The Importance Of Keeping The Promise And Potential Of Immunotherapy Alive
Almost 40 percent of men and women will be diagnosed with cancer during their lifetime. Thankfully, in this day of medical advancements and innovation, cancer is no longer a certain death sentence. More than 15.5 million people lived beyond a cancer diagnosis as of Jan. 1, 2016, and that number is expected to surpass 20 million by 2026. The goal in cancer treatment now is to target care more precisely to patients through individualized health care. This is called precision medicine, and it is an especially welcome change for cancer patients who traditionally have been exposed to treatment such as chemotherapy and radiation that attacks their cancer but often damages healthy tissue in the process.
Precision medicine is at the heart of immunotherapy, currently one of the hottest areas of cancer research. Immunotherapy is a new approach that harnesses the power of our immune systems to identify and control diseases such as cancer. Immunotherapy is being studied in just about every type of cancer. The number of cancers successfully treated by immunotherapy stands at 15 and growing and includes skin, lung, kidney and bladder cancers.
As You Combine More Therapies Are Side Effects Increasing
There can be increased side effects including the onset of diabetes, inflammatory arthritis and other serious conditions, even death. Steroids and other treatments usually help avoid serious consequences and the hope is that as researchers learn more, they can inhibit signals on cells that cause damage.
What Are Immune Checkpoint Inhibitors
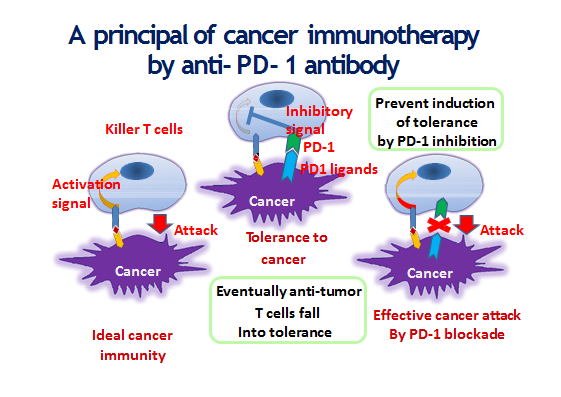
Most of the time, cancer cells bump into the immune system at locations called checkpoints, or PD-1 and PD-L1 receptorsmuch as if they were driving down the street and a policeman stopped them to make sure theyre allowed in that area of town.
When they arrive at these checkpoints, cancer cells simply show their ID badges and evade the immune system. What immune checkpoint inhibitors do is get in the way of that interaction. They help your immune system recognize that, in fact, that cancer cell is not a normal lung cell, and it needs to be eliminated.
Checkpoint inhibitors block;the signal between lung cancer cells and your immune cells thats interfering with your body’s ability to identify cancer cells as harmful. This triggers an immune response that causes the body to immediately release T-cells to attack and destroy the cancer cells.
Common checkpoint inhibitors used to treat lung cancer include:
- Pembrolizumab
- Nivolumab This checkpoint inhibitor is sometimes used in combination with another immune drug called ipilimumab
- Atezolizumab
- Durvalumab
Recommended Reading: How To Treat Melanoma Under Toenail
Immunotherapy For Lung Cancer: Unleashing The Power Of The Immune System
Immunotherapy is used to treat many forms of cancer, including lung cancer. Its goal is simple: to teach your body’s immune system to recognize and fight cancer cells.
More conventional treatments, such as chemotherapy and radiation therapy, attack lung cancer cells in ways that risk affecting both cancerous and healthy cells alike. Immunotherapy, on the other hand, helps your body fight cancer using its natural defenses, which means it has the potential to be a more effective treatment option, sometimes controlling the disease for years.
Patients diagnosed with lung cancer frequently come to us wondering whether this new treatment is the magic pill they’ve read or heard about and whether itll work for them. What we say to them is that immunotherapy has been shown to take an active cancer and turn it into a controllable disease for some patients, but it doesnt work for everyone.
That’s because lung cancers vary from person to person. The appropriate treatment for a patient depends on the type, stage, molecular characteristics and aggressiveness of each particular lung cancer, and whether the disease has metastasized to other areas of the body.
