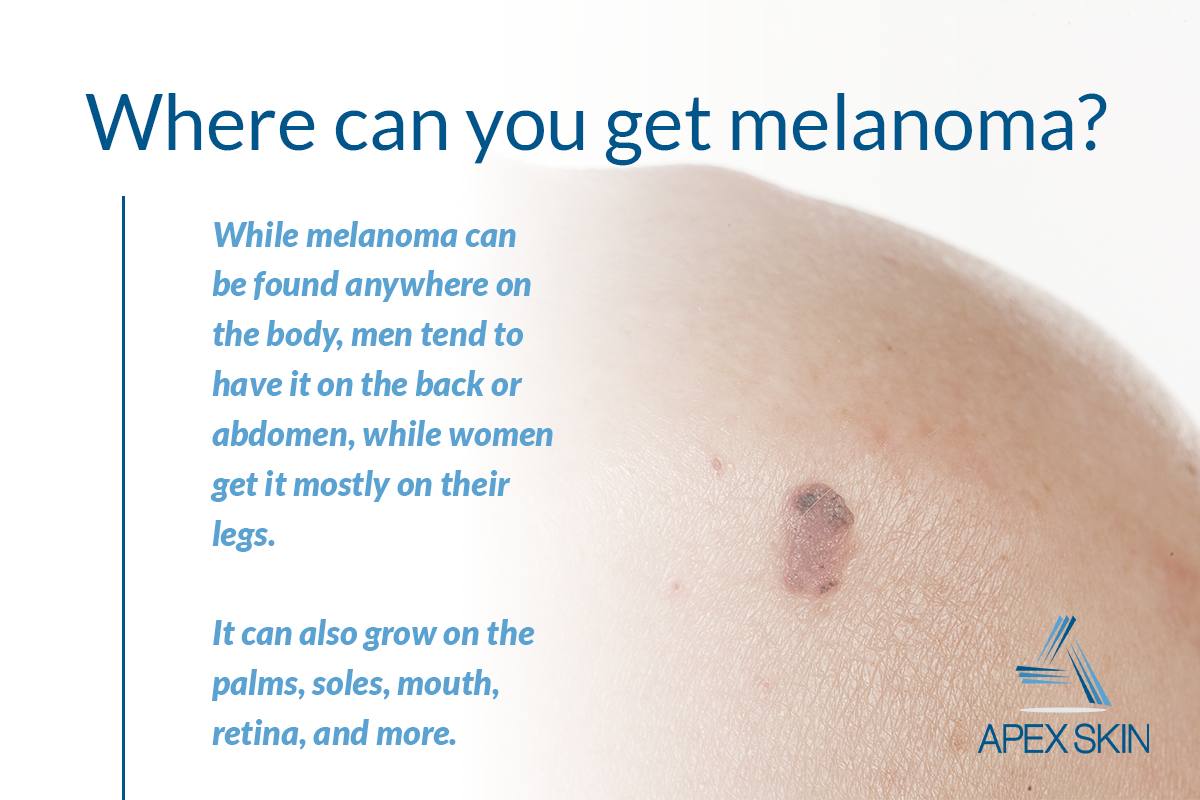
Okay We All Know That Black And Ugly Describes Melanoma And Online Images Show Melanoma To Be Evil
But we must also consider that often, by the time a melanoma is photographed by a dermatologist, its at a later stage of development.
Who spots a tiny innocent-looking dot, says to their doctor, Ive never seen this before, and the doctor decides to take a photo of it before excising it?
What more likely happens is that when what obviously appears to be a melanoma, with classic features, is presented to a dermatologist, the doctor THEN takes the photo. And it ends up onlinelooking mighty nasty.
Note that the dark pink melanoma in the lower left is quite round, symmetrical and all the same color.
In actuality, not all melanomasby the time theyre diagnosedare scary looking or have any of the classic features such as jagged edges and bumpy portions.
This one here below is relatively symmetrical, and keep in mind that its magnified which accentuates asymmetry in any lesion.
You May Like: Stage 1 Cancer Symptoms
What Should People Do If They Have A Dysplastic Nevus
Everyone should protect their skin from the sun and stay away from sunlamps and tanning booths, but for people who have dysplastic nevi, it is even more important to protect the skin and avoid getting a suntan or sunburn.
In addition, many doctors recommend that people with dysplastic nevi check their skin once a month . People should tell their doctor if they see any of the following changes in a dysplastic nevus :
- The color changes.
