Types Of Basal Cell Cancer: Nodular Superficial And Infiltrative Carcinomas
Basal cell carcinoma is a common variety of skin cancer that most frequently develops on the head, neck, torso, and other areas of the body that are at risk for excessive sun exposure. Not all types of basal cell cancer are the same. The physical characteristics of these skin carcinomas can be grouped into three main categories, which are described in further detail below.
What Is A Basal Cell Carcinoma
Basal cell carcinoma is a type of skin cancer that occurs when there is damage to the DNA of basal cells in the top layer, or epidermis, of the skin. They are called basal cells because they are the deepest cells in the epidermis. In normal skin, the basal cells are less than one one-hundredth of an inch deep, but once a cancer has developed, it will spread deeper.
Skin Color And Being Exposed To Sunlight Can Increase The Risk Of Basal Cell Carcinoma And Squamous Cell Carcinoma Of The Skin
Anything that increases your chance of getting a disease is called a risk factor. Having a risk factor does not mean that you will get cancer; not having risk factors doesnt mean that you will not get cancer. Talk with your doctor if you think you may be at risk.
Risk factors for basal cell carcinoma and squamous cell carcinoma of the skin include the following:
- Being exposed to natural sunlight or artificial sunlight over long periods of time.
- Having a fair complexion, which includes the following:
- Fair skin that freckles and burns easily, does not tan, or tans poorly.
- Blue, green, or other light-colored eyes.
- Red or blond hair.
Although having a fair complexion is a risk factor for skin cancer, people of all skin colors can get skin cancer.
Older age is the main risk factor for most cancers. The chance of getting cancer increases as you get older.
Don’t Miss: What Is The Worst Skin Cancer To Have
Preventing Basal Cell Carcinoma
Basal cell carcinoma prevention is the same as prevention methods for all skin cancers, with the goal of protecting skin from harmful UV rays.
The number one thing people can do is to practice good sun protection and sun avoidance, meaning wear sunscreen and protect the skin from getting sun damage, says Stevenson. Its also important to get skin checks regularly for early detection.
Stevenson says if someone is prone to skin cancers for example, has very fair skin, sunburns as a child, or a history of skin cancer in the family its better to go out in the late afternoon or early morning when the sun isnt as strong, or stay primarily in the shade.
Anyone spending time in the sun, regardless of complexion, should practice sun protective behaviors, including wearing sunscreen.
The Centers for Disease Control and Prevention recommends a sunscreen with a minimum sun protection factor of 15, and UVA and UVB broad spectrum protection. It also advises people to stay in the shade as much as possible and wear protective clothing including brimmed hats and sunglasses. Stevenson suggests looking for a SPF over 30.
Lebwohl says the SPF number directly correlates with the amount of protection it gives you. He says to divide the amount of time in the sun by the SPF number. For example, if someone is in the sun for 60 minutes, and wearing SPF 30, its as if they were exposed to two minutes of damaging rays rather than the full 60 minutes.
There Are Three Ways That Cancer Spreads In The Body
Cancer can spread through tissue, the lymph system, and the blood:
- Tissue. The cancer spreads from where it began by growing into nearby areas.
- Lymph system. The cancer spreads from where it began by getting into the lymph system. The cancer travels through the lymph vessels to other parts of the body.
- Blood. The cancer spreads from where it began by getting into the blood. The cancer travels through the blood vessels to other parts of the body.
Read Also: How Does Skin Cancer Feel
Basal And Squamous Cell Skin Cancer Stages
After someone is diagnosed with cancer, doctors will try to figure out if it has spread, and if so, how far. This process is called staging. The stage of a cancer describes how much cancer is in the body. It helps determine how serious the cancer is and how best to treat it.
The stage is based on the results of the physical exam, the skin biopsy , and the results of imaging tests if they are done. These exams and tests are described in Tests for Basal and Squamous Cell Skin Cancers.
