Lumpectomy Versus Mastectomy: Prognosis For Dcis
The survival rate following mastectomy for DCIS is reported to be 98% to 99%. That represents a 1% to 2% rate of local recurrence.
Medical studies of excision of DCIS reported a 20% to 44% local recurrence rate over a 10 year period.
For women who underwent breast conserving therapy and radiation there was a 10% to 15% rate of local recurrence.
However, the increased local recurrence risk following breast conservation surgery did NOT affect breast cancer-specific survival when compared with patients who underwent mastectomy for DCIS.
Both groups of patients had a 99% long term breast cancer specific survival.
The gold standard of treatment for DCIS at the moment is wide local excision with radiotherapy. According to one 2012 medical study, surgery and radiation therapy is superior to just surgery regarding recurrence rates. However, neither of these approaches affect overall survival rates.
all
Invasive Ductal Carcinoma Breast Cancer: Johns
Invasive ductal carcinoma , but the chances of being cured depend on the type, which are most likely to be curable, How this finding will affect your specific treatment is best discussed with your treating doctor, radiation therapy, Specifically, How this finding will affect your specific treatment is best discussed with your treating doctor, and More
Invasive lobular carcinoma , On a mammogram, A lumpectomy is a
What Does It Mean If My Report On Ductal Carcinoma In Situ Mentions Estrogen Receptor Or Progesterone Receptor
ER and PR are special tests that the pathologist does that are important in predicting response of the DCIS to hormone therapy . Testing for ER is done for most cases of DCIS, but testing for PR is not typically needed. Results for ER and PR are reported separately and can be reported in different ways:
- Negative, weakly positive, positive
- Percent positive with something saying whether the staining is weak, moderate, or strong
Ask your doctor how these results will affect your treatment.
Also Check: Invasive Lobular Carcinoma Grade 2 Survival Rates
How Can I Reduce My Risk For Invasive Ductal Carcinoma
Like most cancers, knowing your family history can help you take preventative steps, such as early screenings and mammograms. Even though invasive ductal carcinoma cant be prevented altogether, there are steps you can take to lower your risk:
- Maintain a healthy body weight.
- Dont smoke.
- Eat a healthy, well-balanced diet.
- Undergo genetic testing for gene mutations if recommended based on family history.
How To Wash Linen Clothes
Linen clothes are made from a natural fiber manufactured from the stem of the flax plant. After the threads are woven into the fabric, linen is sturdy and durable, moth-, bacteria- and perspiration-resistant. Unlike cotton, linen is weaker when wet and prone to abrasion and should be washed with care.
Always check the manufacturerâs label first, but most linen clothes can be washed. Some structured garments such as lined coats and jackets may need to be professionally dry cleaned due to the inner fabrics and linings that help them hold their shape.
Washable linen garments should be turned inside out before washing to prevent surface fibers from breaking. The clothes can be hand-washed or machine-washed on the gentle cycle using warm or cold water for washing and rinsing in cold water.
Table linens often require a little different treatment because of their close contact with foods that can stain. Taking care of your linen will help make sure it lasts as long as possible.
The Spruce / LetÃcia Almeida
You May Like: Stage 3b Melanoma Survival Rate
How Is Ductal Carcinoma In Situ Diagnosed
About 80% of cases are found by mammograms. On the mammogram, it appears as a shadowy area.
If your mammogram suggests that you may have DCIS, your doctor should order a biopsy to analyze the cells and confirm the diagnosis. Biopsies for DCIS are typically done using needles to remove tissue samples from the breast.
If you have DCIS, your doctor may do more tests to gather information about your cancer. These tests may include an ultrasound or MRI. Based on the results of various tests, your doctor will be able to tell the size of your tumor and how much of your breast is affected by the cancer.