With that in mind, this article answers questions about immunotherapy for lung cancer, including:
A Sense Of Empowerment

Our online research of melanoma yielded an interesting fact. A series of new treatments had gone through clinical trials and been approved by the U.S. Food and Drug Administration for the treatment of metastatic melanoma. They were called immunotherapy drugs, and they were showing amazing results in certain people with melanoma, including former U.S. President Jimmy Carter. We had no idea whether I would benefit from these drugs or if my insurance would pay for them, but we kept hearing more about their successes in both clinical trials and the real world.;
The moment I was approved for treatment with nivolumab and ipilimumab was when hope came alive for Elvira and me. We had never really lost hope, but we knew the odds were stacked against us. Now, we felt that I had a chance against this diagnosis.
Immunotherapy is so powerful because it does not fight the cancer directly. Instead, it prompts the patients own immune system to recognize and destroy the cancer cells. Once those drugs were coursing through my system, my immune system was actually doing the hard work. It was incredibly empowering to realize that my own body was no longer a bystander in my cancer treatment.; It was working with a singular purpose: to rid my body of cancer cells.
Also Check: How Fast Does Melanoma Develop
Should I Try Immunotherapy
This type of treatment isn’t right for everyone. It doesn’t work on all types of cancer. And if surgery, radiation, or chemotherapy has stopped your cancer from growing, you might not need it.
Immunotherapy might be for you if it’s approved for your cancer. Even if it isn’t, you still might be able to get it in a clinical trial if your first treatments didn’t work. Ask your doctor if any trials are testing out new immunotherapy treatments for your cancer type.
Here are questions to ask your doctor to decide if itâs right for you:
- Are any immunotherapy treatments approved for my cancer?
- If not, are any clinical trials testing these treatments for my cancer?How might it help my cancer?
- Will I get it alone or with other treatments?
- How will I get it ?
- How often will I need it?
- What kinds of side effects can it cause?
- For how long will I need to take it?
- What happens if it doesn’t work?
Make sure you understand how it might help you and what side effects it can cause before you start treatment.
Sentinel Lymph Node Biopsy
A;sentinel lymph node biopsy is a procedure to test for the spread of cancer.
It may be offered to people with stage 1B to 2C melanoma. It’s done at the same time as surgical excision.
You’ll decide with your doctor whether to have a sentinel lymph node biopsy.
If you decide to have the procedure;and the results show no spread to nearby lymph nodes, it’s unlikely you’ll have further problems with this melanoma.
If the results confirm melanoma has spread to nearby nodes, your specialist will discuss with you whether further surgery is required.
Additional surgery involves removing the remaining nodes, which is known as a lymph node dissection or completion lymphadenectomy.
Recommended Reading: How Quickly Can Melanoma Appear
How Are They Treated
For most people, steroids can help manage the symptoms and not stop the drugs from working. Topical corticosteroid creams and oral antihistamines can often give quick relief for skin symptoms. Over-the-counter treatments should work for mild diarrhea as well.
High-test steroids like prednisolone or other drugs that suppress your immune system are also the choice to treat most other problems, which you may hear your doctor refer to as adverse events, or AEs.
In addition to steroids, you might have to take permanent hormone supplements after being on this type of treatment. If the symptoms are too severe, your doctor may pause your treatment for a while. But if you have a life-threatening reaction, youâll need to stop treatment.
What Are The Benefits Of Immunotherapy
Key benefits of immunotherapy over conventional therapies, such as chemotherapy and radiation, include:
- Fewer immediate and long-term side effects
- The ability to continue treatment on a long-term basis while maintaining good quality of life
Conventional therapies may cure some cancers, but they may also cause difficult, long-term side effects, like peripheral neuropathy, heart problems, surgical complications, lung damage, hormone dysfunction and memory and cognition problems. Eventually, standard therapies may also compromise or overpower the immune system.
