How Does Immunotherapy Work
Immunotherapy is Nobel Prize-winning science that is making the untreatable treatable.
The field is one of the most exciting in cancer treatment.
The immune system constantly patrols our body, fighting off hostile invaders such as viruses.
It should attack cancers too – but cancers are a corrupted version of healthy tissue and can evolve ways of evading the immune system.
Ipilimumab and nivolumab both stop some cancers from hiding and allow the immune system to attack.
They interrupt the chemical signals that cancers use to put the brakes on the immune system.
Nivolumab blocks the off-switch on white blood cells called PD-1. Ipilimumab blocks a similar switch called CTLA-4.
It is described as taking the brakes off the immune system.
“By giving these drugs together you are effectively taking two brakes off the immune system rather than one so that the immune system is able to recognise tumours it wasn’t previously recognising and react to that and destroy them,” Prof Larkin said.
How Long Can You Live With Melanoma
Even though more people are aware of the harmful effects of the sun, rates of skin cancer are on the rise. Melanoma is the least common but often more aggressive type of skin cancer, diagnosed in more than 100,000 Americans each year. It can spread to the liver, brain, lung or soft tissue throughout the body, so treating the disease correctly is critical. No matter how advanced the disease may be at the time of diagnosis, every patient asks the same question: How long can I live with melanoma?
Forever, says Igor Puzanov, MD, MSCI, FACP, Chief of Melanoma at Roswell Park. Thanks to new drugs and treatments, survival rates are improving for melanoma patients as high as 54% at four years for stage 4 patients, with an ipilimumab and nivolumab combination. Thats not to say someone diagnosed with stage 3 or 4 melanoma is left hanging onto a sliver of hope. We are improving survival rates across the board. As survival rates for stage 4 improve, so do those for Stage 3 and so on, down the line.
Treating Stage 4 Melanoma
If melanoma comes back or spreads to other organs it’s called stage 4 melanoma.
In the past, cure from stage 4 melanoma was very rare but new treatments, such as immunotherapy and targeted treatments, show encouraging results.
Treatment for stage 4 melanoma is given in the hope that it can slow the cancer’s growth, reduce symptoms, and extend life expectancy.
You may be offered surgery to remove other melanomas that have grown away from the original site. You may also be able to have other treatments to help with your symptoms, such as radiotherapy and medicine.
If you have advanced melanoma, you may decide not to have treatment if it’s unlikely to significantly extend your life expectancy, or if you do not have symptoms that cause pain or discomfort.
It’s entirely your decision and your treatment team will respect it. If you decide not to receive treatment, pain relief and nursing care will be made available when you need it. This is called palliative care.
Also Check: How Do They Remove Basal Cell Carcinoma
What Do Stage 4 Tumors Look Like
A change to an existing mole or normal skin can be the first sign that the cancer has spread. But the physical symptoms of stage 4 melanoma arent the same for everyone. A doctor will diagnose stage 4 melanoma by looking at the primary tumor, the spread to nearby lymph nodes, and whether the tumor has spread to different organs. While your doctor wont base their diagnosis only on what your tumor looks like, part of their diagnosis involves looking at the primary tumor.
What Do Experts Think
Prof Charles Swanton, chief clinician at Cancer Research UK, said the progress in melanoma had been “incredibly fast”.
He said: “I’m inspired seeing the advancements being made in the development of immunotherapies, and their potential to transform the outlook for some patients, giving them time with friends and family they never thought they would have.
“And now work continues to make sure more people with different types of cancer can also benefit from these innovative treatments.”
Read Also: Is Squamous Cell Carcinoma Slow Growing
What Are The Prognosis And Survival Rates For Metastatic Melanoma
The prognosis for thin melanomas completely removed by surgery remains quite good although patients require long-term monitoring to watch for both new melanomas as well as evidence of late recurrence and previously undiagnosed metastasis of the original one. Survival rates for melanoma, especially for metastatic melanoma, vary widely according to many factors, including the patient’s age, overall health, location of the tumor, particular findings on the examination of the biopsy, and the depth and stage. Survival statistics are generally based on five-year survival. Much of the success reported for the targeted therapies focus on “disease free” time because, in many cases, the actual five-year survival is not affected. It is hoped that combination therapy with two or more agents targeting different stages of the melanoma cell cycle will change that.
- For stage 1 , five-year survival is near 100%.
- For stage 2 , five-year survival is 80%-90%.
- For stage 3 , five-year survival is around 50%.
- For stage 4 , five-year survival is 10%-25% depending upon sex and other demographic factors.
Clinical Characteristics Of The Patients With Brain Metastasis
A total of 79 patients were identified for this analysis. The demographic and baseline characteristics of the patients are described in Table . The median time from primary melanoma diagnosis to brain metastasis was 3.2 years , and the median time from stage IV diagnosis to brain metastasis was 2 months . Forty patients had prior extracranial metastasis at the time of initial brain metastasis 28 had concurrent extracranial metastasis at the time of brain metastasis and 5 patients developed extracranial metastasis subsequently, defined as at least 1 month after initial diagnosis of brain metastasis. Six patients had brain metastasis as the only site of distant metastasis until death or at the time of the analysis.
Table 1 Patient characteristics and treatment
The cerebrum was the most common site of brain metastasis , and 21.5% and 8.9% patients had metastasis to the cerebellum and pons, respectively. Thirty-nine had a solitary brain metastasis at the initial brain metastasis diagnosis, and the largest size of the initial brain metastasis was 10 mm or less in 31.7%. Thirty-six patients had neurological symptoms associated with brain metastasis. Forty-nine of the 79 patients had received systemic therapy prior to or at the time of brain metastasis, including checkpoint inhibitors, targeted drugs, cytotoxic chemotherapy and/or cytokine therapy.
Don’t Miss: Is Basal Cell Carcinoma Slow Growing
Clinical Staging And Pathologic Staging
To add to the complexity of staging, the cancer also may have a clinical stage and a pathologic stage.
Clinical staging takes place before surgery, based on blood tests, physical exams or imaging tests such as X-rays, a computed tomography scan, magnetic resonance imaging or positron emission tomography scans.
What doctors discover during surgery may provide more detailed information about the cancers size and spread. Often, some tissue from the surgery will be examined afterward to provide more clues. This process is known as pathologic staging, or surgical staging.
If surgery isnt possible, doctors will use the clinical stage when determining a treatment plan.
Advanced Skin Cancer Was Once A Death Sentence Immunotherapy Is Changing That
Most cancer patients are haunted by the same two questions:
“Why me?”
“Why now?”
Walton, 34, actually feels lucky advanced melanoma struck when it did.
If I had been diagnosed five years prior, who knows if I would be here,” she says.
Stage 4 melanoma used to be a death sentence. The disease doesnt respond to radiation or chemotherapy, and patients survived, on average, less than a year.
But over the last decade, doctors are successfully using a new approach, one significantly different than the treatment options available for the last 150 years.
Instead of burning or poisoning cancer cells, new medicines unleash the body’s natural defenses to fight them.
This treatment is called immunotherapy.
Beating the Odds
When Walton was 26, she found a mole on the back of her hip.
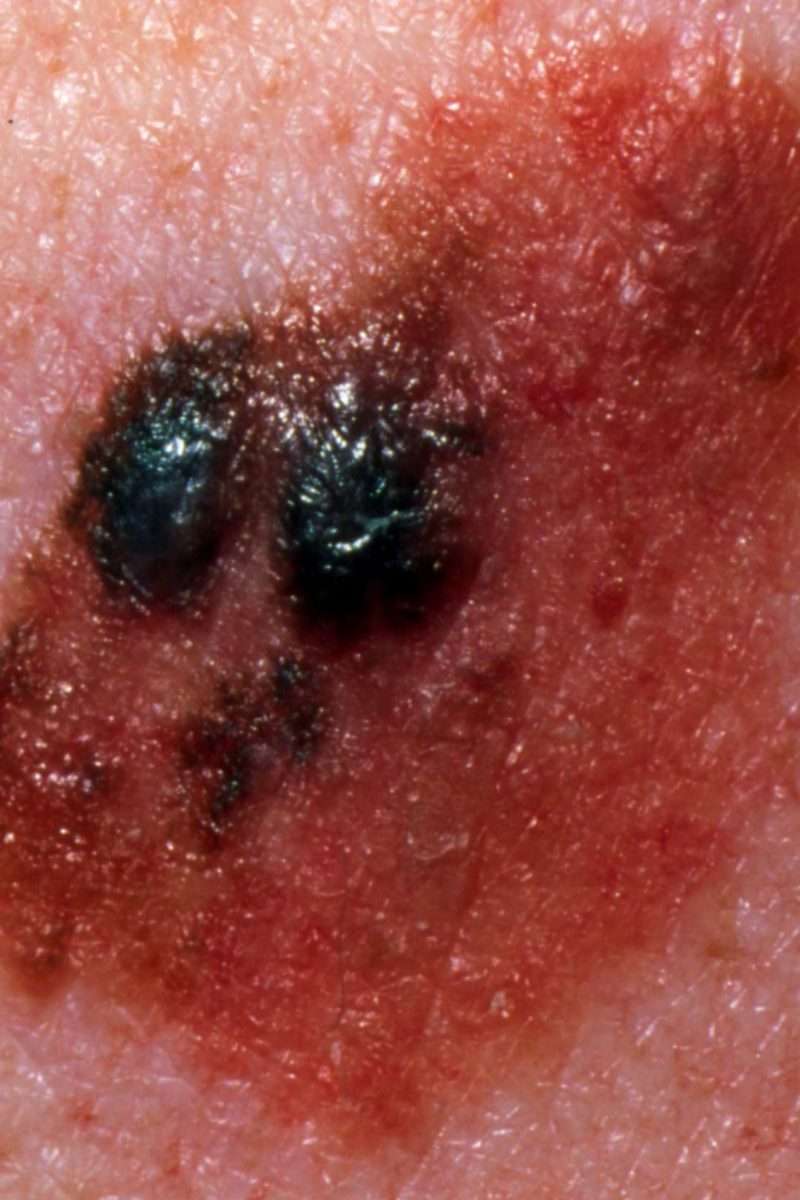
“It started morphing into this ugly, dark, bleeding thing,” she says, grimacing. “I just knew something was wrong.”
Doctors surgically removed her tumor. But a couple of years later, she discovered a tiny lump in her abdomen. It felt like a popcorn kernel, and within a few weeks grew to the size of a walnut.
A biopsy revealed she had stage 4 melanoma.
Walton searched online for information about the disease. She recalls the moment she discovered the average survival rate: six to nine months.
“I remember sort of losing my hearing, almost losing my vision to where I felt like I was in a tunnel,” she says.
But when she consulted with her oncologist, Dr. Adil Daud of UC San Francisco, he had consoling news.
Don’t Miss: What Does Oral Melanoma Look Like
Are These Patients Cured
Saying cured is always difficult in cancer, but five-year-survival is a hugely significant milestone.
Some patients taking the drugs are in total remission with no sign of any abnormality on scans.
Others like Pam still have a tumour inside their bodies, but they are no longer growing.
Out of the patients that survived, three-quarters no longer need any form of cancer treatment.
Burn Peel Repeat: A Stage Iv Melanoma Survivor Reflects On His Youthful Mistakes
Melanoma survivor Kelly Leggett was proactive about getting his skin checked, which ultimately saved his life.
Growing up in the 1960s and 1970s, we had a different relationship with the sun. We didnt think we looked good or healthy unless we had a tan. Ironic, isnt it? I spent many hours in my teens and 20s laying out in the sun burn, peel, repeatuntil the tan took hold.
In 2003, I noticed a mole behind my right ear that seemed to be changing. At a routine check-up I asked my doctor to look at the mole he told me it was nothing to worry about. Some time went by and I noticed the mole had changed dramatically so I went back to my doctor. Again, he told me it was nothing, but my gut told me otherwise, so I asked for a referral to a dermatologist. The dermatologist removed the mole immediately, sent it out for a biopsy and told me that hed follow up in a week. When he called two days later and asked to see me right away, I knew I was in trouble.
I was diagnosed with melanoma stage IIB in July 2007. Surgery was required to remove all the cancerous tissue, and plastic surgery a week later to restore the area. My oncologist prescribed a 12-month regimen of high-dose interferon injections. When the interferon treatments ended the following year, my scans showed no evidence of cancer.
At that time there was only one FDA-approved course of action for metastatic melanoma, and the success rate for it was only about 10 percent. If I did nothing, I had six months to live.
Read Also: Can Someone Die From Skin Cancer
How Can Melanoma Spread To The Brain
While melanoma normally begins in the skin, cancer cells sometimes grow and break away from the place where the cancer began. The cells that break away often travel to nearby:
-
Blood vessels
-
Lymph nodes
Once in the blood or lymph , the melanoma cells often travel to the lungs, liver, spleen, or brain.
Cancer cells growing bigger than normal cells
Cancer cells can grow, break off, and spread.
What Else Should I Know About Treatment For Advanced Melanoma
Thanks to research breakthroughs, more patients diagnosed with advanced melanoma are living longer some for years.
Because these breakthrough are relatively recent, its important to:
-
Work with a team of melanoma specialists.
-
Ask your melanoma specialists if any of the newer treatments are appropriate for you.
-
Realize that no one treatment works for everyone, so you may need to try different treatments or combine treatments.
Researchers continue to study advanced melanoma, and next-generation treatments are now being studied in clinical trials. If you want to know whether you are a match for a trial, you can find out if there are any relevant trials at, Clinical Trial Finder.
Related AAD resources
ReferencesChukwueke U, Batchelor T, et al. Management of brain metastases in patients with melanoma. J Oncol Pract. 2016 12:536-42.
Emory Medical Center. A year in the life: Jimmy Carter shares his cancer experience. Posted July 11, 2016. Last accessed March 26, 2018.
Podlipnik S, Carrera C, et al. Performance of diagnostic tests in an intensive follow-up protocol for patients with American Joint Committee on Cancer stage IIB, IIC, and III localized primary melanoma: A prospective cohort study. J Am Acad Dermatol. 2016 75:516-24.
Nordmann N, Hubbard M, et al. Effect of gamma knife radiosurgery and programmed cell death 1 receptor antagonists on metastatic melanoma. Cureus. 2017 9: e1943.
You May Like: What Is Merkel Cell Skin Cancer
Is Stage 4 Cancer Always Terminal
More severe cancers are more likely to be terminal. However, that is never a certainty. For example, the American Cancer Society say the 5-year survival rate for breast cancer that spreads to distant body parts is 27%, or 86% when it only spreads locally.
Determining the severity of cancer and its stage is a complex process. Doctors are still learning about all the factors that affect how cancer develops and affects the body.
Living As A Melanoma Skin Cancer Survivor
For many people with melanoma, treatment can remove or destroy the cancer. Completing treatment can be both stressful and exciting. You may be relieved to finish treatment, but find it hard not to worry about cancer growing or coming back. This is very common if youve had cancer.
For some people, the melanoma may never go away completely. These people may get regular treatment with immunotherapy, targeted therapy, chemotherapy, or other treatments to try to help keep the cancer under control for as long as possible. Learning to live with cancer that does not go away can be difficult and very stressful. It has its own type of uncertainty.
Also Check: How Long Does Melanoma Take To Spread
Treating Stage 3 Melanoma
If the melanoma has spread to nearby lymph nodes , further surgery may be needed to remove them.
Stage 3 melanoma may be diagnosed by a sentinel node biopsy, or you or a member of your treatment team may have felt a lump in your lymph nodes.
The diagnosis of melanoma is usually confirmed using a needle biopsy .
Removing the affected lymph nodes is done under general anaesthetic.
The procedure, called a lymph node dissection, can disrupt the lymphatic system, leading to a build-up of fluids in your limbs. This is known as lymphoedema.
Cancer Research UK has more information about surgery to remove lymph nodes.
The Trial Is A Lifesaver
“I’ve never had chemotherapy, but I have seen it up close, and it can be pretty harsh,” she says, referring to her experience as an MD Anderson volunteer and with her father’s treatment years ago.
“Dealing with cancer can be such a difficult fight,” she says. “Without this clinical trial, I wouldn’t be here, and it’s a great pleasure for me to know that this study will be used to help other people.”
Tawbi notes oncologists continue to work with radiation oncologists and neurosurgeons to further improve outcomes and provide the best guidance for patients on initial treatment and the best timing for subsequent treatments, if needed.
“Helping 57 or 58 percent of these patients is significant improvement, but our goal is to reach 100 percent,” Tawbi says.
Read Also: How Fast Does Squamous Cell Skin Cancer Spread
It Usually Starts With Suspicious Spot
Maybe you noticed a mole that stood out from the rest . Its edges were irregular, maybe it was asymmetrical in shape, unevenly pigmented, noticeably large , or rapidly changing . These are the spots that concern dermatologists. If you had one, your doc did a biopsy on your own ugly duckling. During this in-office procedure, your doctor either shaved off a layer of your mole, punched it out with a hole-punch-like tool, or removed it with surgical excision, along with a margin of healthy skin to check for wandering cancer cells.
Gearing Up For The Fight
Tim reached out to friends, family and friends of friends and family to figure out his next steps. Repeatedly, the top recommendation was The University of Kansas Cancer Center.
When I first met with Dr. Doolittle, I felt very confident in him. I told him I wanted to fight this thing head on, and he told me that was his style, too, Tim says. Gary Doolittle, MD, is a medical oncologist who specializes in melanoma.
An avid Royals baseball fan, Tim told Dr. Doolittle that he wanted to delay treatment for just 1 week. I had plans to meet friends out of town and go to the last Royals game of the season. I needed that week to enjoy myself so I could gear up for my fight, says Tim. Dr. Doolittle agreed it was a good choice. From then on, I knew he was my guy.
Treatment has been tough. Tim enrolled in a testing the effectiveness of a combined treatment for metastatic melanoma that kick-starts the immune system to attack cancer cells. He had an adverse reaction to one of the medications, which sometimes happens. Still, he was able to continue with the other medication, which could only be administered in the hospital. He received 54 doses of that drug over 5 months.
I was totally wiped out, he says.
Even with the intensive therapy, the cancer spread to his brain. It was time for a new plan of attack. The next round of treatment, which did not involve a clinical trial, kept his cancer from advancing, but didnt shrink his tumors.
Also Check: Does Skin Cancer Make You Tired