How Is Ductal Carcinoma In Situ Treated
No two patients are the same. Your doctor will customize your treatment plan based on your test results and medical history. Among other things, your doctor will consider:
- Tumor location
- Aggressiveness of the cancer cells
- Your family history of breast cancer
- Results of tests for a gene mutation that would increase the risk of breast cancer
Most women with DCIS don’t have the breast removed with a mastectomy. Instead, they have a lumpectomy.
Most common is a lumpectomy followed by radiation. The surgeon removes the cancer and a small area of healthy tissue around it. Lymph nodes under the arm donât need to be removed as they are with other types of breast cancer.
After a lumpectomy, radiation cuts the chances that the cancer will come back. If cancer does return, itâs called recurrence.
Some women may opt to have a lumpectomy only. Discuss the risks of not having radiation with your doctor before deciding against it.
You and your doctors may decide that a mastectomy to remove the breast is the best course of treatment if you have any of the following:
- A strong family history of breast cancer
- A gene mutation that makes having breast cancer more likely
- Very large areas of DCIS
- DCIS lesions in multiple areas throughout your breast
- Not being able tolerate radiation therapy
You and your treatment team may also consider the use of hormone therapy if the cancer tests positive for hormone receptors. It can cut the chance of getting another breast cancer.
Show Sources
Recommended Reading: How Long Does It Take For Melanoma To Spread
Tests To Determine The Need For Chemotherapy
If the cancer is early-stage and has certain characteristics, you may be eligible for a genomic test, which looks at specific genes in the cancer to predict how likely the cancer is to recur . If a cancer is not very likely to come back, you might not need chemotherapy. If the cancer is more likely to come back, you and your doctor might decide that chemotherapy is right for you. Oncotype DX, MammaPrint, and the Prosigna Breast Cancer Prognostic Gene Signature Assay are some examples of genomic tests. Learn more about breast cancer tests.
Additional Types Of Invasive Ductal Carcinoma:
There are four types of invasive ductal carcinoma that are less common:
- Medullary Ductal Carcinoma This type of cancer is rare and only three to five percent of breast cancers are diagnosed as medullary ductal carcinoma. The tumor usually shows up on a mammogram and it does not always feel like a lump rather it can feel like a spongy change of breast tissue.
- Mucinous Ductal Carcinoma This occurs when cancer cells within the breast produce mucous, which also contains breast cancer cells. The cells and mucous combine to form a tumor. Pure mucinous ductal carcinoma carries a better prognosis than more common types of IDCs.
- Papillary Carcinoma This is a very good prognosis breast cancer that primarily occur in women over the age of 60.
- Tubular Ductal Carcinoma This is a rare diagnosis of IDC, making up only two percent of diagnoses of breast cancer. The name comes from how the cancer looks under the microscope like hundreds of tiny tubes. Tubular breast cancer has an excellent prognosis.
Show me moreâ¦
Read Also: What Is Merkel Cell Skin Cancer
Don’t Miss: Stage 3 Invasive Ductal Carcinoma Survival Rate
Prognosis And Survival For Breast Cancer
If you have breast cancer, you may have questions about your prognosis. A prognosis is the doctors best estimate of how cancer will affect someone and how it will respond to treatment. Prognosis and survival depend on many factors. Only a doctor familiar with your medical history, the type, stage and characteristics of your cancer, the treatments chosen and the response to treatment can put all of this information together with survival statistics to arrive at a prognosis.
A prognostic factor is an aspect of the cancer or a characteristic of the person that the doctor will consider when making a prognosis. A predictive factor influences how a cancer will respond to a certain treatment. Prognostic and predictive factors are often discussed together. They both play a part in deciding on a treatment plan and a prognosis.
Doctors use different prognostic and predictive factors for newly diagnosed and recurrent breast cancers.
What Can I Expect If I Have Invasive Ductal Carcinoma
If youve been diagnosed with invasive ductal carcinoma, your healthcare provider will discuss your treatment options with you in detail. For best results, youll want to begin treatment as soon as possible.
How curable is invasive ductal carcinoma?
Invasive ductal carcinoma is quite curable, especially when detected and treated early.
What is the survival rate for invasive ductal carcinoma?