Cancer immunotherapy, on the other hand, may have fewer immediate and long-term side effects. The most common immunotherapy side effects;patients may experience while receiving treatment include:
- Diarrhea
- Rash
- Autoimmune response
If you experience a side effect from immunotherapy, we may be able to treat it directly, or we may delay your next treatment to allow you some time to recover. Supportive care therapies may also help you manage side effects. Occasionally, steroids may be used to suppress the reaction. If the reaction involves a severe autoimmune response, you may have to discontinue immunotherapy.
Recommended Reading: How Basal Cell Carcinoma Is Treated
How Is Immunotherapy Administered
Patients usually receive immunotherapy treatment at an outpatient oncology center via infusion through a port or intravenous therapy . The dosage and frequency depend on the specific medicine. Therapy intervals may range between every two weeks to every four weeks. In April, however, the FDA approved a six-week dosing regimen for the immunotherapy drug, pembrolizumab , a monoclonal antibody.
Currently, theres no designated end to immunotherapy treatment. You may continue on the regimen as long as you continue to have a good response.
Patients sometimes ask to take a break from treatment. They may be experiencing side effects or want a break for a personal reason. When that happens, we monitor the patient with scans and tests every three months or so. We dont fully understand why yet, but somenot allcontinue to have a good response after stopping therapy. One possibility is that for those patients, immunotherapy may work like a light switch: Once its been turned on, it stays on.
For example, one recent study showed patients with PD-L1expressing advanced nonsmall-cell lung cancer who were treated for at least two years with pembrolizumab continued to experience long-term benefits of treatment, even after taking a break from treatment. Researchers and oncologists are trying to figure out who may be able to stop immunotherapy indefinitely and still maintain the benefits.
What Are The Benefits Of Immunotherapy Treatment For Lung Cancer Patients
When patients ask me what the benefits of immunotherapy for lung cancer are, I usually answer with another question: What better way to help your body get back to health from cancer than using your own natural defenses?
Teaching your body’s immune system to recognize and destroy cancer cells is a less toxic way of treating lung cancer, one that has a lower chance of harming healthy cells.
Another benefit of immunotherapy is that it can, for some patients, be kept up for a long time. Patients who see good results fighting their lung cancer with immunotherapy can sometimes continue receiving the treatment for years with fewer immediate and long-term side effects than those experienced by patients undergoing conventional therapies
In some instances, patients stop immunotherapy for a time, and when we perform periodic computed tomography scans, we see no sign of cancer cell activity or growth. This happens for a small percentage of immunotherapy patients, but it does happen. In other cases, while the cancer might not go away forever, immunotherapy may help keep it under control.
Don’t Miss: What Types Of Skin Cancer Are There
Study Sets A New Standard For Treating Metastatic Melanoma
CheckMate 067 includes data from 945 people with stage 3 or stage 4 melanoma who were randomly assigned to take either Opdivo alone, Yervoy alone, or both. Researchers analyzed data according to the stage of metastasis and some molecular markers, such as PD-L1 status and the BRAF gene mutation. PD-L1 and BRAF status reveal the possible molecular mechanisms involved in the disease process and can help predict the effectiveness of a particular treatment.
The study showed a long-term impact in preventing death for the combination of Opdivo and Yervoy. The overall five-year survival rate was 52 percent in the patients receiving the combination compared with 44 percent for patients receiving Opdivo and 26 percent for patients receiving Yervoy.
Overall, 112 of the 151 patients who received Opdivo plus Yervoy were alive and treatment-free five years following treatment. The authors noted that the drug combination is currently the only treatment for metastatic melanoma for which the median survival rate has not been reached at the five-year mark.
You have this group who are holding steady at five years and counting, he says. This is truly the best evidence we have. Every practitioner looks at this data as the source of information. Weve come to appreciate the value of looking at five-year data for all of these therapies.
The study also shows that the treatment response lasts in some patients even when they have to stop the therapy early because of serious side effects.
Immunotherapy For Stage 3 Melanoma
People with Stage III melanoma often have surgery to remove the melanoma. Lymph nodes near the cancer might also be removed to look for cancer cells. Your doctors will use the results to decide what treatment options are best for you. Sometimes, many lymph nodes near the tumor are removed . Other times, only one or a few lymph nodes are removed . In some cases, the lymph nodes do not need to be removed.