Determining the stage of basal cell skin cancers is rarely needed, because these cancers are almost always cured before they spread to other parts of the body.
Squamous cell skin cancers are more likely to spread , so determining the stage can be more important, particularly in people who are at higher risk. This includes people with weakened immune systems, such as those who have had organ transplants and people infected with HIV, the virus that causes AIDS. Most squamous cell skin cancers occur in the head and neck region and tend to have a higher risk of recurring or spreading compared to those in other locations.
Basal Cell Carcinoma Staging
Staging;is the process of determining whether cancer has spread and, if so, how far. The stage of the disease may affect the treatment plan.
The stage is based on the size of the tumor, how deeply into the skin it has grown, and whether cancer has spread beyond the tumor to the lymph nodes. Your doctor will look at the results of the biopsy to determine the stage.;In rare cases, your doctor may recommend imaging such as CT or PET-CT scan to see if the cancer has spread beyond the skin
Stages are numbered in Roman numerals between 0 and IV.
Most non-melanoma skin cancers are Stage 0 or Stage 1. Stage 3 and 4 are relatively rare. Based on the type of cancer, the stage of cancer, your overall health, and other factors, your doctor works with you to develop a treatment plan.
High risk features for primary tumor staging
- Depth/invasion: >2 mm thickness , Clark level IV, Perineural invasion
- Anatomic: Primary site ear
- Location: Primary site hair-bearing lip
- Differentiation: Poorly differentiated or undifferentiated
Recommended Reading: Can Basal Cell Carcinoma Be Fatal
Can Basal Cell Carcinoma Spread
Basal cell carcinoma, the most common type of skin cancer, develops most commonly after frequent sun exposure or tanning bed use. Basal cell carcinoma is a slow-growing cancer, but early treatment is important because, if left untreated, basal cell carcinoma can spread and grow deep into the skin. My surgeon told me many years ago that, what appears to be a small area of basal cell carcinoma on the surface of the skin, can actually be as large as a silver dollar in other layers of the skin.
What Are The Signs And Symptoms Of Basal Cell Carcinoma
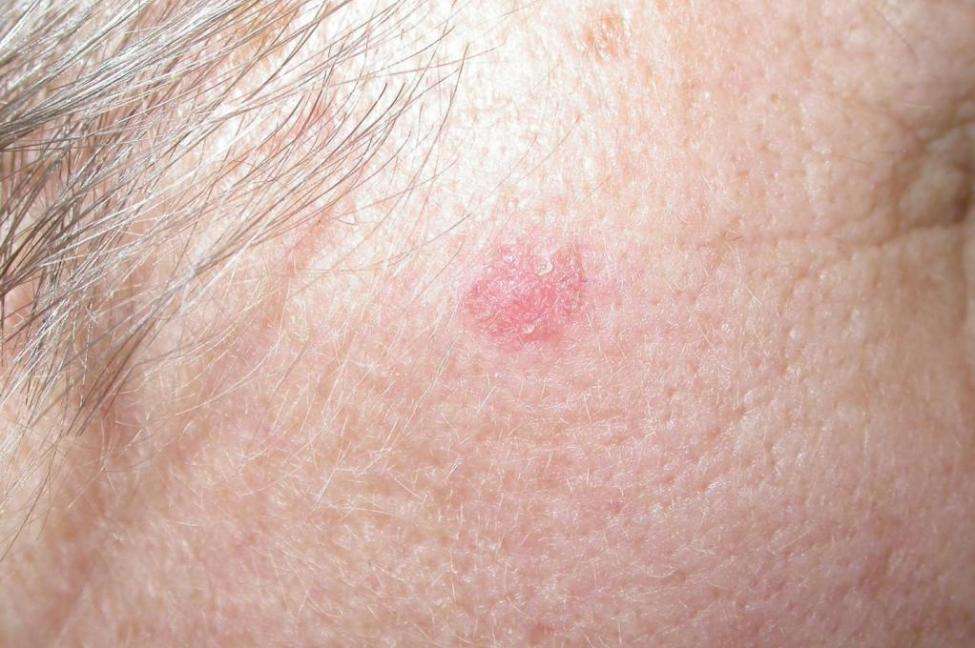
Basal cell carcinomas can appear anywhere on the body but the most common sites are sun exposed areas such as the face and arms. Its important to keep a close eye on your skin to try and identify early basal cell carcinoma, as its easier to treat if identified early on.