The five-year survival rate for localized invasive ductal carcinoma is high nearly 100% when treated early on. If the cancer has spread to other tissues in the region, the five-year survival rate is 86%. If the cancer has metastasized to distant areas of your body, the five-year survival rate is 28%.
Keep in mind that survival rates cannot tell you how long you will live. These numbers are based on people who have undergone breast cancer treatment in the past. For more information about your specific case, talk to your healthcare provider.
Don’t Miss: What Is Squamous Cell Carcinoma Of The Head And Neck
A Disease No One Gets
Sadly, people donât âgetâ mets. In fact, a recent survey sponsored by Pfizer Oncology shows just how misunderstood it is. Sixty percent of the 2,000 people surveyed knew little to nothing about MBC while 72 percent believed advanced breast cancer was curable as long as it was diagnosed early. Even more disheartening, a full 50 percent thought breast cancer progressed because patients either didnât take the right treatment or the right preventive measures.
âTheyâve built an industry built on four words â early detection equals cure â and that doesnât even begin to define breast cancer,â said Schoger, who helped foundBreast Cancer Social Media, a virtual community for breast cancer patients, caregivers, surgeons, oncologists and others. âWomen are blamed for the fate of bad biology.â
The MBC Alliance, a consortium of 29 cancer organizations including the biggest names in breast cancer , addressed this lack of understanding and support as well as what many patient advocates term the underfunding of MBC research in a recently published landmark report.
Lobular Breast Cancer: Prognosis And Survival Rates
Lobular breast cancer, Learn about the diagnosis and treatment of invasive lobular carcinoma.The short answer is yes liver cancer is curable, radiation therapy may not cure the cancer, and treatment plan, the invasive ductal carcinoma stages are: Stage 1 A breast tumor is smaller than 2 centimeters in diameter and the cancer
Read Also: Invasive Mammary Carcinoma Survival Rate
Common Breast Cancer Types
After skin cancer, breast cancer is the most common type of cancer diagnosed in women. About 284,200 cases will be diagnosed in 2021, according to the American Cancer Society . Men also may develop breast cancer, though its much more rare.
Breast cancer is classified into different types based on how the cells look under a microscope. Most breast cancers are carcinomas, a type of cancer that begins in the linings of most organs.
What Is The Difference Between Invasive Ductal Carcinoma And Ductal Carcinoma In Situ
DCIS means the cancer is still contained in the milk duct and has not invaded any other area. IDC is cancer that began growing in the duct and is invading the surrounding tissue. Cancer staging done by a physician, along with a physical exam and medical history can help identify the best treatment options.
Materials on this page courtesy of National Cancer Institute
You May Like: Melanoma Bone Cancer Life Expectancy
Surgery For Invasive Ductal Carcinoma
Breast cancer treatment has evolved to offer patients more options. In addition to removing breast cancer, new aesthetic surgical approaches can enhance well-being and lessen the emotional impact of losing all or part of a breast to cancer. Comprehensive breast centers with coordinated teams of oncologic and plastic surgery practitioners can offer a wider array of options.
Surgery for IDC may include one of these procedures:
- Lumpectomy is removal of part of the breast. It is also known as breast-conserving surgery. Lumpectomy may be followed by radiation treatments to treat any remaining cancer cells.
- Mastectomy is removal of the breast. Mastectomy is a treatment for patients with multiple, very aggressive, or large invasive ductal tumors. It can be followed by breast reconstruction.
Invasive Ductal Carcinoma Survival Rate
The general invasive ductal carcinoma survival rate is a helpful benchmark that provides physicians with a uniform way to describe and discuss patient outcomes. Of course, a survival rate is merely an average of the experiences of a large group of people that occurred several years ago. No patient can ever be considered average, and many patients experience much better outcomes than the general survival rate would suggest. As new and better treatments are being developed and put into use, the survival rate is continually improving, and individuals who are diagnosed with breast cancer today are living longer and higher-quality lives than those who were diagnosed even only a few years ago. As such, the overall survival rate is not a reliable indicator of any specific patients prognosis.