After surgery, your doctor may recommend immunotherapy to reduce the risk of your cancer coming back.
Sometimes, the surgeon cannot remove all of the cancer. This type of cancer is called “unresectable.” These cancers are treated more like Stage 4 melanoma.
You May Like: Can Melanoma Be Treated Successfully
Which Cancers Can Be Treated With Immunotherapy
Not all types of cancer have been approved for immunotherapy treatment at this time. Researchers need to prove that a new treatment is as effective as or better than the current, accepted therapies before it can be approved as standard of care. Scientists have made advances in immunotherapy research through clinical trials, such as those offered at CTCA®;and other cancer research hospitals.
Melanoma and non-small cell lung cancer were the first;cancers to get FDA approval for immunotherapy treatment because studies have amassed more long-term data for its use with those cancers. Until about five years ago, these cancers were primarily treated with interleukin-2 and interferons;. Today, immune checkpoint inhibitors are more commonly used.
Other types of cancer that may be treated with immunotherapy include:
- Liver cancer
- Bladder cancer
- Lymphoma
The FDA has not specifically approved immunotherapy for pancreatic cancer;and colon cancer. Exceptions have been made in using immunotherapy to treat these and other cancers, however, thanks to advances in advanced genomic testing.;
How Is Immunotherapy Treatment Given
How often and how long you receive immunotherapy may depend on:
- the type of immunotherapy
- how advanced the cancer is
- how you respond to treatment
- the side effects you may experience.
Checkpoint inhibitors are usually given with an injection into a vein .
When immunotherapy is used to treat some;melanoma;cases, a cream called imiquimond may be applied directly to the affected area.
Sometimes more than one type of immunotherapy drug is prescribed. Immunotherapy drugs appear to keep working for varying periods of time, and in some cases, can keep working long after other treatments are no longer used.
Don’t Miss: How Is Skin Cancer Diagnosed
What Should You Do If Youre Interested In Immunotherapy Treatment
If youre wondering whether immunotherapy may be an option for you, researching treatments on your own may be a good place to start. Read about treatment options for your specific type of cancer.
Have an honest conversation with your doctor and your care team to get better insight into your disease. Some questions to consider asking are:
- What’s my overall outlook? Is my cancer curable?
- What are our goals? What’s the realistic outcome?
- Am I a candidate for genomic testing?
- Am I a candidate for immunotherapy? If so, when would we use that in my treatment, and what are the common side effects?
- Do you have any clinical trials I may qualify for?
Try to get access to genomic testing as early as possible in your cancer journey. Some rare genetic mutations have a high response rate to targeted therapy. If you wait until youre out of other options, you may be too sick to qualify or to travel for treatment if its not available locally.
Consider getting a second opinion. A second opinion may give you a better understanding of your cancer type and stage, but it may also reveal innovative treatment options your current doctor may not have access to.
Immunotherapy is not an appropriate solution for all cancer patients, but some are thriving on the treatment. Those patients are potentially living longer with fewer side effects and a higher quality of life.
Rounding The Final Turn
Immunotherapy protocol at that time required I get boosters of nivolumab for a year. In May 2017, I developed my final immunotoxicity pneumonitis. The condition is a well-known side effect of nivolumab, and it’s like a severe case of pneumonia.
Rounding into the home stretch of treatment, I went on a high dose of prednisone. Steroids bloat you up I transformed from looking like a stick figure to resembling the Pillsbury Doughboy for several months!
Through it all, I had an amazing mentor and dear friend who had survived lung cancer and melanoma. He was given six months to live 12 years before my melanoma reappeared and he’s still going strong today.
As an athlete and an attorney, I’ve always been mentally tough. But this was much more of a mental load than I’d ever taken on. I definitely had my bad days. When I would begin to get low, I would think about my friend. If he could do it, so could I.
Don’t Miss: What Does Skin Cancer Of The Vulva Look Like