Typical Basal cell carcinoma symptoms are:
- New skin lesion
- Change in colour of a lesion
The typical lesions to watch out for are as follows:
- Pink or translucent, shiny bumps or pearly nodules, sometimes with dark spots or black, blue, or brown surface
- Growths, pink in color, with raised edges and sunken center, usually with irregular blood spoke-wheel vessels on its surface
- Pale or yellow scar-like areas
- Elevated reddish patches
- Oozing, crusted, scaly and open sores that dont heal over time
Recommended Reading: What Is Soft Tissue Carcinoma
Diagnosing Basal Cell Carcinoma
The most common way dermatologists diagnose basal cell carcinoma is with a full body skin check.
Stevenson says during the diagnosis process dermatologists are looking for papules with skin cancer characteristics. Sometimes dermatologists will use a tool called a dermatoscope, which uses a polarized light to look for other signs of skin cancer. With their training, dermatologists should be able to tell patients if the lesion is benign or something that should be removed because of a skin cancer concern.
RELATED: Do You Need to Wear Sunscreen Indoors?
Basal Cell Carcinoma Stages
There are certain features that are considered to make the cancer at higher risk for spreading or recurrence, and these may also be used to stage basal cell carcinomas. These include:
- Greater than 2 mm in thickness
- Invasion into the lower dermis or subcutis layers of the skin
- Invasion into the tiny nerves in the skin
- Location on the ear or on a hair-bearing lip
After the TNM components and risk factors have been established, the cancer is given a stage. For basal cell carcinoma staging, the factors are grouped and labeled 0 to 4. The characteristics and stages of basal cell carcinoma are:
Stage 0: Also called carcinoma in situ, cancer discovered in this stage is only present in the epidermis and has not spread deeper to the dermis.
Stage 1 basal cell carcinoma: The cancer is less than 2 centimeters, about 4/5 of an inch across, has not spread to nearby lymph nodes or organs, and has one or fewer high-risk features.
Stage 2;basal cell carcinoma: The cancer is larger than 2 centimeters across, and has not spread to nearby organs or lymph nodes, or a tumor of any size with 2 or more high-risk features.
Stage;3 basal cell carcinoma: The cancer has spread into facial bones or 1 nearby lymph node, but not to other organs.
Stage 4 basal cell carcinoma: The cancer can be any size and has spread to 1 or more lymph nodes which are larger than 3 cm and may have spread to bones;or other organs in the body.
Recommended Reading: Can Melanoma Be Treated Successfully
What Are The Clinical Features Of Basal Cell Carcinoma
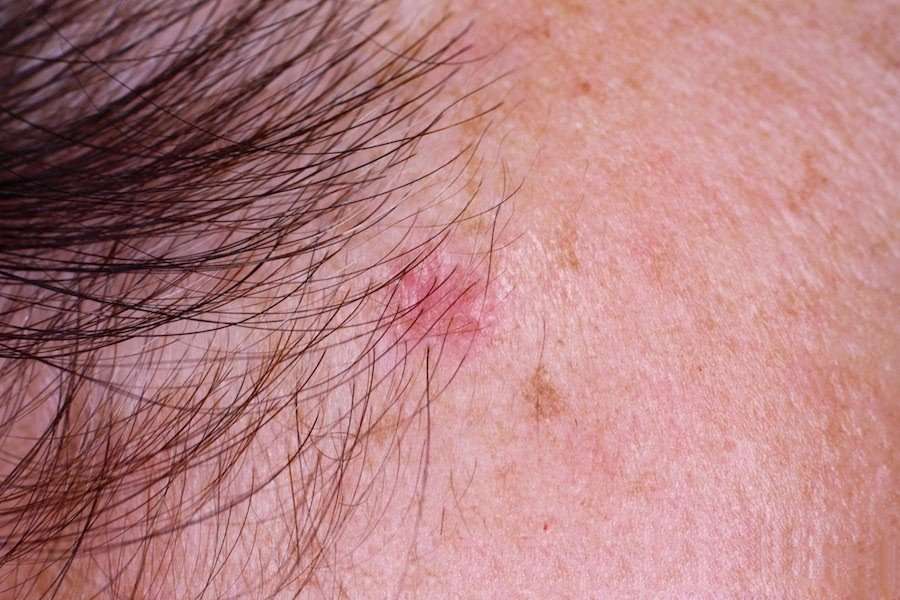
BCC is a locally invasive skin tumour. The main characteristics are:
- Slowly growing plaque or nodule
- Skin coloured, pink or pigmented
- Varies in size from a few millimetres to several centimetres in diameter
- Spontaneous bleeding or ulceration
BCC is very rarely a threat to life. A tiny proportion of BCCs grow rapidly, invade deeply, and/or metastasise to local lymph nodes.
Who Gets Basal Cell Carcinoma
Risk factors for BCC include:
- Age and sex: BCCs are particularly prevalent in elderly males. However, they also affect females and younger adults
- Repeated prior episodes of sunburn
- Fair skin, blue eyes and blond or red hairnote; BCC can also affect darker skin types
- Previous cutaneous injury, thermal burn, disease
- Inherited syndromes: BCC is a particular problem for families with basal cell naevus syndrome , Bazex-Dupré-Christol syndrome, Rombo syndrome, Oley syndrome and xeroderma pigmentosum
- Other risk factors include ionising radiation, exposure to arsenic, and immune suppression due to disease or medicines
Also Check: What Does Skin Cancer Look Like On Your Head
What Is Squamous Cell Cancer
Squamous cell carcinoma of the skin is a common skin cancer that typically develops in chronic sun-exposed areas of your body. This type of skin cancer is usually not nearly as aggressive as melanoma and is uncontrolled growth of cells in the epidermis of your skin.
It can become disfiguring and sometimes deadly if allowed to grow. Squamous cell carcinomas are at least twice as frequent in men as in women. They rarely appear before age 50 and are most often seen in individuals in their 70s.
An estimated 700,000 cases of SCC are diagnosed each year in the United States, resulting in approximately 2,500 deaths.
Basal Cell Carcinoma Causes And Prevention
Several causes for basal cell carcinoma have been identified. BCC can, however, arise without any of these. They start with a single cell that becomes abnormal due to damage to its DNA. These cells then multiply, and as abnormal cells build-up, the skin lesion becomes visible.4
Basal cell carcinoma risk factors include: 5
- Ultraviolet lightUV light from sunshine and commercial tanning beds can both cause damage to cells mentioned, ultimately resulting in abnormal skin lesions. More sun exposure from warm climates, excess suntanning and excess use of tanning beds all make BCC more likely. Severe sunburn can also be a factor.
- Fair skinFair skin is a risk factor as there is less protection for the deeper skin layers from melanin.
- AgeAs detailed, BCC starts with damage to cells and as we get more damage over time, increasing age is a significant factor.
- Medical treatmentRadiotherapy for other medical conditions and immunosuppressants drugs can increase the risks of basal carcinoma and must be taken into account when assessing skin lesions.
For more details of risks factors, see this article.
Basal cell carcinoma prevention
Avoiding or minimising these risk factors is the mainstay of basal cell carcinoma prevention. The most important preventable factor is sun exposure.
Also Check: What Is The Main Cause Of Skin Cancer
Taking Care Of Yourself
After you’ve been treated for basal cell carcinoma, you’ll need to take some steps to lower your chance of getting cancer again.