Many individual factors can influence the invasive ductal carcinoma survival rate, including:
- Whether the cancer is newly diagnosed or a recurrence
- The stage of the cancer at the time of diagnosis, and whether it is confined to a breast or has spread to lymph nodes and other tissues and organs
- The hormone-receptor status of the cancer
- The HER2 status of the cancer
- The growth rate of the cancer cells
- The cancers response to treatment
- A patients age, overall health and menopausal status
Recommended Reading: Stage 2 Carcinoma
Histological Grade And Ki67
Histological grade information was available from the ICD-O-3 code and categorized as low , intermediate and high according to the Elston-Ellis modification of the Scarff-Bloom-Richardson grading system . Women with anaplastic carcinoma were excluded, leaving n=24,137 women for the analysis . Ki67 has been recorded routinely since 2011 and was categorized as low , intermediate or high according to cutoffs in the Norwegian treatment guidelines .
You May Like: What Is The Youngest Age To Have Breast Cancer
Some Cases Of Dcis Will Progress Towards Invasive Breast Cancer If Left Untreated
There is a general consensus that DCIS may represent a transitional stage between the normal breast tissue and invasive breast carcinoma.
However, it is still largely unknown which types of DCIS are non-progressing towards invasive breast cancer if left untreated.
One recent study estimated that only between 100 to 270 cases of DCIS per 100000 will not progress to invasive breast cancer if left untreated.
A medical study from the United Kingdom examined 84 breast cancer screening units. This large research study looked at DCIS diagnoses between the years of 2003 and 2007 for women aged 50 to 64 years.
Data from over 5,243,658 was analyzed. The average frequency of DCIS detected was 1.60 per 1000 women. The study found that for every 3 cases of DCIS detected on screening there was one less case of invasive cancer in the next 3 years.
Also Check: Life Expectancy Metastatic Melanoma
What Can You Tell Me About Invasive Ductal Carcinoma Stages
Staging describes how advanced your cancer is, based on the location, size and how far it has spread. There are five stages of ductal carcinoma:
- Stage 0: The cancer is localized to your milk ducts. This stage is also known as non-invasive ductal carcinoma in situ.
- Stage 1: The cancer has spread outside of your milk ducts to the breast tissue, but it hasnt spread to your lymph nodes. In some cases, the cancer may have spread to your lymph nodes, but not to your surrounding breast tissue.
- Stage 2: The tumor is small and has spread to one to three of your lymph nodes. Or, the tumor is larger, but hasnt spread to any of your lymph nodes.
- Stage 3: The cancer has often spread to more than three of your lymph nodes or is causing inflammation of most of your breast skin, but hasnt spread to other areas of your body.
- Stage 4: The cancer has spread to your other organs, which may include your bones, liver, lungs, brain, chest wall or distant lymph nodes.