- It gets smaller or bigger.
- It changes in shape, texture, or height.
- The skin on the surface becomes dry or scaly.
- It becomes hard or feels lumpy.
- It starts to itch.
- It bleeds or oozes.
Another thing that people with dysplastic nevi should do is get their skin examined by a doctor . Sometimes people or their doctors take photographs of dysplastic nevi so changes over time are easier to see . For people with many dysplastic nevi, doctors may conduct a skin exam once or twice a year because of the moderately increased chance of melanoma. For people who also have a family history of melanoma, doctors may suggest a more frequent skin exam, such as every 3 to 6 months .
Get To Know Your Skin
The sooner a skin cancer is identified and treated, the better your chance of avoiding surgery or, in the case of a serious melanoma or other skin cancer, potential disfigurement or even death.
It is also a good idea to talk to your doctor about your level of risk and for advice on early detection.
It’s important to get to know your skin and what is normal for you, so that you notice any changes. Skin cancers rarely hurt and are much more frequently seen than felt.
Develop a regular habit of checking your skin for new spots and changes to existing freckles or moles.
Also Check: How Long Does It Take Melanoma To Metastasize
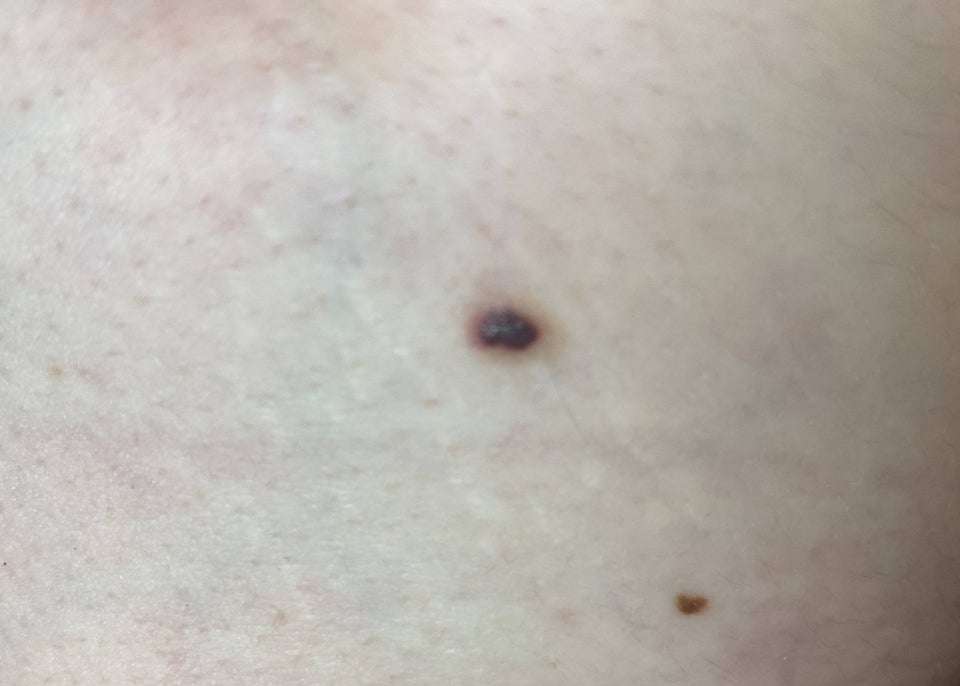
Answer: Sounds Like You’re In Luck
here’s the good news…tiny moles the size of a pin prick are overwhelmingly okay…in fact the likelihood of a melanoma in something this size is almost nil…change can be due to any number of issues…if something is only 1-2 millimeters in diameter, I’d do nothing other than watch it for further changes…an old adage that’s generally correct is that pigmented spots smaller than the diameter of a pencil eraser are not melanoma…the spot may not even be a mole…might be a small blood vessel…no harm in seeing a doctor if you’re worried or if it continues to change…but overwhelmingly nothing to worry about…
Possible Signs And Symptoms Of Melanoma
The most important warning sign of melanoma is a new spot on the skin or a spot that is changing in size, shape, or color.
Another important sign is a spot that looks different from all of the other spots on your skin .
If you have one of these warning signs, have your skin checked by a doctor.
The ABCDE rule is another guide to the usual signs of melanoma. Be on the lookout and tell your doctor about spots that have any of the following features:
- A is for Asymmetry: One half of a mole or birthmark does not match the other.
- B is for Border:The edges are irregular, ragged, notched, or blurred.
- C is for Color:The color is not the same all over and may include different shades of brown or black, or sometimes with patches of pink, red, white, or blue.
- D is for Diameter:The spot is larger than 6 millimeters across , although melanomas can sometimes be smaller than this.
- E is for Evolving: The mole is changing in size, shape, or color.
Some melanomas dont fit these rules. Its important to tell your doctor about any changes or new spots on the skin, or growths that look different from the rest of your moles.
Other warning signs are:
- A sore that doesnt heal
- Spread of pigment from the border of a spot into surrounding skin
- Redness or a new swelling beyond the border of the mole
- Change in sensation, such as itchiness, tenderness, or pain
- Change in the surface of a mole scaliness, oozing, bleeding, or the appearance of a lump or bump
Read Also: Basaloid Tumor
The Abcdes Of Melanoma
To help people find a possible melanoma on their skin, dermatologists created the ABCDEs of melanoma:
| A is for Asymmetry |
If you find a spot on your skin that has any of the ABCDEs of melanoma, see a board-certified dermatologist for a skin exam.
The following pictures can help you see how the ABCDEs of melanoma can appear on the skin.
How Common Is It
Overall, skin cancers are the most common cancers in the United States. But melanoma is less common than the other two major types, basal cell and squamous cell carcinoma.
Each year about 91,000 people in the U.S. are diagnosed with melanoma of the skin, according to the American Cancer Society. By comparison, about 3.3 million are diagnosed with one or more basal cell or squamous cell carcinomas.
Read Also: Is Melanoma Cancer Curable
Tools That Can Help You Find Melanoma On Your Skin
To help you find melanoma early, the American Academy of Dermatology developed the following:
Melanoma can look different on a childs skin. Taking this short quiz can help you hone your skills at finding childhood melanoma.
ImagesImages 1,3,4,5,6,7,8,10: Images used with permission of the American Academy of Dermatology National Library of Dermatologic Teaching Slides.
Image 2: Developed by the American Academy of Dermatology
Image 9: Used with permission of the Journal of the American Academy of Dermatology.
ReferencesBarnhill RL, Mihm MC, et al. Malignant melanoma. In: Nouri K, et al. Skin Cancer. McGraw Hill Medical, China, 2008: 140-167.
Gloster HM Jr, Neal K. Skin cancer in skin of color. J Am Acad Dermatol 2006 55:741-60.
National Comprehensive Cancer Network. NCCN guidelines for patients: Melanoma. 2018. Last accessed February 12, 2019.
Early Warning Signs Of Melanoma
The key to detecting melanoma early is to know what to look for and where to look for it. This isnt always easy, as melanoma can be a master of disguise. It may look like an age spot, a bruise, a sore, a cyst, a scar or a dark line beneath your nail. You may not feel a melanoma, but there are times that it may itch, hurt or bleed.
The ABCDE method may help you determine whether an abnormal skin growth may be melanoma:
- A is for asymmetry: Does the mark look different on each half?
- B is for border: Are the edges jagged or irregular?
- C is for color: Is your lesion uneven in color with specks of black, brown and tan?
- D is for diameter: Is your lesion getting larger?
- E is for evolving or elevation: Has your lesion changed in size, shape or texture over the past few weeks or months?
If the answer to any of these questions is yes, or even maybe, see a dermatologist for a proper evaluation. The only way to be sure whether a mole is melanoma is to visit a doctor.
Other melanoma warning signs may include:
- Sores that dont heal
- Pigment, redness or swelling that spreads outside the border of a spot to the surrounding skin
- Itchiness, tenderness or pain
Read Also: Stage 5 Cancer Symptoms
What Is Recurrent Melanoma
Recurrent melanoma refers to a recurrence of tumor at the site of removal of a previous tumor, such as in, around, or under the surgical scar. It may also refer to the appearance of metastatic melanoma in other body sites such as skin, lymph nodes, brain, or liver after the initial tumor has already been treated. Recurrence is most likely to occur within the first five years, but new tumors felt to be recurrences may show up decades later. Sometimes it is difficult to distinguish recurrences from new primary tumors.
What Are The Survival Rates For Metastatic Melanoma
Survival rates for melanoma, especially for metastatic melanoma, vary widely according to many factors, including the patient’s age, overall health, location of the tumor, particular findings on the examination of the biopsy, and of course the depth and stage of the tumor. Survival statistics are generally based on 5-year survival rates rather than raw cure rates. Much of the success reported for the targeted therapies focuses on disease-free time because in many cases the actual 5-year survival is not affected. It is hoped that combination therapy discussed above will change that.
- For stage 1 , 5-year survival is ⥠90%.
- For stage 2 , 5-year survival is 80%-90%.
- For stage 3 , 5-year survival is around 50%.
- For stage 4 , 5-year survival is 10%-25% depending upon sex and other demographic factors.
Recommended Reading: In Situ Cancer Melanoma
What Are The Signs Of Symptoms Of Metastatic Melanoma
Signs and symptoms depend upon the site of metastasis and the amount of tumor there. Metastases to the brain may first appear as headaches, unusual numbness in the arms and legs, or seizures. Spread to the liver may be first identified by abnormal blood tests of liver function long before the patient has jaundice, a swollen liver, or any other signs of liver failure. Spread to the kidneys may cause pain and blood in the urine. Spread to the lungs may cause shortness of breath, other trouble breathing, chest pain, and continued cough. Spread to bones may cause bone pain or broken bones called pathologic fractures. A very high tumor burden may lead to fatigue, weight loss, weakness and, in rare cases, the release of so much melanin into the circulation that the patient may develop brown or black urine and have their skin turn a diffuse slate-gray color. The appearance of multiple blue-gray nodules in the skin of a melanoma patient may indicate widespread melanoma metastases to remote skin sites.
Can You Have Melanoma For 3 Years And Not Know
How long can you have melanoma and not know it? It depends on the type of melanoma. For example, nodular melanoma grows rapidly over a matter of weeks, while a radial melanoma can slowly spread over the span of a decade. Like a cavity, a melanoma may grow for years before producing any significant symptoms.
Also Check: Melanoma Braf Positive
Brown Spots And Freckles
Freckles are small flat brown marks that most often appear on the face and other exposed parts of the body in the summer months. They are most often seen in fair-skinned people with red hair but can be seen in people with darker skin colour too. Freckles are formed when the skin is exposed to the sun. Freckles are harmless, but if one starts to look funny compared to others then its best to get it checked out.
Larger, flat, brown spots on the face and hands that start to appear in middle-aged people, known as age spots or liver spots, are properly called solar lentigines. These occur in people of all skin types if they have spent too much time exposed to the sun. Solar lentigines are harmless too but because they can sometimes turn into melanoma it is good to get them checked out, especially if they start to change colour or shape.
What If The Skin Changes Are Rapid Or Dramatic
Guideline # 4: The more rapid and dramatic the change, the less serious the problem.
When changes such as pain, swelling, or even bleeding come on rapidly, within a day or two, they are likely to be caused by minor trauma, often a kind one doesn’t remember . If a spot changes rapidly and then goes back to the way it was within a couple of weeks, or falls off altogether, it is not likely to represent anything serious. Nevertheless, this would be a good time to say once again: Nobody can diagnose him- or herself. If one sees a spot that looks as though it is new or changing, show it to a doctor. If one see a spot that doesn’t look like one’s other spots, it should be evaluated.
Also Check: Nodulo Infiltrative Basal Cell Carcinoma
What Are The Causes And Risk Factors For Melanoma
Guideline # 5: Individual sunburns do raise one’s risk of melanoma. However, slow daily sun exposure, even without burning, may also substantially raise someone’s risk of skin cancer.
Factors that raise one’s risk for melanoma include the following:
- Caucasian ancestry
- Fair skin, light hair, and light-colored eyes
- A history of intense, intermittent sun exposure, especially in childhood
- Many moles
- Large, irregular, or “funny looking” moles
- Close blood relatives — parents, siblings, and children — with melanoma
The presence of close family with melanoma is a high risk factor, although looking at all cases of melanoma, only 10% of cases run in families.
Having a history of other sun-induced skin cancers raises one’s risk of melanoma because they are markers of long-term sun exposure. The basic cell type is different, however, and a basal cell or squamous cell carcinoma cannot “turn into melanoma” or vice versa.
It is no longer recommended to do large batteries of screening tests on patients with thin, uncomplicated melanoma excisions, but patients who have had thicker tumors diagnosed or who already have signs and symptoms of metastatic melanoma may need to have MRIs, PET scans, CT scans, chest X-rays, or other X-rays of bones when there is a concern of metastasis.
The biopsy report may show any of the following:
In general, early localized melanoma is treated by surgery alone.