Check your skin. Keep an eye out for new growths. Some signs of cancer include areas of skin that are growing, changing, or bleeding. Check your skin regularly with a hand-held mirror and a full-length mirror so that you can get a good view of all parts of your body.
Avoid too much sun. Stay out of sunlight between 10 a.m. and 2 p.m., when the sun’s UVB burning rays are strongest.
Use sunscreen. The suns UVA rays are present all day long — thats why you need daily sunscreen. Make sure you apply sunscreen with at least a;6% zinc oxide and a sun;protection factor of 30 to all parts of the skin that aren’t covered up with clothes every day. You also need to reapply it every 60 to 80 minutes when outside.
Dress right. Wear a broad-brimmed hat and cover up as much as possible, such as long-sleeved shirts and long pants.
Continued
Infiltrated Basal Cell Carcinoma
This version of basal cell carcinoma is presented as thin bundles of basaloid cells with nest-like configuration located between the collagenous fibers on the dermis and infiltrating in the depth. Clinically, it is a whitish, compact, not-well defined plaque . The most common localization is in the upper part of the trunk or the face. Seldom had the paresthesia or hyperesthesia as a symbol of perineural infiltration appeared, especially when the tumor is localized on face. This clinical version is often underestimated when the borders of surgical excision are estimated. Histologically this variant is presented as thin, nest-like bundles of basaloid cells infiltrating in the dermal collagenous fibers .
Infiltrated basal cell carcinoma. Thin bundles of basaloid cells invade the dermis
Read Also: How Is Basal Cell Carcinoma Removed From The Nose
Squamous Cell Carcinoma Treatment
Squamous cell carcinomas detected at an early stage and removed promptly are almost always curable and cause minimal damage. However, left untreated, they may grow to the point of being very difficult to treat.
A small percentage may even metastasize to distant tissues and organs. Your doctor can help you determine if a particular SCC is at increased risk for metastasis and may need treatment beyond simple excision.
Fortunately, there are several effective ways to treat squamous cell carcinoma. The choice of treatment is based on the type, size, location, and depth of penetration of the tumor, as well as the patients age and general health. Squamous cell carcinoma treatment can almost always be performed on an outpatient basis.
Staging For Basal Cell Carcinoma And Squamous Cell Carcinoma Of The Skin Depends On Where The Cancer Formed
Staging for basal cell carcinoma and squamous cell carcinoma of the eyelid is different from staging for basal cell carcinoma and squamous cell carcinoma found on other areas of the head or neck. There is no staging system for basal cell carcinoma or squamous cell carcinoma that is not found on the head or neck.
Surgery to remove the primary tumor and abnormal lymph nodes is done so that tissue samples can be studied under a microscope. This is called pathologic staging and the findings are used for staging as described below. If staging is done before surgery to remove the tumor, it is called clinical staging. The clinical stage may be different from the pathologic stage.
Recommended Reading: What Are The 4 Types Of Melanoma
Mohs Microscopically Controlled Surgery
|
Because skin cancer cells often have spread beyond the edges of the visible patch on the skin, doctors sometimes use a special surgical technique to make sure they remove all of the cancer. In this technique, called Mohs microscopically controlled surgery or Mohs micrographic surgery, doctors first remove the visible tumor and then begin cutting away the edges of the wound bit by bit. During surgery, doctors examine pieces of tissue to look for cancer cells. Tissue removal from the area continues until the samples no longer contain cancer cells. This procedure enables doctors to limit the amount of tissue removed and thus is especially useful for cancers near such important sites as the eye. After removing all of the cancer, doctors decide how best to replace the skin that has been cut away. They may bring the edges of the remaining skin together with sutures or use a skin graft or skin flap. Or they may place dressings on top of the wound and let the skin heal on its own. Mohs surgery reduces recurrence rates for skin cancers. This surgery is useful for basal cell and squamous cell cancers but is less often used for melanoma. |