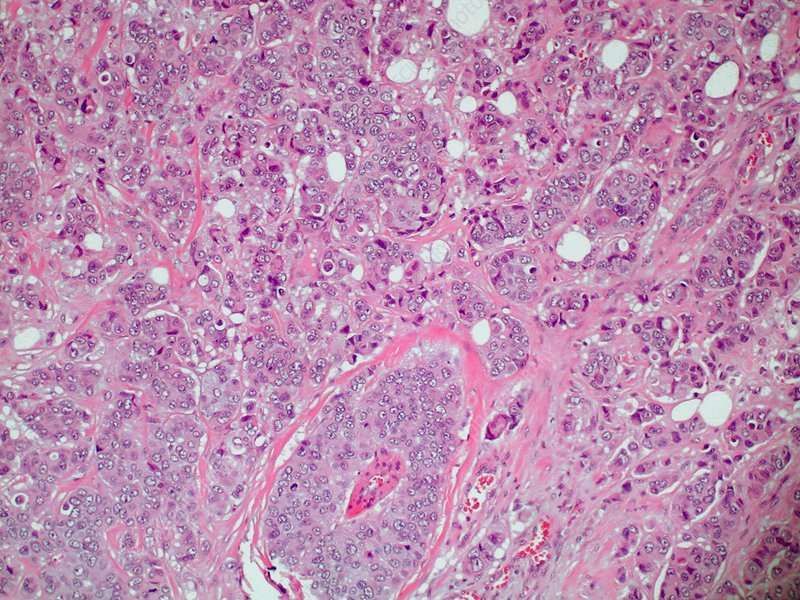
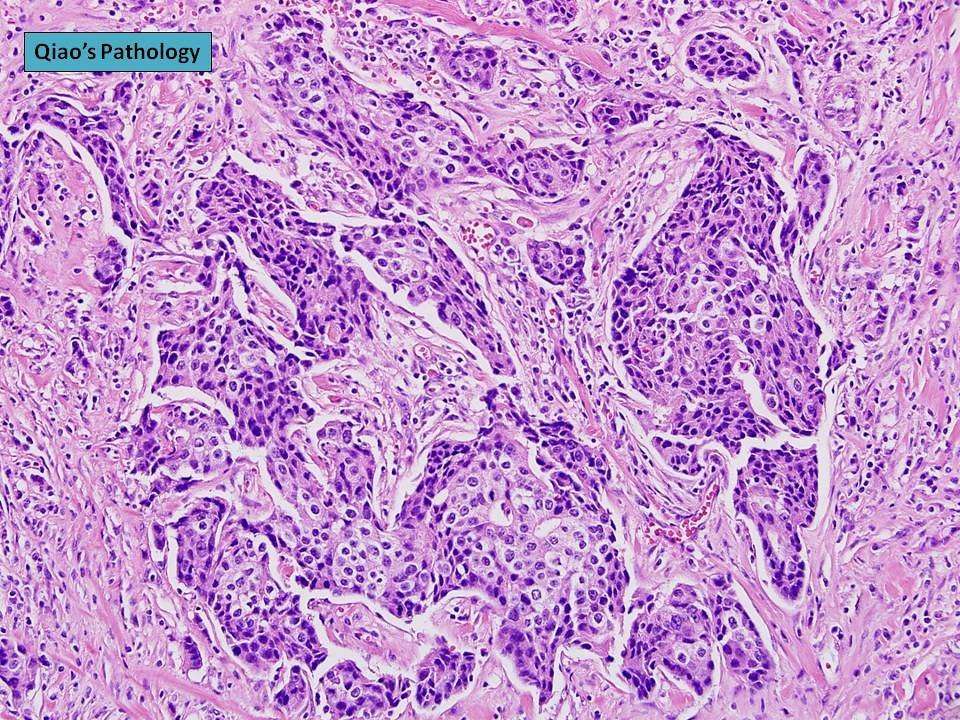
Microvinvasive Breast Carcinoma Cells Are Often Comedotype
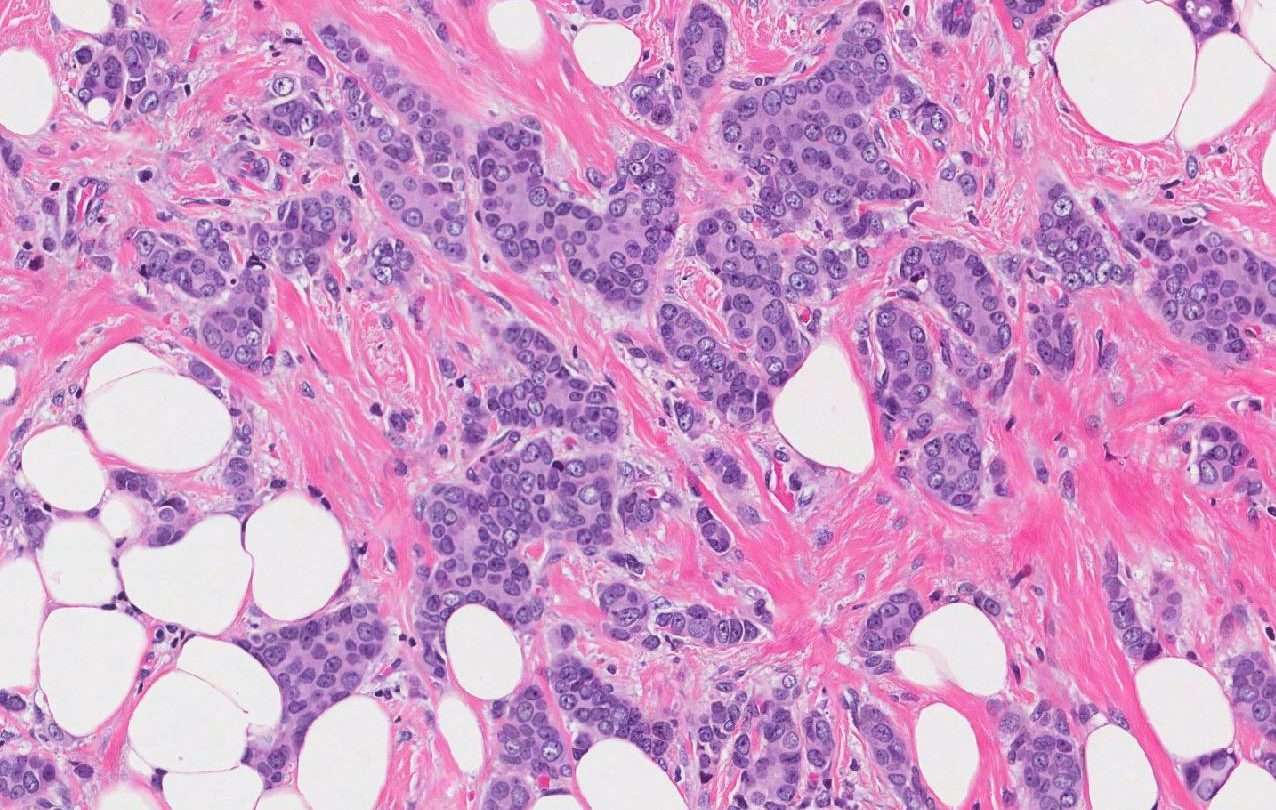
Microinvasive ductal carcinoma are frequently associated with a higher nuclear grade comedo type ductal carcinoma in situ. Other histologic subtypes of DCIS such as cribriform, papillary and solid, are thought to invade less frequently than comedo DCIS. If the microinvasive DCIS element comprises cells of either the solid, papillary, or cribriform pattern, the changes of lymph node metastasis are reduced even further.
Read Also: Merkel Cell Carcinoma Immunotherapy
Hormonal Therapy For Idc
If the cancer tested positive for hormone receptors, your doctor likely will recommend some form of hormonal therapy. Hormonal therapy, also called anti-estrogen therapy or endocrine therapy, works by lowering the amount of estrogen in the body or blocking the estrogen from signaling breast cancer cells to grow. Because hormonal therapy affects your whole body, its sometimes called a systemic treatment.
In some cases of advanced-stage IDC, hormonal therapy can be given before surgery to help shrink the cancer . Still, it’s more common for hormonal therapy to start after other treatments, such as chemotherapy or radiation therapy, unless these treatments arent needed.
Hormone receptors are special proteins found on the surface of certain cells throughout the body, including breast cells. These receptor proteins are the eyes and ears of the cells, receiving messages from the hormones in the bloodstream and then telling the cells what to do. In other words, the receptors act like an on-off switch for a particular activity in the cell. If the right substance comes along that fits into the receptor like a key fitting into a lock the switch is turned on and a particular activity in the cell begins.
You and your doctor will work together to decide which form of hormonal therapy is best in your situation. Two types of hormonal therapy are most frequently used: